9 Common Risk Factors for Heart Disease That Are Within Your Control
Heart disease remains the leading cause of death globally, claiming millions of lives annually and affecting countless families worldwide. While genetics and age play undeniable roles in cardiovascular health, the empowering truth is that many of the most significant risk factors for heart disease are entirely within your control. Research consistently demonstrates that lifestyle modifications can reduce heart disease risk by up to 80%, making prevention not just possible but highly effective. The nine controllable risk factors we'll explore—including diet, physical activity, smoking, stress management, sleep quality, weight maintenance, alcohol consumption, blood pressure monitoring, and cholesterol management—represent powerful tools in your arsenal against cardiovascular disease. Understanding these factors and implementing targeted strategies to address them can dramatically transform your heart health trajectory. This comprehensive exploration will provide you with evidence-based insights and practical approaches to take charge of your cardiovascular wellness, potentially adding years to your life while significantly improving your quality of life along the way.
1. Poor Dietary Choices - The Foundation of Heart Health

Your dietary choices serve as the cornerstone of cardiovascular health, with research consistently showing that what you eat directly impacts your heart's well-being. The Western diet, characterized by high consumption of processed foods, saturated fats, trans fats, excessive sodium, and refined sugars, creates a perfect storm for heart disease development. Studies published in the Journal of the American College of Cardiology demonstrate that individuals following heart-healthy eating patterns, such as the Mediterranean diet, experience up to 30% reduction in cardiovascular events. The mechanism behind this protection involves multiple pathways: healthy fats from sources like olive oil and nuts help reduce inflammation, while fiber-rich foods lower cholesterol levels and stabilize blood sugar. Conversely, processed foods trigger inflammatory responses and contribute to arterial plaque buildup. The good news is that dietary changes can yield rapid results—improvements in cholesterol levels and blood pressure can be observed within weeks of adopting healthier eating patterns. Focusing on whole foods, lean proteins, colorful vegetables, fruits, whole grains, and healthy fats while minimizing processed foods, excessive salt, and added sugars creates a powerful foundation for long-term heart health.
2. Sedentary Lifestyle - Moving Toward Better Heart Health

Physical inactivity stands as one of the most modifiable yet overlooked risk factors for heart disease, with sedentary behavior contributing to approximately 35% of coronary heart disease deaths. The human cardiovascular system is designed for movement, and when we remain inactive, our heart muscle weakens, blood circulation becomes sluggish, and metabolic processes become inefficient. Research from the American Heart Association reveals that just 150 minutes of moderate-intensity exercise per week—equivalent to a brisk 30-minute walk five days weekly—can reduce heart disease risk by 35%. Regular physical activity strengthens the heart muscle, improves blood flow, helps maintain healthy blood pressure, increases HDL (good) cholesterol while lowering LDL (bad) cholesterol, and enhances the body's ability to use insulin effectively. The benefits extend beyond the cardiovascular system, as exercise also helps manage weight, reduces stress hormones, and improves sleep quality—all additional factors that support heart health. The beauty of this risk factor lies in its accessibility; you don't need expensive equipment or gym memberships to make a difference. Simple activities like taking stairs instead of elevators, parking farther away, gardening, dancing, or playing with children can accumulate meaningful health benefits when performed consistently.
3. Tobacco Use - Breaking Free from a Major Heart Threat

Smoking represents one of the most devastating yet completely preventable risk factors for heart disease, with tobacco use increasing the risk of coronary heart disease by 2-4 times compared to non-smokers. The toxic chemicals in tobacco smoke—over 7,000 compounds, including at least 70 known carcinogens—wreak havoc on the cardiovascular system through multiple mechanisms. Nicotine increases heart rate and blood pressure, while carbon monoxide reduces the blood's oxygen-carrying capacity, forcing the heart to work harder. Additionally, smoking damages the inner lining of arteries, promotes blood clot formation, reduces HDL cholesterol, and accelerates the development of atherosclerosis. The encouraging news is that the cardiovascular benefits of quitting smoking begin almost immediately: within 20 minutes, heart rate and blood pressure drop; within 12 hours, carbon monoxide levels normalize; within one year, the risk of heart disease is cut in half; and within 15 years, the risk approaches that of someone who never smoked. This dramatic recovery timeline underscores the remarkable ability of the cardiovascular system to heal when given the opportunity. Modern smoking cessation tools, including nicotine replacement therapy, prescription medications, behavioral counseling, and support groups, have made quitting more achievable than ever before, offering hope and practical pathways to freedom from tobacco dependence.
