15 Ways to Support Joint Health as You Age
# 15 Ways to Support Joint Health as You Age: A Comprehensive Guide to Maintaining Mobility and Comfort
As we journey through life, our joints serve as the intricate mechanical marvels that enable every movement, from the simplest gesture to the most complex athletic endeavor. These remarkable structures, comprising bones, cartilage, synovial fluid, ligaments, and surrounding muscles, face increasing challenges as we age. The natural wear and tear of decades, combined with lifestyle factors, environmental influences, and genetic predispositions, can gradually compromise joint function and comfort. However, the narrative of inevitable joint deterioration is far from predetermined. Modern research has illuminated numerous evidence-based strategies that can significantly impact joint health trajectories, offering hope and practical solutions for maintaining mobility, reducing discomfort, and preserving quality of life well into our golden years. This comprehensive exploration will delve into fifteen scientifically-backed approaches to joint health maintenance, each representing a crucial piece of the complex puzzle that is musculoskeletal wellness. From nutritional interventions and exercise protocols to lifestyle modifications and emerging therapeutic approaches, we'll examine how proactive measures can transform the aging experience, enabling individuals to remain active, independent, and comfortable regardless of their chronological age.
1. Embrace Regular Low-Impact Exercise

Low-impact exercise forms the cornerstone of joint health maintenance, offering the perfect balance between movement stimulation and joint protection. Research consistently demonstrates that regular physical activity promotes synovial fluid circulation, which acts as the joint's natural lubricant and nutrient delivery system. Activities such as swimming, cycling, walking, and elliptical training provide cardiovascular benefits while minimizing stress on weight-bearing joints. The aquatic environment is particularly beneficial, as water's buoyancy reduces joint loading by up to 90% while providing gentle resistance for muscle strengthening. Studies published in arthritis research journals show that individuals who engage in regular low-impact exercise experience significantly less joint stiffness, improved range of motion, and reduced pain levels compared to sedentary counterparts. The key lies in consistency rather than intensity – even 30 minutes of moderate activity five days per week can yield substantial benefits. Additionally, low-impact exercises help maintain bone density, strengthen supporting muscles, and improve proprioception, all of which contribute to joint stability and injury prevention as we age.
2. Prioritize Strength Training for Joint Support

Strength training represents one of the most powerful interventions for joint health, as strong muscles act as dynamic stabilizers that reduce stress on joint structures. Research from the American College of Sports Medicine indicates that resistance training can increase muscle mass by 20-30% and bone density by 1-3% annually in older adults. When muscles surrounding joints are well-developed, they absorb more of the mechanical forces that would otherwise be transmitted directly to cartilage and bone. Progressive resistance training, using weights, resistance bands, or bodyweight exercises, stimulates bone remodeling and enhances the production of growth factors that support cartilage health. Studies focusing on knee osteoarthritis have shown that quadriceps strengthening can reduce pain by up to 40% and improve function significantly. The eccentric component of strength training is particularly beneficial, as it promotes collagen synthesis in tendons and ligaments while improving muscle-tendon unit compliance. For optimal joint health benefits, strength training should target all major muscle groups, with special attention to the core, glutes, and muscles surrounding commonly affected joints like the knees, hips, and shoulders.
3. Maintain Optimal Body Weight

Body weight management stands as one of the most impactful modifiable factors in joint health preservation, particularly for weight-bearing joints such as the knees, hips, and spine. Each pound of excess body weight translates to approximately four pounds of additional force across the knee joint during walking activities. Research published in the Journal of Biomechanics demonstrates that even modest weight loss of 5-10% can significantly reduce joint loading and slow cartilage degradation. The relationship between obesity and joint health extends beyond mechanical stress, as adipose tissue produces inflammatory cytokines that can accelerate cartilage breakdown and promote systemic inflammation. Studies following individuals over decades have shown that maintaining a healthy BMI throughout life can reduce the risk of developing osteoarthritis by up to 50%. Weight management strategies should focus on sustainable lifestyle changes rather than rapid weight loss, as gradual reduction allows joints to adapt while preserving muscle mass. The combination of caloric awareness, portion control, and increased physical activity creates a synergistic effect that benefits both weight management and joint health simultaneously.
4. Incorporate Anti-Inflammatory Foods

