Guide To Diagnosing And Treating Christmas Disease (Hemophilia B)
Christmas disease, also called hemophilia B, is an uncommon bleeding disorder that causes a deficiency of a protein called coagulation factor IX, which is essential for blood clotting. Hemophilia B is caused by a mutation in the gene that encodes instructions for the production of factor IX. Healthy blood clotting requires many clotting factors, including factor IX, to prevent excessive blood loss. Affected individuals bleed longer than unaffected individuals. Factor IX activity level is what determines hemophilia B severity. Mild hemophilia B falls between five to forty percent of normal levels, and severe hemophilia B is one percent or less of normal levels.
Common symptoms include excessive bleeding and bruising following a dental procedure, injury, surgery, or trauma. Bleeding into the muscles and joints, nosebleeds, bloody urine, and bloody stools may also occur. Several tests may be used to make a hemophilia B diagnosis, and a few treatment methods are available.
Factor IX Test
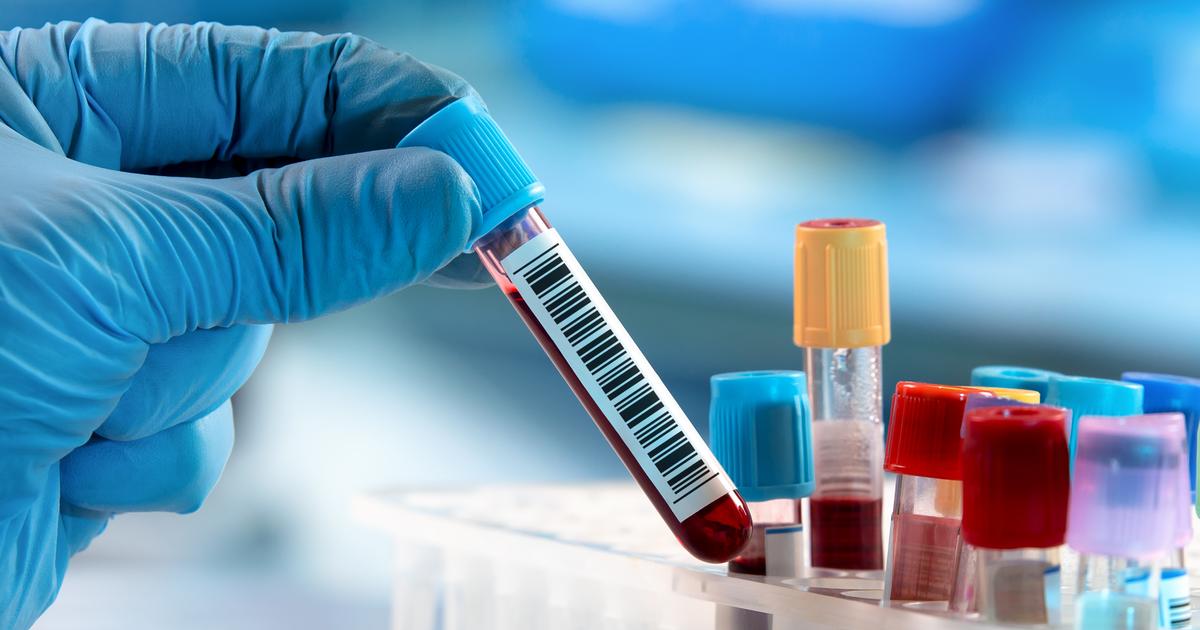
A factor IX test can be utilized by a physician to help make a diagnosis upon suspicion an individual may have hemophilia B. The results of an individual's activated cephalin time (ACT) along with a family history of hemophilia B may prompt a physician to order the factor IX clotting assay. Factor IX is made in an individual's liver and has a half-life of between eighteen and twenty-four hours. Normal values of factor IX in a collected blood sample fall between fifty and two hundred percent of the reference value or the laboratory control.
