11 Signs of Vitamin D Deficiency and How to Address It
Vitamin D deficiency has emerged as one of the most widespread nutritional deficiencies of the 21st century, affecting an estimated one billion people worldwide across all age groups and ethnicities. Often dubbed the "sunshine vitamin," vitamin D plays a crucial role far beyond its well-known function in bone health, serving as a hormone that regulates over 1,000 genes in the human body. The modern lifestyle, characterized by increased indoor activities, extensive use of sunscreen, limited dietary sources, and geographic factors, has created a perfect storm for widespread deficiency. This silent epidemic manifests through a complex array of symptoms that are often misattributed to other conditions, making it particularly challenging to diagnose without proper testing. Understanding the multifaceted signs of vitamin D deficiency is essential for maintaining optimal health, as this vital nutrient influences immune function, cardiovascular health, mental well-being, and numerous other physiological processes. The following exploration will illuminate eleven key indicators of vitamin D deficiency and provide evidence-based strategies for restoration and maintenance of adequate levels.
1. Frequent Illness and Compromised Immune Function

One of the most prominent signs of vitamin D deficiency is an increased susceptibility to infections and a generally compromised immune system. Vitamin D plays a pivotal role in maintaining immune homeostasis by regulating both innate and adaptive immune responses. Research has consistently demonstrated that individuals with low vitamin D levels experience more frequent respiratory tract infections, including common colds, flu, and pneumonia. The vitamin enhances the pathogen-fighting effects of monocytes and macrophages, white blood cells that are crucial components of immune defense, while also decreasing inflammation. Studies have shown that people with vitamin D levels below 30 ng/ml are significantly more likely to report recent upper respiratory tract infections compared to those with adequate levels. Furthermore, vitamin D deficiency has been linked to increased severity and duration of illnesses, as the vitamin is essential for the production of antimicrobial peptides like cathelicidin, which help destroy bacteria, viruses, and fungi. To address this issue, maintaining optimal vitamin D levels through supplementation, safe sun exposure, and dietary sources can significantly strengthen immune function and reduce the frequency and severity of infections.
2. Persistent Fatigue and Weakness

Chronic fatigue and unexplained weakness represent another hallmark of vitamin D deficiency that significantly impacts quality of life. This overwhelming sense of tiredness often persists despite adequate sleep and rest, leaving individuals feeling drained and unable to perform daily activities with their usual vigor. The mechanism behind this fatigue is multifaceted, involving vitamin D's role in cellular energy production and muscle function. Research indicates that vitamin D receptors are present in muscle tissue, and deficiency can lead to muscle weakness, reduced physical performance, and increased perception of effort during physical activities. A landmark study involving healthcare workers found that those with severe vitamin D deficiency were significantly more likely to report fatigue compared to their colleagues with adequate levels. Additionally, vitamin D deficiency affects mitochondrial function, the cellular powerhouses responsible for energy production, potentially explaining the profound exhaustion experienced by deficient individuals. The fatigue associated with vitamin D deficiency is often accompanied by a general sense of malaise and reduced motivation. Addressing this deficiency through targeted supplementation has been shown to improve energy levels and reduce fatigue in numerous clinical trials, with many individuals reporting noticeable improvements in vitality within weeks of beginning treatment.
