11 Things Your Doctor Wants You to Know About High Blood Pressure
High blood pressure, medically known as hypertension, affects nearly half of all American adults, yet many remain unaware of its presence until serious complications arise. This "silent killer" earned its ominous nickname because it typically develops without obvious symptoms while quietly damaging vital organs throughout the body. Healthcare professionals worldwide consider hypertension one of the most significant preventable risk factors for heart disease, stroke, kidney failure, and premature death. Despite its prevalence and serious consequences, research consistently shows that patients often underestimate the importance of blood pressure management, leading to poor medication adherence and lifestyle modifications. Your doctor wants you to understand that high blood pressure isn't just a number on a medical chart—it's a critical health indicator that requires immediate attention, ongoing monitoring, and comprehensive lifestyle changes. The following eleven essential points represent the most crucial information that healthcare providers wish every patient understood about hypertension, from recognizing early warning signs to implementing effective long-term management strategies that can dramatically improve your quality of life and longevity.
1. Understanding Blood Pressure Numbers - Decoding Your Health's Vital Statistics

Your doctor wants you to understand that blood pressure readings consist of two important numbers that tell a complete story about your cardiovascular health. The systolic pressure (top number) measures the force of blood against artery walls when your heart beats and pumps blood, while the diastolic pressure (bottom number) represents the pressure when your heart rests between beats. Normal blood pressure is defined as less than 120/80 mmHg, while elevated readings fall between 120-129 systolic and less than 80 diastolic. Stage 1 hypertension occurs when systolic pressure ranges from 130-139 or diastolic pressure measures 80-89, and Stage 2 hypertension is diagnosed when systolic pressure reaches 140 or higher, or diastolic pressure exceeds 90. Healthcare providers emphasize that both numbers matter significantly—isolated systolic hypertension (high top number with normal bottom number) is particularly common in older adults and carries substantial health risks. Understanding these classifications helps patients recognize the urgency of their condition and motivates them to take appropriate action. Your doctor monitors trends in these numbers over time rather than focusing on single readings, as blood pressure naturally fluctuates throughout the day based on various factors including stress, physical activity, caffeine consumption, and sleep patterns.
2. The Hidden Dangers - Why High Blood Pressure Silently Destroys Your Body

Medical professionals want patients to comprehend the devastating long-term consequences of uncontrolled hypertension, which systematically damages organs throughout the body without producing noticeable symptoms until irreversible damage occurs. Chronic high blood pressure forces the heart to work harder than normal, leading to left ventricular hypertrophy (enlarged heart muscle), which significantly increases the risk of heart failure, arrhythmias, and sudden cardiac death. The constant pressure damages delicate blood vessel walls, creating microscopic tears that become sites for cholesterol and plaque accumulation, accelerating atherosclerosis and dramatically increasing stroke and heart attack risks. Kidney damage represents another serious consequence, as high pressure destroys the tiny filtering units called nephrons, potentially leading to chronic kidney disease and eventual kidney failure requiring dialysis or transplantation. The eyes also suffer significant damage as hypertension causes retinal blood vessels to narrow, leak, or rupture, potentially resulting in vision loss or blindness. Brain damage occurs through multiple mechanisms, including increased risk of both ischemic and hemorrhagic strokes, vascular dementia, and cognitive decline. Healthcare providers emphasize that these complications develop gradually over years or decades, making prevention and early intervention crucial for maintaining long-term health and preventing disability.
