7 Things to Know About Medication Storage and Expiration Dates
# 7 Things to Know About Medication Storage and Expiration Dates: A Complete Guide to Safe Drug Management
Proper medication storage and understanding expiration dates represent fundamental pillars of safe healthcare practice that millions of people overlook daily. Whether you're managing a single prescription or multiple medications for chronic conditions, the way you store your drugs and interpret their expiration dates can mean the difference between effective treatment and potential harm. The pharmaceutical industry invests billions of dollars in research to determine optimal storage conditions and shelf life parameters, yet many patients remain unaware of how environmental factors like temperature, humidity, and light exposure can dramatically alter medication potency and safety. From the moment a medication leaves the pharmacy to its final dose, a complex interplay of chemical, physical, and environmental factors determines whether that drug will deliver its intended therapeutic benefit or potentially cause adverse effects. Understanding these principles isn't just about following label instructions—it's about taking an active role in your healthcare safety and ensuring that every medication you take performs exactly as your healthcare provider intended when they prescribed it.
1. Temperature Control - The Foundation of Medication Stability

Temperature represents the most critical environmental factor affecting medication stability, with even minor deviations from recommended storage conditions potentially compromising drug efficacy and safety. Most medications are designed to remain stable at room temperature, typically defined as 68-77°F (20-25°C), but this seemingly simple requirement becomes complex when considering real-world storage scenarios. Heat accelerates chemical degradation processes, causing active pharmaceutical ingredients to break down into less effective compounds or, in some cases, potentially harmful byproducts. Conversely, freezing can cause physical changes in liquid medications, such as separation or crystallization, that render them ineffective even after returning to room temperature. Refrigerated medications, including many insulin formulations, vaccines, and certain antibiotics, require consistent temperatures between 36-46°F (2-8°C) to maintain their molecular structure and therapeutic properties. The challenge extends beyond simply placing medications in appropriate locations—temperature fluctuations during transport, power outages affecting refrigeration, or storing medications in cars during extreme weather can all compromise drug integrity. Healthcare professionals recommend using a refrigerator thermometer to monitor storage temperatures and avoiding common mistakes like storing medications in bathroom medicine cabinets, where steam from hot showers creates temperature spikes, or in kitchen areas near heat-generating appliances.
2. Humidity and Moisture - The Silent Destroyers of Drug Integrity
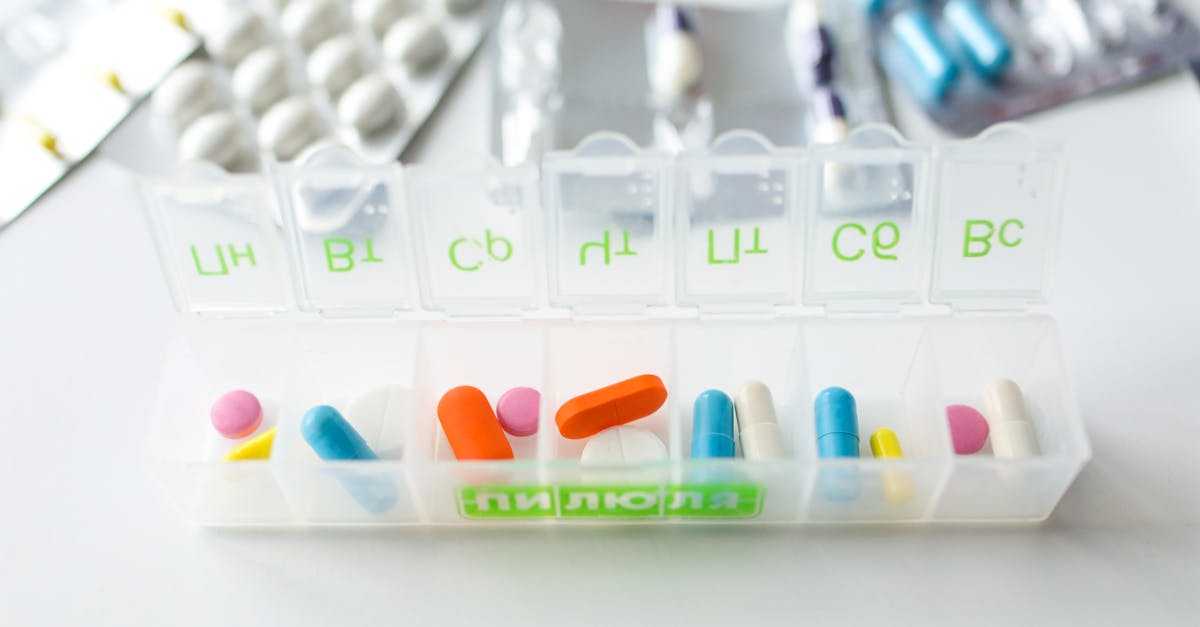
Moisture represents one of the most insidious threats to medication stability, often causing irreversible damage before visible signs of deterioration appear. Many pharmaceutical compounds are hygroscopic, meaning they readily absorb water from the surrounding environment, which can trigger chemical reactions that alter their therapeutic properties or create toxic degradation products. The bathroom medicine cabinet, despite its traditional role as a medication storage location, represents one of the worst possible environments due to high humidity levels from showers and baths that can reach 80-90% relative humidity. Tablets and capsules are particularly vulnerable to moisture damage, with some medications beginning to degrade within hours of exposure to high humidity conditions. Moisture can cause tablets to crumble, capsules to become sticky or dissolve prematurely, and powdered medications to clump together or change color. The pharmaceutical industry addresses this concern through sophisticated packaging, including desiccant packets, moisture-resistant blister packs, and specially