12 Virtual Health Coaches That Deliver Personalized Care on Demand
Virtual health coaches are guided programs and human-plus-digital teams that help people set and reach health goals, manage chronic conditions, and get timely support without always visiting a clinic. They include app-based coaches that use AI for daily check-ins, licensed clinicians offering video sessions, and condition-specific teams that pair clinical oversight with practical coaching. For people navigating diabetes risk, cancer treatment side effects, persistent joint pain, or simply trying to build steady habits, these services offer tailored plans, on-demand communication, and tools that fit into day-to-day life. Some programs are recognized by official bodies, which adds a layer of trust. Other services partner with employers or insurers, which can lower or remove out-of-pocket costs for eligible members. This piece walks through a mix of well-known platforms, core technology features, evidence points, access choices, and practical steps to help you pick what fits. The aim is to give readers clear options and realistic expectations. We’ll highlight what each option does well, what the research shows for outcomes where available, and what questions to ask before enrolling. If you’re thinking about a digital coach for yourself or a loved one, these profiles and practical tips will make it easier to compare programs, check coverage, and take the first steps toward steady, sustainable support.
1. Lark — CDC-Recognized Diabetes Prevention Coaching

Lark offers a digital Diabetes Prevention Program that’s recognized by the CDC and is designed around daily coaching, bite-sized lessons, and automated feedback informed by your activity and weight trends. The platform serves millions of users and pairs conversational, AI-driven coaching with goal tracking so people can build healthier habits without frequent in-person visits. For adults at risk of type 2 diabetes, this approach focuses on steady weight loss, moving more each day, and tracking food choices—practical habits that add up. Because the program has CDC recognition, it follows a structured curriculum and collects measurable progress markers. Some members access Lark at low or no cost through employer or insurance arrangements; eligibility varies, so it’s worth checking benefits first. If you prefer more human touchpoints, look for plans that add clinician check-ins or health coach sessions. For older adults, the main practical step is to confirm device compatibility and to start with simple daily tasks that don’t require heavy tech setup. This program works best when you set one clear goal, log small wins, and use the app’s daily prompts to build momentum.
2. Greatly Health — Cancer-Focused Symptom and Wellness Coaching

