11 Signs of High Cholesterol and What Your Numbers Actually Mean
High cholesterol stands as one of the most insidious health conditions affecting millions worldwide, earning its reputation as a "silent killer" because it typically presents no obvious symptoms until serious complications arise. This waxy, fat-like substance naturally produced by your liver becomes problematic when levels exceed healthy ranges, creating a cascade of cardiovascular risks that can culminate in heart attacks, strokes, and peripheral artery disease. Understanding the subtle signs your body may be sending, coupled with a comprehensive grasp of what your cholesterol numbers actually represent, forms the cornerstone of effective prevention and management. While many people assume they'll feel unwell if their cholesterol is elevated, the reality is far more complex – high cholesterol often operates beneath the surface for years or even decades before manifesting in life-threatening events. This comprehensive exploration will decode the warning signs your body may be displaying, demystify the numerical values that appear on your lipid panel, and provide you with the knowledge necessary to take proactive control of your cardiovascular health. By recognizing these indicators early and understanding the science behind cholesterol metabolism, you can work with healthcare professionals to implement targeted interventions that may prevent serious complications and promote long-term wellness.
1. Chest Pain and Angina - Your Heart's Cry for Help

Chest pain, medically known as angina, represents one of the most significant warning signs that high cholesterol may be compromising your cardiovascular system through the development of coronary artery disease. When cholesterol builds up in the arteries supplying blood to your heart muscle, it creates plaques that narrow these vital pathways, reducing the flow of oxygen-rich blood to cardiac tissue. This reduction in blood flow becomes particularly problematic during periods of increased demand, such as physical exertion, emotional stress, or even after eating large meals. The resulting chest pain typically manifests as a squeezing, pressure-like sensation that may radiate to the left arm, jaw, neck, or back, often accompanied by shortness of breath, sweating, or nausea. Unlike the sharp, stabbing pain associated with muscle strains or other non-cardiac causes, angina related to cholesterol-induced arterial blockages tends to be more diffuse and may worsen with activity while improving with rest. The pain may also present differently in women, who might experience more subtle symptoms such as fatigue, indigestion-like discomfort, or upper back pain rather than the classic crushing chest sensation. Research indicates that individuals with total cholesterol levels above 240 mg/dL face significantly higher risks of developing coronary artery disease, making chest pain a critical red flag that demands immediate medical evaluation and comprehensive cholesterol management strategies.
2. Shortness of Breath - When Simple Tasks Become Challenging

