16 Ways to Remember to Take Your Medication Every Day
Medication adherence represents one of the most significant challenges in modern healthcare, with studies revealing that approximately 50% of patients fail to take their medications as prescribed. This seemingly simple task of remembering to take pills daily has profound implications for health outcomes, healthcare costs, and quality of life. Poor medication adherence contributes to an estimated 125,000 deaths annually in the United States alone and costs the healthcare system between $100-300 billion each year. The consequences extend far beyond statistics, affecting individuals' ability to manage chronic conditions like diabetes, hypertension, and heart disease effectively. Whether dealing with complex multi-drug regimens or single daily medications, the human brain's natural tendency to forget routine tasks creates a universal challenge that transcends age, education, and socioeconomic status. Understanding that medication adherence is not simply a matter of willpower but rather a complex interplay of psychological, practical, and environmental factors is crucial for developing effective strategies. The following comprehensive guide presents 16 evidence-based methods to transform medication-taking from a burdensome chore into a seamlessly integrated part of daily life, empowering individuals to take control of their health outcomes through consistent, reliable medication management.
1. Establish a Consistent Daily Routine
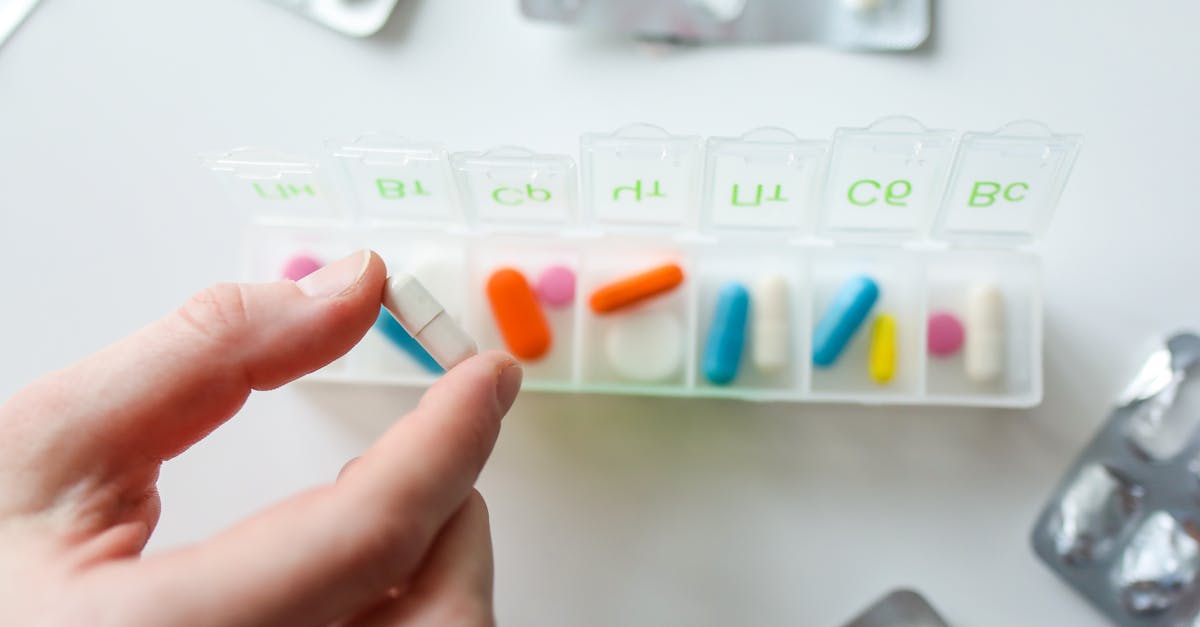
Creating a structured daily routine serves as the foundation for successful medication adherence, leveraging the brain's natural inclination to form habits through repetition and consistency. Research in behavioral psychology demonstrates that when medications are taken at the same time each day within the context of established routines, the likelihood of remembering increases dramatically. The key lies in anchoring medication-taking to existing, well-established daily activities that rarely vary, such as brushing teeth, eating breakfast, or preparing for bed. This technique, known as habit stacking, creates powerful neural pathways that make medication-taking feel as automatic as other daily hygiene practices. The timing should align with both the medication's optimal absorption requirements and the individual's natural circadian rhythms to maximize both effectiveness and adherence. For morning medications, linking them to the first cup of coffee or the act of checking morning emails creates a reliable trigger. Evening medications can be tied to dinner preparation, evening news, or bedtime routines. The consistency of timing not only improves memory but also helps maintain steady medication levels in the bloodstream, optimizing therapeutic outcomes. Studies show that patients who establish consistent routines are 40% more likely to achieve optimal medication adherence compared to those who take medications at random times throughout the day.