Greatly Health was developed with oncologists and integrative medicine specialists and offers coaching tailored for people undergoing cancer treatment and survivorship. Their program blends symptom management, nutrition guidance, mental health support, and practical coping tools so patients and caregivers have guided support during a stressful time. Reported outcomes associated with the program include notable reductions in physical pain and hospitalization rates during treatment, along with meaningful improvements in anxiety and depression measures for many participants. High recommendation rates from users point to real-world usefulness for people navigating complex care schedules. Greatly’s model shows how condition-specific coaching can complement clinical care by filling gaps between visits and offering daily support for side-effect management. If you or a family member are considering this option, ask how the coach coordinates with your oncology team and whether data from the program can be shared with your providers. That coordination is what keeps digital coaching rooted in the larger clinical picture.
3. Hinge Health — Musculoskeletal Care and Guided Therapy
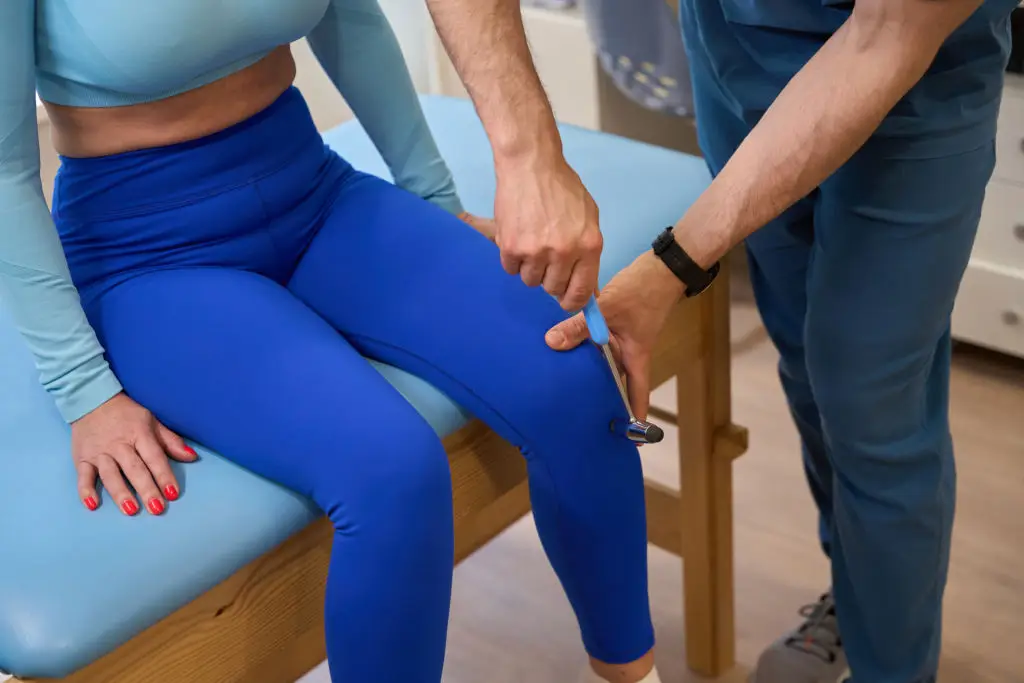
Hinge Health focuses on musculoskeletal conditions like chronic back pain, arthritis, and post-surgical recovery by combining guided exercise therapy, personalized coaching, and educational content delivered through an app. The platform often pairs structured exercise programs with coaching check-ins and sometimes with wearable sensors or motion-tracking tools to ensure you’re performing movements safely. Hinge’s model aims to reduce pain and improve function by encouraging consistent, progressive exercises rather than occasional, unstructured workouts. Employers and insurers frequently offer Hinge Health programs, which can remove financial barriers for participants. The practical benefit for older adults is a clear exercise plan tailored to current ability, with coaches who can adjust guidance and encourage gentle progress. When evaluating MSK programs, check whether the platform offers live clinician oversight for complex conditions and whether there’s an option to access a physical therapist or physician if pain doesn’t improve.
4. TimelyCare — Campus-Focused Virtual Clinical Coaching

TimelyCare specializes in campus health and provides on-demand virtual clinical care, mental health support, and coaching services for students through video, phone, and chat options. The platform’s team-based approach lets students access medical guidance and behavioral health coaching without traveling to a clinic, which is helpful when schedules are tight or when students are off-campus. TimelyCare can also support wellness topics like sleep, stress, and substance-use conversations with short, focused coaching sessions. For families or older students considering the service, the practical advantage is ease of access and rapid connection to care teams who understand student-life rhythms. If you’re part of a campus community, ask how the service integrates with on-site health services and whether notes can be shared confidentially with campus clinicians. That clarity helps ensure coaching complements, rather than replaces, necessary in-person care.
5. Optimal U — Whole-Person Wellness and Preventive Coaching

Optimal U takes a whole-person approach to wellness coaching by blending habit-focused modules, lifestyle medicine principles, and both group and one-on-one coaching options aimed at long-term prevention and resilience. Programs typically encourage small, manageable changes across nutrition, activity, sleep, and stress management—changes that can fit into busy lives without dramatic disruption. The coaching style emphasizes sustainable steps rather than quick fixes, and it offers practical tools for tracking progress and celebrating steady improvement. For older adults, that steady approach is often more realistic and kinder to maintain. When considering a general wellness platform, look for coaching that allows personalization based on medical history and that provides clear pathways for escalation to clinicians if a health issue arises. That safety net makes preventive coaching safer and more credible.
6. AI Personalization — How Intelligent Coaching Tailors Your Plan

AI is increasingly woven into digital coaching to create personalized goals, summarize user interactions, and suggest small next steps based on patterns in your data. Platforms using AI can generate tailored SMART-style goals and triage which items need clinician attention, so your coach spends time on higher-value conversations. An expert in lifestyle medicine noted that AI tools can also save clinicians time by automating documentation and allowing coaches to focus on care delivery. That saves staff hours and can make programs more affordable for users when costs are passed along. But AI-driven personalization works best when paired with human oversight; algorithms can suggest helpful nudges but should not replace clinical judgment when symptoms are serious. Privacy and data security are central concerns here, so check how the platform stores and shares data and whether you control what’s shared with your provider or employer. Used thoughtfully, AI can make coaching feel more responsive and practical for everyday life.
7. Device Integration — Wearables, Scales, and Remote Monitoring