Nutrition plays a pivotal role in joint health, with certain foods possessing powerful anti-inflammatory properties that can help combat the chronic low-grade inflammation associated with aging joints. The Mediterranean diet pattern, rich in omega-3 fatty acids, antioxidants, and phytonutrients, has been extensively studied for its joint-protective effects. Fatty fish such as salmon, mackerel, and sardines provide EPA and DHA omega-3 fatty acids that help reduce inflammatory markers and may slow cartilage degradation. Colorful fruits and vegetables supply anthocyanins, flavonoids, and other compounds that neutralize free radicals and support tissue repair processes. Research published in nutrition journals indicates that individuals following anti-inflammatory dietary patterns experience less joint pain and stiffness compared to those consuming pro-inflammatory foods. Specific foods like tart cherries have been shown to reduce inflammatory markers by up to 25% in clinical trials. Turmeric, containing the active compound curcumin, demonstrates comparable anti-inflammatory effects to some non-steroidal anti-inflammatory drugs without the associated side effects. Green tea polyphenols, particularly EGCG, have been shown to inhibit cartilage-degrading enzymes and protect against oxidative stress in joint tissues.
5. Stay Adequately Hydrated

Proper hydration is fundamental to joint health, as synovial fluid – the lubricating substance within joint capsules – is approximately 80% water. When hydration levels drop, synovial fluid becomes more viscous and less effective at reducing friction between joint surfaces. Research indicates that even mild dehydration can affect joint lubrication and increase the risk of injury during physical activity. The intervertebral discs in the spine are particularly susceptible to dehydration effects, as these structures rely on fluid exchange for nutrient delivery and waste removal. Studies using MRI imaging have shown that disc height and hydration status are directly correlated, with dehydrated discs showing increased susceptibility to degeneration. Adequate hydration also supports the transport of nutrients to cartilage, which lacks its own blood supply and depends on diffusion from synovial fluid. The general recommendation of eight glasses of water daily may need adjustment based on activity level, climate, and individual factors. Monitoring urine color provides a practical hydration assessment tool, with pale yellow indicating optimal hydration status. Additionally, consuming water-rich foods like fruits and vegetables contributes to overall fluid intake while providing additional joint-supporting nutrients.
6. Prioritize Quality Sleep for Joint Recovery

Sleep represents a critical yet often overlooked component of joint health maintenance, as this restorative period allows for tissue repair, inflammation reduction, and growth hormone release. During deep sleep phases, the body increases production of growth hormone, which plays a vital role in cartilage repair and regeneration. Research published in sleep medicine journals demonstrates that individuals with poor sleep quality experience higher levels of inflammatory markers and increased pain sensitivity. The relationship between sleep and joint health is bidirectional – joint pain can disrupt sleep patterns, while poor sleep can exacerbate joint discomfort and slow healing processes. Studies following individuals with arthritis have shown that sleep quality improvements correlate with reduced pain levels and better functional outcomes. The recommended 7-9 hours of quality sleep per night allows for complete sleep cycle progression, ensuring adequate time for tissue repair processes. Sleep position and mattress quality can significantly impact joint stress, particularly for the spine, hips, and shoulders. Creating an optimal sleep environment with appropriate temperature, darkness, and comfortable bedding supports both sleep quality and joint recovery. Additionally, establishing consistent sleep schedules helps regulate circadian rhythms, which influence inflammatory processes and pain perception.
7. Manage Stress Effectively

Chronic stress exerts profound effects on joint health through multiple physiological pathways, making stress management an essential component of comprehensive joint care. Elevated stress hormones, particularly cortisol, can accelerate cartilage breakdown while suppressing the immune system's ability to manage inflammation effectively. Research in psychoneuroimmunology demonstrates that chronic stress increases production of inflammatory cytokines that directly contribute to joint degradation. The muscle tension associated with chronic stress can also create imbalances that place additional strain on joints, particularly in the neck, shoulders, and back. Studies following individuals with rheumatoid arthritis have shown that stress reduction techniques can significantly improve symptoms and slow disease progression. Effective stress management strategies include meditation, deep breathing exercises, progressive muscle relaxation, and mindfulness practices. Regular meditation has been shown to reduce inflammatory markers by up to 30% in some studies while improving pain tolerance and quality of life. Physical activities like yoga and tai chi provide dual benefits by combining stress reduction with gentle joint movement and strengthening. Social support systems and professional counseling can also play crucial roles in stress management, as emotional well-being directly impacts physical health outcomes.
8. Consider Targeted Supplementation

