12 Important Questions to Ask Before Starting a Long-Term Prescription
# 12 Important Questions to Ask Before Starting a Long-Term Prescription: A Comprehensive Guide to Informed Healthcare Decisions
Starting a long-term prescription medication represents one of the most significant healthcare decisions you'll make, with implications that extend far beyond the immediate treatment of your condition. Unlike short-term medications that address acute symptoms, long-term prescriptions become integrated into your daily life, potentially affecting your physical health, mental well-being, financial situation, and overall quality of life for months or even years to come. The complexity of modern pharmaceuticals means that each medication carries its own unique profile of benefits, risks, interactions, and considerations that must be carefully weighed against your individual circumstances, medical history, and personal preferences. Research consistently shows that patients who actively engage in shared decision-making with their healthcare providers achieve better outcomes, experience fewer adverse effects, and maintain higher levels of treatment satisfaction. However, the fast-paced nature of modern healthcare often leaves little time for comprehensive discussions about long-term medication therapy. This article presents twelve essential questions that every patient should ask before committing to a long-term prescription, providing you with the knowledge and framework necessary to make informed decisions that align with your health goals, lifestyle, and values while ensuring the safest and most effective treatment possible.
1. What Is My Exact Diagnosis and How Will This Medication Help?
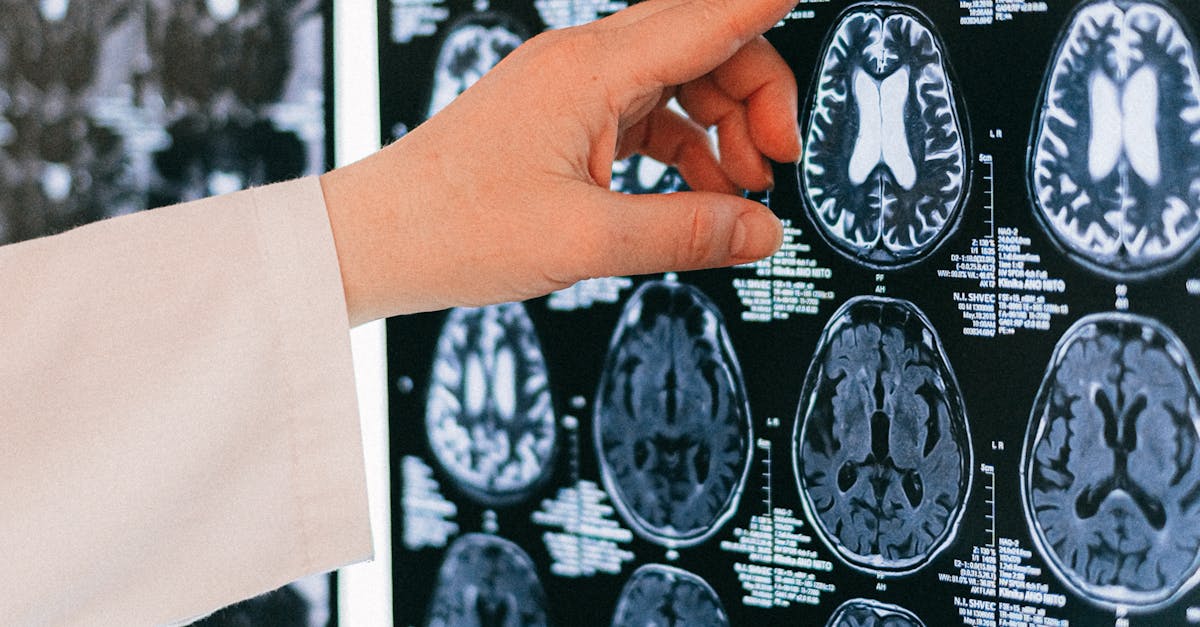
Understanding your precise diagnosis and how the prescribed medication addresses your specific condition forms the foundation of informed consent and treatment adherence. Many patients leave their doctor's office with a prescription but lack a clear understanding of their medical condition, its underlying mechanisms, and how the medication works to address the problem. This knowledge gap can lead to poor adherence, unrealistic expectations, and missed opportunities for lifestyle modifications that could enhance treatment effectiveness. When discussing your diagnosis, ask for detailed explanations in terms you can understand, request written information or reliable online resources, and don't hesitate to ask follow-up questions about the progression of your condition without treatment. Understanding the mechanism of action of your medication—whether it's blocking certain receptors, replacing deficient hormones, or modulating immune responses—helps you appreciate why consistent dosing is important and what to expect in terms of therapeutic effects. Additionally, knowing your diagnosis empowers you to become an active participant in your care, enabling you to monitor symptoms effectively, recognize potential complications, and make informed decisions about complementary treatments or lifestyle changes that could support your medication therapy.
2. What Are the Potential Side Effects and How Common Are They?