## Section 4: Risk Factors You Can and Cannot Control - Identifying Your Personal Hypertension Profile
Your doctor wants you to understand that high blood pressure develops through a complex interaction of modifiable and non-modifiable risk factors, empowering you to focus your efforts on areas where you can make meaningful changes. Non-modifiable factors include advancing age (blood pressure typically increases after age 45 in men and 65 in women), genetic predisposition (family history significantly increases risk), race (African Americans develop hypertension earlier and more severely), and gender (men face higher risk until women reach menopause). However, numerous modifiable risk factors offer opportunities for prevention and management, including obesity (excess weight forces the heart to pump more blood), physical inactivity (sedentary lifestyle weakens the cardiovascular system), excessive sodium intake (most Americans consume twice the recommended amount), inadequate potassium consumption, chronic stress, smoking, excessive alcohol consumption, and poor sleep quality. Medical conditions such as diabetes, kidney disease, sleep apnea, and thyroid disorders also contribute to hypertension development. Healthcare providers emphasize that even individuals with strong genetic predisposition can significantly reduce their risk through lifestyle modifications, while those with multiple modifiable risk factors may develop hypertension despite having no family history. Understanding your personal risk profile helps your doctor develop targeted prevention strategies and helps you prioritize the most impactful lifestyle changes for your specific situation.
3. The Crucial Role of Regular Monitoring - Why Home Blood Pressure Checks Save Lives

Healthcare professionals strongly advocate for regular blood pressure monitoring both in clinical settings and at home, as this practice provides comprehensive data essential for accurate diagnosis and effective treatment management. White coat hypertension, a phenomenon where blood pressure elevates specifically in medical settings due to anxiety, affects approximately 20% of patients and can lead to unnecessary medication prescriptions if not properly identified through home monitoring. Conversely, masked hypertension occurs when blood pressure appears normal in the doctor's office but remains elevated during daily activities, affecting roughly 15% of individuals and significantly increasing cardiovascular risk if undetected. Home blood pressure monitoring allows healthcare providers to identify these patterns while providing valuable information about how blood pressure responds to medications, lifestyle changes, and daily stressors. Your doctor wants you to understand proper monitoring techniques, including using a validated, properly-sized cuff, sitting quietly for five minutes before measurement, avoiding caffeine and exercise for 30 minutes prior, and taking multiple readings at consistent times. The American Heart Association recommends taking readings twice daily for one week each month, recording the results for review during medical appointments. This data helps physicians make informed decisions about medication adjustments, identify treatment resistance, and monitor progress toward blood pressure goals, ultimately leading to better outcomes and reduced cardiovascular risk.
## Section 6: Medication Myths and Realities - Separating Facts from Fiction About Blood Pressure Drugs
Your doctor wants to dispel common misconceptions about blood pressure medications that often prevent patients from achieving optimal control and maintaining long-term cardiovascular health. Many patients believe that feeling fine means they can skip medications, but hypertension rarely causes symptoms until serious complications develop, making consistent medication adherence crucial regardless of how you feel. Another prevalent myth suggests that natural remedies alone can replace prescription medications for moderate to severe hypertension, while research demonstrates that lifestyle changes, though beneficial, typically cannot achieve adequate blood pressure reduction in patients requiring pharmacological intervention. Some individuals fear medication dependency, not understanding that blood pressure medications don't cure hypertension but rather manage it effectively, similar to how insulin manages diabetes. Healthcare providers emphasize that modern blood pressure medications are generally well-tolerated, with side effects often diminishing as the body adjusts, and alternative medications are available if initial choices cause problems. The concern about medications masking underlying problems is unfounded, as hypertension itself is the underlying problem requiring treatment to prevent organ damage. Your doctor wants you to understand that medication effectiveness requires time—typically 2-4 weeks to see full effects—and that combination therapy using multiple medications with different mechanisms often provides better control with fewer side effects than single high-dose medications. Open communication about concerns, side effects, and cost issues enables healthcare providers to optimize treatment regimens for individual patient needs.
