Guide To The Prevention And Treatment Of Hemolytic Uremic Syndrome
Hemolytic uremic syndrome is a condition that affects both the blood and blood vessels. The syndrome destroys red blood cells, and these destructed cells clog the kidneys, eventually leading to serious kidney failure. Hemolytic uremic syndrome often occurs in young children, and the majority of cases are caused by an infection. For children under five years old, the most common cause of hemolytic uremic syndrome is an E. coli infection. Some immunosuppressive and antimalarial medications may also cause this syndrome. In rare cases, it can be triggered by pneumonia, HIV or AIDS, and pregnancy. Symptoms generally include abdominal pain, bruising, bloody diarrhea, blood in the urine, fatigue, hypertension, and swelling of the face or extremities. Some patients may appear very pale, and they may also have confusion or experience seizures. To diagnose hemolytic uremic syndrome, doctors will perform blood and urine tests, and a stool culture is sometimes needed.
The steps outlined below are some of those most commonly recommended for the treatment and prevention of hemolytic uremic syndrome.
Platelet Transfusion

Platelet transfusions can improve blood clotting in patients with hemolytic uremic syndrome, and these transfusions are often needed when patients are experiencing bruising or blood in the urine or stool. Prior to a platelet transfusion, the patient will have a blood test to determine their platelet count to determine the transfusion's necessity. To administer the transfusion, a medical professional will start an intravenous line, and the transfusion itself usually takes around fifteen to thirty minutes. Medical staff will monitor the patient's blood pressure, pulse, and temperature during the transfusion. Side effects are rare, though they include increased temperature, shivering, itching, or a skin rash. Patients should tell staff immediately if they feel sick at any time during the transfusion. After the transfusion, the patient's platelet count will increase right away, and most patients feel a significant improvement in their energy levels. If necessary, repeated platelet transfusions can be given.
Keep reading to reveal more options for treating and preventing hemolytic uremic syndrome now.
Kidney Dialysis
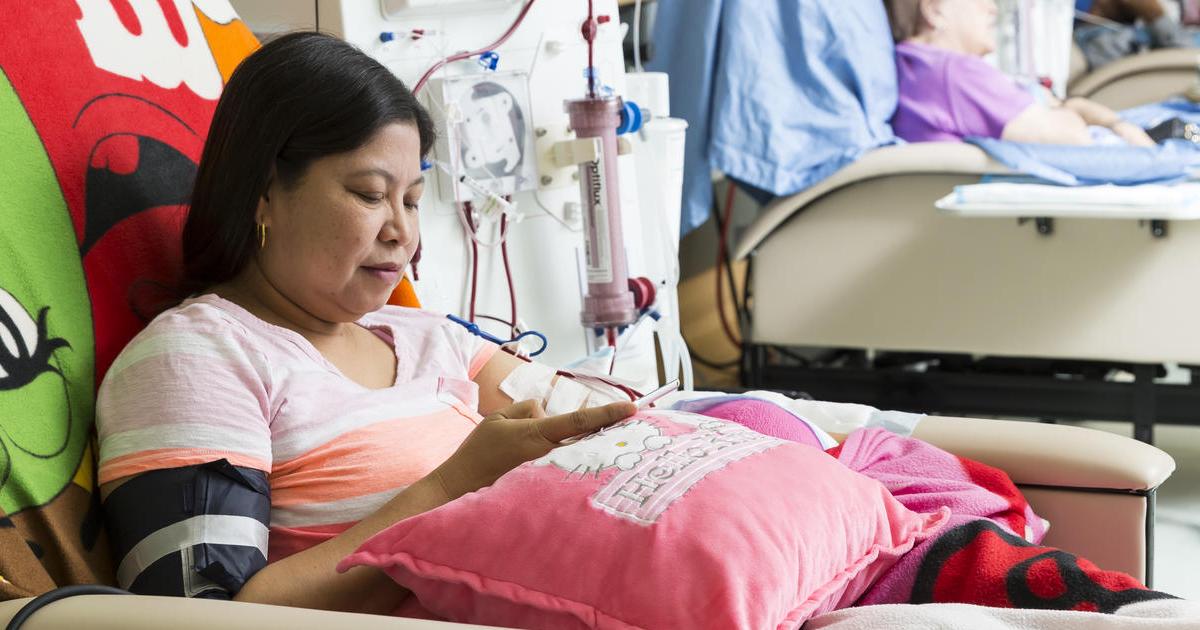
Kidney dialysis may be needed for patients with severe kidney damage as a result of hemolytic uremic syndrome. Normally, the kidneys filter waste products from the body. When they are not working properly, dialysis is used as a filtering system so the kidneys can heal. It can filter waste, salt, and excess water from the body, and it assists the body in maintaining proper levels of sodium and potassium. Dialysis also helps patients with hypertension by reducing blood pressure. Most patients with hemolytic uremic syndrome only need dialysis for a short time.
