14 Signs of Sleep Apnea That Often Go Unrecognized
Sleep apnea affects an estimated 22 million Americans, yet approximately 80% of cases remain undiagnosed, making it one of the most underrecognized health conditions in modern medicine. This potentially life-threatening disorder involves repeated interruptions in breathing during sleep, causing oxygen levels to drop and forcing the brain to briefly wake the body to restore normal breathing patterns. While many people associate sleep apnea solely with loud snoring, the reality is far more complex, with numerous subtle signs that often masquerade as unrelated health issues. These overlooked symptoms can manifest during both sleeping and waking hours, affecting everything from cognitive function and mood to cardiovascular health and metabolic processes. The consequences of untreated sleep apnea extend far beyond poor sleep quality, increasing the risk of heart disease, stroke, diabetes, depression, and even premature death. Understanding these lesser-known warning signs is crucial for early detection and treatment, as proper intervention can dramatically improve quality of life and prevent serious health complications. This comprehensive exploration will unveil fourteen often-missed indicators that could signal the presence of this silent but serious sleep disorder.
1. Morning Headaches - The Dawn of Discomfort

One of the most frequently overlooked signs of sleep apnea is the presence of persistent morning headaches that seem to appear without explanation. These headaches typically develop due to the repeated drops in oxygen levels and increases in carbon dioxide that occur during apneic episodes throughout the night. When breathing stops during sleep, the brain experiences hypoxemia (low oxygen) and hypercapnia (elevated carbon dioxide), leading to vasodilation of blood vessels in the head and subsequent pain upon waking. Unlike tension headaches or migraines that may develop later in the day due to stress or other triggers, sleep apnea-related headaches are characteristically present immediately upon awakening and often improve within a few hours as normal oxygen levels are restored. Research indicates that individuals with sleep apnea are significantly more likely to experience morning headaches compared to those without the condition, with studies showing that up to 29% of sleep apnea patients report frequent dawn headaches. These headaches are often described as dull, pressing sensations that affect both sides of the head, and they may be accompanied by feelings of grogginess or mental fog. The severity and frequency of these morning headaches often correlate with the severity of the sleep apnea, making them a valuable diagnostic clue when evaluated alongside other symptoms.
2. Excessive Daytime Sleepiness - Beyond Normal Tiredness

Excessive daytime sleepiness represents one of the most debilitating yet commonly dismissed symptoms of sleep apnea, often attributed to busy lifestyles or natural aging rather than an underlying sleep disorder. This overwhelming fatigue goes far beyond the occasional afternoon slump, manifesting as an irresistible urge to sleep during inappropriate times such as while driving, working, or engaging in conversation. The fragmented sleep caused by repeated breathing interruptions prevents individuals from achieving the deep, restorative sleep stages necessary for physical and mental recovery, leading to a persistent state of sleep debt. Research demonstrates that people with untreated sleep apnea experience microsleeps—brief episodes of unconsciousness lasting seconds to minutes—which can occur without their awareness and pose significant safety risks. The Epworth Sleepiness Scale, a standardized assessment tool, reveals that sleep apnea patients consistently score higher than normal populations, indicating pathological levels of daytime drowsiness. This excessive sleepiness can severely impact work performance, academic achievement, and social relationships, as individuals struggle to maintain alertness and concentration throughout the day. The condition creates a vicious cycle where poor nighttime sleep leads to daytime fatigue, which in turn can worsen sleep quality and exacerbate the underlying sleep apnea through factors such as weight gain and reduced physical activity.
3. Cognitive Impairment and Memory Problems - The Foggy Mind Connection

Sleep apnea significantly impacts cognitive function, creating a constellation of mental symptoms that are often attributed to stress, aging, or other conditions rather than the underlying sleep disorder. The repeated oxygen deprivation and sleep fragmentation characteristic of sleep apnea directly affect brain regions responsible for memory consolidation, attention, and executive function. Individuals with untreated sleep apnea frequently report difficulty concentrating, problems with short-term memory, and challenges with decision-making and problem-solving tasks. Neuroimaging studies have revealed that chronic sleep apnea can lead to structural brain changes, including reduced gray matter volume in areas critical for cognitive processing, such as the hippocampus and frontal cortex. The cognitive impairment associated with sleep apnea can manifest as forgetfulness in daily activities, difficulty learning new information, reduced processing speed, and impaired working memory. These symptoms can be particularly pronounced in the morning hours when the effects of overnight oxygen deprivation are most acute. Research indicates that individuals with severe sleep apnea perform significantly worse on neuropsychological tests compared to healthy controls, with deficits often resembling those seen in mild cognitive impairment or early dementia. The good news is that many of these cognitive symptoms can improve with appropriate treatment, as continuous positive airway pressure (CPAP) therapy has been shown to enhance memory, attention, and overall cognitive performance in sleep apnea patients.
4. Mood Disorders and Irritability - The Emotional Toll