A factor IX assay is typically performed on multiple compounded dilutions of the patient's blood plasma to eliminate circulating anticoagulant antibody interference. Usually, tests for factors VIII, XII, and XI are performed to confirm they are not partially or fully responsible for the abnormality in the previous test. Because lupus anticoagulant can cause inaccurate factor IX test results in a patient with lupus, a negative lupus anticoagulant test is required for the proper diagnosis of hemophilia B.
Activated Partial Thromboplastin Time Test
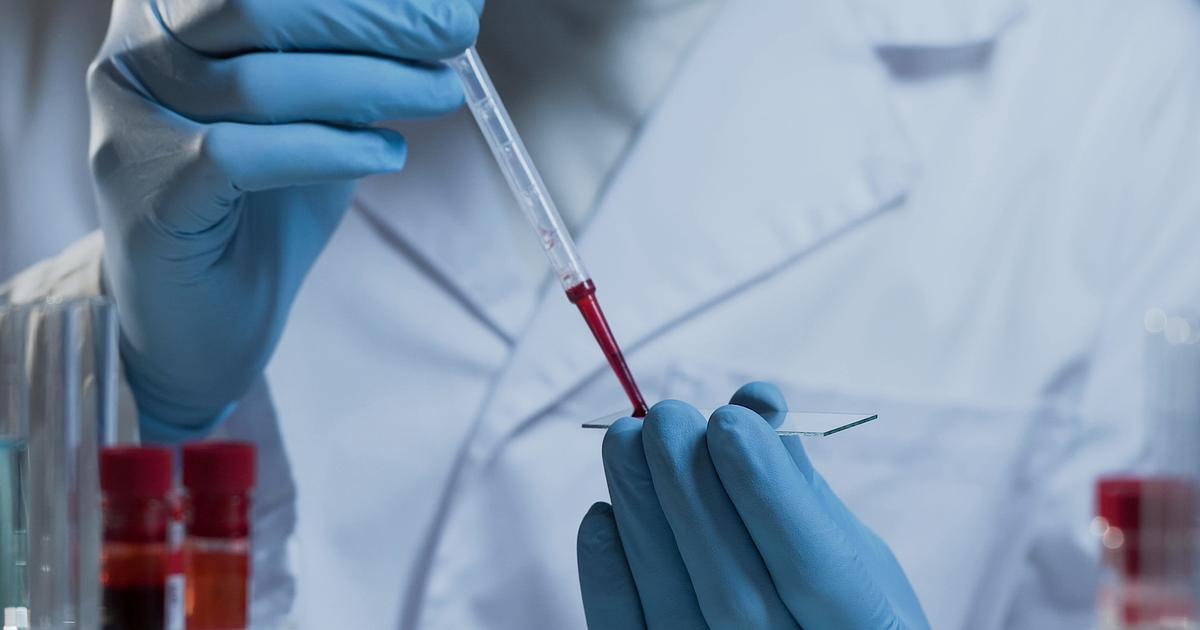
Activated partial thromboplastin clotting time (aPTT) is one of a handful of diagnostic coagulation tests that provides a measurement for the length of time it takes an individual's blood to form a clot. Blood clotting factors come together in a cascade process when a blood vessel is damaged to form a blood clot and stop bleeding. Clotting factors XII, IX, II, X, XI, VIII, V, fibrinogen, prekallikrein, and high-molecular-weight kininogen are components that make up the intrinsic clotting pathway and the common final pathway. These factors are measured in the aPTT test. The partial thromboplastin time test is performed before the activated partial thromboplastin time.
The difference between these two tests is a special activation solution is added to the sample for the aPTT that increases the clotting time to provide a smaller reference range. If both the PTT and aPTT tests yield abnormal results, it is suggested the patient has a deficiency of factor I, V, X, or II. A normal PTT with an abnormal aPTT result suggests the patient has a deficiency of factor IX, XIII, VIII, or X. The typical presentation for factor IX deficiency or hemophilia B is a normal PTT with a prolonged aPTT.