3. Bone and Back Pain
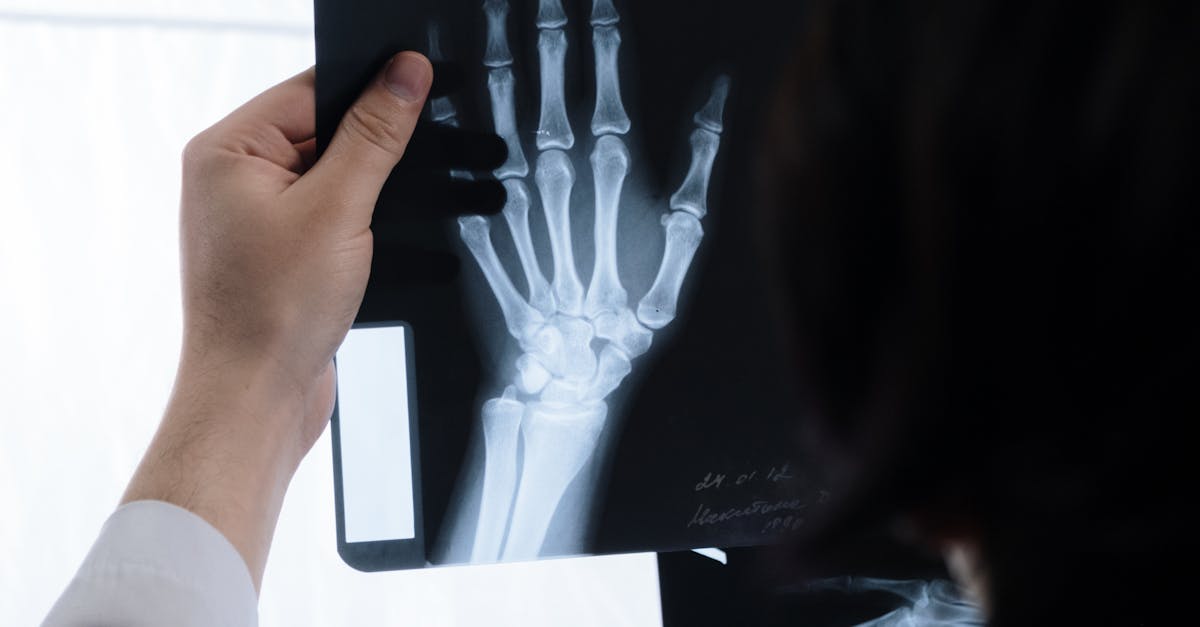
Bone and back pain, particularly in the lower back, serve as classic indicators of vitamin D deficiency due to the vitamin's fundamental role in calcium absorption and bone mineralization. Vitamin D facilitates the absorption of calcium and phosphorus from the intestines, and without adequate levels, the body can only absorb 10-15% of dietary calcium compared to 30-40% with sufficient vitamin D. This impaired absorption leads to secondary hyperparathyroidism, where the parathyroid glands increase hormone production to maintain blood calcium levels, ultimately resulting in bone demineralization and pain. Large-scale studies have consistently found strong correlations between low vitamin D levels and chronic lower back pain, with some research indicating that individuals with deficiency are twice as likely to experience bone pain. The pain associated with vitamin D deficiency is often described as deep, aching, and persistent, affecting the spine, pelvis, and ribs most commonly. Women are particularly susceptible to this symptom, especially during menopause when estrogen levels decline. Clinical trials have demonstrated that vitamin D supplementation can significantly reduce bone pain in deficient individuals, with improvements often noted within 6-12 weeks of treatment. The restoration of adequate vitamin D levels not only alleviates existing pain but also helps prevent future bone-related complications and maintains skeletal integrity throughout life.
4. Depression and Mood Disorders

The relationship between vitamin D deficiency and mental health, particularly depression and mood disorders, has garnered significant scientific attention in recent years. Vitamin D receptors are widely distributed throughout the brain, including areas responsible for mood regulation such as the hippocampus, hypothalamus, and substantia nigra. Research has revealed that vitamin D influences the synthesis of neurotransmitters like serotonin and dopamine, which are crucial for maintaining emotional balance and mental well-being. Epidemiological studies have consistently shown higher rates of depression among individuals with low vitamin D levels, with some research indicating that people with deficiency are 8-14% more likely to experience depression. Seasonal Affective Disorder (SAD), a type of depression that occurs during winter months when sun exposure is limited, provides compelling evidence of vitamin D's impact on mood. The deficiency can manifest as persistent sadness, hopelessness, irritability, anxiety, and cognitive difficulties including problems with concentration and decision-making. Meta-analyses of clinical trials have demonstrated that vitamin D supplementation can be an effective adjunctive treatment for depression, particularly in individuals with confirmed deficiency. The mood-enhancing effects of vitamin D restoration are thought to occur through multiple mechanisms, including improved neurotransmitter function, reduced inflammation in the brain, and enhanced neuroplasticity.
