12 Lifestyle Changes That Can Help Support Heart Health
Heart disease remains the leading cause of death globally, claiming millions of lives annually and affecting countless more through reduced quality of life and increased healthcare burdens. However, emerging research consistently demonstrates that up to 80% of premature heart disease cases are preventable through strategic lifestyle modifications. The human cardiovascular system, while remarkably resilient, responds dramatically to the choices we make daily—from the foods we consume and the activities we pursue to how we manage stress and prioritize sleep. This comprehensive exploration delves into twelve evidence-based lifestyle changes that can significantly enhance heart health, reduce cardiovascular risk factors, and promote longevity. Each modification represents a powerful tool in building a robust defense against heart disease, supported by decades of clinical research and real-world outcomes. By understanding and implementing these changes systematically, individuals can take control of their cardiovascular destiny, transforming their health trajectory through informed, purposeful action that extends far beyond simple dietary adjustments or exercise routines.
1. Embracing a Heart-Healthy Mediterranean Diet

The Mediterranean diet stands as one of the most extensively researched and scientifically validated nutritional approaches for cardiovascular protection, with studies spanning over five decades demonstrating its profound impact on heart health outcomes. This eating pattern, inspired by the traditional dietary habits of countries bordering the Mediterranean Sea, emphasizes whole foods, healthy fats, and nutrient-dense ingredients that work synergistically to reduce inflammation, improve cholesterol profiles, and enhance overall cardiovascular function. The diet's foundation rests on abundant consumption of fruits, vegetables, whole grains, legumes, nuts, and seeds, while featuring olive oil as the primary fat source and including moderate amounts of fish, poultry, and dairy products. Research published in the New England Journal of Medicine found that individuals following a Mediterranean diet supplemented with extra virgin olive oil or nuts experienced a 30% reduction in major cardiovascular events compared to those on a low-fat diet. The anti-inflammatory compounds found in Mediterranean foods, including polyphenols, omega-3 fatty acids, and antioxidants, work collectively to protect arterial walls, reduce oxidative stress, and maintain healthy blood pressure levels, making this dietary approach a cornerstone of cardiovascular disease prevention.
2. Incorporating Regular Aerobic Exercise

Aerobic exercise serves as a fundamental pillar of cardiovascular health, functioning as both a preventive measure and therapeutic intervention that strengthens the heart muscle, improves circulation, and enhances the body's overall efficiency in oxygen utilization. The American Heart Association recommends at least 150 minutes of moderate-intensity aerobic activity or 75 minutes of vigorous-intensity exercise weekly, guidelines supported by extensive research demonstrating significant reductions in heart disease risk among physically active individuals. Regular aerobic exercise triggers numerous physiological adaptations that benefit cardiovascular health, including increased stroke volume, improved cardiac output, enhanced endothelial function, and better blood pressure regulation. Activities such as brisk walking, cycling, swimming, dancing, and jogging not only strengthen the heart muscle but also promote the development of collateral circulation, creating alternative pathways for blood flow that can prove crucial during cardiovascular events. Studies have shown that even modest increases in physical activity can yield substantial benefits, with sedentary individuals experiencing the greatest relative improvements in cardiovascular risk reduction. The exercise-induced release of nitric oxide improves arterial flexibility and reduces inflammation, while regular physical activity helps maintain healthy cholesterol levels, supports weight management, and enhances insulin sensitivity, creating a comprehensive cardiovascular protection profile.
3. Managing Stress Through Mindfulness and Relaxation Techniques

Chronic stress represents a significant yet often underestimated risk factor for cardiovascular disease, triggering a cascade of physiological responses that can damage the heart and blood vessels over time through elevated cortisol levels, increased inflammation, and disrupted autonomic nervous system function. The body's stress response, while designed for short-term survival situations, becomes harmful when persistently activated by modern life's constant pressures, leading to elevated blood pressure, increased heart rate, and heightened risk of arrhythmias. Mindfulness-based stress reduction techniques, including meditation, deep breathing exercises, progressive muscle relaxation, and yoga, have demonstrated remarkable efficacy in mitigating these harmful effects while promoting cardiovascular resilience. Research published in the Journal of the American Heart Association found that individuals practicing transcendental meditation experienced significant reductions in blood pressure, decreased risk of heart attack and stroke, and improved overall cardiovascular outcomes compared to control groups. These practices work by activating the parasympathetic nervous system, promoting relaxation responses that counteract stress-induced cardiovascular damage while improving heart rate variability, reducing inflammatory markers, and enhancing emotional regulation. Regular stress management practice also supports better sleep quality, improved decision-making regarding health behaviors, and enhanced overall quality of life, creating a positive feedback loop that reinforces cardiovascular wellness.