2. Utilize Modern Technology and Smartphone Apps

The digital revolution has transformed medication management through sophisticated smartphone applications that offer personalized, intelligent reminder systems far beyond simple alarms. These apps leverage advanced features like GPS location tracking, medication interaction databases, and artificial intelligence to provide comprehensive medication support. Popular applications such as Medisafe, MyTherapy, and PillPack offer customizable reminder schedules, visual pill identification, dosage tracking, and even family notification systems when doses are missed. The visual and auditory cues provided by these apps can be tailored to individual preferences, incorporating favorite songs, personalized messages, or gentle vibrations for discreet reminders in professional settings. Many apps also feature progress tracking capabilities that gamify the medication-taking experience, providing visual feedback on adherence rates and celebrating consecutive days of successful medication management. Advanced features include medication interaction warnings, refill reminders based on remaining pill counts, and integration with pharmacy systems for automatic prescription renewals. The data collected by these apps can be invaluable during medical appointments, providing healthcare providers with accurate adherence information to guide treatment decisions. Research indicates that patients using medication reminder apps show a 25-30% improvement in adherence rates compared to traditional reminder methods, with the highest success rates observed among users who actively engage with the app's tracking and feedback features.
3. Implement Strategic Pill Organization Systems

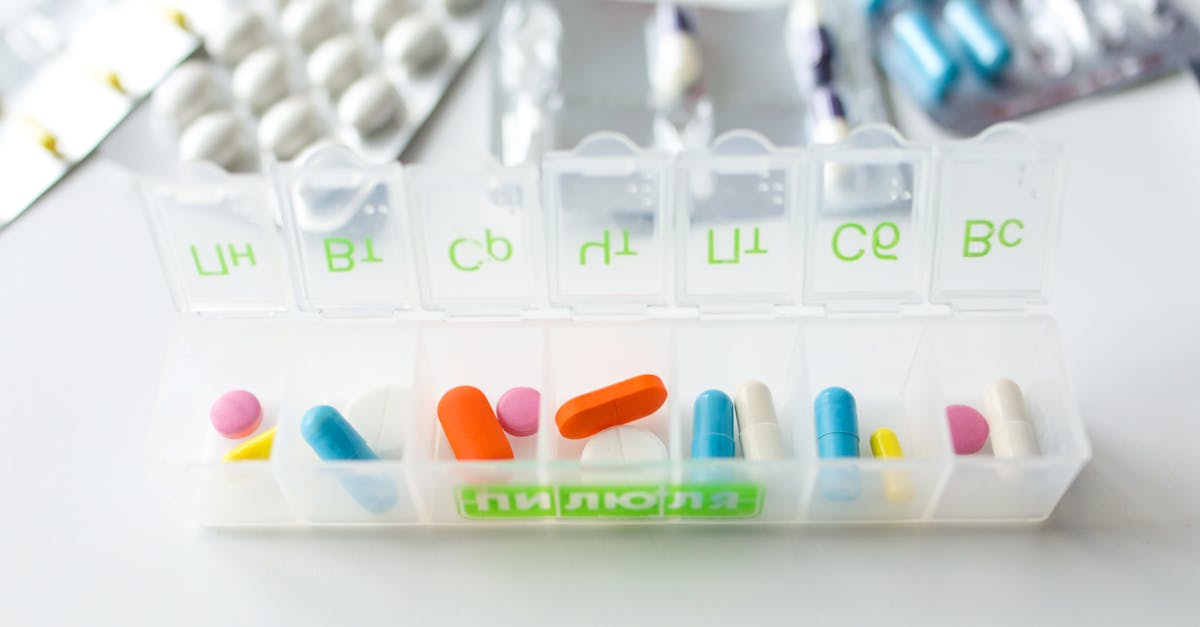
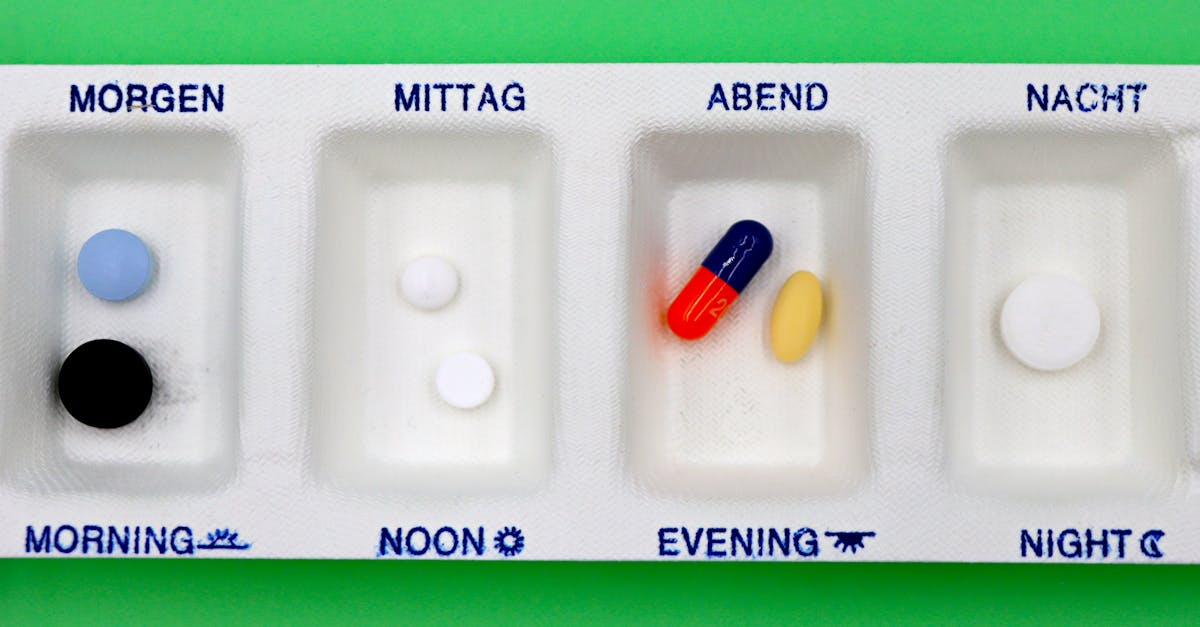
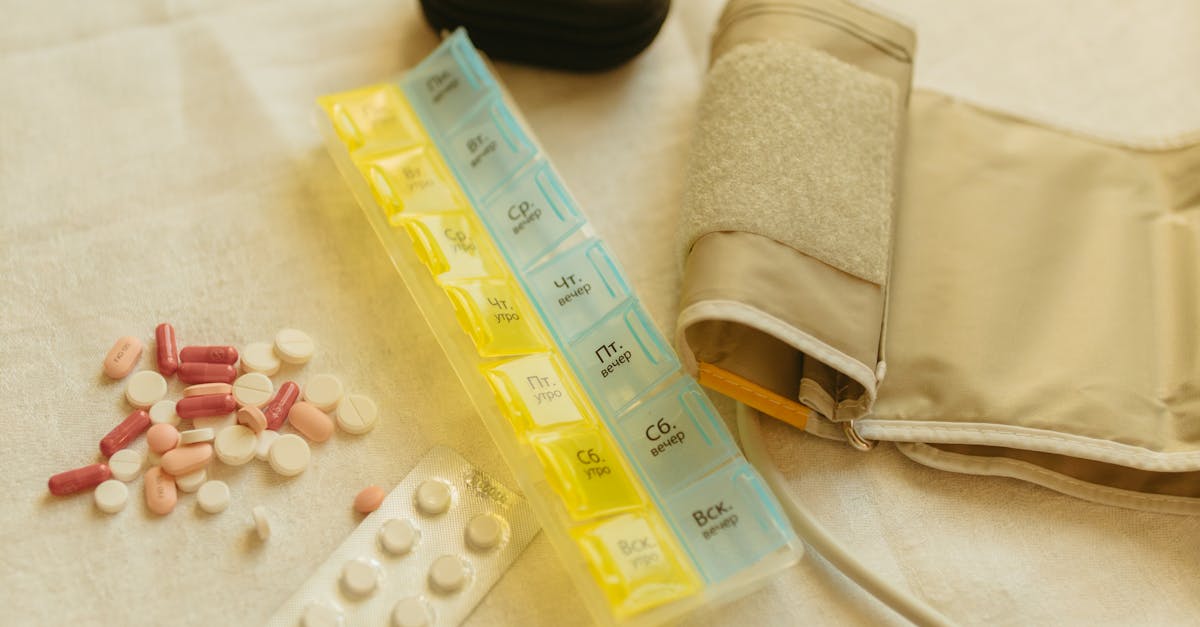
Effective pill organization systems transform the chaos of multiple medications into a streamlined, visual management system that reduces errors and improves adherence. The traditional weekly pill organizer remains one of the most effective tools, but modern versions offer enhanced features like multiple daily compartments, color-coding systems, and locking mechanisms for controlled substances. The act of filling pill organizers weekly serves as both a medication inventory check and a visual commitment to the upcoming week's treatment regimen. This preparation ritual allows individuals to identify potential supply shortages before they become critical and provides an opportunity to review any changes in their medication routine. For complex regimens involving multiple daily doses, compartmentalized organizers with morning, noon, evening, and bedtime sections prevent confusion and ensure proper timing. Clear, labeled compartments eliminate guesswork and reduce the cognitive load associated with remembering which medications to take when. Some advanced organizers feature built-in alarms or smartphone connectivity to provide additional reminder layers. The visual feedback of empty compartments serves as immediate confirmation that medications have been taken, addressing the common concern of wondering whether a dose was already consumed. Studies demonstrate that patients using organized pill systems show significantly higher adherence rates and report reduced anxiety about medication management, with particular benefits observed among elderly patients managing multiple chronic conditions.
4. Create Visual Cues and Environmental Triggers

Environmental design plays a crucial role in medication adherence by creating visual and spatial cues that naturally prompt medication-taking behaviors without relying solely on memory. Strategic placement of medications in highly visible, frequently accessed locations transforms the environment into an active reminder system. The bathroom mirror, kitchen counter near the coffee maker, or bedside table serve as natural focal points that catch attention during daily routines. However, placement must balance visibility with safety considerations, particularly in households with children or visitors. Visual cues extend beyond simple placement to include colorful sticky notes, medication calendars, or even photographs of medications placed in strategic locations. The principle of environmental cueing leverages the psychological concept of contextual memory, where specific locations and visual stimuli become associated with particular behaviors. Creating a dedicated "medication station" with all necessary supplies—pills, water, pill organizer, and reminder materials—establishes a consistent physical context for medication-taking. This approach is particularly effective for individuals with busy lifestyles who benefit from reducing the number of decisions required for medication management. Color-coding systems can further enhance visual cueing, with different colored containers or labels for morning versus evening medications. Research in environmental psychology shows that well-designed visual cue systems can improve medication adherence by up to 35%, with the greatest benefits observed when cues are integrated naturally into existing daily environments rather than requiring significant behavioral changes.
