10 Common Medications That Work Differently Depending on When You Take Them
The human body operates on a sophisticated internal clock system known as circadian rhythms, which regulate everything from hormone production to cellular repair processes throughout a 24-hour cycle. This biological timekeeper doesn't just influence when we feel sleepy or alert—it fundamentally affects how our bodies process, absorb, and respond to medications. The emerging field of chronotherapy has revealed that the timing of medication administration can dramatically impact drug efficacy, side effects, and therapeutic outcomes. Research spanning decades has demonstrated that many common medications work significantly better when taken at specific times of day, aligning with our body's natural rhythms. From blood pressure medications that are more effective when taken at bedtime to cholesterol-lowering drugs that work optimally during evening hours, the "when" of medication timing has proven to be just as crucial as the "what" and "how much." This revolutionary understanding challenges the traditional one-size-fits-all approach to medication scheduling and opens new possibilities for personalized medicine. Understanding these timing-dependent effects can help patients maximize therapeutic benefits while minimizing adverse reactions, ultimately leading to better health outcomes and improved quality of life.
1. Blood Pressure Medications - Nighttime Dosing for Maximum Cardiovascular Protection
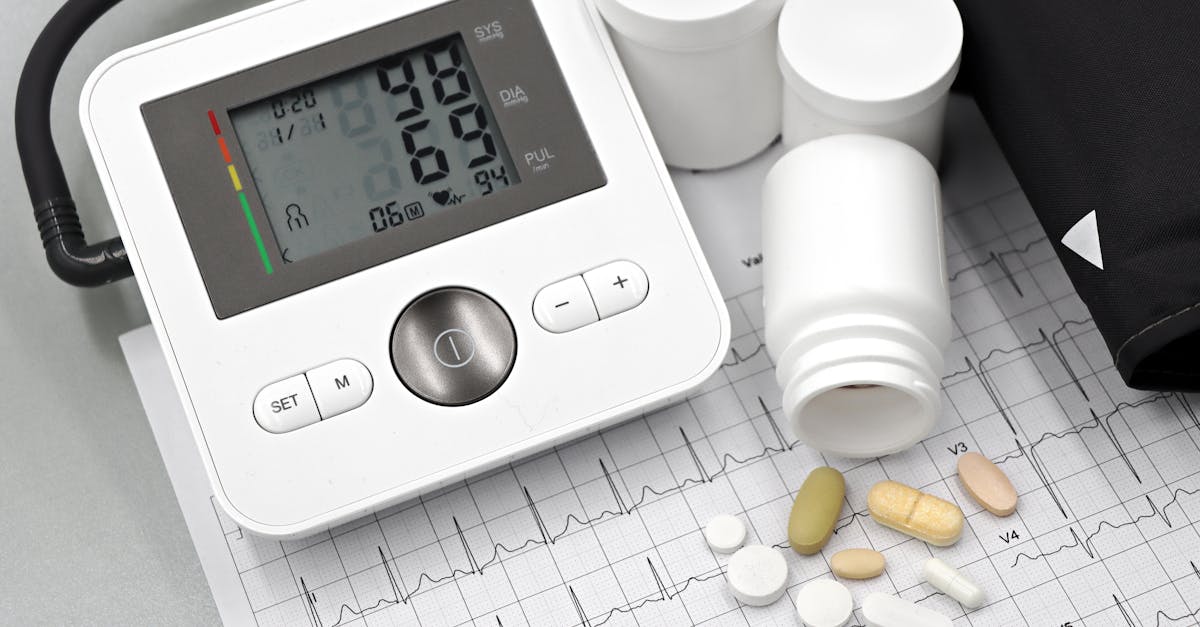
Blood pressure medications represent one of the most compelling examples of chronotherapy in action, with mounting evidence suggesting that bedtime dosing provides superior cardiovascular protection compared to morning administration. The landmark MAPEC study, involving over 3,000 patients followed for more than five years, demonstrated that taking at least one antihypertensive medication at bedtime reduced the risk of cardiovascular events by 61% compared to taking all medications in the morning. This dramatic difference stems from the body's natural circadian blood pressure pattern, where pressure typically dips during sleep and surges in the early morning hours. ACE inhibitors, ARBs (Angiotensin Receptor Blockers), and calcium channel blockers show enhanced efficacy when taken at night, as they can better control the dangerous morning blood pressure surge that coincides with increased heart attack and stroke risk. The kidneys also exhibit circadian variations in sodium handling and renin production, making evening dosing particularly effective for medications that target the renin-angiotensin system. Additionally, nighttime dosing helps counteract the natural reduction in nitric oxide production that occurs during sleep, maintaining better vascular function throughout the night. Patients who switch to bedtime dosing often experience not only better blood pressure control but also improved sleep quality, as the medications help maintain more stable cardiovascular function during rest periods.