Unexplained shortness of breath, particularly during routine activities that previously posed no difficulty, can signal that high cholesterol is affecting your cardiovascular system's ability to efficiently deliver oxygen throughout your body. As cholesterol plaques accumulate in coronary arteries, the heart muscle receives insufficient blood supply, forcing it to work harder to maintain adequate circulation. This increased workload can lead to a condition called heart failure, where the heart cannot pump blood effectively enough to meet the body's demands. Consequently, even simple activities like climbing stairs, walking short distances, or performing household chores may leave you feeling breathless and fatigued. The mechanism behind this symptom involves the heart's compensatory response to reduced efficiency – when cardiac output decreases due to compromised blood flow, the body attempts to maintain oxygen delivery by increasing breathing rate and depth. Additionally, high cholesterol can contribute to the development of pulmonary complications, as reduced cardiac function may cause fluid to back up into the lungs, creating a condition known as pulmonary edema. This fluid accumulation further impairs gas exchange, exacerbating breathing difficulties and creating a cycle of worsening symptoms. Studies have shown that individuals with LDL cholesterol levels exceeding 160 mg/dL are at substantially increased risk for developing heart failure, making persistent shortness of breath a symptom that warrants immediate medical attention and comprehensive cholesterol evaluation.
3. Xanthomas - Visible Cholesterol Deposits on Your Skin
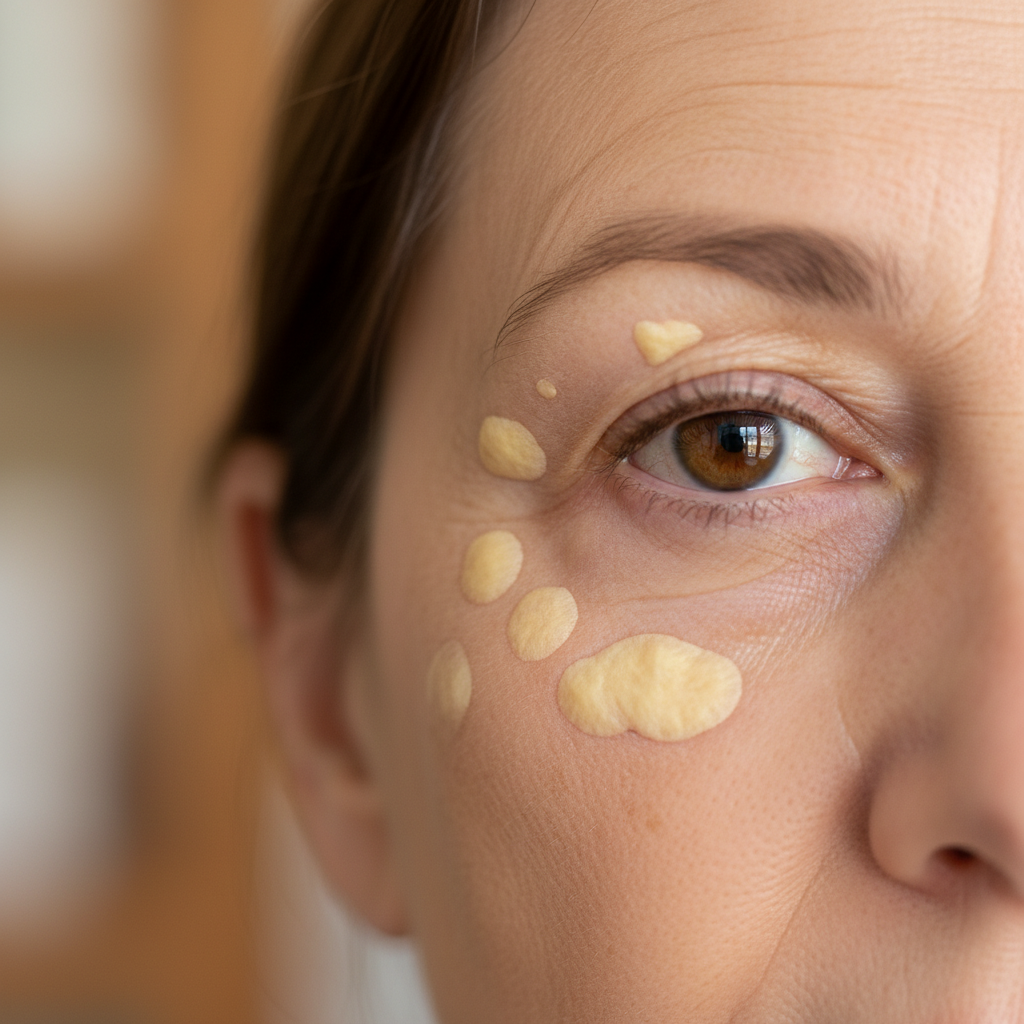
Xanthomas represent one of the most visible and distinctive signs of severely elevated cholesterol levels, manifesting as yellowish, waxy deposits that appear on various parts of the body, particularly around the eyes, joints, and tendons. These distinctive lesions occur when cholesterol levels become so elevated that the excess lipids begin to accumulate in tissues outside the bloodstream, creating palpable nodules or plaques that can range from small, flat patches to larger, raised growths. The most common locations for xanthomas include the eyelids (xanthelasma), where they appear as soft, yellowish plaques along the upper or lower lid margins, and the Achilles tendons, where they may create noticeable thickening or nodular formations. Elbow creases, knuckles, and knee areas are also frequent sites for these cholesterol deposits, which may initially be mistaken for cysts or other benign skin growths. The presence of xanthomas typically indicates extremely high cholesterol levels, often associated with genetic conditions such as familial hypercholesterolemia, where total cholesterol levels may exceed 300-400 mg/dL. While not painful, these deposits can become cosmetically concerning and may interfere with joint function if they develop in areas of high mechanical stress. Research demonstrates that individuals presenting with xanthomas often have underlying lipid disorders that require aggressive treatment, as the visible cholesterol deposits usually correlate with significant arterial plaque formation throughout the cardiovascular system. Early recognition and treatment of the underlying hypercholesterolemia can sometimes lead to regression of these deposits, making them important clinical markers for both diagnosis and treatment monitoring.
4. Peripheral Artery Disease Symptoms - When Circulation Fails