5. Impaired Wound Healing
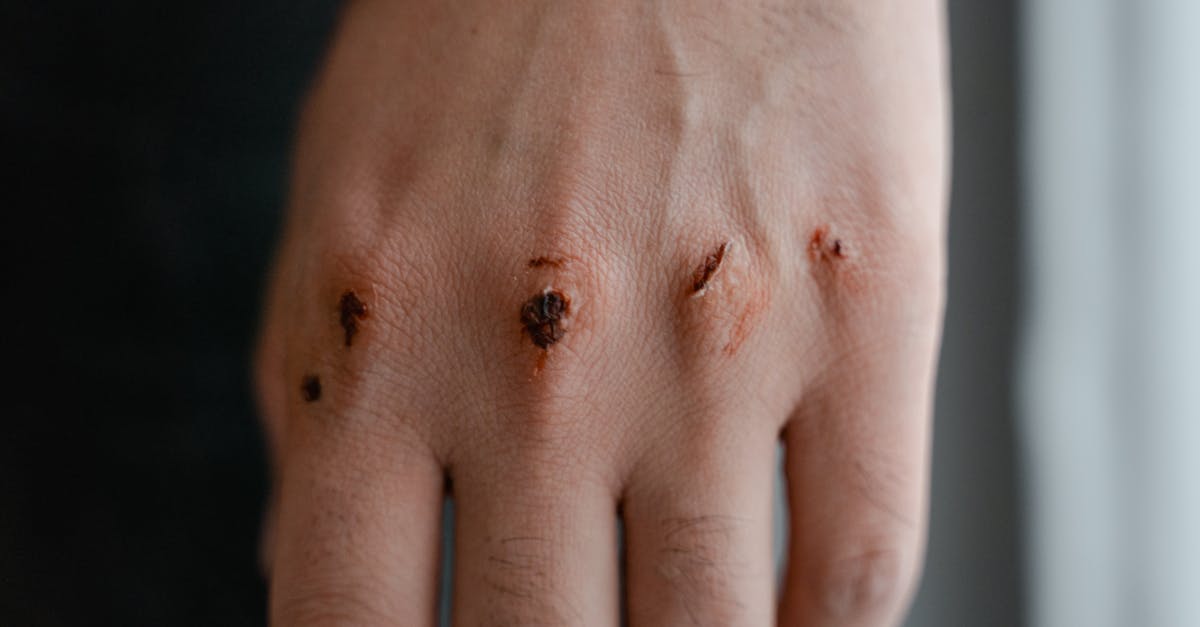
Delayed or impaired wound healing represents a less commonly recognized but significant sign of vitamin D deficiency that can have serious health implications. Vitamin D plays a crucial role in the wound healing process through multiple mechanisms, including the regulation of inflammation, promotion of cell proliferation, and enhancement of antimicrobial peptide production. Research has shown that vitamin D is essential for the proper function of keratinocytes, the primary cells of the epidermis, and influences the production of cathelicidin, an antimicrobial peptide that helps prevent wound infections. Studies involving surgical patients have found that those with adequate vitamin D levels experience faster healing times and reduced complications compared to deficient individuals. The vitamin also regulates the inflammatory response during wound healing, ensuring that inflammation is appropriately controlled to promote tissue repair without causing excessive damage. Deficient individuals may notice that cuts, scrapes, and surgical incisions take longer to heal, are more prone to infection, and may result in poor scar formation. Dental procedures are particularly affected, with vitamin D deficiency linked to delayed healing after tooth extractions and oral surgeries. Clinical research has demonstrated that optimizing vitamin D levels before and after surgical procedures can significantly improve healing outcomes, reduce infection rates, and minimize complications, making adequate vitamin D status an important consideration in both preventive care and treatment protocols.