4. Chronic Stress - Managing the Silent Heart Killer

Chronic stress acts as a silent but potent contributor to heart disease, with prolonged exposure to stress hormones creating a cascade of cardiovascular damage that many people underestimate. When faced with stressful situations, the body releases cortisol and adrenaline, which temporarily increase heart rate, blood pressure, and blood sugar levels—responses that are beneficial in short bursts but destructive when sustained over time. Research published in The Lancet demonstrates that chronic stress increases heart disease risk by up to 27%, with the mechanism involving persistent inflammation, elevated blood pressure, disrupted sleep patterns, and often leading to unhealthy coping behaviors like overeating, smoking, or excessive alcohol consumption. The modern lifestyle, with its constant connectivity, work pressures, financial concerns, and social obligations, creates an environment where many people exist in a state of chronic stress activation. However, stress management is entirely within your control through evidence-based techniques such as regular meditation, deep breathing exercises, yoga, progressive muscle relaxation, and mindfulness practices. Additionally, maintaining strong social connections, setting healthy boundaries, engaging in hobbies, spending time in nature, and seeking professional counseling when needed can significantly reduce stress levels. The key lies in recognizing stress as a serious health threat and actively implementing strategies to manage it before it takes a toll on your cardiovascular system.
5. Poor Sleep Quality - The Overlooked Heart Health Factor

Sleep quality and duration play crucial roles in cardiovascular health, yet sleep disorders and poor sleep hygiene remain underappreciated risk factors for heart disease. Research consistently shows that both insufficient sleep (less than 6 hours per night) and excessive sleep (more than 9 hours per night) are associated with increased heart disease risk, with the optimal range being 7-8 hours of quality sleep nightly. During sleep, the cardiovascular system undergoes essential repair processes: blood pressure naturally decreases, heart rate slows, and inflammatory markers are reduced. Poor sleep disrupts these restorative processes and triggers a cascade of harmful effects including elevated stress hormones, increased inflammation, insulin resistance, weight gain, and elevated blood pressure. Sleep apnea, a condition affecting millions worldwide, creates particularly severe cardiovascular stress through repeated episodes of oxygen deprivation and sleep fragmentation. The good news is that sleep quality is highly modifiable through proper sleep hygiene practices: maintaining consistent sleep and wake times, creating a cool, dark, quiet sleep environment, avoiding screens before bedtime, limiting caffeine and alcohol consumption, and establishing relaxing bedtime routines. For those with sleep disorders like sleep apnea, seeking medical evaluation and treatment can dramatically improve both sleep quality and cardiovascular health. Prioritizing sleep as an essential component of health, rather than viewing it as time that could be spent on other activities, represents a fundamental shift that can yield profound cardiovascular benefits.