4. Prioritizing Quality Sleep for Heart Recovery

Sleep quality and duration play crucial roles in cardiovascular health, with inadequate or poor-quality sleep serving as an independent risk factor for heart disease, hypertension, and stroke through complex mechanisms involving hormonal regulation, inflammatory processes, and autonomic nervous system function. During sleep, the cardiovascular system undergoes essential recovery processes, including blood pressure reduction, heart rate normalization, and cellular repair mechanisms that maintain arterial health and cardiac function. Adults require 7-9 hours of quality sleep nightly for optimal cardiovascular protection, yet millions struggle with sleep disorders or insufficient rest due to lifestyle factors, stress, or underlying health conditions. Sleep deprivation disrupts the delicate balance of hormones that regulate appetite, stress response, and inflammation, leading to increased cortisol levels, elevated blood pressure, and heightened risk of developing diabetes and obesity—all significant cardiovascular risk factors. Research demonstrates that individuals sleeping less than six hours nightly face a 48% increased risk of developing heart disease compared to those achieving adequate rest. Implementing good sleep hygiene practices, including maintaining consistent sleep schedules, creating optimal sleep environments, limiting screen time before bed, and addressing underlying sleep disorders like sleep apnea, can significantly improve cardiovascular outcomes while enhancing overall health and well-being.
5. Eliminating Tobacco Use and Avoiding Secondhand Smoke
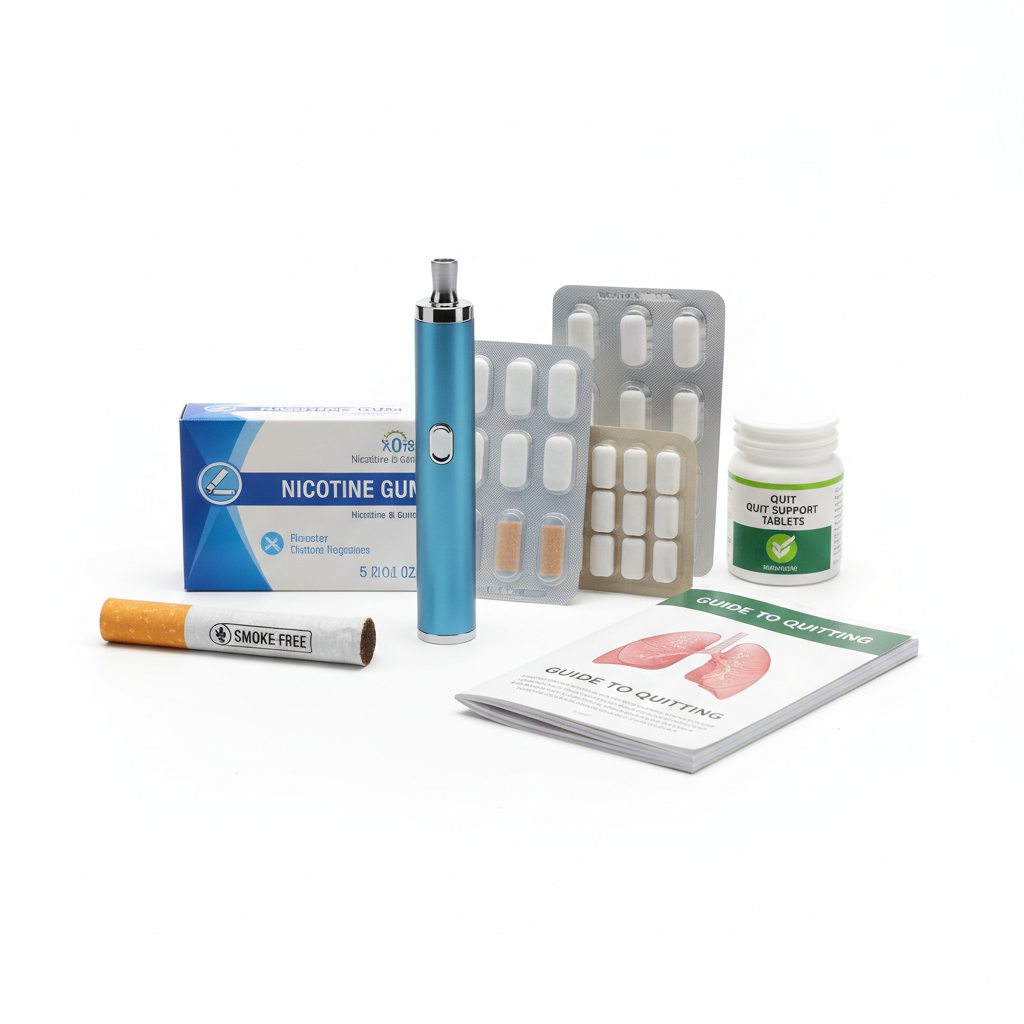
Tobacco use represents one of the most preventable and devastating risk factors for cardiovascular disease, with smoking dramatically accelerating atherosclerosis, increasing blood clot formation, and damaging the delicate endothelial lining of blood vessels through toxic chemical exposure and oxidative stress. The cardiovascular benefits of smoking cessation begin almost immediately, with heart rate and blood pressure dropping within 20 minutes of the last cigarette, carbon monoxide levels normalizing within 12 hours, and circulation improving within weeks of quitting. Cigarette smoke contains over 7,000 chemicals, including numerous carcinogens and toxins that directly damage cardiovascular tissues, promote inflammation, reduce oxygen-carrying capacity of blood, and increase the risk of dangerous blood clots. Even exposure to secondhand smoke significantly elevates cardiovascular risk, with non-smokers exposed to environmental tobacco smoke facing a 25-30% increased risk of heart disease. The nicotine in tobacco products causes immediate vasoconstriction, reducing blood flow to vital organs while increasing heart rate and blood pressure, creating additional strain on an already compromised cardiovascular system. Comprehensive smoking cessation programs that combine behavioral support, nicotine replacement therapy, and sometimes prescription medications have proven highly effective in helping individuals overcome tobacco addiction while dramatically reducing their cardiovascular risk profile within months of quitting.
6. Maintaining Healthy Weight Through Balanced Nutrition