While a balanced diet should provide most essential nutrients, certain supplements have demonstrated specific benefits for joint health when used appropriately. Glucosamine and chondroitin sulfate, components naturally found in cartilage, have been extensively studied for their potential to support joint structure and function. Meta-analyses of clinical trials suggest that these supplements may help slow cartilage degradation and reduce pain in some individuals with osteoarthritis. Omega-3 fatty acid supplements provide concentrated doses of EPA and DHA that may be difficult to achieve through diet alone, with studies showing anti-inflammatory effects equivalent to consuming fish multiple times per week. Vitamin D supplementation is particularly important for joint health, as deficiency is associated with increased risk of osteoarthritis and poor bone health. Research indicates that maintaining optimal vitamin D levels (30-50 ng/mL) supports calcium absorption, bone mineralization, and immune function regulation. Collagen peptides have gained attention for their potential to stimulate cartilage synthesis, with some studies showing improvements in joint pain and function. However, supplement quality varies significantly, making it essential to choose products that have been third-party tested for purity and potency. Consultation with healthcare providers is recommended before starting any supplement regimen, particularly for individuals taking medications or with existing health conditions.
9. Maintain Proper Posture and Body Mechanics

Proper posture and body mechanics serve as fundamental protective factors for joint health, distributing mechanical forces evenly and preventing excessive stress on specific structures. Poor posture creates muscle imbalances that can lead to compensatory movement patterns, ultimately resulting in increased wear on certain joints while underutilizing others. Research in occupational health demonstrates that forward head posture, commonly associated with computer work, can increase cervical spine loading by up to 60 pounds of additional force. The kinetic chain concept illustrates how dysfunction in one area can cascade to affect distant joints – for example, ankle stiffness can contribute to knee, hip, and back problems. Ergonomic workplace setups play crucial roles in maintaining proper spinal alignment during prolonged sitting, with adjustable chairs, monitor positioning, and keyboard placement all contributing to joint health. Body mechanics training for daily activities such as lifting, carrying, and reaching can significantly reduce injury risk and joint stress. Studies of healthcare workers have shown that proper lifting technique education can reduce back injury rates by up to 50%. Regular posture checks throughout the day, combined with targeted stretching and strengthening exercises, help maintain optimal alignment and prevent the development of chronic postural problems that accelerate joint degeneration.
10. Incorporate Flexibility and Mobility Work

Flexibility and mobility work form essential components of joint health maintenance, ensuring that joints can move through their full range of motion while maintaining tissue extensibility. Regular stretching helps prevent the development of adhesions and contractures that can limit joint movement and increase injury risk. Research published in physical therapy journals demonstrates that individuals who maintain good flexibility experience less joint stiffness and better functional outcomes as they age. Dynamic stretching before activities prepares joints for movement by increasing synovial fluid production and elevating tissue temperature, while static stretching after exercise helps maintain muscle length and joint range of motion. Yoga and tai chi represent comprehensive approaches to flexibility and mobility, combining stretching with strength, balance, and mindfulness components. Studies of older adults participating in yoga programs show significant improvements in joint flexibility, balance, and quality of life measures. Fascial release techniques, including foam rolling and self-massage, can help maintain tissue quality and improve movement patterns. The concept of "use it or lose it" applies particularly to joint mobility – joints that are not regularly moved through their full range of motion will gradually lose that capacity. Targeted mobility work should address common problem areas such as hip flexors, thoracic spine, and shoulders, which tend to become restricted due to modern lifestyle patterns.
11. Protect Joints During Activities