5. Leverage Social Support Networks

Social support networks provide powerful external accountability and emotional encouragement that significantly enhance medication adherence through shared responsibility and caring oversight. Family members, friends, caregivers, and support groups can serve as medication partners who provide reminders, encouragement, and practical assistance when needed. This approach is particularly effective for individuals managing chronic conditions where long-term adherence is crucial for health outcomes. The involvement of trusted individuals creates a safety net that catches potential lapses before they become problematic patterns. Medication partners can assist with prescription pickups, provide transportation to medical appointments, and offer emotional support during challenging periods when motivation wanes. Technology facilitates modern social support through apps that allow family members to receive notifications when medications are missed or through shared calendars that track medication schedules. The psychological benefit of knowing that others care about one's health and are actively involved in supporting medication adherence cannot be overstated. Support groups, whether in-person or online, connect individuals with others facing similar challenges, providing practical tips, emotional validation, and motivation through shared experiences. Healthcare providers can also serve as part of the support network through regular check-ins, medication reviews, and accessible communication channels for questions or concerns. Studies consistently show that patients with strong social support networks demonstrate 20-40% higher medication adherence rates and report greater satisfaction with their treatment regimens compared to those managing medications independently.
6. Establish Reward Systems and Positive Reinforcement

Behavioral psychology principles demonstrate that positive reinforcement significantly improves long-term medication adherence by creating psychological incentives that make medication-taking feel rewarding rather than burdensome. Reward systems can range from simple daily acknowledgments to more elaborate weekly or monthly treats that celebrate consistent adherence. The key lies in selecting rewards that are meaningful to the individual while being sustainable over time. Daily rewards might include favorite beverages, brief entertainment activities, or small personal indulgences that follow successful medication-taking. Weekly rewards could involve special meals, entertainment purchases, or enjoyable activities that celebrate a full week of adherence. Monthly rewards might include larger purchases, special outings, or experiences that recognize sustained commitment to health management. The timing of rewards is crucial—immediate positive reinforcement following medication-taking strengthens the neural pathways associated with the behavior, while delayed rewards provide motivation for sustained adherence. Self-tracking systems that visually display progress, such as calendars with stickers or apps with achievement badges, provide ongoing positive feedback that reinforces successful behaviors. The psychological principle of variable reinforcement suggests that occasional, unpredictable rewards can be even more powerful than consistent ones, creating anticipation and excitement around medication management. Family members can participate in reward systems by acknowledging adherence achievements and celebrating milestones. Research indicates that individuals using structured reward systems show 30-45% better long-term adherence rates and report more positive attitudes toward their medication regimens compared to those relying solely on health-related motivation.
7. Optimize Timing with Meal and Activity Anchors

Linking medication schedules to consistent daily activities, particularly meals and established routines, creates powerful behavioral anchors that improve adherence through natural timing cues. Meal-based scheduling is particularly effective because eating patterns tend to be relatively consistent and provide natural reminders three times daily. However, this approach requires careful consideration of medication-specific requirements, as some drugs must be taken on empty stomachs while others require food for optimal absorption. Morning medications can be anchored to breakfast preparation, coffee brewing, or the first meal of the day, creating a natural sequence that becomes automatic over time. Lunch-time medications might be linked to midday meal preparation or specific work routines for individuals with consistent schedules. Evening medications can be tied to dinner preparation, family meal times, or evening snack routines. Beyond meals, other consistent daily activities serve as excellent anchors: morning shower routines, commute preparations, evening television programs, or bedtime preparations. The key is identifying activities that occur at consistent times and rarely get skipped, ensuring the medication anchor remains reliable. For individuals with irregular schedules, multiple anchor options provide flexibility while maintaining consistency. Weekend routines may require different anchors than weekday schedules, necessitating adaptable systems that account for lifestyle variations. Activity-based anchoring also helps address the common problem of taking medications at optimal times for absorption and effectiveness while working within realistic lifestyle constraints. Studies show that patients using meal and activity anchors demonstrate 25-35% better adherence rates and report that medication-taking feels more natural and less disruptive to their daily lives.
