Breast Cancer Identified Risks, Diagnostic, And Treatment Advancements Worth Knowing About
The survival rates for women diagnosed with breast cancer have significantly increased, thanks to many medical advances implemented over the last ten years. More effective therapies are resulting in far less side effects than traditional procedures. An increase in understanding both risk and preventive measures, have all given women the necessary tools to take preventative action against breast cancer. Start reading now to learn about the major advancements in breast cancer risk factors, diagnosis, and treatment everyone should know about.
HER2-Directed Therapies

Human epidermal growth factor receptor 2 (HER2) is a protein that promotes the growth of cancer cells. Recent treatments directed at HER2 have been shown to play a vital role in breast cancer survival. Not all breast cancers are bombarded with the protein, and those that are can be adequately treated with specific drugs that target it. HER2-directed therapies have completely revolutionized treatment options, as these drugs can be utilized for both early and late stage breast cancer and can assist in reducing recurrence risk in the early stages of the disease.
Continue reading to learn about gene expression testing next.
Gene Expression Testing

Assays, which are tests to uncover the types of genes that cancer expresses, have permitted healthcare physicians to craft effective therapies based on a person’s individual needs. Breast cancer specialists are utilizing two assays, Oncotype DX® and MammaPrint®, to better determine a woman’s risk of any recurrence or metastasis (the spread) based upon varying genes cancer expresses, through a process called gene subtyping. From here, they can better plan treatments to reduce these risks effectively. These tests can also assist in finding out who is more likely to benefit from treatments with chemotherapy in addition to hormone therapy.
Continue reading to learn about an advancement made in chemotherapy for treating breast cancer.
Less Aggressive Chemo

Super aggressive chemotherapy, when combined with a drug called trastuzumab, can work effectively in curing one early stage, yet highly aggressive, form of breast cancer, called lymph node negative HER2+ breast cancer. This type of breast cancer affects approximately fifteen to twenty percent of all breast cancer patients. Researchers are now finding a less aggressive chemotherapy drug called taxol, when combined with trastuzumab, is just as effective in helping ward off breast cancer recurrences and even death following a three-year duration. The major difference is the impact on the patient, since they seem to struggle less with the less aggressive form of chemotherapy.
Continue reading to learn about strengthening bones.
Bone Strengthening Medications

Breast cancer will most commonly move to the bones, and research has debated whether or not bone-strengthening medications, which are called bisphosphonates and are developed to treat osteoporosis, can help prevent this. A recent meta-analysis of these debates has confirmed osteoporosis medications can lower breast cancer recurrence in bones and lower death rates in postmenopausal women. The medications also have the added benefit of reducing bone fractures. These results were all in middle-aged or older women who were candidates for bisphosphonate medication. Younger women with breast cancer are advised to talk to their doctors regarding available options. As with numerous medications, bisphosphonates can have serious side effects, such as osteonecrosis of the jaw, where the gum recedes and the jaw bone becomes exposed to air.
Read on to discover the details about immunotherapy as it applies to breast cancer treatment.
Immunotherapy