Preventative Blood Transfusions
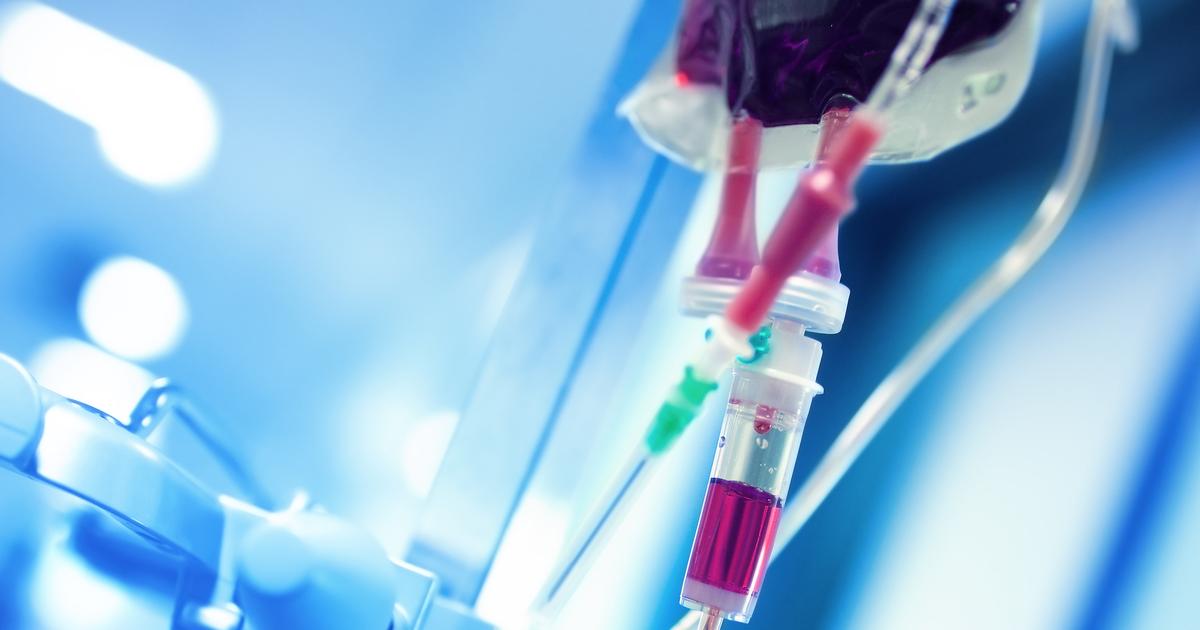
Preventative blood transfusions may be utilized as a part of a patient's treatment for their hemophilia B. Preventative blood transfusions are typically only needed in patients who have a severe degree of hemophilia B. The purpose of this preventative treatment method is to keep bleeding from occurring. This type of treatment may be referred to as prophylactic therapy and has proven to be effective at decreasing complications caused by recurrent bleeds. These complications may include intracranial hemorrhage and joint damage. Joint damage, in particular, is taken into consideration when a patient chooses to have prophylactic treatment because joint damage progressively worsens over their life even if they do not experience more bleeds in that joint.
Preventative blood transfusions are utilized in patients who have already had hemophilia-associated joint damage with the goal of minimizing inflammation, pain, and immobility. Depending on circumstances regarding transfusion availability, bleeding triggers, and the number of acceptable joint bleeds, preventative blood transfusions may not be the most ideal method of treatment.