Joint protection strategies during daily activities and exercise can significantly reduce cumulative damage and preserve function over time. Understanding proper biomechanics for common movements helps distribute forces appropriately and avoid excessive stress on vulnerable structures. Wearing appropriate footwear provides crucial support and shock absorption, with studies showing that proper shoes can reduce impact forces by up to 30% during walking and running activities. Activity modification doesn't necessarily mean activity avoidance – rather, it involves making smart choices about timing, intensity, and technique to minimize joint stress while maintaining fitness and function. Using assistive devices when appropriate, such as braces for unstable joints or ergonomic tools for repetitive tasks, can help preserve joint integrity without significantly limiting activity participation. Research in sports medicine demonstrates that proper warm-up protocols can reduce injury risk by up to 50% by preparing joints and muscles for activity demands. Cross-training approaches help prevent overuse injuries by varying movement patterns and stress distribution across different joints. Environmental considerations, such as exercising on softer surfaces when possible and avoiding activities during extreme weather conditions, also contribute to joint protection. The key is finding the balance between staying active enough to maintain joint health while avoiding excessive stress that could accelerate wear and tear.
12. Address Injuries Promptly and Completely
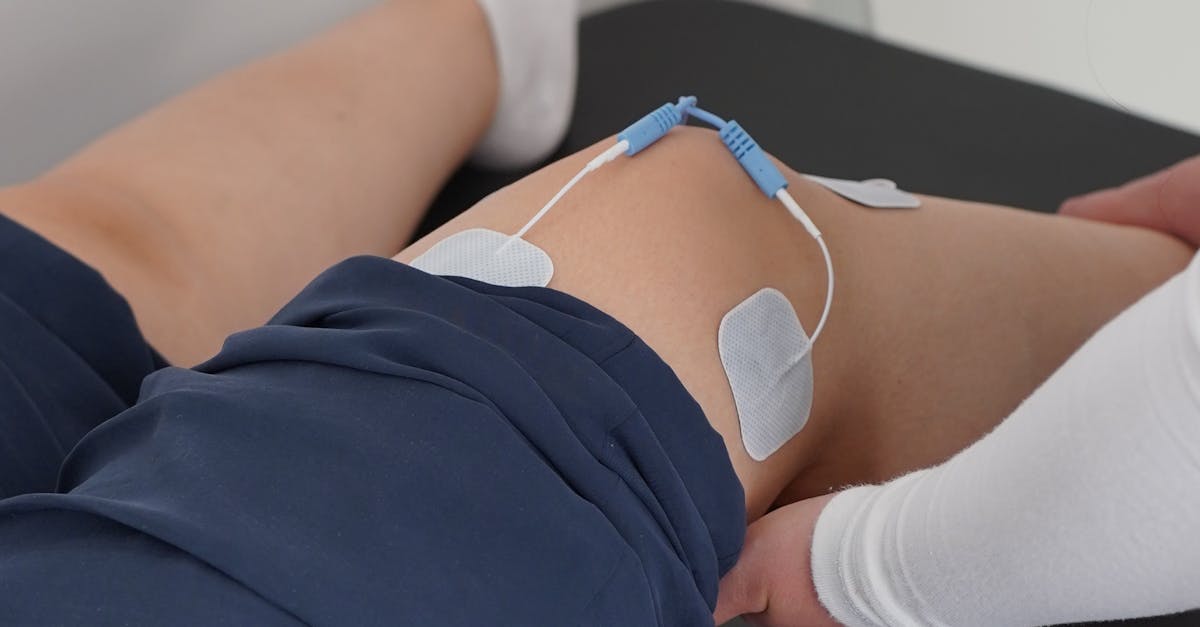
Proper injury management represents a critical factor in long-term joint health, as inadequately treated injuries can lead to chronic problems and accelerated degeneration. The acute inflammatory response following injury serves important healing functions, but prolonged inflammation can become destructive to joint tissues. Research shows that individuals who receive appropriate early intervention for joint injuries have significantly better long-term outcomes compared to those who ignore symptoms or delay treatment. The RICE protocol (Rest, Ice, Compression, Elevation) remains valuable for acute injury management, though recent research suggests that some movement and loading may be beneficial during the healing process when tolerated. Professional evaluation is essential for