Triple-negative breast cancer, a type that accounts for ten to twenty percent of all breast cancers, is much more aggressive and also more likely to affect young women, black and Latino women, and women with the BRCA1 gene mutation. These tumors do not have estrogen receptors, progesterone receptors, or the HER2 growth factor, which means three forms of targeted treatment are not an option.
Only radiation therapy, surgery, and chemotherapy can be used to combat against this form of tumor, often with very little effect, as it is highly likely to come back and spread. Immunotherapy medication can activate an individual’s immune system against the tumor, and though further research is needed, could one day prove to be a promising therapy against triple negative breast cancer.
Read about more advancements in breast cancer treatment now.
Cryoablation
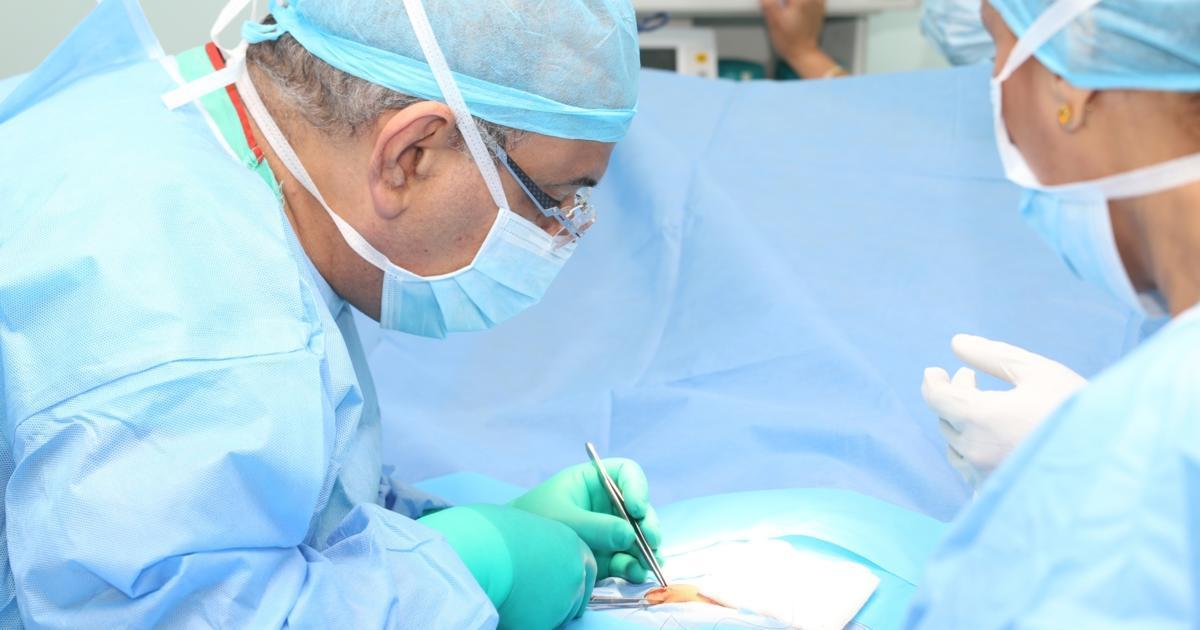
Cryoablation is a new type of minimally invasive cancer treatment that kills cancerous cells on the spot by deep freezing them to death. At this time, only certain types of breast cancer can be treated with this method. During the procedure, a surgeon utilizes imaging technology to direct a cryoprobe or needle-like tool through an incision in the patient's skin and into the malignant breast tissues. Once in place, the cryoprobe infuses the area with liquid nitrogen that freezes and kills the malignant cells. This technique uses a freeze of temperatures at least forty degrees below zero for an increment of six to eight minutes. The freezing period is followed by a thawing increment of ten minutes. This process may be repeated several times to achieve the desired effect on the tumor. Not only is this technique successful at the eradication of cancerous cells, but it may also have a beneficial impact on the individual's immune system. When the cancerous cells are frozen and burst open, their genetic material is released into the body. The immune system of the patient responds to this genetic material and remembers it in order to eradicate any remaining cancer cells or stop new cancers from developing.
Get more details on breast cancer treatment advancements now.
Use Of Nanotechnology
Nanotechnology is an emerging treatment option for an individual affected by aggressive breast cancer. Nanotechnology is the utilization of very small particles that are 1/100,000th the diameter of a human hair. These nanoparticles are used to allow for more targeted and precise delivery of effective chemotherapy medications that already exist in breast cancer treatment. The nanoparticles are able to bind to specific proteins present only on the cancer cells and able to ignore other healthy cells entirely. Chemotherapy drugs can be delivered to only act on such cancer cells the nanoparticles have identified. Some of these chemotherapy drugs can be programmed not to have any effect until they have reached the target cells and are activated by a type of light or radiation manually administered by a physician. The mechanism that utilizes nanotechnology to deliver chemotherapy is the key to the considerable reduction and even the elimination of harsh side effects commonly associated with chemotherapy.
Uncover details on more breast cancer advancements now.
Improvements In Imaging Tests
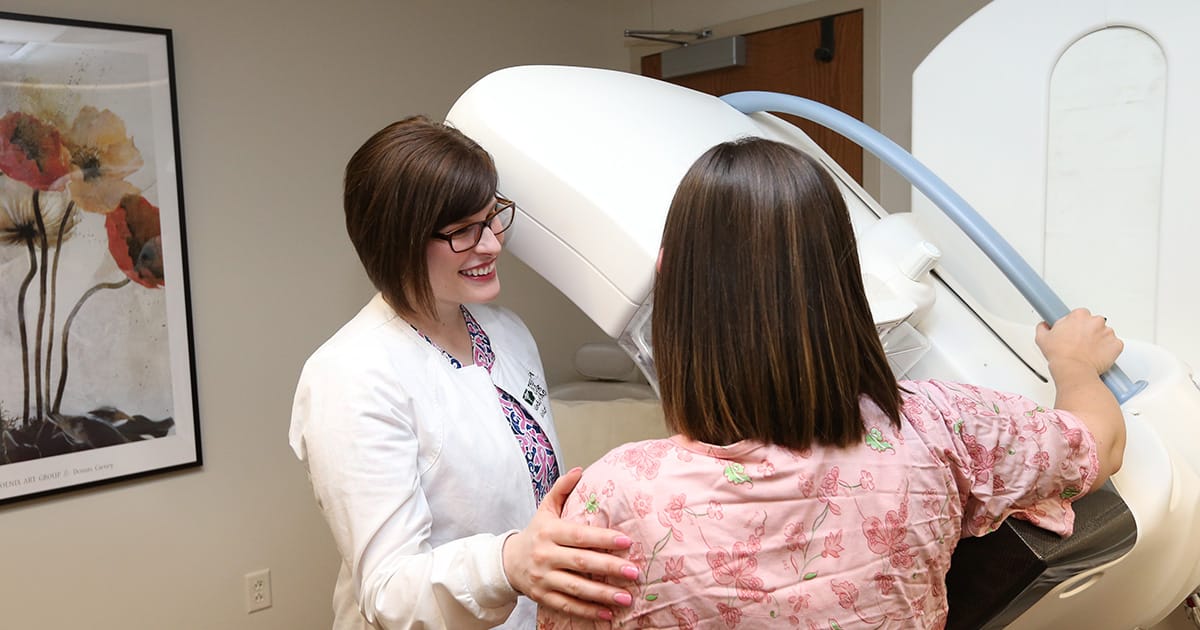