6. Excess Body Weight - Achieving and Maintaining a Healthy Weight

Excess body weight, particularly abdominal obesity, significantly increases heart disease risk through multiple interconnected pathways that strain the cardiovascular system. Carrying extra weight forces the heart to pump harder to supply blood to additional tissue, while excess fat tissue, especially visceral fat around organs, produces inflammatory substances that contribute to atherosclerosis. Research indicates that obesity increases heart disease risk by 64% in women and 46% in men, with the risk escalating progressively with increasing body mass index. The metabolic consequences of excess weight include insulin resistance, type 2 diabetes, elevated blood pressure, abnormal cholesterol levels, and sleep apnea—all independent risk factors for heart disease that compound the cardiovascular threat. However, even modest weight loss can yield significant cardiovascular benefits: losing just 5-10% of body weight can improve blood pressure, cholesterol levels, and blood sugar control. Sustainable weight management involves creating a modest caloric deficit through a combination of healthy eating and regular physical activity, rather than pursuing extreme diets that are difficult to maintain long-term. Focus should be placed on developing healthy habits rather than achieving a specific number on the scale, as improvements in fitness and metabolic health often occur before significant weight loss becomes apparent. The key lies in making gradual, sustainable changes that can be maintained for life, such as portion control, mindful eating, regular meal timing, and finding enjoyable forms of physical activity that become integral parts of daily routine.
7. Excessive Alcohol Consumption - Finding the Heart-Healthy Balance

Alcohol consumption presents a complex relationship with heart health, where moderation may offer some protective benefits while excessive intake significantly increases cardiovascular risk. Research suggests that light to moderate alcohol consumption—defined as up to one drink per day for women and up to two drinks per day for men—may provide some cardiovascular protection through mechanisms including increased HDL cholesterol, reduced blood clotting, and anti-inflammatory effects. However, excessive alcohol consumption, defined as more than these moderate levels or binge drinking patterns, dramatically increases heart disease risk through multiple pathways including elevated blood pressure, cardiomyopathy (weakening of the heart muscle), irregular heart rhythms, increased triglyceride levels, and weight gain. Heavy drinking also contributes to other cardiovascular risk factors such as high blood pressure, stroke risk, and can interfere with medications used to treat heart conditions. The challenge lies in maintaining the fine line between potential benefits and definite harms, as the threshold between moderate and excessive consumption varies among individuals based on factors like body weight, genetics, medications, and overall health status. For many people, the safest approach involves limiting alcohol consumption to special occasions or eliminating it entirely, especially if other cardiovascular risk factors are present. Those who choose to drink should do so mindfully, tracking their consumption, avoiding binge drinking patterns, and understanding that any potential cardiovascular benefits of moderate alcohol consumption can be achieved through other lifestyle modifications without the associated risks that come with alcohol use.
8. Uncontrolled High Blood Pressure - The Silent Cardiovascular Threat
