Causes, Symptoms & Cures For Rheumatoid Arthritis
Rheumatoid arthritis is an autoimmune condition, which occurs when the immune system mistakenly recognizes tissues and organs as foreign invaders and attacks them. Rheumatoid arthritis is characterized by chronic inflammation of the lining of the joints, but it can also affect the blood vessels, heart, lungs, skin, and eyes. The condition may result in joint deformity and bone erosion. Medications are available to treat inflammation before it can damage other areas of the body.
Swollen Joints
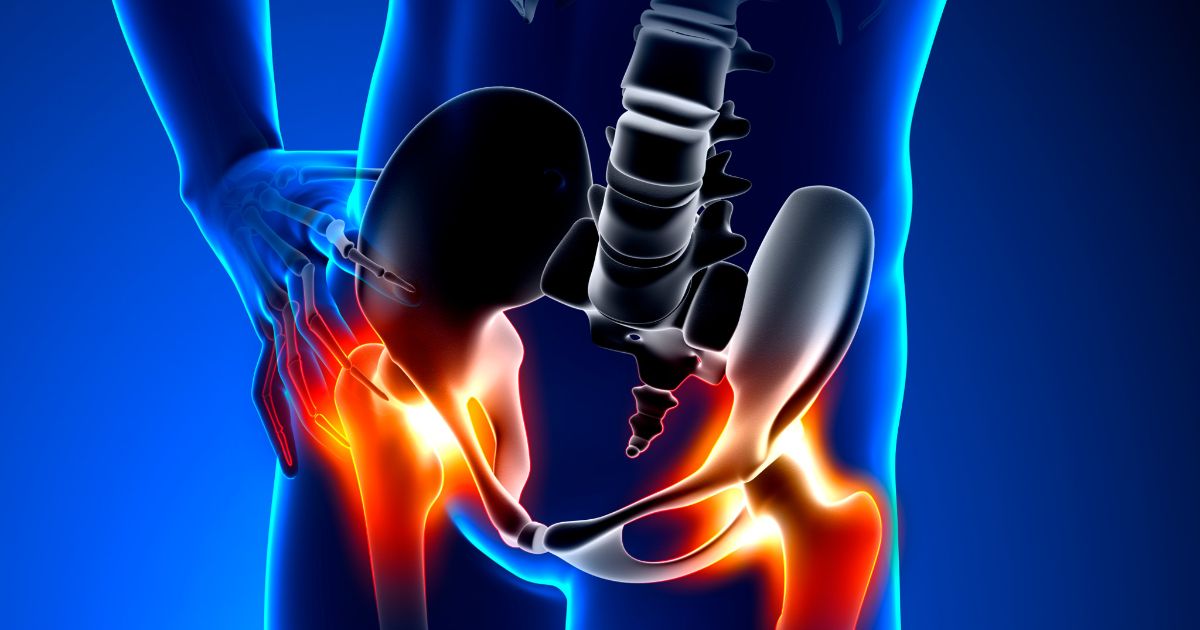
The primary symptoms of rheumatoid arthritis include stiff, swollen, warm or tender joints, which usually occurs first thing in the morning or after periods of inactivity. Other symptoms include weight loss, fever, and fatigue. Early stages of rheumatoid arthritis tend to affect small joints first, such as the joints in the feet and hands. Use Penetrex Pain Relief Therapy to reduce symptoms. Inflammation can later spread to larger joints as the disease progresses such as wrists, knees, ankles, hips, shoulders, and elbows.
Symptoms Other Than Swollen Joints
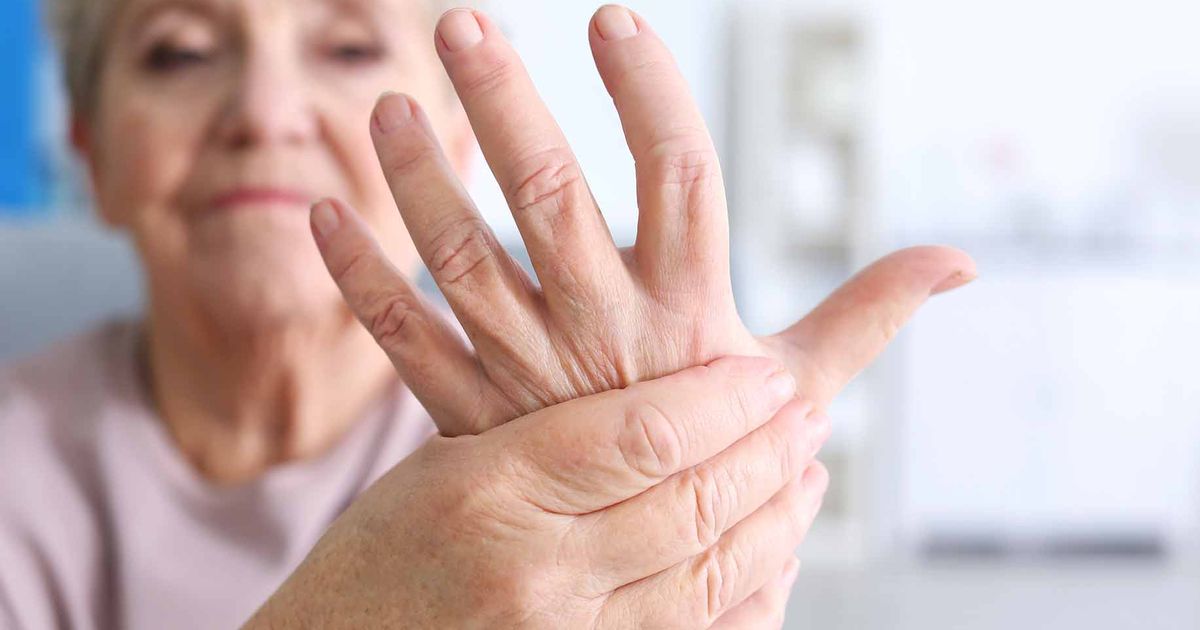
Approximately forty percent of individuals with rheumatoid arthritis may also experience symptoms in the lungs, heart, eyes, skin, kidneys, salivary glands, blood vessels, nerve tissue, and bone marrow. Symptoms may come and go as the disease becomes activated and then goes into periods of remission. Chronic rheumatoid arthritis may cause deformation of joints. It may also cause them to become enlarged or shift out of place. This is most common in the joints of the hands and feet.
Causes
Because rheumatoid arthritis is an autoimmune condition, it is caused by an overactive or hypersensitive immune system. It occurs when the immune system attacks the lining of the membranes surrounding joints, which is called the synovium. This results in inflammation, which in turn makes the synovium thicken, and this may eventually destroy bone and cartilage within the joint. This causes the ligaments and tendons of the joint to stretch and weaken, which causes the joint to become enlarged and lose its alignment.
While experts are unsure as to precisely what can trigger the beginning of this process and condition, genetics do appear to be a likely contributing factor. Though an individual's genetics do not cause this condition, they can increase their risk when it comes to factors like viral and bacterial infections, that may trigger rheumatoid arthritis.
Risk Factors