Peripheral artery disease (PAD) symptoms, including leg pain during walking (claudication), cold extremities, and poor wound healing, often serve as early indicators that high cholesterol is compromising circulation throughout the body's arterial network. When cholesterol plaques develop in the arteries supplying blood to the legs, arms, and other peripheral tissues, they create significant restrictions in blood flow that become particularly apparent during periods of increased demand. Claudication, the hallmark symptom of PAD, typically manifests as cramping, aching, or fatigue in the leg muscles during walking or exercise, with symptoms reliably improving after a few minutes of rest. This pain pattern occurs because the narrowed arteries cannot deliver sufficient oxygen-rich blood to meet the metabolic demands of working muscles, creating a temporary ischemic condition that resolves when activity ceases. Additional signs of compromised peripheral circulation include chronically cold hands or feet, even in warm environments, diminished or absent pulses in the extremities, and changes in skin color or texture, particularly a pale or bluish appearance in the affected areas. Wounds, cuts, or sores on the legs or feet may heal slowly or poorly due to reduced blood flow, increasing the risk of infection and other complications. Hair loss on the legs and brittle, slow-growing toenails can also indicate chronic circulation problems related to cholesterol-induced arterial disease. Studies reveal that individuals with total cholesterol levels above 240 mg/dL face a significantly elevated risk of developing PAD, with the condition affecting approximately 8-12% of adults over age 50, making these circulation-related symptoms important early warning signs that demand comprehensive cholesterol evaluation and management.
5. Erectile Dysfunction - An Unexpected Cardiovascular Warning

Erectile dysfunction (ED) in men can serve as an early and often overlooked indicator of high cholesterol and developing cardiovascular disease, as the delicate blood vessels supplying the penis are among the first to be affected by cholesterol-induced arterial damage. The physiological mechanism of normal erectile function depends entirely on adequate blood flow through small arteries and arterioles, which are particularly vulnerable to the atherosclerotic changes caused by elevated cholesterol levels. When cholesterol plaques begin to narrow these vessels, they impair the vascular engorgement necessary for achieving and maintaining erections, often years before similar blockages become apparent in larger coronary or cerebral arteries. Research has consistently demonstrated that men experiencing ED have significantly higher rates of coronary artery disease, with studies showing that erectile problems may precede heart attack symptoms by an average of 2-5 years. The connection between cholesterol and erectile function extends beyond simple mechanical blockage – high cholesterol levels also promote endothelial dysfunction, reducing the production of nitric oxide, a crucial molecule that facilitates both penile blood vessel dilation and coronary artery health. Additionally, the chronic inflammation associated with elevated cholesterol levels can damage the smooth muscle cells within penile blood vessels, further compromising erectile function. Men with total cholesterol levels exceeding 240 mg/dL or LDL levels above 160 mg/dL show substantially higher rates of erectile dysfunction compared to those with optimal lipid profiles. This relationship has led many cardiologists to view ED as a potential "canary in the coal mine" for cardiovascular disease, prompting comprehensive cholesterol screening and aggressive risk factor modification in men presenting with sexual dysfunction, particularly those over age 40.
6. Fatigue and Weakness - When Energy Levels Plummet