Factor IX Injections
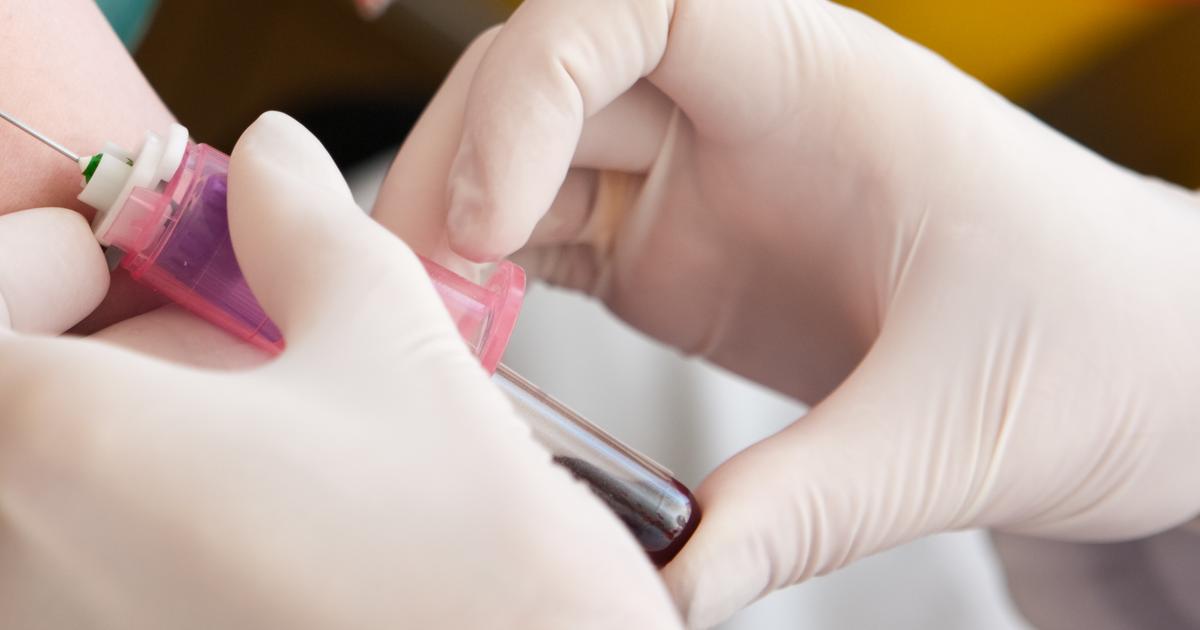
An individual affected by hemophilia B may choose to have factor IX injections to treat their disorder. Factor IX injections are most often administered in response to an individual's active bleeding episode. In some less common cases, factor IX injections may be utilized as prophylactic treatment. The factor IX complex used in these subcutaneous injections may contain an artificial, man-made derivative of factor IX or may be obtained from donor blood. Factor IX complexes made from human donor blood have been treated and purified through a specialized process to ensure no harmful viruses are present such as hepatitis C, hepatitis A, parvovirus B19, West Nile virus, HIV, and hepatitis B.
Factor IX complex injections come in the form of a dry powder medicine meant to be mixed with a liquid diluent prior to injection. Cases have been reported where regular use of factor IX injections have induced the production of an antibody against factor IX, making the injection less effective. Factor IX injections may be used as a preventative measure in hemophilia B patients undergoing any type of surgical procedure.
Desmopressin Acetate

Hemophilia B patients may benefit from the use of a medication called desmopressin acetate in situations that warrant blood-saving such as severe injury, childbirth, or invasive surgical procedures. Desmopressin acetate is derived from the naturally occurring antidiuretic hormone in the body. This medication is not specifically used for the treatment of hemophilia disorders but is used for a range of disorders that can cause an individual to bleed excessively in certain circumstances. Desmopressin acetate is not accepted as an officially approved treatment for hemophilia B due to conflicting study results showing improvement in some patients and no change in others.
The efficacy of desmopressin acetate for factor IX deficiency alone has not been proven. However, rare cases of individuals affected by a factor VII deficiency or Von Willebrand disease alongside factor IX deficiency may benefit from the use of desmopressin acetate. The mechanism thought to be behind the improvements seen in a portion of individuals who have factor IX deficiency and other bleeding disorders has to do with better adhesion of platelets to the blood vessel walls, increased general coagulability, and acceleration of fibrinogen formation.