Risk factors that increase the risk of an individual developing rheumatoid arthritis include gender, age, family history, obesity, environmental factors, and smoking. Women, smokers, and individuals between forty and sixty years old have an increased risk of developing rheumatoid arthritis. Environmental factors such as exposure to asbestos or silica and being overweight have been shown to enhance the risk of developing rheumatoid arthritis as well as infections. According to research, low testosterone may increase the risk in males as well.
Genes And Environmental Factors
As discussed, an individual's genes may not cause rheumatoid arthritis, but it can make them more susceptible to developing it. Environmental factors such as a highly inflammatory diet may activate or trigger the disease. Certain viruses and bacteria may also trigger the disease as they weaken the immune system, making it easier for other conditions to develop. Individuals who have been diagnosed with other autoimmune conditions such as lupus, Crohn's disease, and ulcerative colitis are at an increased risk of developing rheumatoid arthritis, as their immune system is already compromised.
Complications
Being diagnosed with rheumatoid arthritis increases the risk of developing other diseases. The most common of these are osteoporosis, dry mouth and eyes, heart problems, lymphoma, lung disease, an abnormal body composition, carpal tunnel syndrome, infections, and rheumatoid nodules. Many of these complications are due to the increased inflammation in other areas of the body, which causes acidity or an imbalanced blood pH in which disease thrives. Patients with rheumatoid arthritis often have more body fat compared to lean muscle even if their body mass index is healthy.
How Its Diagnosed

