9 Things That Can Affect How Your Body Processes Medication
When you swallow a pill or receive an injection, you might assume that the medication will work exactly as intended, but the reality is far more complex. Your body's ability to process medication—known as pharmacokinetics—involves an intricate dance of absorption, distribution, metabolism, and elimination that can vary dramatically from person to person. This process is influenced by a multitude of factors, ranging from your genetic makeup and age to what you ate for breakfast and whether you've been taking other medications. Understanding these variables is crucial not only for healthcare providers prescribing treatments but also for patients who want to maximize their medication's effectiveness while minimizing potential side effects. The way your body handles medication can mean the difference between therapeutic success and treatment failure, or even between safety and toxicity. Some people may need higher doses to achieve the same effect, while others might experience adverse reactions at standard dosages. By exploring the nine key factors that influence medication processing, we can better understand why personalized medicine is becoming increasingly important and why a one-size-fits-all approach to medication dosing is often inadequate for optimal patient care.
1. Genetic Variations - Your DNA's Role in Drug Response

Your genetic code serves as a blueprint that significantly influences how your body processes medications, with variations in specific genes determining whether you're a fast, slow, or normal metabolizer of certain drugs. The cytochrome P450 enzyme system, particularly enzymes like CYP2D6, CYP2C19, and CYP3A4, plays a crucial role in breaking down many common medications, and genetic polymorphisms in these enzymes can dramatically alter drug effectiveness and safety. For instance, individuals with certain genetic variants may metabolize codeine too quickly, leading to dangerous levels of morphine in their system, while others may not convert codeine to morphine at all, rendering the pain medication ineffective. Similarly, genetic variations affect how people respond to blood thinners like warfarin, with some requiring significantly higher or lower doses based on their genetic profile. Pharmacogenomics testing is becoming increasingly available and can help healthcare providers tailor medication choices and dosages to individual genetic profiles. This personalized approach can prevent adverse drug reactions, improve therapeutic outcomes, and reduce the trial-and-error process often associated with finding the right medication. As our understanding of genetic influences on drug metabolism continues to expand, genetic testing may become a standard part of medication prescribing, particularly for drugs with narrow therapeutic windows or high potential for adverse effects.
2. Age-Related Changes - How Time Affects Drug Processing
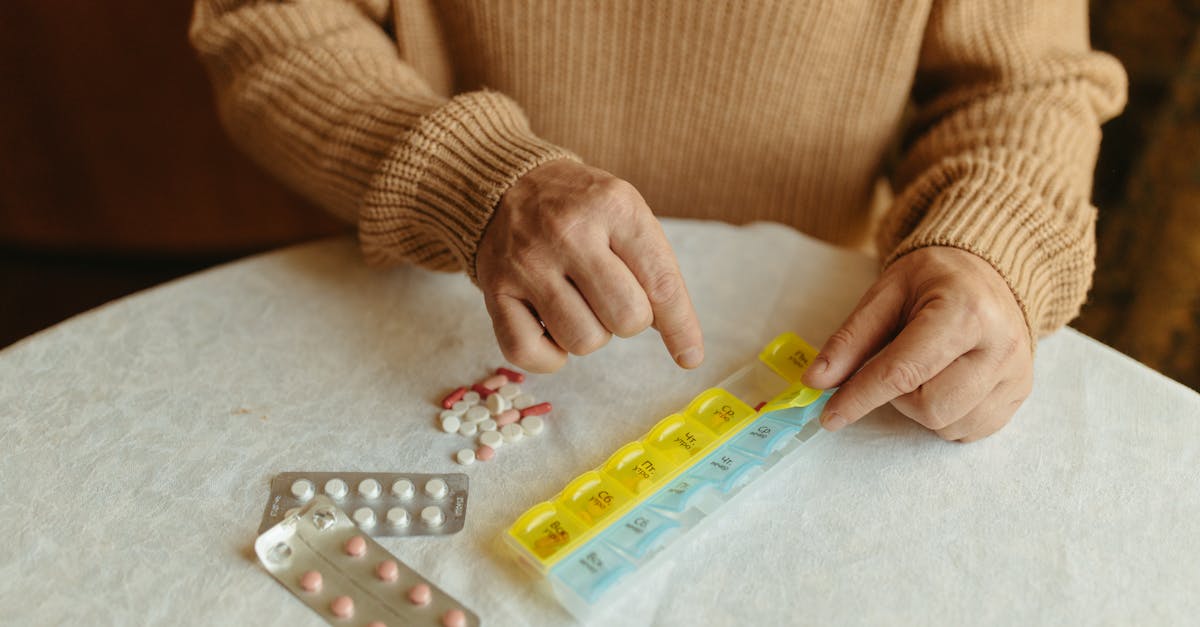
As we age, our bodies undergo significant physiological changes that profoundly impact how medications are absorbed, distributed, metabolized, and eliminated, making age one of the most critical factors in drug processing. In elderly patients, decreased gastric acid production can affect the absorption of certain medications, while reduced blood flow to the gastrointestinal tract may slow the rate at which drugs enter the bloodstream. The aging process also brings changes in body composition, with decreased muscle mass and increased fat tissue altering the distribution of medications throughout the body—fat-soluble drugs may have prolonged effects, while water-soluble drugs may reach higher concentrations due to reduced body water content. Perhaps most significantly, liver and kidney function typically decline with age, leading to slower drug metabolism and elimination, which can result in medication accumulation and increased risk of toxicity if doses aren't appropriately adjusted. Additionally, older adults often take multiple medications simultaneously, increasing the complexity of drug interactions and the potential for adverse effects. The blood-brain barrier may also become more permeable with age, making elderly patients more susceptible to central nervous system side effects from medications. Healthcare providers must carefully consider these age-related changes when prescribing medications to older adults, often starting with lower doses and monitoring more closely for both therapeutic effects and adverse reactions.
