10 Must-Know Insights to Decode Your BMI and Boost Your Health
Body Mass Index, commonly known as BMI, is a simple calculation used to assess whether a person has a healthy body weight for a given height. Developed by Belgian mathematician Adolphe Quetelet in the 19th century, BMI is calculated by dividing a person's weight in kilograms by the square of their height in meters. Despite its simplicity, BMI remains a widely used tool in health assessments globally. The significance of BMI lies in its ability to serve as a preliminary screening tool. While it doesn’t measure body fat directly, it correlates well with more precise measures of body fat obtained through advanced techniques like dual-energy X-ray absorptiometry (DEXA) scans. Health professionals often use BMI as a starting point to determine whether further testing is necessary. However, it’s vital to remember that BMI is just one piece of the puzzle. It should be considered alongside other factors such as age, sex, muscle mass, and overall health to develop a comprehensive understanding of an individual's health status. This article will delve into the intricacies of BMI, offering 10 essential insights to help you harness this tool for a healthier lifestyle.
1. The Science Behind BMI

The scientific foundation of BMI is rooted in its ability to provide a rough estimate of body fatness, which is a critical factor in assessing health risks. BMI is calculated by dividing a person's weight in kilograms by the square of their height in meters, yielding a single number that classifies individuals into categories such as underweight, normal weight, overweight, and obese. This classification helps in identifying potential health risks associated with each category. For instance, a higher BMI often correlates with an increased risk of chronic diseases such as heart disease, diabetes, and certain cancers. The relationship between BMI and health outcomes is well-documented in scientific literature. Numerous studies have demonstrated that individuals with a BMI in the overweight or obese range are more likely to experience adverse health outcomes compared to those with a BMI in the normal range. However, it is essential to recognize that BMI is not a perfect measure. It does not account for variations in muscle mass, bone density, and distribution of fat, which can vary significantly among individuals. Therefore, while BMI is a valuable tool, it should be used in conjunction with other assessments to provide a more comprehensive picture of an individual's health.
2. Interpreting Your BMI Results

Interpreting BMI results involves understanding the categories defined by the World Health Organization (WHO) and other health organizations. A BMI of less than 18.5 is considered underweight, a BMI between 18.5 and 24.9 is classified as normal weight, a BMI between 25 and 29.9 is categorized as overweight, and a BMI of 30 or higher is classified as obese. These categories are used to identify individuals who may be at risk for health problems related to their weight. It's important to approach BMI results with a nuanced perspective. For example, an athlete with a high muscle mass may have a BMI that categorizes them as overweight or obese, despite having a low body fat percentage. Conversely, an individual with a normal BMI may still have excess body fat, particularly if they lead a sedentary lifestyle. Therefore, while BMI can provide a useful initial assessment, it should be complemented with additional measurements such as waist circumference, body fat percentage, and lifestyle evaluations to gain a more accurate understanding of an individual's health.
3. Limitations and Criticisms of BMI

Despite its widespread use, BMI has faced criticism for its limitations in accurately assessing an individual's health. One of the primary criticisms is that BMI does not differentiate between muscle and fat. As a result, individuals with high muscle mass, such as athletes, may be classified as overweight or obese, even though they have low body fat and are in excellent health. Similarly, BMI does not account for the distribution of body fat, which is an important factor in assessing health risks. For instance, abdominal fat is more strongly associated with health risks than fat in other areas of the body. Another limitation of BMI is its inability to account for differences in body composition across different ethnic groups. Research has shown that individuals from different ethnic backgrounds may have different body fat distributions and health risks at the same BMI. For example, Asian populations may experience health risks at lower BMI thresholds compared to Caucasian populations. These limitations highlight the need for a more comprehensive approach to assessing an individual's health, one that considers a range of factors beyond BMI alone.
4. The Role of Genetics in BMI

Genetics plays a significant role in determining an individual's BMI and body composition. Research has shown that genetic factors can influence body weight and fat distribution, accounting for approximately 40-70% of the variation in BMI among individuals. Specific genes have been identified that are associated with body weight regulation, appetite control, and metabolism. For instance, variations in the FTO gene have been linked to an increased risk of obesity. Understanding the genetic influences on BMI can provide valuable insights into the complex interplay between genetics and lifestyle factors in determining an individual's weight. While genetics can predispose individuals to higher or lower BMI, environmental factors such as diet, physical activity, and lifestyle choices also play a crucial role. Recognizing the genetic component of BMI can help individuals and healthcare professionals develop personalized strategies for weight management and health improvement.
5. The Impact of Lifestyle on BMI