6. Hair Loss and Thinning

Hair loss and thinning, particularly in women, can be an overlooked manifestation of vitamin D deficiency that significantly impacts self-esteem and quality of life. Vitamin D receptors are present in hair follicles, and the vitamin plays a crucial role in the hair growth cycle, specifically in the anagen (growth) phase. Research has established strong connections between vitamin D deficiency and various forms of alopecia, including androgenetic alopecia (pattern baldness) and alopecia areata (patchy hair loss). Studies have shown that women with female pattern hair loss have significantly lower vitamin D levels compared to controls, with severity of hair loss correlating inversely with vitamin D status. The mechanism involves vitamin D's role in keratinocyte proliferation and differentiation, processes essential for healthy hair follicle function. Additionally, vitamin D deficiency can lead to telogen effluvium, a condition characterized by diffuse hair thinning due to premature entry of hair follicles into the resting phase. Clinical observations have noted that individuals with severe vitamin D deficiency may experience not only scalp hair loss but also thinning of eyebrows and body hair. Treatment studies have shown promising results, with vitamin D supplementation leading to hair regrowth in deficient individuals, though improvements typically require several months of consistent treatment. The restoration of adequate vitamin D levels, combined with topical treatments when appropriate, can help reverse hair loss and promote healthy hair growth patterns.
7. Muscle Pain and Weakness
Muscle pain and weakness represent significant clinical manifestations of vitamin D deficiency that can substantially impact physical function and quality of life. Vitamin D receptors are abundantly present in skeletal muscle tissue, where the vitamin plays essential roles in muscle protein synthesis, calcium handling, and mitochondrial function. Research has consistently demonstrated that vitamin D deficiency leads to muscle weakness, particularly affecting proximal muscles of the arms and legs, resulting in difficulty with activities such as climbing stairs, rising from chairs, or lifting objects overhead. The pain associated with vitamin D deficiency is often described as deep, aching muscle discomfort that may be mistaken for fibromyalgia or other musculoskeletal conditions. Studies have shown that individuals with vitamin D levels below 20 ng/ml are significantly more likely to experience muscle pain and weakness compared to those with adequate levels. The mechanism involves impaired calcium transport within muscle cells, reduced muscle protein synthesis, and altered muscle fiber composition. Additionally, vitamin D deficiency can lead to increased muscle fatigue and reduced physical performance, with research showing decreased muscle strength and power output in deficient individuals. Clinical trials have demonstrated that vitamin D supplementation can improve muscle strength, reduce pain, and enhance physical performance in deficient individuals, with improvements typically observed within 6-12 weeks of treatment. The restoration of adequate vitamin D levels is particularly important for older adults, as it can help prevent falls and maintain functional independence.
8. Bone Loss and Increased Fracture Risk
Bone loss and increased fracture risk represent the most well-established and serious consequences of vitamin D deficiency, with implications that extend far beyond immediate injury concerns. Vitamin D is essential for maintaining bone mineral density through its regulation of calcium and phosphorus absorption, and deficiency leads to secondary hyperparathyroidism, resulting in accelerated bone resorption and decreased bone formation. Research has consistently shown that individuals with vitamin D deficiency have significantly lower bone mineral density and are at substantially higher risk for fractures, particularly of the hip, spine, and wrist. Studies indicate that people with vitamin D levels below 20 ng/ml have a 30-50% higher risk of hip fractures compared to those with adequate levels. The bone loss associated with vitamin D deficiency is often silent and progressive, with many individuals unaware of their deteriorating bone health until a fracture occurs. Dual-energy X-ray absorptiometry (DEXA) scans of deficient individuals frequently reveal osteopenia or osteoporosis, even in relatively young adults. The impact is particularly pronounced in postmenopausal women and older adults, populations already at increased risk for bone loss due to hormonal changes and aging. Clinical trials have demonstrated that vitamin D supplementation, particularly when combined with calcium, can significantly reduce fracture risk and slow bone loss. The prevention and treatment of vitamin D deficiency is considered a cornerstone of osteoporosis prevention and management, with major medical organizations recommending routine screening and supplementation for at-risk populations.