2. Statins - Evening Administration for Optimal Cholesterol Management
Cholesterol-lowering medications, particularly statins, demonstrate remarkable timing-dependent efficacy that directly relates to the body's natural cholesterol production cycle. The liver produces approximately 70% of the body's cholesterol, with peak synthesis occurring during the early morning hours between 2 AM and 6 AM when dietary cholesterol intake is minimal. This nocturnal cholesterol production surge makes evening or bedtime administration of statins significantly more effective than morning dosing. Short-acting statins like simvastatin and lovastatin show the most pronounced timing effects, with studies revealing up to 30% greater cholesterol reduction when taken in the evening compared to morning administration. The enzyme HMG-CoA reductase, which statins inhibit, exhibits peak activity during these overnight hours, making the medications more potent when present in higher concentrations during this critical window. Longer-acting statins like atorvastatin and rosuvastatin show less dramatic timing effects due to their extended half-lives, but even these medications often perform better with evening dosing. The timing advantage extends beyond cholesterol numbers—patients taking statins in the evening often experience fewer muscle-related side effects, possibly due to better alignment with natural muscle repair cycles. Furthermore, evening statin administration may provide additional cardiovascular benefits by reducing inflammatory markers and improving endothelial function during the vulnerable overnight period when many cardiac events occur.
3. Proton Pump Inhibitors - Strategic Timing for Acid Suppression

Proton pump inhibitors (PPIs) like omeprazole, lansoprazole, and esomeprazole require precise timing to achieve optimal acid suppression, as their mechanism of action depends on the activation state of gastric parietal cells. These medications work by irreversibly binding to the hydrogen-potassium ATPase enzyme, but they can only do so when the proton pumps are actively secreting acid. Stomach acid production follows a distinct circadian pattern, with minimal secretion during fasting states and peak activity triggered by meals and vagal stimulation. For maximum effectiveness, PPIs should be taken 30-60 minutes before the first meal of the day, allowing the medication to be absorbed and reach the parietal cells just as acid production ramps up in response to food intake. This timing strategy ensures that the maximum number of proton pumps are in their active state when the drug arrives, leading to more complete and sustained acid suppression. Taking PPIs with food or too close to meals can actually reduce their effectiveness, as food can interfere with absorption and the proton pumps may already be maximally stimulated. The timing principle also explains why twice-daily PPI regimens work best when the second dose is taken before dinner rather than at bedtime. Patients with nocturnal acid breakthrough may benefit from taking a second dose 30 minutes before their evening meal, providing better 24-hour acid control and improved healing of acid-related conditions like GERD and peptic ulcers.
4. Thyroid Hormones - Morning Dosing for Natural Rhythm Alignment

Thyroid hormone replacement therapy with levothyroxine requires careful timing consideration to mimic the body's natural thyroid hormone production pattern and ensure optimal absorption. The thyroid gland naturally produces the highest levels of thyroid hormones in the early morning hours, with TSH (thyroid-stimulating hormone) peaking during sleep and triggering increased hormone synthesis before awakening. Taking levothyroxine first thing in the morning on an empty stomach best replicates this natural rhythm and provides the steady hormone levels needed throughout the day. The medication requires an acidic environment for optimal dissolution and absorption, which is naturally present in the fasting stomach during morning hours. Food, particularly high-fiber foods, calcium, iron supplements, and coffee, can significantly impair levothyroxine absorption by up to 40%, making the timing of administration crucial for therapeutic success. The four-hour window between taking levothyroxine and consuming food or other medications is essential for maximizing bioavailability. Some patients who experience insomnia or anxiety with morning dosing may benefit from bedtime administration, but this requires strict adherence to a four-hour fast and careful monitoring of thyroid function tests. Recent studies have also explored weekly dosing regimens, which may provide more consistent hormone levels for some patients while simplifying the dosing schedule. The key to successful thyroid hormone replacement lies not just in the correct dose, but in consistent timing that allows the body to maintain steady hormone levels throughout the day.