significant injuries, as what appears minor may involve structures that require specific treatment approaches. Physical therapy plays a crucial role in injury recovery, addressing not only the injured tissue but also the compensatory patterns that often develop. Studies of athletes returning to sport after injury demonstrate that comprehensive rehabilitation programs reduce re-injury rates by up to 70%. Gradual return to activity protocols help ensure that healing tissues can adapt to increasing demands without re-injury. The psychological aspects of injury recovery are also important, as fear of re-injury can lead to movement avoidance and subsequent deconditioning that actually increases future injury risk.
13. Regular Health Monitoring and Professional Care
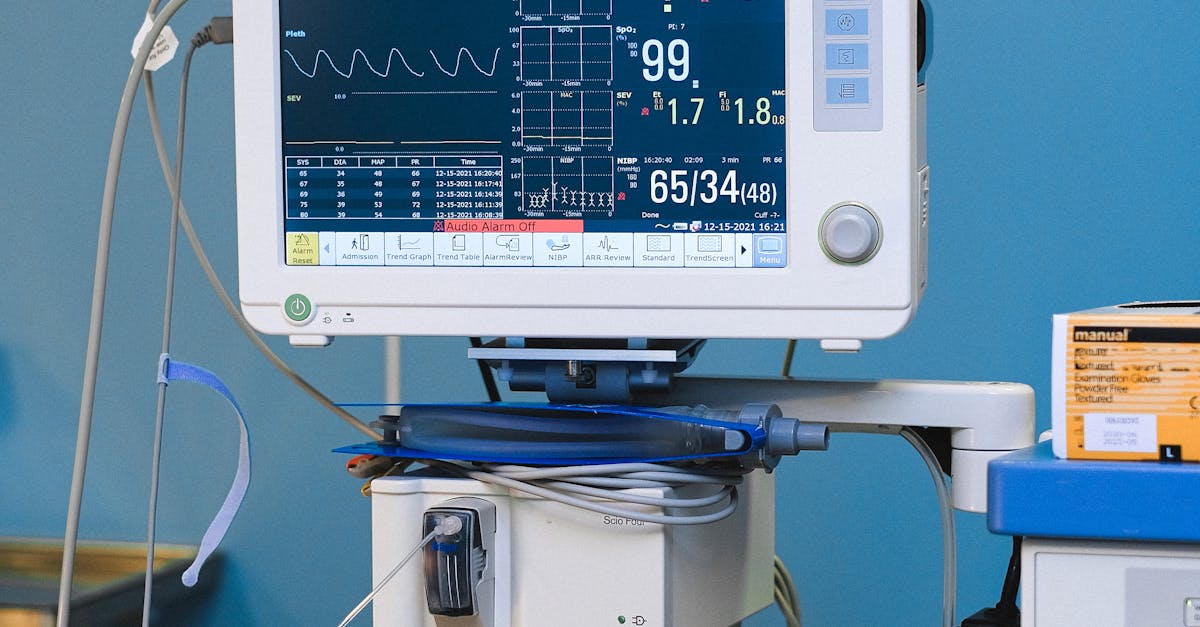
Proactive health monitoring and professional care form essential components of comprehensive joint health management, enabling early detection and intervention for potential problems. Regular check-ups with healthcare providers allow for assessment of joint function, identification of risk factors, and development of personalized prevention strategies. Baseline measurements of joint range of motion, strength, and functional capacity provide valuable reference points for tracking changes over time. Research demonstrates that individuals who receive regular preventive care experience better long-term outcomes and lower healthcare costs compared to those who seek treatment only after problems develop. Screening for conditions that can affect joint health, such as diabetes, thyroid disorders, and autoimmune diseases, enables early intervention that can prevent or slow joint complications. Professional movement assessments can identify biomechanical issues and muscle imbalances before they lead to injury or degeneration. Periodic imaging studies may be appropriate for individuals with risk factors or symptoms, though routine imaging of asymptomatic joints is generally not recommended. Collaboration between different healthcare providers, including primary care physicians, orthopedists, physical therapists, and nutritionists, can provide comprehensive care that addresses all aspects of joint health. Keeping detailed records of symptoms, activities, and treatments helps healthcare providers make informed decisions and track progress over time.
14. Explore Temperature Therapy Benefits