designed bottles with tight-sealing caps, but these protective measures become ineffective once packages are opened in humid environments. To combat moisture-related degradation, medications should be stored in cool, dry locations with relative humidity levels below 60%, such as bedroom closets or dedicated medication storage areas away from kitchens and bathrooms. Additionally, keeping medications in their original containers with tightly closed lids, avoiding the transfer of pills to weekly pill organizers in humid environments, and using silica gel packets in storage areas can help maintain optimal moisture levels.
3. Light Exposure - Protecting Medications from Photodegradation

Light exposure, particularly ultraviolet radiation, can trigger photochemical reactions that fundamentally alter medication structure and potency, making proper light protection essential for maintaining drug efficacy. Many medications contain light-sensitive compounds that undergo photodegradation when exposed to natural sunlight or even artificial lighting, resulting in reduced therapeutic effectiveness or the formation of potentially harmful breakdown products. This photosensitivity explains why many medications come in amber-colored bottles or opaque packaging designed to filter out harmful wavelengths of light. Medications stored in clear containers or left on windowsills, kitchen counters, or other areas with direct light exposure can experience significant potency loss within days or weeks, regardless of their expiration date. The degradation process often occurs without visible changes to the medication's appearance, making it impossible for patients to detect compromised drugs through visual inspection alone. Certain medication classes, including some antibiotics, cardiovascular drugs, and psychiatric medications, are particularly susceptible to light-induced degradation and may lose substantial potency when improperly stored. Healthcare professionals recommend storing all medications in dark locations, such as closed cabinets or drawers, and avoiding transparent pill organizers that expose medications to ambient light. For medications that must be kept in refrigerators, wrapping them in aluminum foil or storing them in opaque containers provides additional protection from refrigerator lighting that cycles on and off throughout the day.
4. Understanding Expiration Dates - Science Behind the Numbers

Expiration dates represent the culmination of extensive scientific testing and regulatory oversight, providing consumers with evidence-based guidance on medication safety and efficacy timelines. The process of determining expiration dates involves rigorous stability testing under controlled conditions, where pharmaceutical manufacturers monitor drug potency, purity, and safety parameters over extended periods to establish the timeframe during which medications maintain at least 90% of their labeled potency. This testing occurs under specific storage conditions, meaning that expiration dates are only valid when medications are stored according to manufacturer recommendations. The distinction between "use by," "expiration," and "discard after" dates can be confusing, but each serves a specific purpose in medication safety protocols. "Use by" dates typically indicate the period of optimal effectiveness, while "expiration" dates mark the point after which manufacturers can no longer guarantee full potency or safety. "Discard after" dates, commonly found on liquid medications and those requiring reconstitution, indicate when medications may become unsafe due to bacterial growth or chemical instability. Research conducted by the FDA's Shelf Life Extension Program has demonstrated that many medications retain significant potency well beyond their labeled expiration dates when stored properly, but this doesn't mean expired medications are universally safe or effective. The variability in post-expiration potency depends on numerous factors, including the specific drug formulation, storage conditions, and the medication's inherent chemical stability, making it impossible to provide blanket recommendations about using expired medications.