3. Gender Differences - How Sex Hormones and Biology Influence Drug Response

Biological sex and gender-related factors create significant differences in how men and women process medications, stemming from variations in body composition, hormone levels, enzyme activity, and organ function. Women typically have a higher percentage of body fat and lower muscle mass compared to men, which affects the distribution of fat-soluble and water-soluble drugs differently between the sexes. Hormonal fluctuations throughout the menstrual cycle, pregnancy, and menopause can dramatically alter drug metabolism, with estrogen and progesterone levels influencing the activity of various drug-metabolizing enzymes. For example, oral contraceptives can affect the metabolism of certain medications, potentially reducing their effectiveness or increasing side effects. Women also tend to have slower gastric emptying times, which can affect drug absorption, and generally have lower levels of gastric acid, potentially impacting the bioavailability of certain medications. Kidney function differences between men and women can affect drug elimination, with women typically having lower creatinine clearance rates. Additionally, women are more likely to experience certain types of adverse drug reactions, including cardiac arrhythmias from some medications and liver toxicity from others. The underrepresentation of women in clinical trials historically has meant that many medications were primarily tested in men, leading to dosing recommendations that may not be optimal for women. This recognition has led to increased focus on sex-specific research and the development of gender-sensitive prescribing guidelines.
4. Food and Dietary Interactions - When What You Eat Affects What You Take

The timing, composition, and quantity of food consumed can significantly influence medication absorption, effectiveness, and safety through various mechanisms that alter drug bioavailability and metabolism. Some medications require food for optimal absorption, as the presence of dietary fats can enhance the uptake of fat-soluble drugs, while others must be taken on an empty stomach to prevent food from interfering with absorption or causing drug degradation in the acidic environment created by eating. Grapefruit juice is perhaps the most well-known food-drug interaction, as it contains compounds that inhibit intestinal CYP3A4 enzymes, leading to increased blood levels of many medications including certain statins, calcium channel blockers, and immunosuppressants, potentially causing dangerous side effects. High-fiber foods can bind to certain medications in the digestive tract, reducing their absorption, while calcium-rich foods can interfere with the absorption of antibiotics like tetracycline and fluoroquinolones by forming insoluble complexes. Vitamin K-rich foods can counteract the effects of blood thinners like warfarin, requiring careful dietary monitoring and potential dose adjustments. The timing of meals relative to medication administration is equally important—some drugs work better when taken with food to reduce stomach irritation, while others need to be taken on an empty stomach for maximum absorption. Additionally, alcohol consumption can affect drug metabolism by either inhibiting or inducing liver enzymes, potentially leading to increased toxicity or reduced effectiveness of medications.