5. Corticosteroids - Morning Administration to Minimize Adrenal Suppression

Corticosteroid medications like prednisone and prednisolone require morning administration to align with the body's natural cortisol production cycle and minimize the risk of adrenal suppression. The hypothalamic-pituitary-adrenal (HPA) axis follows a distinct circadian rhythm, with cortisol levels peaking in the early morning hours around 8 AM and gradually declining throughout the day to reach their lowest point around midnight. This natural pattern serves to provide energy and alertness for daily activities while allowing the body to rest and repair during sleep. When corticosteroids are taken in the morning, they supplement the natural cortisol peak and then decline throughout the day, closely mimicking the body's physiological pattern. This timing strategy helps preserve the natural HPA axis function and reduces the risk of adrenal suppression that can occur with long-term steroid use. Taking corticosteroids later in the day or at bedtime can disrupt this natural rhythm, leading to elevated cortisol levels during times when they should be low, potentially causing insomnia, mood changes, and metabolic disturbances. Morning dosing also takes advantage of the body's natural anti-inflammatory mechanisms, as cortisol naturally helps resolve inflammation that may have accumulated overnight. For patients requiring multiple daily doses, the largest dose should still be given in the morning, with smaller doses spaced throughout the day. Understanding and respecting this timing principle is crucial for maximizing therapeutic benefits while minimizing the serious side effects associated with long-term corticosteroid use.
6. Antidepressants - Timing Based on Activation vs. Sedation Profiles

The optimal timing for antidepressant medications varies significantly based on their specific pharmacological profiles, particularly their effects on energy, sleep, and alertness. Activating antidepressants such as fluoxetine (Prozac), sertraline (Zoloft), and bupropion (Wellbutrin) are best taken in the morning to harness their energizing effects and prevent sleep disturbances. These medications can increase alertness, motivation, and energy levels, making morning administration ideal for supporting daytime functioning while avoiding nighttime insomnia. Conversely, sedating antidepressants like trazodone, mirtazapine, and some tricyclic antidepressants are more appropriately taken in the evening or at bedtime, as they can cause drowsiness and help improve sleep quality in patients with depression-related insomnia. The timing of antidepressant administration also affects side effect profiles—taking activating medications at night can lead to insomnia, vivid dreams, and restless sleep, while taking sedating medications in the morning can cause daytime drowsiness and impair cognitive function. SSRIs and SNRIs may also affect REM sleep patterns, and timing can influence whether these effects are therapeutic or disruptive. Some patients may need to adjust timing based on individual responses—for example, those who experience initial activation from typically sedating medications might benefit from morning dosing. Additionally, the timing of antidepressant administration can affect sexual side effects, with some patients finding that evening dosing reduces the impact on sexual function. Understanding these timing principles allows healthcare providers to optimize both therapeutic efficacy and quality of life for patients with depression.