8. Address and Overcome Common Barriers
Successful medication adherence requires proactive identification and resolution of common barriers that prevent consistent medication-taking, ranging from practical challenges to psychological obstacles. Cost concerns represent one of the most significant barriers, with many patients rationing medications or skipping doses due to financial constraints. Solutions include exploring generic alternatives, pharmaceutical assistance programs, insurance formulary options, and discussing cost concerns openly with healthcare providers who may suggest equally effective but more affordable alternatives. Side effects create another major barrier, often leading to discontinuation without medical consultation. Addressing this requires open communication with healthcare providers about side effect experiences, timing adjustments to minimize impact, and exploration of alternative medications with better tolerability profiles. Forgetfulness, while seemingly simple, often masks underlying issues like depression, stress, or cognitive changes that require targeted interventions. Complex medication regimens can overwhelm patients, necessitating simplification strategies, clear written instructions, and regular medication reviews to eliminate unnecessary drugs. Travel and schedule disruptions require advance planning, portable organization systems, and backup reminder strategies. Skepticism about medication necessity or effectiveness requires education, shared decision-making with healthcare providers, and clear understanding of treatment goals and expected outcomes. Physical barriers such as difficulty opening containers, swallowing pills, or reading labels need practical solutions like easy-open containers, liquid formulations, or magnifying aids. Psychological barriers including fear of dependency, stigma, or loss of control require empathetic support and education about medication benefits versus risks. Research demonstrates that patients who actively address barriers with healthcare provider support show 40-50% better long-term adherence compared to those who struggle with unresolved obstacles.
9. Develop Backup Plans for Disrupted Routines
Life's unpredictability necessitates robust backup systems that maintain medication adherence during travel, illness, schedule changes, and other routine disruptions that can derail even the most established medication habits. Travel planning requires advance preparation including sufficient medication supplies, prescription copies, time zone adjustment strategies, and portable organization systems. International travel adds complexity with customs regulations, prescription documentation requirements, and access to medical care if needed. Illness can disrupt normal routines while simultaneously making medication adherence more critical, requiring simplified systems that function even when cognitive capacity is reduced. Work schedule changes, family emergencies, or social obligations can shift normal timing patterns, necessitating flexible reminder systems and alternative anchoring activities. Weekend and holiday routines often differ significantly from weekday patterns, requiring separate backup strategies that account for altered sleep schedules, meal times, and daily activities. Technology failures, whether smartphone malfunctions or power outages, require non-digital backup systems like written schedules, traditional alarm clocks, or family member reminders. Medication supply disruptions due to pharmacy closures, insurance issues, or prescription delays need contingency planning including emergency supplies, alternative pharmacy relationships, and healthcare provider communication protocols. Seasonal changes affecting daily routines, such as daylight saving time or holiday schedules, require proactive adjustment strategies. The key to effective backup planning lies in anticipating potential disruptions and developing specific, actionable responses before they occur. Multiple backup layers provide redundancy that ensures medication adherence even when primary systems fail. Studies indicate that patients with comprehensive backup plans maintain 60-70% better adherence during routine disruptions compared to those relying solely on primary reminder systems.