A comprehensive understanding of potential side effects is crucial for making an informed decision about long-term medication therapy, as these effects can significantly impact your quality of life and may influence your willingness to continue treatment. Healthcare providers should discuss both common side effects that affect a significant percentage of patients and rare but serious adverse reactions that, while uncommon, could have severe consequences. Ask for specific percentages or frequency data when available, as understanding that a side effect occurs in 30% of patients versus 3% helps you make more informed risk assessments. It's important to distinguish between side effects that typically diminish over time as your body adjusts to the medication and those that may persist or worsen with continued use. Additionally, inquire about delayed side effects that might not appear until weeks or months after starting treatment, as these can catch patients off guard and lead to unnecessary anxiety or treatment discontinuation. Understanding the difference between bothersome but manageable side effects and those that require immediate medical attention is essential for safe medication use. Your healthcare provider should also discuss strategies for managing common side effects, such as taking medications with food to reduce gastrointestinal upset or timing doses to minimize sleep disruption, as these practical tips can significantly improve your treatment experience and adherence.
3. Are There Alternative Treatment Options Available?

Exploring alternative treatment options ensures that you're choosing the most appropriate therapy for your specific situation rather than simply accepting the first medication suggested. Alternative treatments may include other medications within the same class that have different side effect profiles, medications from entirely different drug classes that work through different mechanisms, or non-pharmacological interventions such as lifestyle modifications, physical therapy, counseling, or medical devices. Understanding why your healthcare provider is recommending a specific medication over alternatives helps you appreciate the thought process behind the decision and may reveal factors you hadn't considered. Some alternatives might be equally effective but have different cost implications, dosing schedules, or side effect profiles that could better suit your lifestyle or preferences. Additionally, combination therapies that use lower doses of multiple medications might be an option for some conditions, potentially reducing side effects while maintaining therapeutic effectiveness. It's also worth discussing whether a trial of non-pharmacological interventions might be appropriate before starting medication, particularly for conditions where lifestyle modifications have proven benefits. Your healthcare provider should be able to explain the evidence supporting different treatment approaches and help you understand why they believe the recommended medication is the best choice for your particular circumstances, medical history, and treatment goals.
4. How Long Will I Need to Take This Medication?

Understanding the expected duration of treatment is essential for planning your healthcare journey and setting realistic expectations about your medication regimen. Some long-term prescriptions are intended for specific periods, such as six months to two years, with the goal of achieving remission or cure, while others may be lifelong commitments for managing chronic conditions like diabetes, hypertension, or autoimmune disorders. Knowing whether your treatment has a defined endpoint helps you mentally prepare for the commitment and understand what success looks like in your particular case. For medications intended to be temporary, ask about the criteria that will be used to determine when it's safe to discontinue treatment, such as specific lab values, symptom resolution, or imaging results. Understanding these benchmarks allows you to track your progress and actively participate in decisions about treatment duration. For potentially lifelong medications, discuss whether periodic attempts to reduce dosages or discontinue treatment might be appropriate as your condition evolves or if your overall health status changes. Some patients may be able to reduce or eliminate medications through significant lifestyle changes, weight loss, or other interventions, while others may require dose adjustments over time due to changes in kidney or liver function, age-related factors, or the natural progression of their condition. Having this conversation upfront helps you understand the long-term commitment and plan accordingly for ongoing medical care and prescription costs.
5. What Are the Potential Drug Interactions and Contraindications?