## Section 7: Dietary Strategies That Actually Work - Evidence-Based Nutrition for Blood Pressure Control
Medical professionals want patients to understand that dietary modifications can significantly impact blood pressure control, with some nutritional interventions proving as effective as medications for mild to moderate hypertension. The DASH (Dietary Approaches to Stop Hypertension) eating plan, extensively researched and endorsed by major medical organizations, emphasizes fruits, vegetables, whole grains, lean proteins, and low-fat dairy while limiting sodium, saturated fats, and added sugars. This approach can reduce systolic blood pressure by 8-14 mmHg, comparable to the effect of a single blood pressure medication. Sodium reduction represents the most critical dietary intervention, as the average American consumes 3,400 mg daily while the recommended limit is 2,300 mg (ideally 1,500 mg for those with hypertension). Your doctor wants you to know that 75% of dietary sodium comes from processed and restaurant foods rather than table salt, making label reading and home cooking essential skills. Potassium-rich foods like bananas, oranges, spinach, and beans help counteract sodium's effects by promoting sodium excretion and relaxing blood vessel walls. Limiting alcohol consumption is crucial, as moderate drinking may slightly lower blood pressure, but excessive consumption (more than two drinks daily for men, one for women) significantly raises blood pressure and interferes with medication effectiveness. Healthcare providers emphasize that dietary changes require patience and persistence, as blood pressure improvements typically become apparent after 2-4 weeks of consistent adherence to heart-healthy eating patterns.
4. Exercise as Medicine - The Prescription Your Heart Needs Most
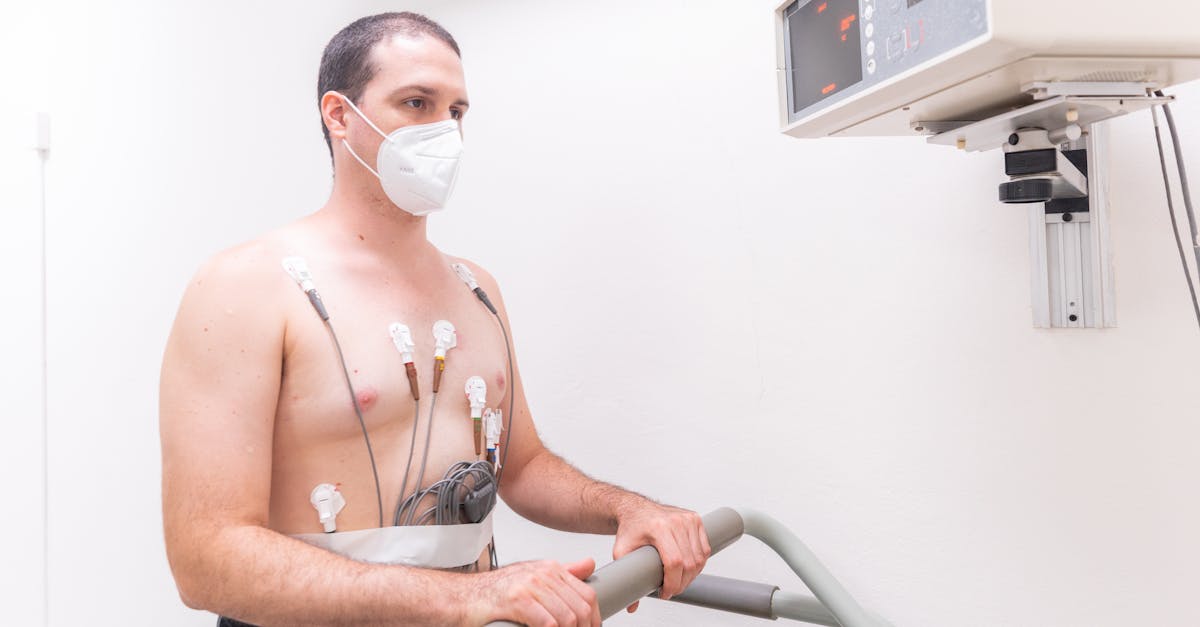
Your doctor wants you to understand that regular physical activity serves as one of the most powerful non-pharmacological treatments for high blood pressure, with effects comparable to many medications when implemented consistently. Aerobic exercise, including brisk walking, swimming, cycling, or dancing, can reduce systolic blood pressure by 4-9 mmHg and diastolic pressure by 3-5 mmHg when performed for 30 minutes most days of the week. The blood pressure-lowering effects of exercise result from multiple physiological mechanisms, including improved heart efficiency (allowing it to pump more blood with less effort), enhanced blood vessel flexibility, reduced arterial stiffness, and decreased sympathetic nervous system activity. Resistance training, when performed 2-3 times weekly using moderate weights and higher repetitions, provides additional cardiovascular benefits and helps maintain muscle mass, which becomes increasingly important with aging. Healthcare providers emphasize that exercise benefits begin with modest activity increases—even 10-minute walks three times daily can provide meaningful blood pressure reductions for sedentary individuals. Your doctor wants you to know that exercise effects on blood pressure are both acute (lasting 12-24 hours after activity) and chronic (developing over weeks to months of regular activity), making consistency more important than intensity. For patients with very high blood pressure or existing cardiovascular disease, medical clearance and gradual progression under professional guidance ensure safety while maximizing benefits. The key is finding enjoyable activities that can be sustained long-term, as the blood pressure benefits of exercise disappear within 2-4 weeks of stopping regular activity.