Maintaining a healthy weight represents a cornerstone of cardiovascular disease prevention, as excess body weight, particularly abdominal obesity, significantly increases the risk of developing hypertension, diabetes, dyslipidemia, and metabolic syndrome—all major contributors to heart disease. The relationship between weight and cardiovascular health extends beyond simple aesthetics, involving complex metabolic processes that affect insulin sensitivity, inflammatory markers, and hormonal balance throughout the body. Excess adipose tissue, especially visceral fat surrounding internal organs, functions as an active endocrine organ that secretes inflammatory cytokines and hormones that promote insulin resistance, elevate blood pressure, and contribute to arterial damage. Research indicates that even modest weight loss of 5-10% of body weight can yield significant cardiovascular benefits, including improved blood pressure, better cholesterol profiles, enhanced insulin sensitivity, and reduced inflammation markers. Sustainable weight management requires a comprehensive approach that combines caloric awareness with nutrient density, emphasizing whole foods, appropriate portion sizes, and consistent eating patterns that support metabolic health. The most effective weight management strategies focus on creating sustainable lifestyle changes rather than restrictive dieting, incorporating regular physical activity, stress management, and behavioral modifications that address the underlying factors contributing to weight gain while promoting long-term cardiovascular wellness.
7. Limiting Alcohol Consumption for Optimal Heart Function

While moderate alcohol consumption has been associated with certain cardiovascular benefits in some populations, excessive drinking poses significant risks to heart health through multiple mechanisms including direct cardiac toxicity, elevated blood pressure, increased triglyceride levels, and heightened risk of arrhythmias and cardiomyopathy. The relationship between alcohol and cardiovascular health follows a complex J-shaped curve, where moderate consumption may offer some protective effects for certain individuals, but these potential benefits are quickly overshadowed by the substantial risks associated with heavy or binge drinking patterns. Alcohol's impact on the cardiovascular system includes immediate effects such as increased heart rate and blood pressure, as well as long-term consequences including weakening of the heart muscle, irregular heartbeats, and increased risk of stroke and sudden cardiac death. Current guidelines suggest that if individuals choose to drink alcohol, consumption should be limited to no more than one drink per day for women and two drinks per day for men, with several alcohol-free days each week to allow the body to recover. However, for individuals with existing cardiovascular conditions, family history of heart disease, or other risk factors, complete abstinence may be the safest approach. The calories in alcoholic beverages also contribute to weight gain and metabolic dysfunction, while alcohol can interfere with sleep quality and stress management, creating additional cardiovascular risk factors that compound the direct effects on heart health.