Drug interactions represent a significant safety concern in long-term medication therapy, as the risk of problematic interactions increases with the number of medications you take and the duration of treatment. Your healthcare provider should review all your current medications, including prescription drugs, over-the-counter medications, supplements, and herbal remedies, to identify potential interactions that could reduce effectiveness or increase the risk of adverse effects. Some interactions are absolute contraindications that make certain medication combinations dangerous, while others may require dose adjustments, increased monitoring, or timing modifications to minimize risks. It's important to understand not only your current medication interactions but also how the new prescription might limit your options for future treatments or require special considerations if you need emergency medical care. Ask about interactions with common over-the-counter medications you might take occasionally, such as pain relievers, cold medications, or antacids, as these seemingly minor interactions can sometimes have significant consequences. Food and alcohol interactions are equally important to discuss, as some medications require specific dietary restrictions or timing relative to meals, while others may have dangerous interactions with alcohol that could persist for days after your last dose. Additionally, certain medical conditions may contraindicate specific medications, so ensure your healthcare provider has a complete picture of your medical history, including conditions that might not seem directly related to your current treatment.
6. How Will This Medication Affect My Daily Life and Routine?
The impact of long-term medication on your daily routine extends far beyond simply remembering to take pills, encompassing effects on work performance, social activities, exercise routines, travel plans, and overall lifestyle flexibility. Some medications require specific timing that may conflict with your work schedule, such as medications that cause drowsiness and are best taken at bedtime, or those that need to be taken on an empty stomach in the morning. Understanding these requirements upfront allows you to plan your daily routine accordingly and discuss potential modifications with your healthcare provider if the recommended schedule isn't practical for your lifestyle. Consider how the medication might affect your ability to drive, operate machinery, or perform job-related tasks, particularly during the initial adjustment period when side effects may be more pronounced. For medications that cause photosensitivity, you'll need to plan for increased sun protection and potentially modify outdoor activities. Some medications may affect your exercise tolerance or require modifications to your fitness routine, while others might impact your sleep patterns or energy levels throughout the day. Travel considerations are particularly important for long-term medications, including how to maintain your dosing schedule across time zones, whether the medication requires special storage conditions, and how to ensure an adequate supply during extended trips. Additionally, consider how the medication might affect social situations, such as alcohol restrictions that could impact social drinking or side effects that might influence your comfort level in various social settings.
7. What Monitoring and Follow-up Care Will Be Required?

Long-term medication therapy typically requires ongoing monitoring to ensure safety, effectiveness, and early detection of potential complications, making it essential to understand the surveillance plan before starting treatment. Different medications require different types of monitoring, ranging from periodic blood tests to check organ function or drug levels, to regular physical examinations, specialized imaging studies, or specific symptom assessments. Understanding the frequency and type of monitoring required helps you plan for the time and cost commitments involved in safe medication management. Some medications require intensive initial monitoring with frequent visits and lab work during the first few months, followed by less frequent but ongoing surveillance, while others may need consistent regular monitoring throughout the duration of treatment. Ask about what specific parameters will be monitored, what values or changes would be concerning, and what symptoms you should watch for between appointments that might indicate problems requiring immediate attention. It's also important to understand who will be responsible for monitoring—whether it's your primary care physician, a specialist, or a shared arrangement—and how results will be communicated to you. Discuss what happens if monitoring reveals concerning changes, including whether dose adjustments, additional medications, or treatment discontinuation might be necessary. Understanding the monitoring plan also helps you prepare questions for follow-up appointments and ensures you're an active participant in tracking your response to treatment.
8. What Are the Financial Implications and Insurance Coverage?