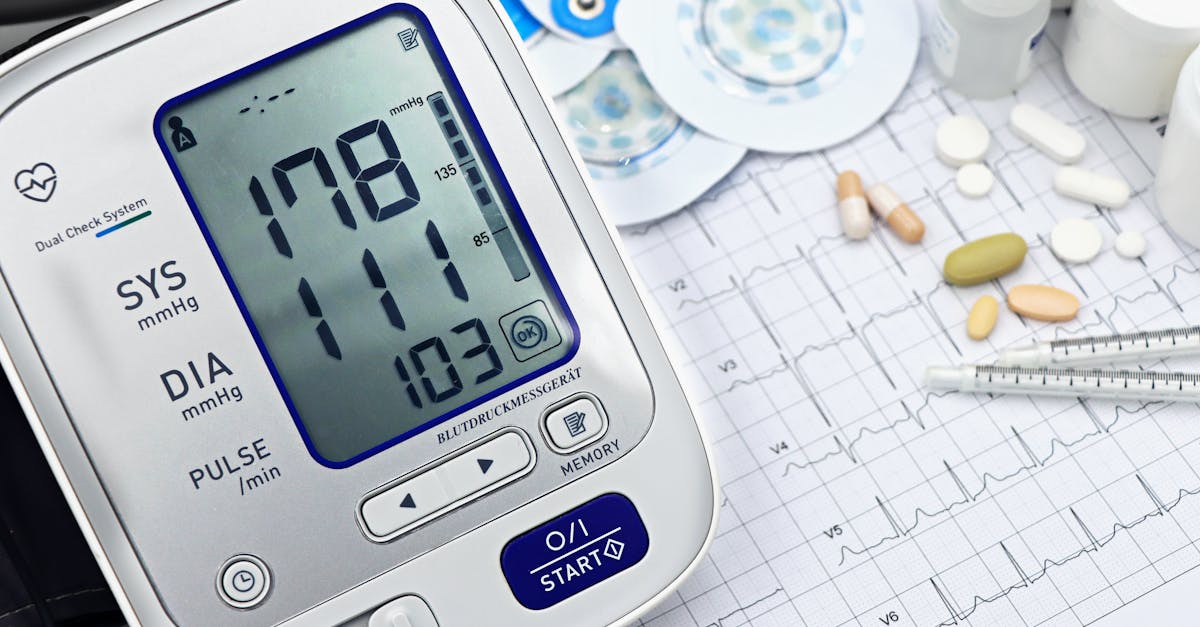
High blood pressure, often called the "silent killer," affects nearly half of all adults and represents one of the most significant yet controllable risk factors for heart disease and stroke. Blood pressure readings consistently above 130/80 mmHg indicate hypertension, a condition that forces the heart to work harder while simultaneously damaging arteries throughout the body. The insidious nature of high blood pressure lies in its typically asymptomatic progression—most people feel perfectly normal while their cardiovascular system sustains ongoing damage. Uncontrolled hypertension accelerates atherosclerosis, increases the risk of heart attack and stroke, can lead to heart failure, and damages kidneys and other organs. The encouraging aspect of this risk factor is that blood pressure is highly responsive to lifestyle modifications: reducing sodium intake, maintaining a healthy weight, engaging in regular physical activity, limiting alcohol consumption, managing stress, and ensuring adequate sleep can all contribute to meaningful blood pressure reductions. The DASH (Dietary Approaches to Stop Hypertension) eating pattern, which emphasizes fruits, vegetables, whole grains, lean proteins, and low-fat dairy while limiting sodium, has been shown to lower blood pressure as effectively as some medications. Regular monitoring is crucial, as blood pressure can fluctuate and change over time. Home blood pressure monitoring devices make it easier than ever to track readings and identify patterns, enabling early intervention when readings begin to climb. For those requiring medication, lifestyle modifications remain important as they can enhance medication effectiveness and sometimes allow for reduced dosages under medical supervision.
9. Poor Cholesterol Management - Balancing the Blood Lipid Equation

Cholesterol management represents a critical yet highly controllable aspect of heart disease prevention, with abnormal cholesterol levels contributing to the development of atherosclerotic plaques that can block coronary arteries. The cholesterol profile includes several components: LDL (low-density lipoprotein) or "bad" cholesterol, which contributes to plaque buildup; HDL (high-density lipoprotein) or "good" cholesterol, which helps remove cholesterol from arteries; and triglycerides, another type of blood fat that can increase heart disease risk when elevated. Optimal levels include LDL cholesterol below 100 mg/dL (or below 70 mg/dL for high-risk individuals), HDL cholesterol above 40 mg/dL for men and above 50 mg/dL for women, and triglycerides below 150 mg/dL. Diet plays a fundamental role in cholesterol management: reducing saturated fat intake, eliminating trans fats, increasing soluble fiber consumption through oats, beans, and fruits, and incorporating heart-healthy fats from sources like nuts, olive oil, and fatty fish can significantly improve cholesterol profiles. Physical activity provides additional benefits by raising HDL cholesterol while helping to lower LDL cholesterol and triglycerides. Weight management also plays a crucial role, as excess weight tends to lower HDL cholesterol while raising LDL cholesterol and triglycerides. Regular cholesterol screening allows for early detection and intervention, with testing recommended every 4-6 years for adults over 20, or more frequently for those with risk factors. The combination of lifestyle modifications and, when necessary, cholesterol-lowering medications can effectively manage cholesterol levels and dramatically reduce heart disease risk.