The relationship between sleep apnea and mood disorders represents a complex bidirectional connection that often goes unrecognized by both patients and healthcare providers. Chronic sleep disruption and oxygen deprivation associated with sleep apnea can significantly alter brain chemistry, affecting neurotransmitter systems that regulate mood, particularly serotonin and dopamine pathways. Individuals with untreated sleep apnea are at substantially higher risk for developing depression, anxiety, and irritability, with studies showing that up to 63% of sleep apnea patients experience clinically significant depressive symptoms. The persistent fatigue and cognitive impairment caused by poor sleep quality can create a cascade of emotional difficulties, including increased stress sensitivity, reduced emotional regulation, and heightened reactivity to daily challenges. Morning irritability is particularly common, as individuals wake feeling unrefreshed and struggle to cope with normal daily demands. The mood symptoms associated with sleep apnea can be severe enough to warrant psychiatric treatment, yet addressing the underlying sleep disorder is often crucial for achieving lasting improvement. Research demonstrates that successful treatment of sleep apnea with CPAP therapy can lead to significant improvements in depression scores and overall emotional well-being. The connection between sleep apnea and mood disorders is so strong that some mental health professionals now routinely screen their patients for sleep-related breathing disorders, recognizing that treating sleep apnea may be essential for resolving psychiatric symptoms.
5. Frequent Nighttime Urination - The Nocturia Connection

Nocturia, or frequent nighttime urination, affects a significant percentage of individuals with sleep apnea and represents an often-overlooked symptom that can provide important diagnostic clues. The physiological mechanisms linking sleep apnea to increased nighttime urination are complex and multifaceted, involving hormonal disruptions and cardiovascular changes that occur during apneic episodes. When breathing stops during sleep, the resulting hypoxemia triggers the release of atrial natriuretic peptide (ANP), a hormone that promotes sodium and water excretion by the kidneys, leading to increased urine production. Additionally, the frequent arousals from sleep caused by breathing interruptions can increase awareness of bladder sensations that might otherwise be ignored during deep sleep. Research indicates that individuals with sleep apnea are significantly more likely to experience nocturia compared to those without the condition, with some studies showing that up to 84% of sleep apnea patients report frequent nighttime urination. The severity of nocturia often correlates with the severity of sleep apnea, and successful treatment with CPAP therapy has been shown to reduce nighttime urination episodes in many patients. This symptom is particularly important to recognize because nocturia is often attributed to aging, prostate problems in men, or bladder issues in women, potentially delaying the diagnosis of underlying sleep apnea. The bidirectional relationship between sleep apnea and nocturia can create a vicious cycle, as frequent nighttime awakenings for urination can further fragment sleep and potentially worsen breathing difficulties.
6. Dry Mouth and Sore Throat Upon Waking - The Respiratory Aftermath

Waking up with a persistently dry mouth and sore throat is a common but frequently overlooked sign of sleep apnea that results from the compensatory breathing patterns and mouth breathing that occur during the night. When the upper airway becomes obstructed during sleep, individuals often unconsciously switch to mouth breathing as their body attempts to maintain adequate airflow, leading to excessive drying of oral and throat tissues. The repeated efforts to breathe against a collapsed or partially blocked airway can cause tissue irritation and inflammation in the throat, resulting in soreness and discomfort upon waking. Additionally, the snoring that frequently accompanies sleep apnea involves vibration of soft tissues in the throat, which can contribute to inflammation and irritation. The dry mouth associated with sleep apnea is often more severe than typical morning dryness and may persist despite adequate hydration before bedtime. This symptom can have cascading effects on oral health, as reduced saliva production during the night can increase the risk of tooth decay, gum disease, and oral infections. Some individuals may notice a bitter or metallic taste in their mouth upon waking, which can be related to mouth breathing and tissue inflammation. The severity of morning dry mouth and throat discomfort often correlates with the severity of sleep apnea, and these symptoms typically improve significantly with effective treatment. Recognition of these symptoms is important because they are often attributed to allergies, acid reflux, or simple dehydration rather than an underlying sleep breathing disorder.
7. Difficulty Staying Asleep - The Fragmented Night