5. Stress Management - Addressing the Often Overlooked Blood Pressure Factor

Medical professionals want patients to recognize chronic stress as a significant contributor to high blood pressure that requires active management strategies for optimal cardiovascular health. Acute stress triggers the release of hormones like adrenaline and cortisol, causing temporary blood pressure spikes, but chronic stress maintains elevated hormone levels that can lead to sustained hypertension through multiple pathways including increased heart rate, blood vessel constriction, and sodium retention. Research demonstrates that individuals experiencing chronic work stress, relationship conflicts, financial pressures, or caregiving responsibilities face significantly higher risks of developing hypertension and experiencing cardiovascular events. Your doctor wants you to understand that stress management isn't just about relaxation—it involves developing practical coping strategies, improving time management, setting realistic expectations, and building strong social support networks. Proven stress-reduction techniques include deep breathing exercises, progressive muscle relaxation, meditation, yoga, tai chi, and regular participation in enjoyable hobbies or social activities. Sleep quality plays a crucial role in stress management and blood pressure control, as chronic sleep deprivation (less than 6-7 hours nightly) increases stress hormones and directly elevates blood pressure. Healthcare providers emphasize that stress management requires individualized approaches, as techniques that work for one person may not be effective for another. Professional counseling or stress management programs may be necessary for individuals dealing with severe chronic stress, depression, or anxiety disorders that significantly impact blood pressure control.
6. Sleep Quality and Blood Pressure - The Vital Connection You Cannot Ignore

Your doctor wants you to understand the profound relationship between sleep quality and blood pressure regulation, as sleep disorders and poor sleep habits significantly contribute to hypertension development and treatment resistance. During normal sleep, blood pressure naturally decreases by 10-20% (called "dipping"), allowing the cardiovascular system to recover from daily stresses, but this protective mechanism is disrupted in individuals with sleep disorders or poor sleep hygiene. Sleep apnea, affecting an estimated 25% of men and 10% of women, causes repeated breathing interruptions that trigger stress hormone release and blood pressure spikes throughout the night, leading to sustained daytime hypertension that often proves resistant to standard treatments. Chronic sleep deprivation (consistently sleeping less than 6-7 hours nightly) disrupts hormonal balance, increases sympathetic nervous system activity, and promotes inflammation, all contributing to elevated blood pressure and increased cardiovascular risk. Healthcare providers emphasize that sleep quality matters as much as sleep duration—frequent awakenings, difficulty falling asleep, or non-restorative sleep can impact blood pressure even when total sleep time appears adequate. Your doctor wants you to practice good sleep hygiene, including maintaining consistent bedtimes and wake times, creating a cool, dark, quiet sleep environment, avoiding caffeine and large meals before bedtime, limiting screen time in the evening, and establishing relaxing bedtime routines. If you experience loud snoring, witnessed breathing pauses, excessive daytime sleepiness, or morning headaches, sleep apnea evaluation may be necessary, as treating sleep disorders often leads to significant blood pressure improvements and enhanced medication effectiveness.