The financial impact of long-term medication therapy can be substantial, making it crucial to understand both immediate and long-term costs before committing to treatment. Beyond the obvious prescription costs, consider expenses related to required monitoring, specialist visits, potential side effect management, and any necessary medical equipment or supplies. Insurance coverage for medications can be complex, with different tiers of coverage, prior authorization requirements, and annual deductible considerations that significantly affect your out-of-pocket expenses. Some medications may not be covered by your current insurance plan, requiring appeals processes or consideration of alternative medications that are covered. Ask about generic alternatives that might be available now or expected to become available in the future, as these can dramatically reduce costs while providing equivalent therapeutic benefits. Patient assistance programs offered by pharmaceutical companies may be available for expensive brand-name medications, but these programs often have specific eligibility requirements and application processes that take time to complete. Additionally, consider how medication costs might change if your insurance situation changes due to job changes, retirement, or other life circumstances. Some medications have significantly different costs depending on the pharmacy you use, and prescription discount programs or mail-order pharmacies might offer substantial savings for long-term medications. Understanding the total financial commitment helps you make informed decisions about treatment options and plan your healthcare budget accordingly.
9. How Will This Medication Interact with My Other Health Conditions?

Understanding how a new long-term medication might affect your other health conditions is crucial for comprehensive care and avoiding unintended consequences that could worsen existing problems or create new health challenges. Many medications have effects beyond their primary therapeutic target, and these secondary effects can be beneficial or harmful depending on your overall health profile. For example, some blood pressure medications may worsen asthma symptoms, while certain antidepressants might affect blood sugar control in diabetic patients. Your healthcare provider should consider your complete medical history, including conditions that might not seem directly related to the current treatment, as seemingly unrelated conditions can sometimes be significantly affected by new medications. Discuss how the medication might impact the management of your other conditions, including whether it could interfere with other treatments you're receiving or require modifications to existing medication regimens. Some medications may actually provide benefits for multiple conditions, potentially allowing for simplification of your overall treatment plan, while others might necessitate additional monitoring or preventive measures to protect against complications. It's also important to consider how the new medication might affect your risk factors for developing other conditions, such as how certain medications might impact bone density, cardiovascular risk, or immune function over time. Understanding these interactions helps ensure that your treatment plan is truly comprehensive and that managing one condition doesn't inadvertently compromise your overall health status.
10. What Happens If I Miss Doses or Want to Stop Taking the Medication?
Understanding the consequences of missed doses and the proper procedures for discontinuing medication is essential for safe long-term therapy, as improper medication management can lead to treatment failure, withdrawal symptoms, or serious health complications. Different medications have varying degrees of tolerance for missed doses, with some requiring strict adherence to maintain therapeutic levels while others may be more forgiving of occasional lapses. Ask about specific guidelines for what to do if you miss a dose, including whether you should take it as soon as you remember, skip it entirely, or adjust subsequent doses. Some medications require gradual dose reduction or tapering schedules to safely discontinue treatment, while others can be stopped abruptly without significant risk. Understanding withdrawal symptoms or rebound effects that might occur when stopping medication helps you prepare for these possibilities and seek appropriate medical support if needed. Discuss scenarios where temporary discontinuation might be necessary, such as before certain surgical procedures or during acute illnesses, and understand how to safely resume treatment afterward. It's also important to know what symptoms or situations would require immediate discontinuation of the medication and urgent medical attention. For medications where sudden discontinuation could be dangerous, such as certain heart medications or seizure medications, understanding these risks is crucial for your safety. Having a clear plan for medication discontinuation, whether planned or emergency, ensures that you can make informed decisions about your treatment and avoid potentially dangerous situations.
11. How Will We Measure Success and When Should I Expect to See Results?

