Warning Signs Of Acute Chest Syndrome
Acute chest syndrome, a life-threatening complication of sickle cell anemia, is characterized by a range of symptoms that occur when sickle cells clump together inside of the lungs. Sickle cells are only present in the blood of sickle cell anemia patients, so acute chest syndrome only occurs in these individuals. The red blood cells in individuals with sickle cell anemia are irregularly shaped and non-functional. Clumps of these sickle cells that develop in the lungs can cause an obstruction in normal blood flow through the lungs. They also can impair the process of carbon dioxide-oxygen exchange that occurs between the lungs and blood. No single condition causes acute chest syndrome, but certain conditions can trigger it, including pneumonia, asthma, and pulmonary embolism. Acute chest syndrome is diagnosed through the use of a chest x-ray in patients with sickle cell anemia.
Shortness Of Breath

Shortness of breath (dyspnea) is described as the sensation of tightness in the chest, a feeling of suffocation, and being unable to inhale enough air. Shortness of breath occurs in a healthy individual when they participate in strenuous exercise, are obese, in conditions of extreme temperatures, and at high altitudes. The sensation of dyspnea occurs when an individual is breathing at a higher rate than normal. An increased breathing rate is a common manifestation of acute chest syndrome because of how it affects the mechanism the body uses to regulate breathing. Respiration rate is managed by a combination of interactions between the brain, chemicals in the air, and chemicals in the blood. The amount of carbon dioxide, oxygen, and hemoglobin in the blood all have an influence on the rate of breathing. In acute chest syndrome, the sickle cells clump in the lungs and stop adequate oxygen exchange in the blood. This insufficient oxygen exchange causes blood carbon dioxide levels to increase. The brain detects this increase, and it tells the lungs to breathe faster and deeper. The fast and deep breathing in individuals with acute chest syndrome is what makes them feel like they have shortness of breath.
Low Oxygen Levels
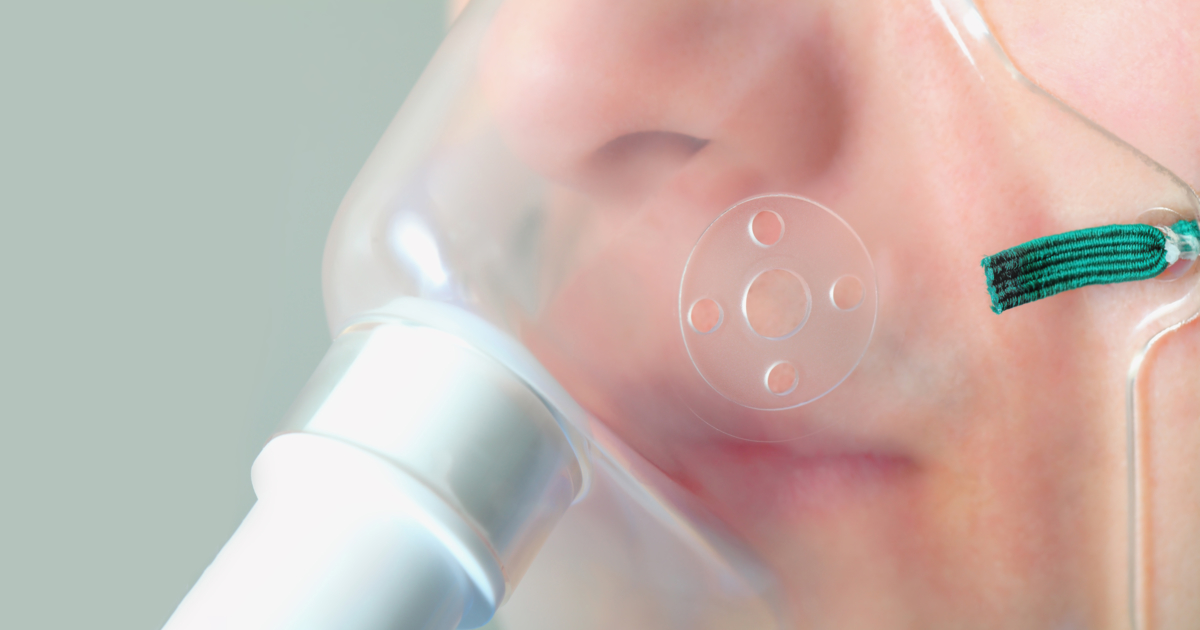
Acute chest syndrome commonly presents with low oxygen levels that accompany other symptoms. General low oxygen levels happen because of a few processes that occur in sickle cell anemia patients. The red blood cells in individuals who have sickle cell anemia have hemoglobin that is irregularly shaped and does not function to carry oxygen. The presence of these abnormal red blood cells causes a decrease in the production of healthy red blood cells that can carry oxygen. In addition, the red blood cells in sickle cell anemia patients have a much shorter lifespan at sixteen days than red blood cells in healthy individuals, which live for 120 days. Both mechanisms result in a low number of red blood cells circulating in the blood. When there are less red blood cells to transport oxygen, there will be a decreased oxygen levels in the blood. The clumping of sickle cells in the lungs that occurs in acute chest syndrome has a compounding effect on top of the other oxygen reducing factors of sickle cell anemia. It is this combination that makes the blood oxygen level in individuals with acute chest syndrome so abnormally low.
High Fever
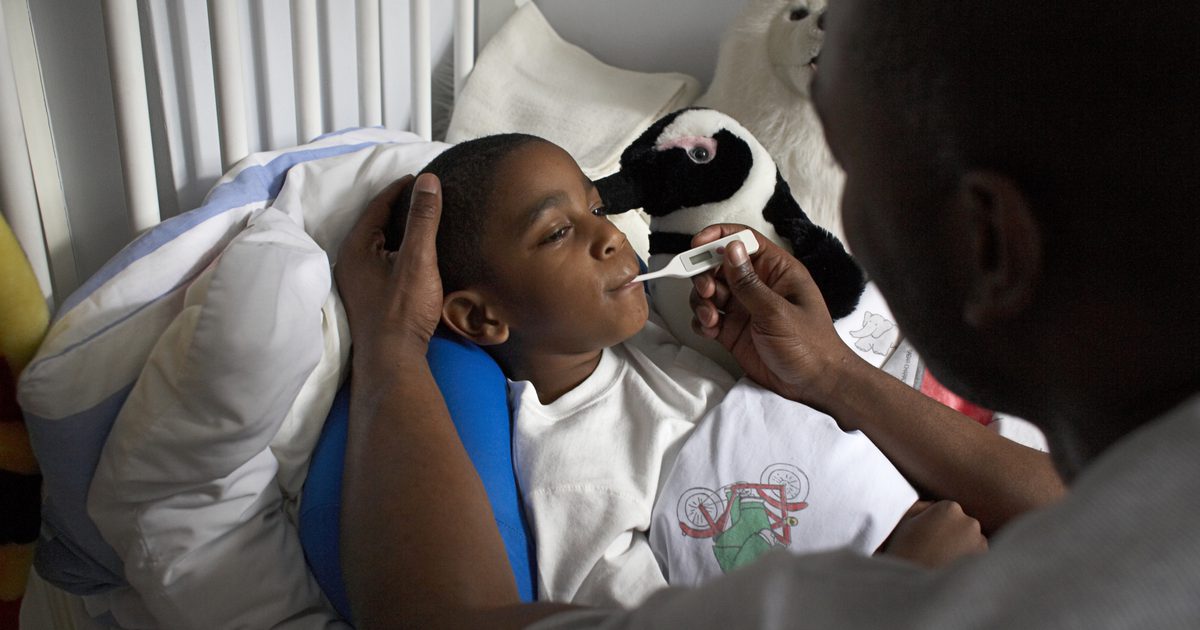
A high fever may manifest in individuals affected by acute chest syndrome. A high fever is any body temperature over 100.9 degrees Fahrenheit or 38.3 degrees Celsius. The high fever that commonly occurs in acute chest syndrome patients can be explained by the fact numerous infections can trigger acute chest syndrome. These infections include respiratory syncytial virus (RSV), pneumonia, sepsis, Streptococcus pneumoniae, Mycoplasma pneumoniae, and Haemophilus influenzae. When the body contracts an infection, the immune system uses its pathogen-fighting mechanisms to try and eradicate the virus or bacteria causing the infection. The immune system uses the body's temperature in an attempt to remove the environment within the body that is allowing the bacteria or virus to grow. Individuals who have sickle cell anemia have a weakened immune system because of its adverse effects on an immunity involved organ called the spleen. A weak immune system causes sickle cell anemia patients to have frequent infections. When one of these infections triggers acute chest syndrome, a high fever is likely to be present.
Severe Chest Pain