5. Liver Function - The Body's Primary Drug Processing Center
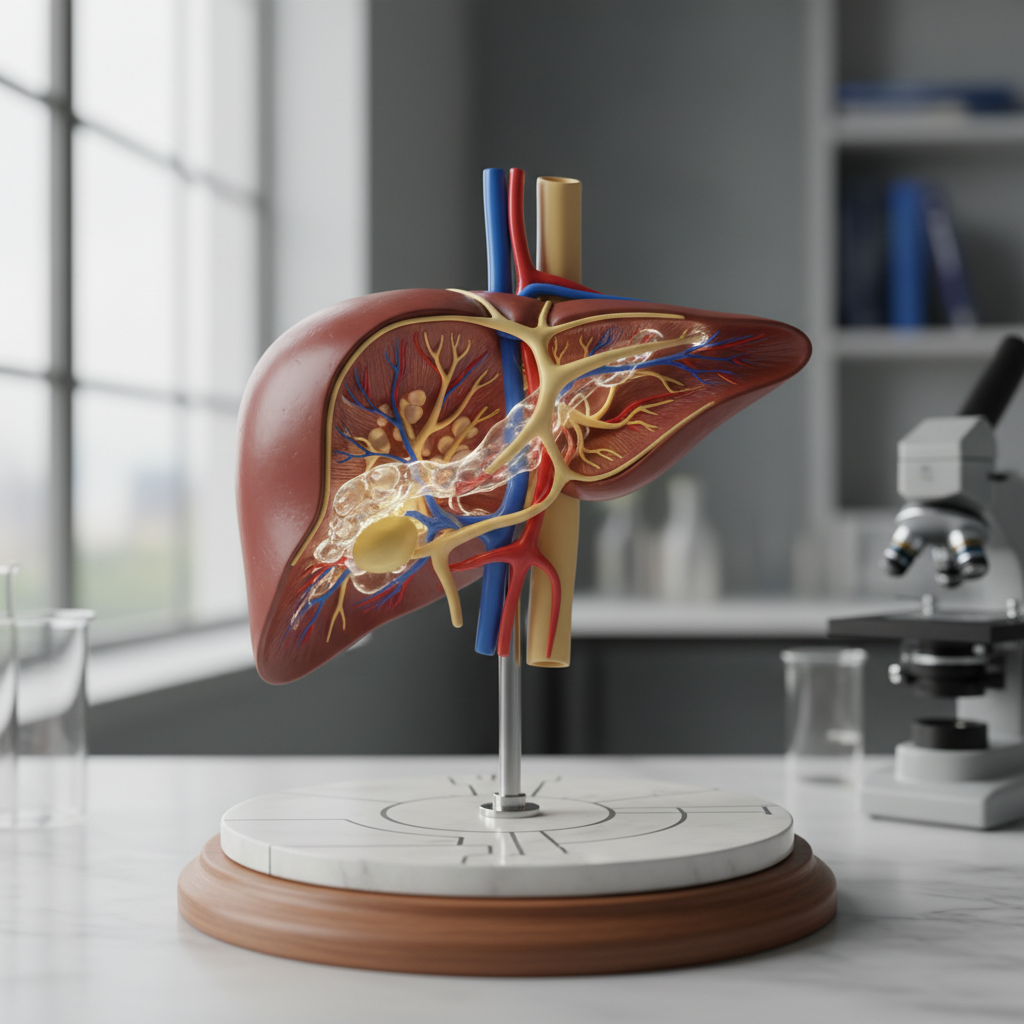
The liver serves as the body's primary drug-processing facility, responsible for metabolizing the majority of medications through complex enzymatic pathways, making liver health and function critical determinants of drug effectiveness and safety. This vital organ contains numerous enzyme systems, particularly the cytochrome P450 family, which transform medications into active metabolites or prepare them for elimination from the body. When liver function is compromised due to conditions such as hepatitis, cirrhosis, fatty liver disease, or acute liver injury, the metabolism of many drugs becomes significantly impaired, leading to prolonged drug action and increased risk of toxicity. Patients with liver disease often require substantial dose reductions or alternative medications to prevent dangerous accumulations of drugs in their system. The liver's ability to produce proteins, including albumin, also affects drug distribution, as many medications bind to these proteins for transport through the bloodstream—reduced protein production can lead to higher levels of free, active drug. Additionally, liver disease can affect bile production and flow, which impacts the elimination of certain medications that are excreted through the bile into the intestines. Chronic alcohol use can induce certain liver enzymes, leading to faster metabolism of some drugs and potentially reducing their effectiveness, while acute alcohol consumption can inhibit these same enzymes, causing drug accumulation. Regular monitoring of liver function through blood tests is essential for patients taking medications that are heavily metabolized by the liver, and healthcare providers must carefully adjust dosing regimens based on liver function status.
6. Kidney Function - The Gateway for Drug Elimination

The kidneys play a crucial role in medication processing by filtering drugs and their metabolites from the blood and eliminating them through urine, making kidney function a critical factor in determining appropriate drug dosing and preventing medication toxicity. When kidney function declines due to chronic kidney disease, acute kidney injury, or age-related changes, the elimination of many medications becomes significantly impaired, leading to drug accumulation and potential toxicity if doses aren't appropriately adjusted. The glomerular filtration rate (GFR) serves as a key indicator of kidney function and is used to guide dosing adjustments for medications that are primarily eliminated through the kidneys. Drugs such as