Persistent fatigue and unexplained weakness can indicate that high cholesterol is compromising your cardiovascular system's ability to efficiently deliver oxygen and nutrients throughout your body, leading to a chronic state of reduced energy and endurance. When cholesterol plaques narrow arteries and reduce blood flow, every organ system receives less than optimal circulation, forcing the body to operate in a state of chronic mild hypoxia that manifests as persistent tiredness and reduced physical capacity. The heart, working harder to pump blood through narrowed vessels, may become less efficient over time, leading to reduced cardiac output and subsequent fatigue that worsens throughout the day or with minimal exertion. This cardiovascular-related fatigue differs from normal tiredness in that it tends to be persistent, doesn't improve significantly with rest, and may be accompanied by other subtle symptoms such as difficulty concentrating, reduced exercise tolerance, or a general sense of malaise. The brain, being particularly sensitive to changes in blood flow and oxygen delivery, may contribute to fatigue through reduced cognitive function and altered neurotransmitter production when cholesterol-related vascular changes affect cerebral circulation. Additionally, high cholesterol levels can contribute to sleep disorders, including sleep apnea, which further exacerbates daytime fatigue and creates a cycle of worsening symptoms. Research indicates that individuals with total cholesterol levels above 240 mg/dL report significantly higher rates of chronic fatigue and reduced quality of life compared to those with optimal lipid profiles. The inflammatory processes associated with elevated cholesterol can also contribute to fatigue by promoting the release of cytokines that affect energy metabolism and mood regulation, making persistent tiredness an important but often overlooked sign of developing cardiovascular disease.
7. Dizziness and Balance Issues - Neurological Warning Signs

Dizziness, lightheadedness, and balance problems can signal that high cholesterol is affecting blood flow to the brain and inner ear, creating neurological symptoms that may precede more serious cerebrovascular events. When cholesterol plaques develop in the carotid arteries or other vessels supplying the brain, they can cause intermittent reductions in cerebral blood flow, leading to episodes of dizziness, vertigo, or feeling faint, particularly when changing positions quickly or during periods of physical exertion. The brain's high metabolic demands make it particularly sensitive to even minor reductions in blood flow, and the complex network of small vessels within the brain can be compromised by the same atherosclerotic processes that affect coronary arteries. These neurological symptoms may manifest as brief episodes of disorientation, difficulty maintaining balance while walking, or a sensation of the room spinning, which can significantly impact daily activities and increase fall risk, particularly in older adults. The inner ear's vestibular system, responsible for balance and spatial orientation, relies on a delicate blood supply that can be disrupted by cholesterol-related vascular changes, leading to persistent balance issues or recurrent vertigo episodes. Additionally, high cholesterol can contribute to the development of small vessel disease in the brain, causing subtle cognitive changes and coordination problems that may initially be attributed to normal aging or stress. Research demonstrates that individuals with total cholesterol levels exceeding 240 mg/dL face significantly increased risks of stroke and transient ischemic attacks (TIAs), with dizziness and balance problems often serving as early warning signs of compromised cerebrovascular function. These symptoms become particularly concerning when they occur in combination with other signs of high cholesterol, warranting immediate medical evaluation and comprehensive cardiovascular risk assessment.
8. Digestive Issues and Abdominal Pain - Unexpected Cholesterol Connections