Patients affected by acute chest syndrome often report severe chest pain. The irregular shape of red blood cells in individuals with sickle cell anemia may cause problems with how the blood flows through their vessels. The round shape of healthy red blood cells allows for the smooth and consistent movement of blood throughout blood vessels. However, sickle cells will often get stuck in vessels, stick to each other, stick to vessel walls, and damage the lining of blood vessels. Sickle cells can obstruct blood flow in any region of the body, resulting in oxygen deprivation in the affected tissues. The oxygen-deprived cells begin to die off quickly, and as a result, the tissues that consist of dying cells may die as well. When tissues die anywhere in the body due to a lack of oxygen supply, it causes a significant amount of pain. In acute chest syndrome patients, the sickle cells clump together and produce one or more blood flow obstructions in the lungs. When lung tissues begin to die, the patient will feel severe chest pain as a result.
Productive Cough

A productive cough can be best described as a cough that produces any form of fluid such as blood, mucus, or any other liquid. A productive cough is commonly seen in individuals with acute chest syndrome triggered by an underlying infection. Due to their weakened immune system, sickle cell anemia patients are more likely to contract frequent infections. When an individual's body contracts an infection of the respiratory tract, the immune system activates a mechanism in an attempt to trap and remove the infectious pathogen from the body. The immune system calls for the production of more mucus in the respiratory tract than it usually would. The purpose of the extra mucus is to trap the infection causing pathogen and expel it through coughing or respiratory spasms. A sickle cell anemia patient with acute chest syndrome is likely to present with a productive cough because the cough is a common complication caused by the infection that triggered acute chest syndrome.