9. Cardiovascular Symptoms and Complications

Emerging research has revealed significant connections between vitamin D deficiency and cardiovascular health, with deficiency potentially contributing to various heart-related symptoms and complications. Vitamin D receptors are present throughout the cardiovascular system, including the heart muscle, blood vessels, and smooth muscle cells, where the vitamin influences blood pressure regulation, inflammation, and vascular function. Studies have shown that individuals with vitamin D deficiency are at increased risk for hypertension, with research indicating that low vitamin D levels are associated with a 30% higher risk of high blood pressure. The deficiency can also contribute to arterial stiffness and endothelial dysfunction, key factors in cardiovascular disease development. Clinical observations have noted that deficient individuals may experience symptoms such as chest pain, palpitations, and shortness of breath, though these symptoms are often attributed to other causes. Large-scale epidemiological studies have found associations between low vitamin D levels and increased risk of heart attack, stroke, and cardiovascular mortality. The mechanisms involve vitamin D's role in regulating the renin-angiotensin-aldosterone system, which controls blood pressure, as well as its anti-inflammatory effects on blood vessels. Additionally, vitamin D deficiency may contribute to insulin resistance and metabolic dysfunction, further increasing cardiovascular risk. While supplementation studies have shown mixed results for cardiovascular outcomes, maintaining adequate vitamin D levels is increasingly recognized as an important component of heart health, particularly for individuals with existing cardiovascular risk factors.
10. Cognitive Impairment and Memory Issues
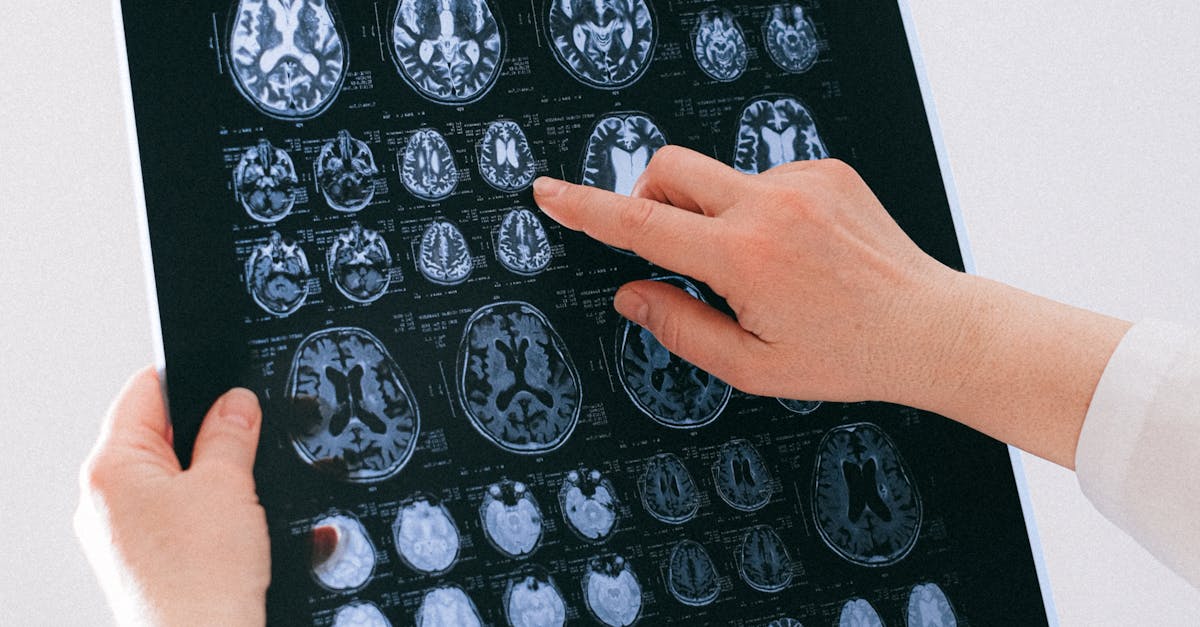
Cognitive impairment and memory issues represent increasingly recognized neurological manifestations of vitamin D deficiency that can significantly impact daily functioning and quality of life. Vitamin D receptors and metabolizing enzymes are widely distributed throughout the brain, including areas critical for learning, memory, and executive function such as the hippocampus, prefrontal cortex, and cerebellum. Research has demonstrated that vitamin D plays crucial roles in neuronal development, neurotransmitter synthesis, and neuroprotection, making deficiency particularly detrimental to cognitive health. Studies have consistently found associations