Recently, the medical field has made improvements in imaging tests used for the identification, diagnosis, and monitoring progress of breast cancer. Traditional mammogram technology has only allowed for two-dimensional viewing of the resulting x-ray images until recently. Digital breast tomosynthesis is a sophisticated type of mammography or breast imaging that utilizes computer regeneration and a system that applies low-dose x-rays to produce three-dimensional breast images. It works by synchronization of multiple images of the breast taken from different angles. This mechanism reduces the chance any abnormality would be masked by overlapping compressed breast tissue like in traditional mammograms. Another addition to breast cancer imaging is called optical breast imaging. Optical breast imaging utilizes NIR or near-infrared light to evaluate the visual properties of the breast tissues. The light aimed through the breast is scattered or absorbed by the tissues, and detectors record the remaining light. The images of the breast are reconstructed by advanced computer algorithms based on the light response recorded. Both digital breast tomosynthesis and optical breast cancer imaging has proven effective in the early detection of breast cancer.
Learn about perhaps the most significant advancement made in identified risk factors for breast cancer now.
BRCA Gene Mutations
BRCA gene mutations are gene abnormalities detected by DNA analysis in the BRCA1 and BRCA2 genes that express breast cancer susceptibility. This BRCA gene testing is reserved for individuals who, based on familial history, are likely to have inherited a mutation. However, this diagnostic test is helpful because up to ten percent of breast cancers and fifteen percent of ovarian cancers are attributed to BRCA gene mutations. Both men and women with specific BRCA gene mutations are at a higher risk of developing breast and ovarian (if applicable) cancers. Having the ability to test for such mutations provides individuals with the knowledge to take specific measures to increase the chances of early detection and reduce their risk of developing cancer. An increase in the frequency of breast cancer screening or surveillance involves having magnetic resonance imaging or MRIs and mammograms done yearly. For some individuals with a BRCA2 gene mutation, medication is available to lower the risk of developing breast cancer. Individuals who have a BRCA gene mutation also have the option of undergoing a preventative mastectomy to decrease the risk of developing breast cancer by ninety percent.
Learn more about advancements made in gene mutations associated with breast cancer now.
Other Discovered Genetic Mutations

Aside from the BRCA genes, mutations that occur in several other genes are associated with the risk of developing breast cancer. These mutations are rare in comparison to BRCA genes mutations. Genetic identification of any of the following mutations can help affected individuals take measures for the prevention and early detection of breast cancer. The presence of one mutated ATM gene can stop the cells from being able to mend damaged DNA, increasing the risk of developing breast cancer. Mutations present in the BARD1 gene or in the BRIP1 gene are responsible for DNA repair that can also make an individual more susceptible to breast and ovarian cancers. Mutations that occur in the CDH1, CHEK2, and MRE11A genes all increase an individual's risk of breast-related cancers. A mutation in the MSH6 gene puts a patient at double the risk of developing cancer compared to a nonaffected individual. Furthermore, mutations in NBN, PALB2, PMS2, PTEN, RAD50, RAD51C, STK11, and TP53 genes are also closely linked to the increased risk for breast cancer. In rare cases, individuals who have inherited two abnormal gene duplicates of BRCA2, MRE11A, PALB2, RAD51C, BRIP1, NBN, or RAD50 genes have a compounded risk of developing certain kinds of cancers, including breast cancer.