8. Monitoring and Managing Blood Pressure Regularly
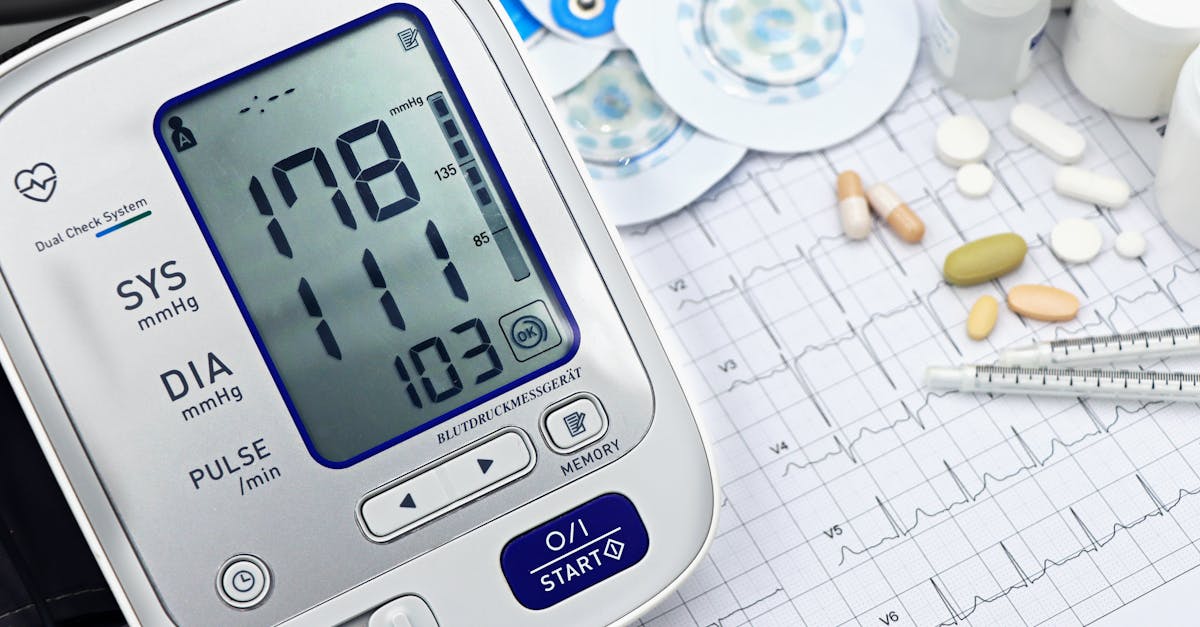
Blood pressure monitoring and management represent critical components of cardiovascular health maintenance, as hypertension often develops silently over years while causing progressive damage to arteries, heart, kidneys, and other vital organs throughout the body. High blood pressure, affecting nearly half of all adults, forces the heart to work harder to pump blood through narrowed or stiffened arteries, leading to left ventricular hypertrophy, increased risk of heart failure, and accelerated atherosclerosis. Regular blood pressure monitoring, both at home and during healthcare visits, enables early detection of hypertension and allows for timely intervention before irreversible cardiovascular damage occurs. Optimal blood pressure levels (less than 120/80 mmHg) can be achieved and maintained through comprehensive lifestyle modifications including dietary changes, regular exercise, stress management, adequate sleep, and weight control, often reducing or eliminating the need for medication. The DASH (Dietary Approaches to Stop Hypertension) eating plan, which emphasizes fruits, vegetables, whole grains, lean proteins, and low-fat dairy while limiting sodium, saturated fats, and added sugars, has demonstrated remarkable efficacy in lowering blood pressure naturally. Home blood pressure monitoring using validated devices enables individuals to track their progress, identify patterns related to lifestyle factors, and work collaboratively with healthcare providers to optimize treatment strategies while maintaining awareness of their cardiovascular risk status.