digoxin, lithium, and many antibiotics require careful dose modifications in patients with reduced kidney function to prevent dangerous accumulations. The kidneys also play a role in drug metabolism through specialized enzymes, and kidney disease can affect the production of hormones like erythropoietin and the activation of vitamin D, potentially influencing the body's response to certain medications. Dehydration can temporarily reduce kidney function and affect drug elimination, while certain medications can themselves cause kidney damage, creating a complex interplay between drug therapy and kidney health. Patients with kidney disease often require more frequent monitoring of drug levels and kidney function tests to ensure safe and effective medication therapy. Additionally, dialysis can remove certain medications from the blood, requiring timing adjustments and potential supplemental dosing for patients undergoing this treatment.
7. Drug Interactions - When Medications Interfere with Each Other

The simultaneous use of multiple medications can create complex interactions that significantly alter how each drug is processed, potentially leading to enhanced effects, reduced efficacy, or dangerous side effects through various mechanisms of interference. Drug interactions can occur at multiple levels: during absorption, where one medication may bind to another in the digestive tract; during distribution, where drugs compete for protein binding sites; during metabolism, where one drug may inhibit or induce the enzymes responsible for metabolizing another; and during elimination, where drugs may compete for the same transport systems in the kidneys. For example, certain antibiotics can inhibit liver enzymes, leading to increased levels of blood thinners and elevated bleeding risk, while some antacids can reduce the absorption of other medications by altering stomach pH or binding to drugs in the digestive tract. Enzyme induction by medications like rifampin or certain anticonvulsants can accelerate the metabolism of other drugs, potentially reducing their effectiveness and requiring dose adjustments. The risk of drug interactions increases exponentially with the number of medications a patient takes, making polypharmacy a significant concern, particularly in elderly patients who often take multiple chronic medications. Healthcare providers must carefully review all medications, including over-the-counter drugs and supplements, when prescribing new treatments, and patients should always inform their healthcare team about all substances they're taking to prevent potentially dangerous interactions.