10. Simplify Complex Medication Regimens

Complex medication regimens with multiple drugs, varying schedules, and intricate instructions create cognitive overload that significantly impairs adherence, making simplification a critical strategy for improving health outcomes. Healthcare providers can often consolidate medications through combination pills, extended-release formulations, or therapeutic substitutions that reduce pill burden while maintaining efficacy. The goal is achieving the simplest effective regimen that minimizes daily decisions and memory requirements. Timing synchronization involves adjusting medication schedules so multiple drugs can be taken simultaneously, reducing the number of daily medication events from potentially eight or more down to two or three manageable sessions. This approach requires careful consideration of drug interactions, absorption requirements, and optimal timing for therapeutic effect. Extended-release formulations can transform multiple daily doses into once-daily regimens, dramatically improving convenience and adherence. However, these formulations may be more expensive and require insurance approval or cost-benefit analysis. Combination medications that include multiple active ingredients in single pills reduce pill burden and simplify regimens, though they may limit dosing flexibility for individual components. Medication reconciliation during healthcare visits provides opportunities to eliminate unnecessary drugs, identify duplications, and streamline regimens based on current health status and treatment goals. Clear, written medication schedules with visual aids help patients understand complex regimens and reduce confusion about timing and dosing. Pharmacist consultation can provide valuable insights into simplification opportunities, generic alternatives, and practical management strategies. The psychological benefit of simplified regimens extends beyond improved adherence to include reduced anxiety, increased confidence in medication management, and better overall treatment satisfaction. Research consistently demonstrates that regimen simplification can improve adherence rates by 20-40%, with the greatest benefits observed in elderly patients and those managing multiple chronic conditions.
11. Monitor Progress and Maintain Accountability
Systematic progress monitoring creates accountability structures that reinforce positive medication-taking behaviors while identifying potential problems before they become serious adherence failures. Self-monitoring through medication diaries, smartphone apps, or simple calendar tracking provides immediate feedback about adherence patterns and helps identify triggers for missed doses. The act of recording medication-taking serves as both a reminder and a commitment device that increases awareness of adherence behaviors. Visual progress tracking through charts, graphs, or app dashboards transforms abstract adherence concepts into concrete, measurable achievements that motivate continued success. Weekly or monthly adherence reviews allow individuals to analyze patterns, identify successful strategies, and adjust approaches based on real-world experience. Healthcare provider involvement in monitoring creates external accountability and provides professional guidance for addressing adherence challenges. Regular medication reviews during appointments offer opportunities to discuss adherence honestly, address barriers, and celebrate successes. Pharmacy-based monitoring through refill tracking can identify potential adherence issues and trigger intervention conversations. Family member involvement in monitoring provides additional support and accountability while ensuring someone notices if adherence patterns change. Technology-enabled monitoring through smart pill bottles, electronic dispensers, or connected devices provides objective adherence data that eliminates guesswork about medication-taking patterns. The key to effective monitoring lies in finding the right balance between helpful accountability and overwhelming surveillance that creates stress or resistance. Positive reinforcement for good adherence patterns is more effective than punitive responses to lapses. Studies show that patients engaged in regular adherence monitoring demonstrate 25-35% better long-term outcomes and report greater confidence in their ability to manage medications effectively over time.
12. Educate Yourself About Your Medications

Comprehensive medication education empowers patients to become active partners in their treatment, significantly improving adherence through increased understanding of medication importance, proper usage, and expected outcomes. Understanding why each medication is prescribed, how it works in the body, and what benefits to expect creates personal investment in the treatment regimen that goes beyond simple compliance. Knowledge about proper timing, food interactions, and administration techniques ensures medications are taken correctly for optimal effectiveness. Awareness of potential side effects, what to expect during initial treatment phases, and when to contact healthcare providers reduces anxiety and prevents premature discontinuation due to normal adjustment periods. Drug interaction education helps patients make informed decisions about over-the-counter medications, supplements, and lifestyle choices that might affect prescription drug effectiveness. Understanding the consequences of missed doses, whether single doses can be doubled up, and how to handle forgotten medications prevents dangerous self-medication decisions. Learning to read prescription labels, understand generic versus brand names, and recognize medication changes helps prevent errors and confusion. Education about proper storage, expiration dates, and disposal methods ensures medication safety and effectiveness. Cost education including insurance coverage, generic options, and assistance programs helps patients make informed financial decisions about their treatment. The education process should be ongoing, with regular updates about new information, treatment changes, and emerging research relevant to the patient's condition. Healthcare providers, pharmacists, and reputable online resources serve as valuable education sources, though information