9. Controlling Cholesterol Through Diet and Lifestyle

Cholesterol management represents a fundamental aspect of cardiovascular disease prevention, requiring a comprehensive understanding of how different types of cholesterol and lipoproteins affect arterial health and overall cardiovascular risk profiles. Low-density lipoprotein (LDL) cholesterol, often termed "bad" cholesterol, contributes to atherosclerotic plaque formation when oxidized and deposited in arterial walls, while high-density lipoprotein (HDL) cholesterol helps transport cholesterol away from arteries to the liver for processing and elimination. Dietary strategies for cholesterol management focus on reducing saturated and trans fats while increasing consumption of soluble fiber, plant sterols, and omega-3 fatty acids that naturally lower LDL cholesterol levels and improve overall lipid profiles. Foods particularly effective for cholesterol management include oats, barley, beans, lentils, nuts, fatty fish, and plant-based proteins that provide essential nutrients while supporting healthy cholesterol metabolism. Regular physical activity enhances cholesterol management by increasing HDL levels, improving LDL particle size and density, and enhancing the body's ability to metabolize fats effectively. The Mediterranean diet pattern, rich in monounsaturated fats from olive oil and nuts, has demonstrated superior cholesterol-lowering effects compared to low-fat diets while providing additional cardiovascular benefits through anti-inflammatory compounds and antioxidants that protect against oxidative damage to cholesterol particles.
10. Building Strength Through Resistance Training

Resistance training, often overlooked in cardiovascular health discussions, provides unique and complementary benefits to aerobic exercise by strengthening skeletal muscles, improving metabolic function, and enhancing overall cardiovascular efficiency through mechanisms that extend far beyond traditional cardio activities. Strength training exercises, including weightlifting, resistance band workouts, and bodyweight exercises, promote cardiovascular health by improving insulin sensitivity, reducing blood pressure, enhancing lipid profiles, and supporting healthy weight management through increased muscle mass and metabolic rate. The American Heart Association recommends at least two sessions of moderate to high-intensity resistance training weekly, targeting all major muscle groups to maximize cardiovascular and overall health benefits. Research demonstrates that individuals who combine aerobic exercise with regular strength training experience greater reductions in cardiovascular risk factors compared to those engaging in either activity alone, highlighting the synergistic effects of comprehensive fitness programs. Resistance training improves cardiac function by enhancing venous return, reducing resting heart rate, and improving the heart's ability to pump blood efficiently during both rest and physical activity. Additionally, strength training helps maintain muscle mass during aging, preventing sarcopenia and maintaining functional capacity that supports continued physical activity and cardiovascular health throughout the lifespan while reducing the risk of falls and maintaining independence in older adults.
11. Staying Hydrated for Optimal Circulation

Proper hydration plays a crucial yet often underappreciated role in cardiovascular health, affecting blood volume, viscosity, and circulation while supporting the heart's ability to pump blood efficiently throughout the body's extensive vascular network. Adequate fluid intake maintains optimal blood volume and consistency, preventing the blood from becoming too thick or viscous, which would force the heart to work harder to circulate blood to vital organs and tissues. Dehydration, even in mild forms, can lead to increased heart rate, elevated blood pressure, and reduced cardiac output as the cardiovascular system struggles to maintain adequate circulation with diminished blood volume. The general recommendation of 8-10 glasses of water daily provides a baseline, but individual needs vary based on activity level, climate, body size, and overall health status, with active individuals and those in hot climates requiring significantly more fluid intake. Quality hydration involves not just water consumption but also maintaining proper electrolyte balance through foods rich in potassium, magnesium, and sodium in appropriate ratios that support optimal cellular function and blood pressure regulation. Chronic dehydration contributes to increased blood viscosity, elevated risk of blood clots, and additional strain on the cardiovascular system, while proper hydration supports kidney function, helps regulate body temperature, and maintains the delicate fluid balance necessary for optimal cardiovascular performance and overall health.