5. The Risks of Using Expired Medications - When Time Becomes Dangerous
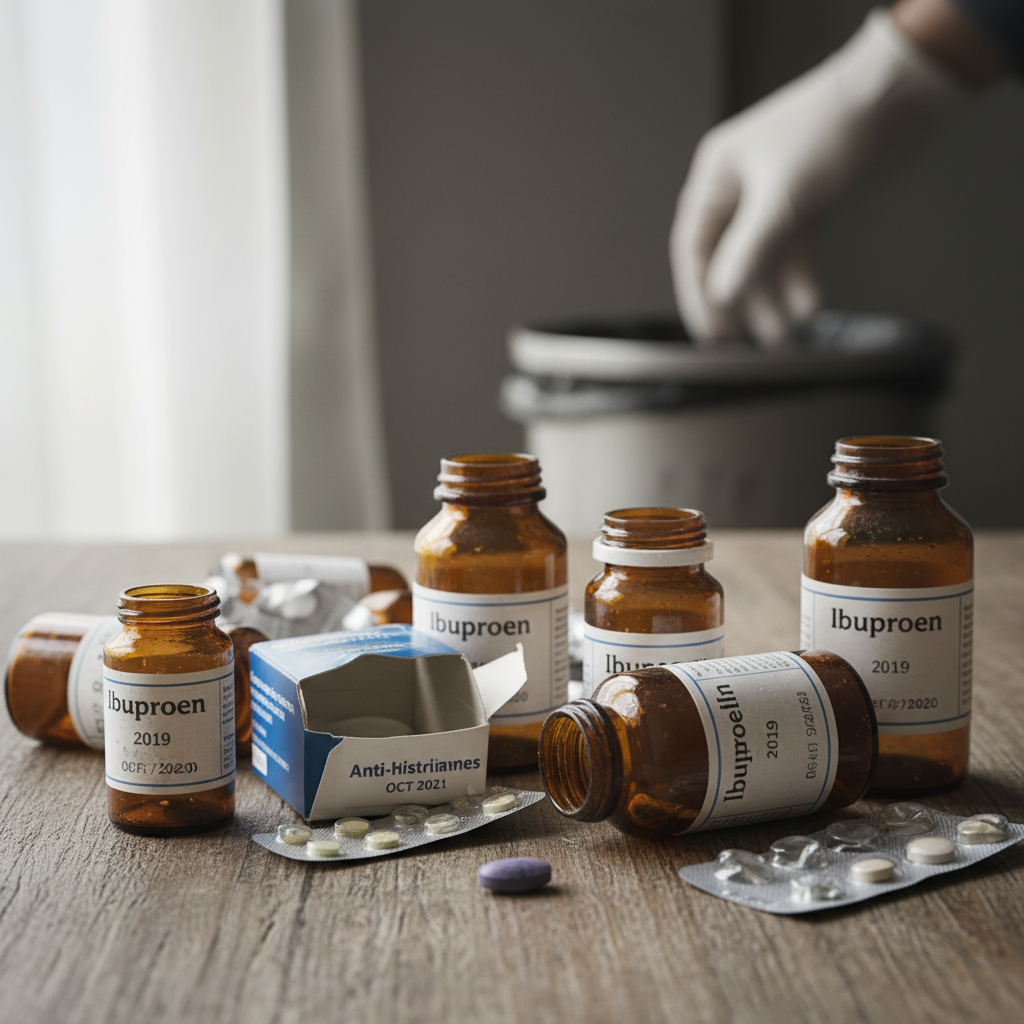
Using expired medications presents a complex risk profile that extends far beyond simple reduced effectiveness, potentially exposing patients to serious health consequences ranging from treatment failure to toxic reactions. The primary concern with expired medications involves decreased potency, which can result in subtherapeutic drug levels that fail to treat the underlying condition effectively. This is particularly dangerous for medications treating serious conditions such as heart disease, diabetes, or infections, where inadequate treatment can lead to disease progression, complications, or life-threatening situations. Beyond reduced effectiveness, some medications undergo chemical changes over time that create toxic degradation products, with tetracycline antibiotics serving as a classic example of drugs that can cause kidney damage when used past their expiration date. Liquid medications, eye drops, and injectable drugs pose additional risks due to potential bacterial contamination over time, especially once opened and exposed to environmental microorganisms. The preservatives included in these formulations have limited effectiveness periods, after which bacterial growth can occur, potentially leading to serious infections. Insulin and other protein-based medications can undergo structural changes that not only reduce their effectiveness but may also trigger immune reactions in some patients. Emergency medications, such as epinephrine auto-injectors for severe allergic reactions, present unique challenges because using an expired device during a life-threatening emergency may provide insufficient treatment, while not using it could result in death. Healthcare professionals emphasize that the risks of using expired medications often outweigh potential benefits, particularly when considering that most medications remain available through prescription refills or over-the-counter purchases.