7. Diuretics - Morning Dosing to Prevent Sleep Disruption
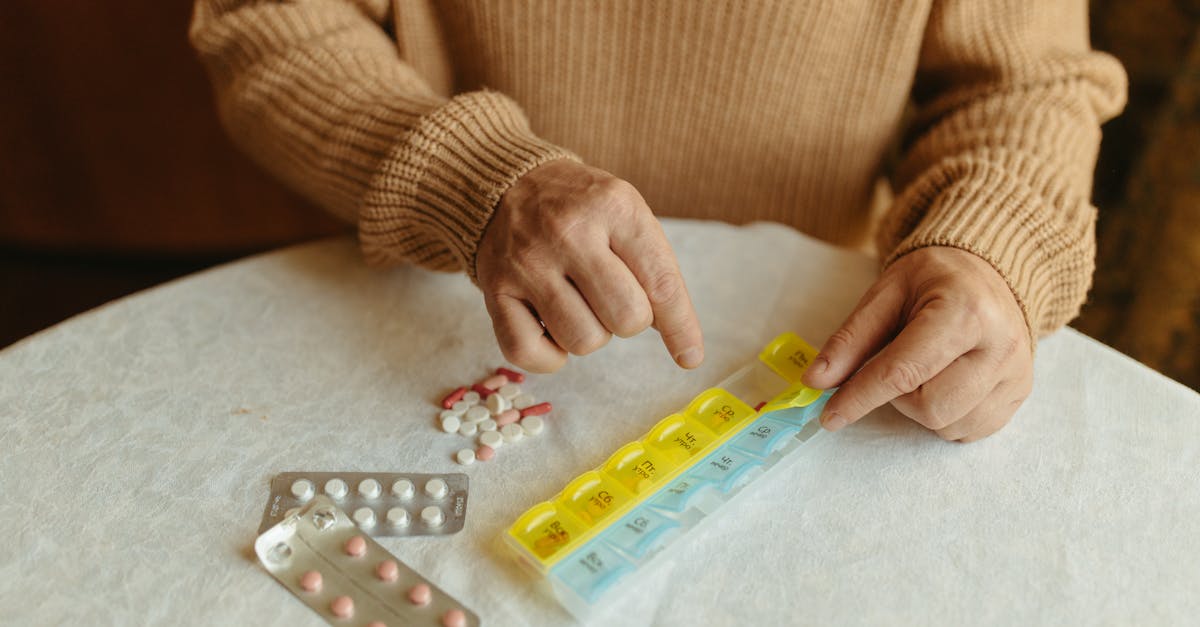
Diuretic medications, commonly known as "water pills," require strategic morning timing to maximize therapeutic benefits while minimizing lifestyle disruption, particularly sleep interference. These medications work by increasing urine production to reduce fluid retention and lower blood pressure, but their timing can significantly impact patient compliance and quality of life. Taking diuretics in the morning allows the peak diuretic effect to occur during daytime hours when access to bathroom facilities is convenient and sleep is not disrupted by frequent urination. The kidneys naturally exhibit circadian variations in function, with glomerular filtration rate and sodium excretion typically higher during daytime hours, making morning administration physiologically advantageous. Loop diuretics like furosemide have a rapid onset of action within one hour and peak effects lasting 6-8 hours, making early morning dosing ideal for achieving maximum fluid removal during active hours. Thiazide and thiazide-like diuretics have longer durations of action but still benefit from morning administration to align peak effects with natural kidney function patterns. Patients who take diuretics in the evening often experience significant sleep disruption due to nocturia (frequent nighttime urination), which can lead to poor medication compliance and worsened cardiovascular outcomes. For patients requiring twice-daily dosing, the second dose should be taken in the early afternoon rather than evening to maintain the sleep-protective timing strategy. This timing approach not only improves patient comfort and compliance but also may provide better long-term cardiovascular protection by ensuring consistent medication adherence.
8. Antihistamines - Timing Based on Sedating vs. Non-Sedating Properties
Antihistamine medications require careful timing consideration based on their sedating properties and intended therapeutic goals, as different generations of these drugs have vastly different effects on alertness and cognitive function. First-generation antihistamines like diphenhydramine (Benadryl) and chlorpheniramine readily cross the blood-brain barrier and cause significant sedation, making them ideal for bedtime administration when treating allergies accompanied by sleep difficulties. These medications can provide dual benefits of allergy relief and sleep aid when taken 30-60 minutes before bedtime, as their sedating effects peak within 1-2 hours of administration. However, morning or daytime use of sedating antihistamines can impair cognitive function, reaction time, and driving ability, sometimes to a degree comparable to alcohol intoxication. Second and third-generation antihistamines like loratadine (Claritin), cetirizine (Zyrtec), and fexofenadine (Allegra) are designed to minimize central nervous system penetration and can be taken at any time of day without significant sedation. However, even these "non-sedating" antihistamines can cause mild drowsiness in some individuals, particularly cetirizine, which may be better tolerated when taken in the evening. The timing of antihistamine administration also affects their interaction with other medications—sedating antihistamines can potentiate the effects of alcohol, benzodiazepines, and other central nervous system depressants, making evening timing safer for avoiding dangerous interactions. For seasonal allergies, taking non-sedating antihistamines in the morning provides all-day protection during peak pollen exposure times, while bedtime dosing may be insufficient for daytime symptom control.