Establishing clear expectations for treatment outcomes and timelines is essential for maintaining motivation, adherence, and realistic expectations throughout your medication therapy. Different medications work on vastly different timelines, with some providing rapid symptom relief within hours or days, while others may require weeks or months to achieve full therapeutic effects. Understanding these timelines helps prevent premature discontinuation due to perceived ineffectiveness and allows you to plan appropriately for the adjustment period. Ask about specific, measurable outcomes that will be used to assess treatment success, such as target blood pressure readings, pain scale improvements, laboratory values, or functional assessments. Having concrete goals helps you track your progress and provides objective measures for evaluating treatment effectiveness. Discuss what constitutes partial versus complete response to treatment, as many conditions may show gradual improvement rather than dramatic changes. Understanding the expected trajectory of improvement helps you recognize normal progress versus concerning lack of response that might require treatment modifications. It's also important to discuss what happens if the medication doesn't work as expected, including how long you should try the current treatment before considering alternatives and what modifications might be attempted before changing medications entirely. Some medications may require dose adjustments or combination with other treatments to achieve optimal results, while others might need to be discontinued in favor of alternative approaches. Having realistic expectations about both the timeline and magnitude of expected improvements helps ensure that you give the medication an adequate trial while recognizing when changes in treatment strategy might be necessary.
12. What Lifestyle Modifications Should Accompany This Medication?

Long-term medication therapy is often most effective when combined with appropriate lifestyle modifications that can enhance therapeutic benefits, reduce side effects, and potentially allow for lower medication doses over time. Understanding which lifestyle changes are recommended, required, or contraindicated with your medication helps you develop a comprehensive treatment plan that maximizes your chances of success. Some medications work synergistically with specific dietary changes, exercise programs, or stress management techniques, while others may require you to avoid certain activities or substances for safety reasons. Ask about dietary recommendations that might enhance medication absorption or effectiveness, such as taking certain medications with food or avoiding specific nutrients that could interfere with drug metabolism. Exercise recommendations are particularly important, as some medications may affect your exercise tolerance or require modifications to your fitness routine, while others might actually enhance your ability to exercise by improving symptoms. Sleep hygiene becomes crucial with medications that affect sleep patterns, and understanding how to optimize your sleep environment and schedule can significantly impact both medication effectiveness and overall well-being. Stress management techniques may be particularly beneficial for medications treating mental health conditions, chronic pain, or stress-related disorders. Additionally, discuss any lifestyle modifications that could potentially reduce your need for medication over time, such as weight loss for diabetes management or stress reduction for hypertension, as these changes might allow for dose reductions or even medication discontinuation in some cases.
13. Empowering Your Healthcare Journey Through Informed Decision-Making

Making informed decisions about long-term prescription medications requires active participation in your healthcare and a comprehensive understanding of the treatment you're considering. The twelve questions outlined in this article provide a framework for meaningful discussions with your healthcare provider, ensuring that you have the information necessary to make decisions that align with your health goals, personal values, and lifestyle preferences. Remember that starting a long-term medication is not just a medical decision but a life decision that will affect multiple aspects of your daily existence, from your morning routine to your travel plans, from your financial budget to your social activities. Taking the time to thoroughly explore these questions before beginning treatment can prevent problems down the road and help ensure that your medication therapy is both safe and effective. Don't hesitate to ask for additional time to consider your options, seek second opinions when appropriate, or request written information that you can review at home with family members or trusted advisors. Your healthcare provider should welcome these questions and view them as signs of an engaged, responsible patient rather than challenges to their expertise. The goal is not to avoid necessary medications but to ensure that when you do start long-term therapy, you do so with full knowledge of what to expect and confidence in your decision. By approaching prescription decisions with this level of thoughtfulness and preparation, you become an active partner in your healthcare rather than a passive recipient of treatment, ultimately leading to better outcomes, greater satisfaction with your care, and improved quality of life throughout your treatment journey.