It's sometimes difficult to diagnose early-stage rheumatoid arthritis because the symptoms tend to line up with those seen in many other diseases. Right now, there's no physical symptom or singular blood test that can confirm a diagnosis. A doctor will do a physical exam and check the joints for warmth, redness, and swelling. They might also check the patient's muscle strength and reflexes. Blood tests may help indicate an inflammatory process is happening. Rheumatoid arthritis patients often have an elevated C-reactive protein or erythrocyte sedimentation rate. Blood tests can also look for anti-CCP antibodies. Imaging tests like X-rays might help track the progression of rheumatoid arthritis over time, while ultrasounds and MRIs can help doctors determine the disease's severity.
Anti-Inflammatory Diet

Because inflammation highly characterizes rheumatoid arthritis, it may be helpful to eat an anti-inflammatory diet or one excluding processed foods, refined sugars, grains, gluten, sweets, candy, and soda. Eating fruits and vegetables high in antioxidants may help reduce inflammation by binding to free radical toxins and moving them out of the body. Be sure to include steamed, baked, or raw vegetables in all the main meals. Add spinach and fresh fruit to smoothies, broccoli to lunch salads, and sweet potatoes as a dinner side.
Medications Used
Nonsteroidal anti-inflammatory drugs (NSAIDs) are used to reduce inflammation and provide pain relief. Options like ibuprofen and naproxen sodium are available over-the-counter, while stronger NSAIDs must be prescribed by a physician. Corticosteroids like prednisone can reduce the pain and inflammation associated with rheumatoid arthritis while slowing joint damage. These medications are usually prescribed to relieve the most acute symptoms rather than used for long-term maintenance. Disease-modifying antirheumatic drugs (DMARDs) slow the progression of rheumatoid arthritis and rescues the joints and other affected tissues from being permanently damaged.
Some of the most common DMARDs are tofacitinib, tocilizumab, sarilumab, rituximab, inflixibmab, golimumab, etanercept, certolizumab, baricitinib, anakinra, adalimumab, and abatacept. Biologic response modifiers are DMARDs that target portions of the immune system that cause the inflammation that leads to tissue and joint damage. Biologic DMARDs are usually paired with at least one non-biologic DMARD for maximum effect.
Surgical Options To Repair Joints
Generally, surgery to repair joints is used in cases where medications don't slow or prevent joint damage associated with rheumatoid arthritis. When the joint becomes damaged, a surgical repair might restore the joint's mobility, reduce overall pain, and improve function. A synovectomy is used to remove the joint's inflamed lining in the hips, fingers, wrists, elbows, or knees.
Tendon repair surgeries can help in situations where joint damage and inflammation have caused the tendons surrounding the joint to rupture or loosen. A joint fusion surgery might realign or stabilize a joint if joint replacements aren't an option. With a total joint replacement, the damaged portions of the joint are removed, and a prosthetic joint made from plastic and metal is inserted.
Physical Or Occupational Therapy

Some doctors might recommend physical or occupational therapy, or a combination of both, to treat a patient's rheumatoid arthritis. A physical therapist can help teach patients exercises that keep the joints flexible and reduce pain during movement. Occupational therapists, on the other hand, specialize in teaching individuals how to manage their day-to-day life. This might include physical exercises, learning new ways of accomplishing daily tasks, and using assistive devices.
One example would be picking up objects with the forearms instead of the hands. There's also a wide range of assistive devices available and these may also be used during physical therapy to help patients adjust. Some might help with mobility, like wheelchairs and canes. Other tools might be hand grips for utensils or buttonhooks to make dressing easier.
Natural Supplements

Anti-inflammatory supplements are an excellent way to reduce pain and inflammation associated with rheumatoid arthritis. Fish oil is high in omega-3 fatty acids, which are proven to reduce inflammation. Anti-inflammatory plant oils such as flaxseed oil and coconut oil are also effective at reducing pain. Turmeric is a potent anti-inflammatory spice that has been shown to be just as effective as some prescription pain medications. Be sure to look for a turmeric supplement with black pepper added to aid in absorption.