Many virtual coaches connect with wearable devices and home monitors—like activity trackers, smart scales, and Bluetooth glucometers—to bring real-life measurements into the coaching conversation. That direct feed of data helps coaches spot trends, celebrate progress, and adjust plans based on actual behavior rather than memory alone. For example, daily step counts can inform activity goals and weight trends can guide nutrition coaching. For people managing chronic conditions, integration with a glucometer or blood pressure monitor can let coaches spot worrisome readings and suggest timely follow-up with clinicians. The practical step when you enroll is to confirm device compatibility and to choose a setup that matches your comfort with technology; many platforms allow manual entry if you prefer less device dependence. Clear device guidance during onboarding reduces frustration and makes tracking useful instead of burdensome.
8. Evidence and Outcomes — What the Studies Say

The evidence for virtual coaching shows promising benefits in specific areas: structured diabetes prevention programs reduce progression risk, MSK coaching often improves pain and function, and condition-specific programs can ease symptom burden for patients in active treatment. Greatly Health reports substantial reductions in pain and hospitalization among its users and strong patient recommendation rates, showing how a clinically informed, tailored model can move measurable outcomes. Lark’s CDC-recognized program points to the value of following an established prevention curriculum digitally. That said, long-term data on sustained behavior change after program completion remain limited across the industry. When you review claims, look for clinical partnerships, peer-reviewed studies or transparent outcome reports, and whether the program publishes its methodology. Those signals help you separate marketing language from programs that have a demonstrable track record.
9. Accessibility and Delivery — Video, Chat, Phone, and 24/7 Support

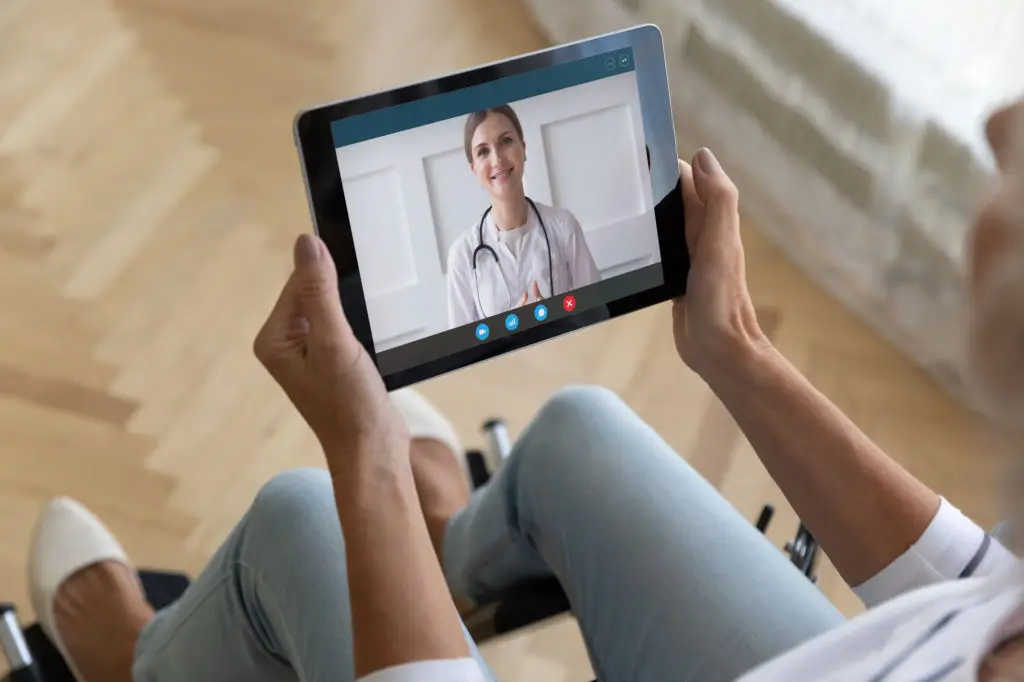
Virtual coaches deliver support through multiple channels: scheduled video visits for deeper conversations, text or chat for quick check-ins, phone calls for familiar interaction, and asynchronous lessons or messages for flexible learning. Some platforms offer 24/7 access for basic triage or coaching nudges, which can be reassuring for people who need help outside regular office hours. Accessibility features like large text, captioning on videos, and simple navigation matter for older adults or anyone with limited tech experience. If language support or culturally relevant coaching matters to you, ask whether the platform offers multilingual coaches or inclusive content. The right delivery mix depends on personal preference: some people want daily chat nudges, while others prefer a weekly video check-in. Choose a program that meets you where you are and that can escalate to a clinician when symptoms or concerns require it.
10. Cost and Insurance — Pricing Models, Employer Benefits, and Coverage