between low vitamin D levels and cognitive decline, with deficient individuals showing poorer performance on tests of memory, attention, and processing speed. Longitudinal research has revealed that people with severe vitamin D deficiency have a significantly higher risk of developing dementia and Alzheimer's disease, with some studies showing a 60-120% increased risk compared to those with adequate levels. The cognitive symptoms of vitamin D deficiency may include difficulty concentrating, problems with short-term memory, reduced mental clarity often described as "brain fog," and impaired decision-making abilities. Neuroimaging studies have shown that vitamin D deficiency is associated with reduced brain volume and altered white matter integrity. Clinical trials investigating vitamin D supplementation for cognitive function have shown promising results, particularly in deficient individuals, with improvements in memory, attention, and overall cognitive performance observed in several studies. The neuroprotective effects of vitamin D restoration may be particularly important for aging populations and individuals at risk for neurodegenerative diseases.
11. Comprehensive Testing and Diagnosis Strategies
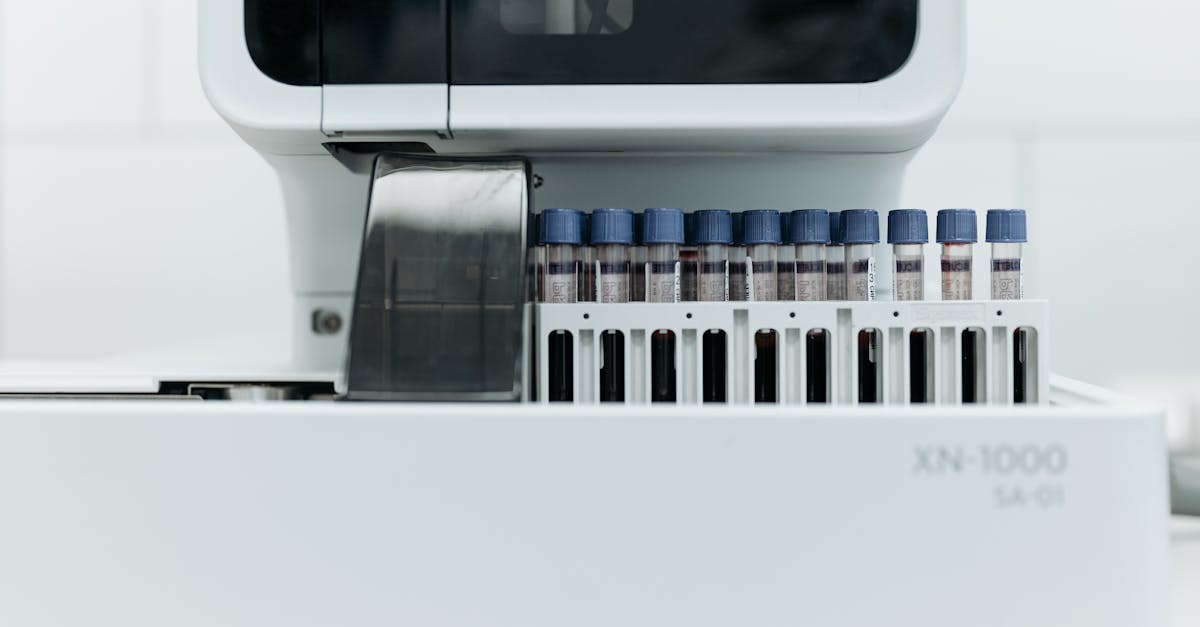
Accurate diagnosis of vitamin D deficiency requires comprehensive testing strategies that go beyond simple symptom assessment, as the clinical presentation can be subtle and overlap with numerous other conditions. The gold standard for assessing vitamin D status is the measurement of 25-hydroxyvitamin D [25(OH)D] in the blood, which reflects both dietary intake and endogenous production from sun exposure. Current medical consensus defines vitamin D deficiency as levels below 20 ng/ml (50 nmol/L), insufficiency as 20-29 ng/ml (50-74 nmol/L), and sufficiency as 30 ng/ml (75 nmol/L) or higher, though some experts advocate for optimal levels of 40-60 ng/ml. Testing should be considered for individuals presenting with suggestive symptoms, those at high risk due to limited sun exposure, dark skin pigmentation, advanced age, malabsorption disorders, or certain medications. Additional laboratory tests may include parathyroid hormone (PTH) levels, which are often elevated in vitamin D deficiency, and markers of bone metabolism such as alkaline phosphatase. Seasonal variation in vitamin D levels should be considered, with testing ideally performed during late winter or early spring when levels are typically at their lowest. For individuals with