10. Empowering Your Heart Health Journey
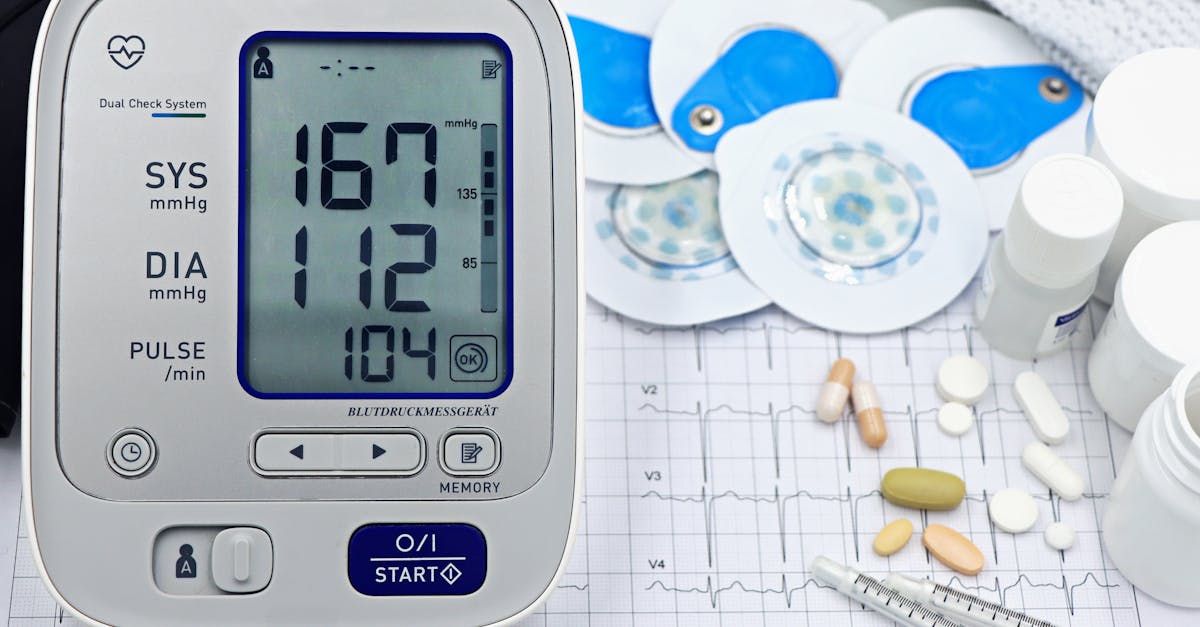
The journey toward optimal heart health is ultimately one of empowerment, choice, and consistent action across multiple interconnected lifestyle factors. The nine controllable risk factors we've explored—diet, physical activity, smoking cessation, stress management, sleep quality, weight management, alcohol moderation, blood pressure control, and cholesterol management—work synergistically to either protect or threaten your cardiovascular system. The remarkable aspect of heart disease prevention lies in the cumulative and compounding effects of positive lifestyle changes: improvements in one area often facilitate improvements in others, creating an upward spiral of better health. For instance, regular exercise not only strengthens the heart directly but also helps with weight management, stress reduction, better sleep, and improved cholesterol levels. Similarly, a heart-healthy diet supports weight management, blood pressure control, and cholesterol optimization while potentially reducing the need for medications. The key to success lies not in perfection but in progress—small, consistent changes maintained over time yield far greater benefits than dramatic but unsustainable modifications. Start with one or two areas that feel most manageable, build confidence through early successes, and gradually expand your heart-healthy practices. Remember that setbacks are normal parts of the journey; what matters most is getting back on track and maintaining a long-term perspective. By taking control of these modifiable risk factors, you're not just preventing disease—you're investing in years of vitality, energy, and the ability to fully engage in life's most meaningful moments with the people you love most.