Virtual coaching pricing ranges from employer- or insurer-covered programs to monthly subscriptions and tiered memberships. Greatly Health lists community and complete care memberships at accessible monthly rates, while other platforms may be fully covered for eligible members through employer wellness benefits or specific insurance plans. Some CDC-recognized programs are offered at low or no cost to qualifying members via insurance. Always check eligibility with your employer and ask the platform about available billing codes or claims support if you plan to seek insurance reimbursement. If cost is a concern, prioritize programs that offer a free trial or a money-back guarantee for a short onboarding period. When evaluating value, consider not only price but the expected intensity of coaching, available clinical oversight, and outcome transparency—those elements determine whether a program delivers practical, lasting benefit for your needs.
11. Choosing the Right Coach — Match Goals, Condition, and Coaching Style
Selecting the right virtual coach starts with clarity about your primary goals: weight and diabetes prevention, cancer symptom support, chronic pain management, or general wellness. Match that goal to a platform that has clinical oversight and evidence for that condition. Look at coaching style—do you prefer automated prompts and nudges, regular human check-ins, or a mix of both? Ask about clinician escalation pathways so coaches can refer you back to in-person care when needed. Consider technology comfort: if you want simple tools, choose platforms that allow manual tracking and straightforward phone-based support. Finally, try short trials when available and set a 30-day check-in to see if the program helps you form a consistent habit. That initial test period is the clearest way to see if the coach’s approach fits your lifestyle and motivation.
12. Getting Started — Enrollment, Trials, and What to Expect in the First Month

A simple starter plan helps you get comfortable with virtual coaching: confirm eligibility and coverage, try any free trial or introductory session, connect basic devices if needed, and set one manageable goal for the first 30 days. During onboarding, provide your medical history and preferred contact method so the coach can tailor recommendations and escalate clinically when necessary. Expect small daily prompts, weekly check-ins, and measurable mini-goals rather than sweeping changes. Track progress with simple metrics like daily steps, a single weight goal, or symptom logs, and schedule a 30-day review to decide whether to continue, adjust intensity, or add clinician support. Keep expectations realistic: sustained habit change usually grows from consistent small wins rather than big, sudden shifts. If you find the tech frustrating, contact support early—many platforms provide step-by-step help to make sure the tool helps you, not hinders you.
Wrap-Up: How Virtual Coaches Fit Into a Health Plan

Virtual health coaches can be a practical, personalized bridge between clinic visits and day-to-day life. For many people managing chronic conditions or trying to build healthier routines, these services offer structured guidance, measurable goals, and on-demand support that make progress feel more possible. Choose a coach that matches your condition and preferred level of human contact, verify clinical partnerships or published outcomes, and confirm cost or employer coverage before committing. Use short trials and a 30-day check-in to see whether the program fits your rhythm and delivers steady, manageable progress. Remember that AI and connected devices can enhance personalization, but human oversight and clear privacy practices are essential. If you’re supporting an older loved one, prioritize simple tech, clear onboarding, and options for phone-based coaching. Above all, treat digital coaching as one tool in a broader care plan—something that can complement your clinician’s advice, help you form sustainable habits, and make day-to-day health tasks feel more doable and supported.