Lifestyle factors, including diet and physical activity, have a profound impact on an individual's BMI. A balanced diet rich in fruits, vegetables, whole grains, and lean proteins can help maintain a healthy weight and prevent excess weight gain. Conversely, diets high in processed foods, sugars, and unhealthy fats are associated with higher BMI and increased risk of obesity-related health conditions. Regular physical activity is also essential for maintaining a healthy BMI, as it helps burn calories, build muscle, and improve overall fitness. In addition to diet and exercise, other lifestyle factors such as sleep, stress, and mental health can influence BMI. Poor sleep quality and chronic stress have been linked to weight gain and higher BMI, as they can disrupt hormonal balance and lead to unhealthy eating habits. Prioritizing a healthy lifestyle that includes a balanced diet, regular physical activity, adequate sleep, and stress management can help individuals achieve and maintain a healthy BMI, reducing the risk of associated health problems.
6. BMI and Chronic Disease Risk

BMI is a valuable tool for assessing the risk of chronic diseases associated with excess body weight. Numerous studies have shown that individuals with a higher BMI are at increased risk of developing conditions such as type 2 diabetes, cardiovascular disease, and certain types of cancer. For example, obesity is a major risk factor for type 2 diabetes, as excess body fat can lead to insulin resistance and impaired glucose metabolism. Similarly, a higher BMI is associated with an increased risk of hypertension, dyslipidemia, and coronary artery disease. Understanding the relationship between BMI and chronic disease risk is essential for developing effective prevention and management strategies. Healthcare professionals often use BMI as part of a comprehensive risk assessment to identify individuals who may benefit from lifestyle interventions or medical treatment to reduce their risk of chronic diseases. By maintaining a healthy BMI through diet, exercise, and lifestyle changes, individuals can significantly reduce their risk of developing these conditions and improve their overall health and well-being.
7. BMI in Children and Adolescents

Assessing BMI in children and adolescents requires a different approach than in adults, as their bodies are still growing and developing. For this age group, BMI is calculated using the same formula as for adults, but the results are interpreted using age- and sex-specific percentiles. These percentiles are based on growth charts developed by the Centers for Disease Control and Prevention (CDC) and help determine whether a child is underweight, at a healthy weight, overweight, or obese. Monitoring BMI in children and adolescents is important for identifying potential health risks and promoting healthy growth and development. Early intervention can help prevent the development of obesity-related health problems and establish healthy habits that can last a lifetime. Parents and caregivers play a crucial role in supporting healthy behaviors, such as providing nutritious meals, encouraging physical activity, and promoting positive body image. By focusing on overall health and well-being rather than weight alone, families can help children achieve and maintain a healthy BMI.
8. BMI and Aging