confirmed deficiency, follow-up testing is recommended 8-12 weeks after initiating treatment to assess response and guide ongoing management. Healthcare providers should also evaluate for underlying conditions that may contribute to deficiency, such as malabsorption syndromes, kidney or liver disease, and medications that interfere with vitamin D metabolism. Comprehensive assessment may include bone density testing for individuals with suspected bone loss and evaluation of other nutritional deficiencies that commonly coexist with vitamin D deficiency.
12. Evidence-Based Treatment and Prevention Strategies
Effective treatment and prevention of vitamin D deficiency requires a multifaceted approach combining supplementation, lifestyle modifications, and ongoing monitoring to achieve and maintain optimal levels. For individuals with confirmed deficiency, high-dose vitamin D supplementation is typically recommended, with common protocols including 50,000 IU weekly for 6-8 weeks followed by maintenance dosing of 1,000-2,000 IU daily. The choice between vitamin D2 (ergocalciferol) and vitamin D3 (cholecalciferol) is important, as research consistently shows that vitamin D3 is more effective at raising and maintaining blood levels. Safe sun exposure remains a natural and effective method for vitamin D production, with recommendations for 10-30 minutes of midday sun exposure several times per week, depending on skin type, geographic location, and season. However, sun exposure must be balanced with skin cancer risk, making supplementation often more practical and reliable. Dietary sources, while limited, include fatty fish, fortified foods, and egg yolks, though it's difficult to achieve adequate levels through diet alone. For individuals with malabsorption issues, higher doses or alternative formulations such as sublingual or topical preparations may be necessary. Prevention strategies should focus on identifying and addressing risk factors, including adequate supplementation during pregnancy and breastfeeding, ensuring sufficient intake in exclusively breastfed infants, and maintaining adequate levels in elderly individuals and those with limited mobility. Regular monitoring is essential, with follow-up testing recommended every 3-6 months initially, then annually once stable levels are achieved. The integration of vitamin D optimization into comprehensive healthcare represents a simple yet powerful intervention for improving multiple aspects of health and preventing numerous chronic diseases.