12. Managing Blood Sugar for Cardiovascular Protection
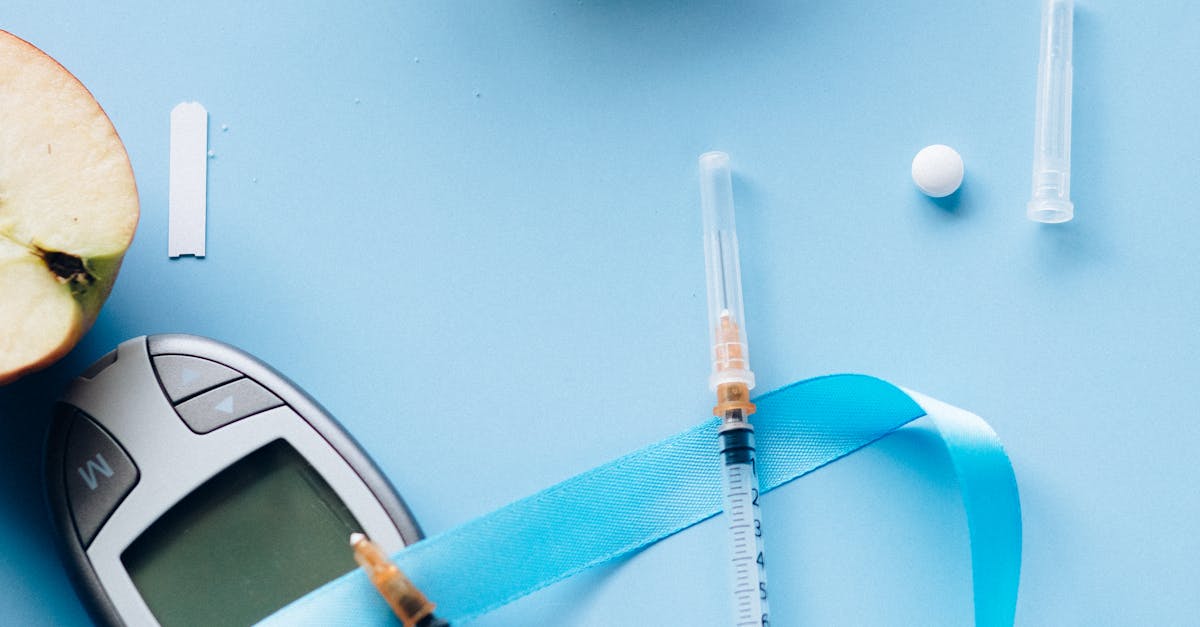
Blood sugar management represents a critical component of cardiovascular health, as diabetes and prediabetes significantly increase the risk of heart disease, stroke, and peripheral vascular disease through multiple pathways involving inflammation, oxidative stress, and accelerated atherosclerosis. Elevated blood glucose levels damage blood vessel walls, promote the formation of advanced glycation end products that stiffen arteries, and create an inflammatory environment that accelerates cardiovascular disease progression. Individuals with diabetes face a two to four times higher risk of developing cardiovascular disease compared to those with normal blood sugar levels, making glucose control a top priority for heart health protection. Effective blood sugar management involves maintaining consistent eating patterns, choosing foods with low glycemic impact, incorporating regular physical activity, and monitoring blood glucose levels to understand how different foods and activities affect individual glucose responses. The hemoglobin A1C test, which reflects average blood sugar levels over the previous three months, should ideally remain below 7% for most adults with diabetes, though individual targets may vary based on age, health status, and other factors. Lifestyle interventions including weight management, regular exercise, stress reduction, and dietary modifications focusing on whole foods, fiber-rich carbohydrates, and balanced meals can significantly improve blood sugar control while providing additional cardiovascular benefits through improved insulin sensitivity and reduced inflammation.
13. Integrating Heart-Healthy Changes for Lifelong Wellness
The journey toward optimal cardiovascular health requires a comprehensive, integrated approach that recognizes the interconnected nature of lifestyle factors and their cumulative impact on heart disease risk and overall wellness. These twelve evidence-based lifestyle modifications work synergistically to create a powerful defense against cardiovascular disease, with each change reinforcing and amplifying the benefits of others to produce outcomes greater than the sum of individual interventions. Success in implementing these changes lies not in perfection but in consistent progress, recognizing that even small improvements in multiple areas can yield significant cardiovascular benefits over time. The most effective approach involves gradual implementation, focusing on one or two changes initially while building sustainable habits that become integrated into daily life rather than temporary modifications that are difficult to maintain long-term. Regular monitoring of key cardiovascular risk factors, including blood pressure, cholesterol levels, blood sugar, and body weight, provides valuable feedback on progress while enabling timely adjustments to lifestyle strategies. Healthcare providers play crucial roles in supporting these lifestyle changes, offering personalized guidance, monitoring progress, and providing medical interventions when necessary to optimize cardiovascular outcomes. By embracing these twelve lifestyle modifications as interconnected components of a comprehensive cardiovascular wellness strategy, individuals can significantly reduce their risk of heart disease while enhancing their overall quality of life, energy levels, and longevity, creating a foundation for vibrant health that extends far beyond cardiovascular benefits alone.