Sleep maintenance insomnia, characterized by frequent awakenings throughout the night and difficulty returning to sleep, is a hallmark symptom of sleep apnea that is often misattributed to stress, anxiety, or primary insomnia. The repeated breathing interruptions that define sleep apnea trigger brief arousals from sleep as the brain responds to dropping oxygen levels by partially awakening the body to restore normal breathing. While many of these micro-arousals are too brief for conscious awareness, they significantly fragment sleep architecture and prevent the achievement of deep, restorative sleep stages. Individuals with sleep apnea may find themselves waking multiple times throughout the night, often feeling short of breath, with a racing heart, or experiencing a sensation of choking or gasping. These awakenings can be accompanied by feelings of anxiety or panic, as the body's stress response is activated by the oxygen deprivation and breathing difficulties. The pattern of sleep fragmentation in sleep apnea is typically most severe during REM sleep, when muscle tone is naturally reduced and the airway is more susceptible to collapse. Research shows that individuals with sleep apnea experience significantly more sleep stage transitions and arousals compared to healthy sleepers, leading to a reduction in sleep efficiency and overall sleep quality. The cumulative effect of these nightly disruptions is profound daytime fatigue and impaired cognitive function, even when total sleep time appears adequate. Understanding this connection is crucial because sleep maintenance problems are often treated with sleep medications that can actually worsen sleep apnea by further relaxing upper airway muscles.
8. High Blood Pressure - The Cardiovascular Silent Alarm
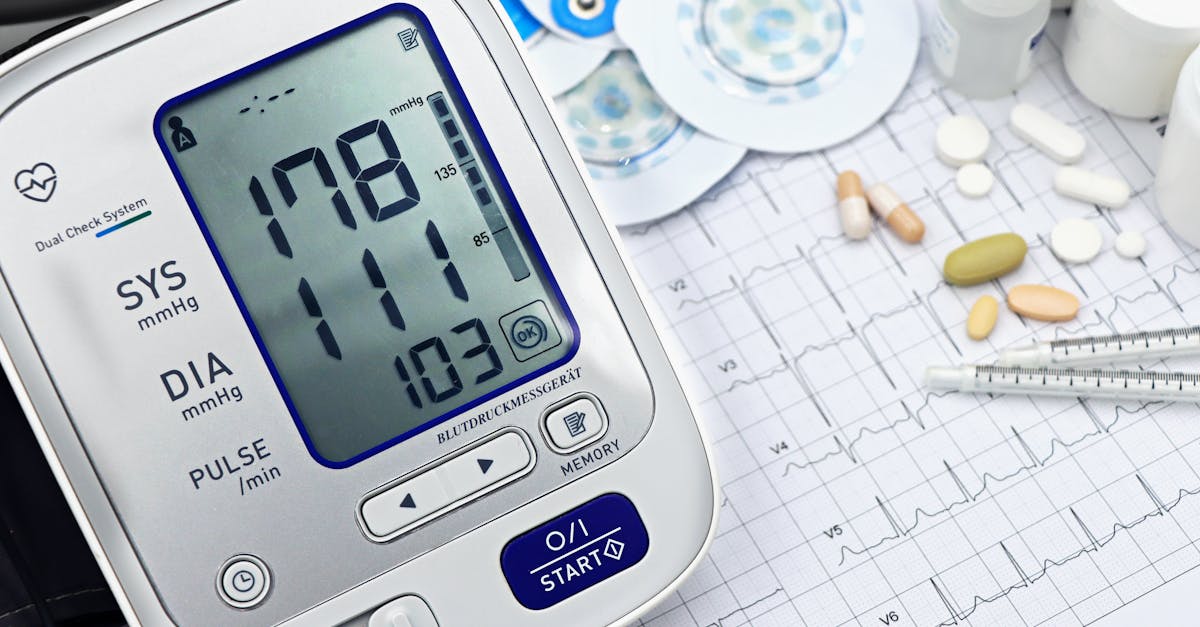
Hypertension represents one of the most serious and frequently unrecognized consequences of untreated sleep apnea, with research demonstrating a strong bidirectional relationship between these two conditions. The repeated episodes of oxygen deprivation and the subsequent stress response triggered during apneic events lead to significant cardiovascular strain throughout the night. Each breathing interruption activates the sympathetic nervous system, causing surges in blood pressure and heart rate as the body attempts to restore normal breathing and oxygenation. Over time, this nightly cardiovascular stress can lead to sustained hypertension that persists during waking hours, as the repeated activation of stress pathways causes long-term changes in blood pressure regulation. Studies indicate that approximately 50% of individuals with sleep apnea have hypertension, and conversely, about 30% of people with high blood pressure have undiagnosed sleep apnea. The relationship is particularly strong with resistant hypertension—high blood pressure that remains elevated despite treatment with multiple medications—where sleep apnea is found in up to 85% of cases. The mechanisms linking sleep apnea to hypertension include increased sympathetic nervous system activity, endothelial dysfunction, inflammation, and alterations in the renin-angiotensin-aldosterone system. Morning blood pressure readings are often particularly elevated in individuals with sleep apnea, reflecting the cumulative effects of overnight cardiovascular stress. Recognition of this connection is crucial because treating sleep apnea can lead to significant improvements in blood pressure control, potentially reducing the need for antihypertensive medications and lowering cardiovascular risk.
9. Weight Gain and Difficulty Losing Weight - The Metabolic Disruption