8. Body Weight and Composition - Size Matters in Drug Processing

Body weight and composition significantly influence medication processing through effects on drug distribution, metabolism, and elimination, with both obesity and underweight conditions presenting unique challenges for optimal drug dosing. In obese patients, the increased volume of distribution for fat-soluble drugs can lead to prolonged drug effects, while the larger body mass may require higher doses of water-soluble medications to achieve therapeutic levels. Additionally, obesity is often associated with altered liver enzyme activity, changes in kidney function, and increased cardiac output, all of which can affect how medications are processed. The distribution of body fat also matters—central obesity may affect drug metabolism differently than peripheral fat distribution due to differences in blood flow and metabolic activity. Conversely, underweight patients or those with muscle wasting may have reduced protein binding sites for medications and altered drug distribution, potentially leading to higher free drug concentrations and increased risk of side effects. Changes in body composition due to illness, aging, or medical treatments can also affect drug processing—for instance, patients with heart failure may have altered drug distribution due to fluid retention, while those with cancer cachexia may have reduced drug metabolism capacity. The challenge for healthcare providers is that many dosing guidelines are based on studies in patients with normal body weight and composition, making it necessary to carefully adjust doses and monitor responses in patients with significantly different body habitus.
9. Smoking and Substance Use - Chemical Influences on Drug Metabolism
Smoking tobacco and the use of various substances can dramatically alter drug metabolism through their effects on liver enzymes and other physiological processes, creating significant challenges for medication management and therapeutic outcomes. Tobacco smoke contains numerous compounds that induce certain cytochrome P450 enzymes, particularly CYP1A2, leading to faster metabolism of many medications including theophylline, clozapine, and some antidepressants, often requiring higher doses to achieve therapeutic effects in smokers. When smokers quit, these enzyme levels gradually return to normal, potentially leading to drug toxicity if doses aren't appropriately reduced. Alcohol use can have complex effects on drug metabolism, with chronic consumption typically inducing liver enzymes and acute use inhibiting them, creating unpredictable interactions with medications. Recreational drugs such as marijuana, cocaine, and amphetamines can also affect drug metabolism and may interact dangerously with prescription medications, potentially causing cardiovascular complications or altered mental status. Additionally, smoking affects cardiovascular and respiratory function, which can influence drug distribution and elimination, while also potentially counteracting the therapeutic effects of certain medications used to treat smoking-related diseases. The use of nicotine replacement therapies or smoking cessation medications adds another layer of complexity to drug interactions. Healthcare providers must obtain honest information about substance use to make appropriate prescribing decisions, and patients should be counseled about the potential need for dose adjustments when starting or stopping smoking or other substance use.
10. Disease States and Medical Conditions - How Illness Affects Drug Processing
Various disease states and medical conditions can significantly alter medication processing by affecting the organs responsible for drug absorption, distribution, metabolism, and elimination, requiring careful consideration and often dose adjustments to maintain therapeutic efficacy and safety. Gastrointestinal diseases such as Crohn's disease, celiac disease, or gastric bypass surgery can dramatically affect drug absorption by altering the structure and function of the digestive tract, potentially reducing bioavailability and requiring alternative routes of administration or higher doses. Cardiovascular diseases can affect drug distribution by altering blood flow to various organs, including the liver and kidneys, potentially slowing drug metabolism and elimination. Heart failure, in particular, can lead to reduced cardiac output and altered drug distribution, while also potentially causing liver congestion that impairs drug metabolism. Thyroid disorders significantly impact drug metabolism, with hyperthyroidism generally increasing metabolic rate and drug clearance, while hypothyroidism tends to slow drug processing. Diabetes can affect drug absorption through gastroparesis and may alter kidney function over time, affecting drug elimination. Inflammatory conditions and infections can alter drug metabolism by affecting liver enzyme activity and protein production, while also potentially changing drug distribution due to altered blood flow and vascular permeability. Mental health conditions may affect medication adherence and the body's stress response, which can influence drug effectiveness. Understanding these disease-drug interactions is crucial for healthcare providers to optimize medication therapy and prevent adverse outcomes in patients with complex medical conditions.