9. Aspirin - Low-Dose Timing for Cardiovascular Protection

Low-dose aspirin therapy for cardiovascular protection demonstrates significant timing-dependent effects that can influence both efficacy and safety profiles. Traditional recommendations have favored morning administration, but emerging research suggests that bedtime dosing may provide superior cardiovascular benefits with potentially fewer side effects. The rationale for bedtime aspirin centers on the body's natural circadian variations in cardiovascular risk, with heart attacks and strokes occurring most frequently in the early morning hours between 6 AM and noon. This "morning surge" in cardiovascular events coincides with increased platelet aggregation, elevated blood pressure, and enhanced coagulation activity that occurs upon awakening. Taking aspirin at bedtime ensures peak antiplatelet effects during these vulnerable morning hours when cardiovascular events are most likely to occur. Studies have shown that bedtime aspirin administration results in better blood pressure control, particularly in patients with hypertension, and may provide more consistent platelet inhibition throughout the 24-hour period. The timing may also affect gastrointestinal side effects—some patients experience less stomach irritation with bedtime dosing, possibly due to the protective effects of sleep on gastric mucosa and reduced acid production during overnight hours. However, individual patient factors must be considered, as some people may experience sleep disruption or increased bleeding risk with bedtime dosing. The optimal timing may also depend on other medications in the patient's regimen, particularly other anticoagulants or blood pressure medications that could interact with aspirin's effects. Healthcare providers should consider individual patient risk profiles and lifestyle factors when determining the most appropriate timing for low-dose aspirin therapy.
10. Osteoporosis Medications - Empty Stomach Morning Dosing for Optimal Absorption

Bisphosphonate medications used to treat osteoporosis, including alendronate (Fosamax), risedronate (Actonel), and ibandronate (Boniva), require extremely specific timing protocols to ensure adequate absorption and prevent serious side effects. These medications have notoriously poor bioavailability, with less than 1% of the oral dose typically absorbed under optimal conditions, making precise timing crucial for therapeutic success. The standard protocol requires taking bisphosphonates first thing in the morning on a completely empty stomach with a full glass of plain water, followed by remaining upright and fasting for at least 30-60 minutes before consuming any food, beverages, or other medications. This timing strategy is essential because food, beverages other than water, and other medications can reduce absorption by up to 90%, essentially negating the therapeutic benefit. The morning timing also aligns with natural bone remodeling cycles, as bone resorption (breakdown) tends to peak during nighttime hours, making morning administration optimal for inhibiting this process. Calcium, magnesium, iron supplements, and even coffee or orange juice can form complexes with bisphosphonates that prevent absorption, emphasizing the importance of the fasting period. The upright positioning requirement is critical for preventing esophageal irritation and potential ulceration, as these medications can cause severe esophageal damage if they become lodged in the esophagus. Some patients who cannot tolerate the strict morning regimen may benefit from weekly or monthly formulations that require the same timing principles but less frequent dosing. Patient education about proper timing and administration is crucial, as improper timing can lead to treatment failure and continued bone loss despite medication use.
11. Implementing Chronotherapy for Better Health Outcomes

The science of chronotherapy represents a paradigm shift in how we approach medication management, moving beyond the simple directive of "take as directed" to a more nuanced understanding of optimal timing for therapeutic success. The ten medication categories discussed demonstrate that timing is not merely a convenience factor but a critical component of drug efficacy, safety, and patient outcomes. From blood pressure medications that provide superior cardiovascular protection when taken at bedtime to thyroid hormones that require morning administration for optimal absorption, these examples illustrate the profound impact that circadian biology has on pharmacotherapy. Healthcare providers and patients must work together to implement timing strategies that align with both physiological principles and practical lifestyle considerations. This may require adjusting work schedules, meal times, or sleep patterns to accommodate optimal medication timing, but the potential benefits—improved efficacy, reduced side effects, and better long-term health outcomes—justify these efforts. Technology can play a supporting role through smartphone apps, smart pill dispensers, and reminder systems that help patients maintain consistent timing schedules. As our understanding of chronobiology continues to evolve, we can expect to see more personalized approaches to medication timing based on individual circadian patterns, genetic factors, and lifestyle preferences. The future of medicine