Digestive problems and abdominal pain may indicate that high cholesterol is affecting blood flow to the gastrointestinal system, a condition known as mesenteric ischemia, where reduced circulation to the intestines creates symptoms that are often misattributed to common digestive disorders. The mesenteric arteries, which supply blood to the small and large intestines, can develop cholesterol plaques similar to those found in coronary arteries, leading to compromised blood flow that becomes particularly problematic after eating when digestive organs require increased circulation. This condition typically manifests as cramping abdominal pain that occurs 15-30 minutes after meals and may last for several hours, often accompanied by nausea, bloating, and changes in bowel habits such as diarrhea or constipation. The pain pattern associated with mesenteric ischemia is often described as deep, aching, and centrally located in the abdomen, and may worsen with larger meals as the digestive system's increased metabolic demands outstrip the compromised blood supply. Weight loss may occur as individuals unconsciously begin to eat smaller meals or avoid eating altogether to prevent the uncomfortable symptoms, creating a cycle of malnutrition that can further compromise overall health. Additionally, high cholesterol can affect the liver's ability to produce bile efficiently, leading to digestive difficulties, particularly with fat absorption, which may manifest as pale, fatty stools, bloating after meals, and deficiencies in fat-soluble vitamins. The gallbladder may also be affected, as high cholesterol levels increase the risk of gallstone formation, which can cause severe abdominal pain, particularly in the right upper quadrant, along with nausea and vomiting. Research indicates that mesenteric ischemia, while relatively uncommon, predominantly affects individuals with significant atherosclerotic disease and multiple cardiovascular risk factors, making persistent post-meal abdominal pain an important symptom that warrants evaluation for underlying cholesterol-related vascular disease.
9. Understanding Total Cholesterol Numbers - The Complete Picture

Total cholesterol represents the sum of all cholesterol-containing particles in your blood and serves as the initial screening measure for assessing cardiovascular risk, though understanding what these numbers actually mean requires examining the complete lipid profile rather than focusing solely on this single value. Optimal total cholesterol levels are generally considered to be below 200 mg/dL (5.2 mmol/L), with levels between 200-239 mg/dL classified as borderline high, and values of 240 mg/dL or above indicating high cholesterol that significantly increases cardiovascular disease risk. However, total cholesterol alone provides an incomplete picture because it includes both beneficial high-density lipoprotein (HDL) cholesterol and potentially harmful low-density lipoprotein (LDL) cholesterol, along with very low-density lipoprotein (VLDL) cholesterol, making it possible for someone with high HDL levels to have elevated total cholesterol without increased cardiovascular risk. The measurement reflects cholesterol content in milligrams per deciliter of blood, with normal daily fluctuations of 10-15% being common due to factors such as recent meals, stress levels, illness, and hormonal changes, which is why fasting measurements are typically recommended for accurate assessment. Age, gender, and ethnicity can influence optimal cholesterol ranges, with women generally having higher HDL levels than men, and cholesterol levels naturally increasing with age due to changes in metabolism and hormone production. Genetic factors play a crucial role in determining baseline cholesterol levels, with some individuals having familial hypercholesterolemia, a condition that can cause total cholesterol levels to exceed 300-400 mg/dL despite healthy lifestyle choices. The timing of cholesterol testing is also important, as levels can be temporarily elevated following heart attacks, strokes, or major surgeries, and may be affected by certain medications, making it essential to interpret results in the context of overall health status and risk factors.
10. LDL Cholesterol - The "Bad" Cholesterol Explained

Low-density lipoprotein (LDL) cholesterol, commonly referred to as "bad" cholesterol, represents the primary target for cholesterol management because these particles are directly responsible for transporting cholesterol from the liver to peripheral tissues, where they can become trapped in arterial walls and initiate the atherosclerotic process that leads to cardiovascular disease. Optimal LDL levels are considered to be below 100 mg/dL (2.6 mmol/L) for most individuals, though people with existing cardiovascular disease, diabetes, or multiple risk factors may benefit from even lower targets of less than 70 mg/dL or even below 55 mg/dL in very high-risk patients. LDL levels between 100-129 mg/dL are classified as near optimal, 130-159 mg/dL as borderline high, 160-189 mg/dL as high, and 190 mg/dL or above as very high, with each category representing progressively increased cardiovascular risk that may warrant different treatment approaches. The mechanism by which LDL cholesterol contributes to atherosclerosis involves the oxidation of these particles within arterial walls, triggering inflammatory responses that attract immune cells and promote the formation of foam cells, which eventually develop into the fatty plaques that narrow arteries and increase risk of rupture. Particle size and density also matter, as small, dense LDL particles are considered more atherogenic than larger, more buoyant particles, though standard lipid panels don't typically measure these subtypes, requiring specialized testing for comprehensive assessment. LDL cholesterol levels are