6. Special Storage Requirements - Medications That Need Extra Care

Certain medications require specialized storage conditions that go beyond standard room temperature recommendations, demanding careful attention to maintain their therapeutic integrity and patient safety. Refrigerated medications, including many insulin formulations, growth hormones, and certain vaccines, must be maintained within narrow temperature ranges and protected from freezing, which can cause irreversible protein denaturation and complete loss of therapeutic activity. These medications often require specific handling procedures, such as allowing refrigerated insulin to reach room temperature before injection to reduce discomfort and ensure proper absorption. Controlled substances present unique storage challenges due to both stability requirements and legal obligations, necessitating secure storage that prevents unauthorized access while maintaining appropriate environmental conditions. Some medications, such as nitroglycerin tablets, require protection from heat, light, and moisture while remaining readily accessible for emergency use, leading to recommendations for small, dark glass containers that can be carried safely. Liquid medications and suspensions often require refrigeration after opening and have significantly shorter shelf lives than their solid counterparts, with some requiring disposal within days or weeks of first use regardless of the printed expiration date. Medications requiring reconstitution, such as certain antibiotics or injectable drugs, present timing challenges because their stability clock begins ticking from the moment water is added, not from the original manufacturing date. Topical medications, including creams, ointments, and patches, can be affected by temperature extremes that alter their consistency, absorption properties, or adhesive qualities. Understanding these special requirements involves reading medication guides carefully, consulting with pharmacists about proper storage techniques, and establishing systems to monitor and maintain appropriate storage conditions consistently.
7. Safe Disposal Methods - Protecting Others and the Environment

Proper medication disposal represents a critical public health and environmental responsibility that requires understanding of various disposal methods and their appropriate applications. The traditional practice of flushing medications down toilets or throwing them in household trash creates significant environmental contamination and public safety risks, as pharmaceutical compounds can persist in water systems and soil for extended periods. The FDA maintains a specific list of medications that should be flushed immediately when no longer needed due to their high potential for abuse or accidental ingestion, but this list is limited to drugs where the immediate risk of improper disposal outweighs environmental concerns. For most medications, the preferred disposal method involves mixing them with unpalatable substances like coffee grounds or cat litter, sealing them in containers, and disposing of them in household trash after removing or obscuring personal information from prescription labels. Drug take-back programs, sponsored by the DEA and local law enforcement agencies, provide the safest and most environmentally responsible disposal option, offering secure collection sites where trained personnel handle pharmaceutical waste according to strict protocols. Many pharmacies and healthcare facilities now offer permanent drop-off locations for unused medications, making safe disposal more convenient for patients. Controlled substances require special attention during disposal due to their abuse potential, with many requiring witness verification or specific documentation during the disposal process. Sharps and injection devices need separate disposal in puncture-resistant containers, which can often be obtained from pharmacies or healthcare providers and returned through specialized collection programs. The environmental impact of pharmaceutical disposal extends beyond immediate contamination concerns, as studies have detected medication residues in drinking water supplies, affecting aquatic ecosystems and potentially contributing to antibiotic resistance development in environmental bacteria.
8. Creating an Effective Medication Management System - Putting Knowledge into Practice

Implementing a comprehensive medication management system transforms theoretical knowledge about storage and expiration dates into practical safeguards that protect health and maximize therapeutic outcomes. An effective system begins with conducting a thorough inventory of all medications, including prescription drugs, over-the-counter medications, vitamins, and supplements, noting their expiration dates, storage requirements, and current condition. This inventory should be updated regularly, ideally every three to six months, to identify expired medications for disposal and ensure that storage conditions remain appropriate. Creating designated storage areas for different types of medications—such as a cool, dry location for room temperature drugs, appropriate refrigerator space for cold-sensitive medications, and secure storage for controlled substances—helps maintain optimal conditions while preventing accidental misuse. Medication organization systems should balance accessibility with safety, ensuring that frequently used medications remain easily accessible while keeping potentially dangerous drugs away from children and unauthorized users. Technology can enhance medication management through smartphone apps that track expiration dates, send refill reminders, and provide storage guidance, while simple solutions like labeling storage areas and maintaining medication logs can be equally effective. Regular communication with healthcare providers and pharmacists about medication storage concerns, questions about expiration dates, and disposal needs ensures that professional guidance supports personal management efforts. Emergency preparedness should be integrated into medication management systems, including maintaining adequate supplies of critical medications, understanding how to store medications during power outages or natural disasters, and having plans for accessing medications during emergencies. The most effective medication management systems are those that can be maintained consistently over time, adapting to changing health needs, living situations, and medication regimens while preserving the fundamental principles of safe storage, timely disposal, and informed decision-making about medication use.