As individuals age, changes in body composition and metabolism can impact BMI and overall health. Older adults often experience a decrease in muscle mass and an increase in body fat, which can affect their BMI and health risk profile. Maintaining a healthy BMI in older age is important for reducing the risk of chronic diseases, maintaining mobility, and promoting independence. Older adults may face unique challenges in managing their BMI, such as age-related changes in metabolism, decreased physical activity, and dietary changes. It is important for older adults to focus on maintaining muscle mass through strength training exercises and consuming adequate protein in their diet. Additionally, regular physical activity and a balanced diet can help older adults maintain a healthy BMI and improve their overall quality of life. Healthcare professionals can provide guidance and support to help older adults navigate these challenges and achieve their health goals.
9. Alternative Measures to BMI
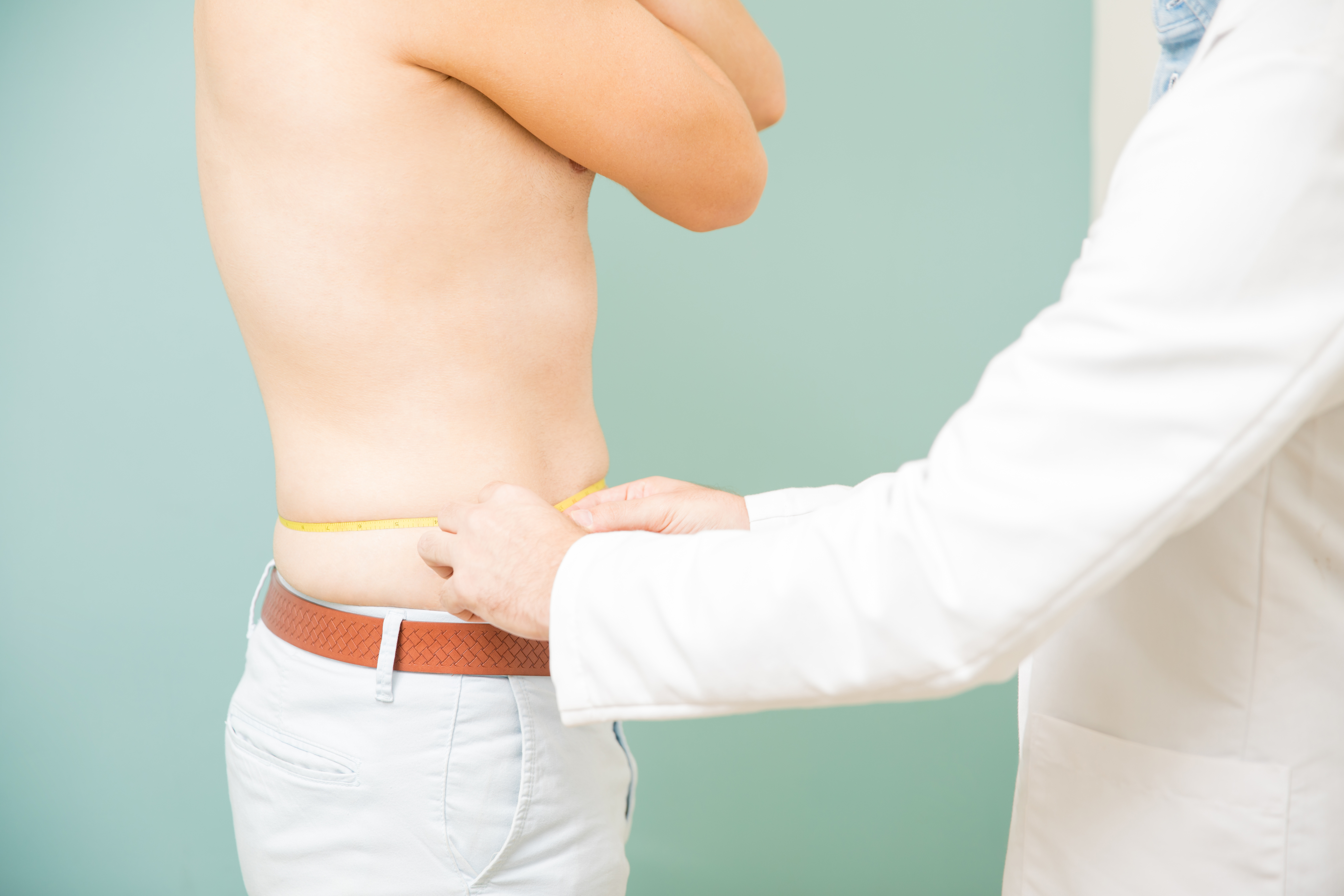
While BMI is a valuable tool for assessing body weight and health risk, it is not the only measure available. Alternative measures, such as waist circumference, waist-to-hip ratio, and body fat percentage, can provide additional insights into an individual's health and risk of chronic diseases. Waist circumference is a simple measure of abdominal fat, which is a strong predictor of health risk. A higher waist circumference is associated with an increased risk of metabolic syndrome, cardiovascular disease, and type 2 diabetes. Body fat percentage, which can be measured using methods such as bioelectrical impedance analysis or DEXA scans, provides a more accurate assessment of body composition than BMI alone. These alternative measures can be used in conjunction with BMI to provide a more comprehensive assessment of an individual's health and guide personalized interventions. By considering multiple measures of body composition, individuals and healthcare professionals can develop more effective strategies for achieving and maintaining a healthy weight and reducing the risk of chronic diseases.
10. BMI and Mental Health: The Overlooked Connection

While BMI is primarily used as a physical health metric, it also intersects with mental health in powerful ways. Individuals with higher or lower BMI may experience stigma, body dissatisfaction, or low self-esteem, all of which can negatively impact mental well-being. Research shows that weight-related stigma can lead to increased levels of anxiety, depression, and disordered eating behaviors—creating a cycle that complicates both physical and emotional health. On the flip side, poor mental health can contribute to lifestyle habits that affect BMI, such as emotional eating or reduced motivation for physical activity. Recognizing the bidirectional relationship between BMI and mental health is essential for holistic wellness. Healthcare providers should consider the psychological implications of BMI discussions, encouraging compassionate, non-judgmental support that promotes both physical and mental health.
Beyond the Numbers: Building a Healthier You

Understanding your BMI and its implications is a crucial step towards achieving and maintaining a healthier lifestyle. While BMI is a valuable tool for assessing body weight and health risk, it is important to consider its limitations and use it in conjunction with other measures and assessments. By focusing on a holistic approach to health that includes a balanced diet, regular physical activity, adequate sleep, and stress management, individuals can achieve and maintain a healthy BMI and reduce their risk of chronic diseases. Practical steps for achieving a healthier BMI include setting realistic goals, making gradual changes to diet and exercise habits, and seeking support from healthcare professionals or support groups. It is also important to focus on overall health and well-being rather than weight alone, as health is influenced by a variety of factors beyond body weight. By taking a comprehensive approach to health, individuals can improve their quality of life and achieve long-term success in maintaining a healthy BMI.