## Section 11: Weight Management - Understanding the Direct Link Between Body Weight and Blood Pressure
Medical professionals want patients to comprehend the strong correlation between body weight and blood pressure, as even modest weight loss can produce clinically significant improvements in cardiovascular health. Research consistently demonstrates that each kilogram (2.2 pounds) of weight loss typically reduces systolic blood pressure by 1-2 mmHg and diastolic pressure by 1 mmHg, making weight management one of the most effective non-pharmacological interventions for hypertension. Excess weight contributes to high blood pressure through multiple mechanisms, including increased blood volume (requiring the heart to pump harder), enhanced sympathetic nervous system activity, insulin resistance, inflammation, and sleep-disordered breathing. Abdominal obesity proves particularly problematic, as visceral fat produces hormones and inflammatory substances that directly impact blood vessel function and blood pressure regulation. Your doctor wants you to understand that sustainable weight loss requires gradual changes rather than extreme diets—losing 1-2 pounds weekly through a combination of reduced calorie intake and increased physical activity provides the best long-term results. Even a 5-10% reduction in body weight can produce meaningful blood pressure improvements and reduce the need for medications in some patients. Healthcare providers emphasize that weight management strategies should focus on overall health rather than just the number on the scale, incorporating nutrient-dense foods, regular physical activity, adequate sleep, and stress management. For individuals with significant obesity (BMI >35) and multiple cardiovascular risk factors, medical weight loss programs or bariatric surgery may be appropriate options that can dramatically improve blood pressure control and overall health outcomes.
7. When to Seek Emergency Care - Recognizing Hypertensive Crisis Warning Signs

Your doctor wants you to recognize the signs of hypertensive crisis, a medical emergency requiring immediate intervention to prevent life-threatening complications such as stroke, heart attack, kidney failure, or organ damage. Hypertensive crisis occurs when blood pressure rises rapidly to extremely high levels (typically systolic pressure >180 mmHg or diastolic pressure >120 mmHg) and is classified into two categories: hypertensive urgency (very high blood pressure without organ damage) and hypertensive emergency (very high blood pressure with evidence of organ damage). Warning signs that require immediate emergency room evaluation include severe headache, chest pain, shortness of breath, visual changes or vision loss, confusion, difficulty speaking, weakness or numbness in arms or legs, nausea and vomiting, seizures, or loss of consciousness. Healthcare providers emphasize that hypertensive crisis can occur in patients with previously well-controlled blood pressure due to medication non-adherence, drug interactions, underlying medical conditions, or substance use. Your doctor wants you to understand that extremely high blood pressure readings alone may not constitute an emergency if you feel well and have no symptoms, but you should contact your healthcare provider immediately for guidance rather than attempting to self-treat. Never abruptly stop blood pressure medications without medical supervision, as rebound hypertension can trigger crisis situations. If you experience any concerning symptoms with elevated blood pressure, call 911 rather than driving yourself to the hospital, as your condition could deteriorate rapidly during transport. Emergency treatment focuses on gradually reducing blood pressure over hours to days rather than minutes to prevent dangerous drops that could compromise blood flow to vital organs.
## Section 13: Building Your Long-Term Management Plan - Creating Sustainable Success with Your Healthcare Team
Medical professionals want patients to understand that successful blood pressure management requires a comprehensive, long-term approach involving collaboration between patients, healthcare providers, and often family members or support systems. Your doctor wants you to view hypertension management as a lifelong commitment rather than a short-term fix, requiring regular monitoring, medication adjustments, lifestyle modifications, and ongoing education about your condition. Effective management plans typically include specific blood pressure targets (usually <130/80 mmHg for most adults), medication regimens tailored to individual needs and tolerances, structured lifestyle modification goals, regular follow-up schedules, and clear communication protocols for questions or concerns. Healthcare providers emphasize the importance of medication adherence, recommending strategies such as pill organizers, smartphone reminders, pharmacy synchronization programs, and honest discussions about cost concerns or side effects that might interfere with compliance. Your doctor wants you to maintain detailed records of home blood pressure readings, medication timing, side effects, and lifestyle factors that might influence your readings, as this information guides treatment decisions and helps identify patterns or problems. Regular follow-up appointments allow for medication adjustments, monitoring for complications, assessment of lifestyle modification