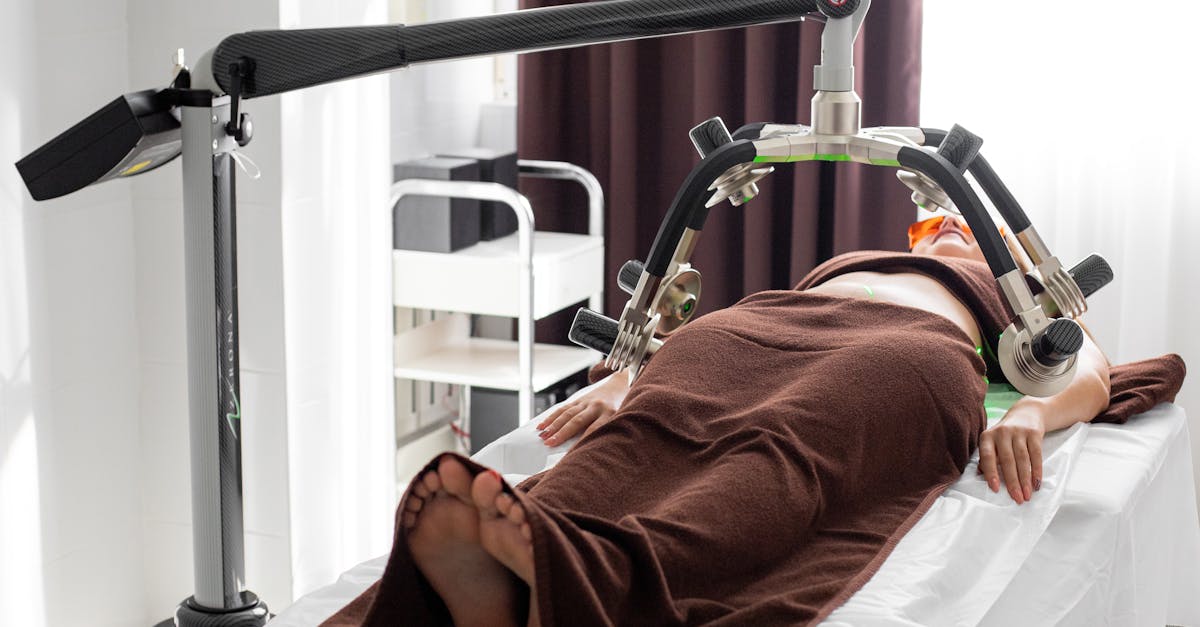
Temperature therapy represents a valuable and accessible tool for joint health management, with both heat and cold applications offering distinct benefits for different situations. Heat therapy increases blood flow, reduces muscle tension, and can help improve joint mobility by increasing tissue extensibility. Research shows that heat application before exercise can improve performance and reduce injury risk by preparing tissues for activity. Warm baths, heating pads, and warm compresses provide convenient heat therapy options, with studies demonstrating pain reduction and improved function in individuals with chronic joint conditions. Cold therapy, conversely, helps reduce inflammation, numbs pain, and can limit tissue damage following acute injuries. Ice baths, cold packs, and cryotherapy chambers have gained popularity among athletes for their recovery benefits, with research showing reduced inflammatory markers and faster return to activity. Contrast therapy, alternating between heat and cold applications, may provide additional benefits by promoting circulation and reducing inflammation simultaneously. The timing and duration of temperature therapy applications are important considerations – heat is generally more beneficial before activity and for chronic conditions, while cold is preferred immediately after injury or intense exercise. Individual responses to temperature therapy can vary significantly, making it important to experiment with different approaches to find what works best. Safety considerations include avoiding extreme temperatures, limiting application duration, and being cautious with temperature therapy in individuals with certain medical conditions or reduced sensation.
15. Maintain Social Connections and Mental Health

The connection between social relationships, mental health, and physical well-being extends significantly to joint health outcomes, making social engagement an often-overlooked but crucial component of comprehensive joint care. Research in social psychology and health sciences demonstrates that individuals with strong social support networks experience lower levels of inflammatory markers and better pain management compared to socially isolated counterparts. Chronic loneliness and depression can increase cortisol production and inflammatory cytokine levels, creating a