The relationship between sleep apnea and weight management represents a complex cycle where each condition can worsen the other, creating significant challenges for individuals trying to maintain a healthy weight. Sleep apnea disrupts normal hormonal regulation, particularly affecting leptin and ghrelin—hormones that control hunger and satiety. The chronic sleep deprivation and fragmentation associated with sleep apnea leads to decreased leptin production (the hormone that signals fullness) and increased ghrelin levels (the hormone that stimulates appetite), resulting in increased hunger and cravings, particularly for high-calorie, carbohydrate-rich foods. Additionally, the excessive daytime fatigue caused by poor sleep quality often leads to reduced physical activity and exercise tolerance, further contributing to weight gain. The metabolic consequences of sleep apnea extend beyond appetite regulation, affecting insulin sensitivity and glucose metabolism, which can lead to weight gain and increased risk of type 2 diabetes. Research demonstrates that individuals with untreated sleep apnea have slower metabolic rates and burn fewer calories at rest compared to those without the condition. The weight gain associated with sleep apnea tends to be concentrated around the neck and upper body, which can further worsen airway obstruction and sleep apnea severity. This creates a vicious cycle where weight gain worsens sleep apnea, which in turn makes weight loss more difficult through hormonal and metabolic disruptions. Studies show that even modest weight loss can significantly improve sleep apnea symptoms, while effective treatment of sleep apnea can facilitate weight loss efforts by normalizing appetite hormones and improving energy levels for physical activity.
10. Decreased Libido and Sexual Dysfunction - The Intimate Consequences

Sexual dysfunction and decreased libido represent significant but often unspoken consequences of untreated sleep apnea that can profoundly impact quality of life and intimate relationships. The chronic sleep deprivation, fatigue, and hormonal disruptions associated with sleep apnea can severely affect sexual function in both men and women through multiple physiological and psychological pathways. In men, sleep apnea is strongly associated with erectile dysfunction, with studies showing that up to 69% of men with sleep apnea experience some degree of erectile problems. The mechanisms include reduced testosterone production due to disrupted sleep, impaired blood flow related to cardiovascular effects of sleep apnea, and the psychological impact of chronic fatigue and mood changes. The repeated oxygen desaturations during sleep can damage the endothelial cells lining blood vessels, affecting the vascular mechanisms necessary for normal erectile function. Women with sleep apnea may experience decreased sexual desire, difficulty with arousal, and reduced sexual satisfaction, often related to hormonal imbalances, fatigue, and mood changes associated with poor sleep quality. The excessive daytime sleepiness and cognitive fog common in sleep apnea can reduce interest in sexual activity and impair the emotional connection necessary for intimacy. Additionally, the mood disorders frequently associated with sleep apnea, including depression and anxiety, can further compound sexual difficulties. Research indicates that successful treatment of sleep apnea with CPAP therapy can lead to significant improvements in sexual function, testosterone levels, and overall sexual satisfaction in both men and women, highlighting the importance of recognizing these symptoms as potential indicators of an underlying sleep disorder.
11. Gastroesophageal Reflux Disease (GERD) - The Digestive Connection

The relationship between sleep apnea and gastroesophageal reflux disease (GERD) represents a complex bidirectional association that is frequently overlooked in clinical practice, yet understanding this connection is crucial for effective treatment of both conditions. Sleep apnea can contribute to the development and worsening of GERD through several mechanisms, including changes in intrathoracic pressure during apneic episodes that can promote acid reflux, and alterations in esophageal motility that may impair the clearance of refluxed acid. The repeated efforts to breathe against an obstructed airway create significant negative pressure changes in the chest cavity, which can draw stomach acid upward into the esophagus. Additionally, the frequent arousals and sleep fragmentation associated with sleep apnea can disrupt normal digestive processes and reduce saliva production, which normally helps neutralize acid in the esophagus. Conversely, GERD can worsen sleep apnea by causing inflammation and swelling in the upper airway tissues, particularly around the larynx and pharynx, which can increase the likelihood of airway collapse during sleep. The acid reflux episodes common in GERD can trigger protective reflexes that cause brief awakenings and further fragment sleep. Studies indicate that individuals with sleep apnea are significantly more likely to experience GERD symptoms, with some research showing that up to 60% of sleep apnea patients also have clinically significant acid reflux. The timing of GERD symptoms can provide diagnostic clues, as individuals with sleep apnea-related reflux often experience symptoms primarily at night or upon waking, rather than after meals. Treatment of sleep apnea with CPAP therapy has been shown to improve GERD symptoms in many patients, while effective management of acid reflux can also contribute to better sleep quality and reduced sleep apnea severity.
12. Chronic Fatigue and Low Energy - The Persistent Exhaustion