Hemodialysis and peritoneal dialysis are the two types of dialysis currently in use. Prior to the first dialysis session, patients may need to have a minor surgical procedure to establish an access point. This involves placing a tube in the arm or leg, and patients having peritoneal dialysis will have a catheter placed in the stomach. Patients having hemodialysis usually have sessions three times a week, and each treatment takes approximately four hours.
Uncover more details on preventing and treating hemolytic uremic syndrome now.
Red Blood Cell Transfusion
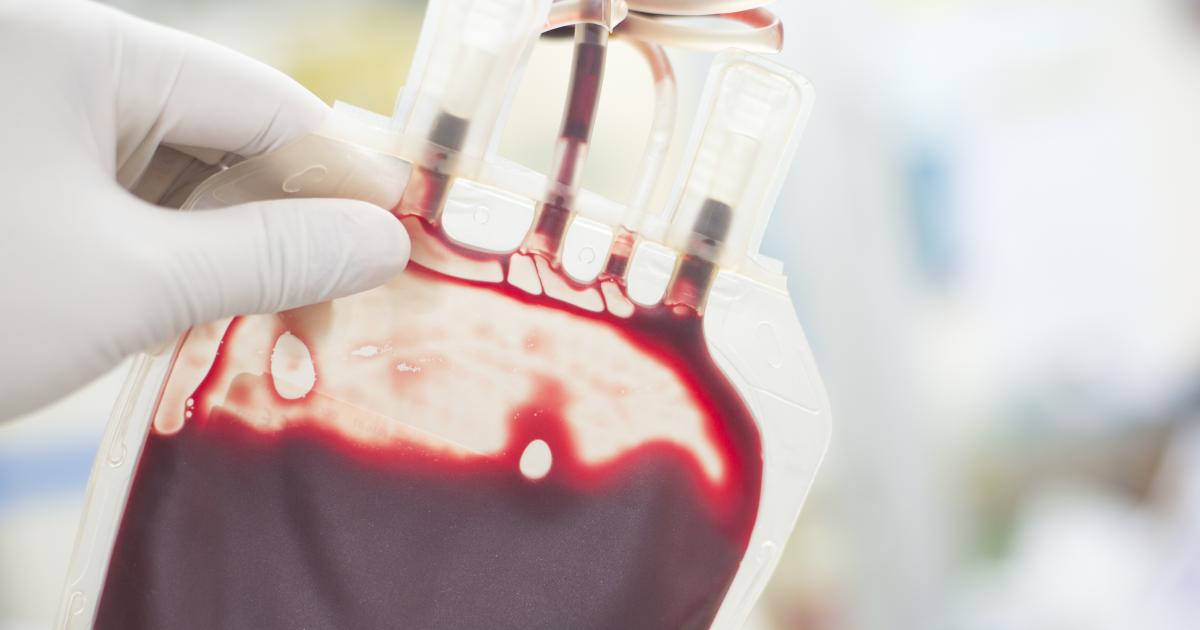
Hemolytic uremic syndrome patients may experience fatigue, chills, increased heart rate, jaundice, and dark urine. For these individuals, a red blood cell transfusion can help in reversing these symptoms and improving quality of life. Transfusions of red blood cells increase both hemoglobin and iron levels in the body, and they also raise the amount of oxygen in the blood. Patients will have complete blood counts before and after these transfusions to monitor progress. To give a red blood cell transfusion, a nurse will insert an intravenous line in the hand or arm, and the red blood cells are transfused over a period of one to four hours. Transfusions can be given in a doctor's office or at a hospital, and patients will be closely monitored for potential allergic reactions or other side effects. In particular, patients should alert staff if they develop any chest tightness, dizziness, nausea, itching, or breathing difficulties. The benefits of a red blood cell transfusion can last as long as two weeks, and repeated transfusions may be given as needed.
Learn more about how to prevent and treat hemolytic uremic syndrome now.
Replace Lost Fluids
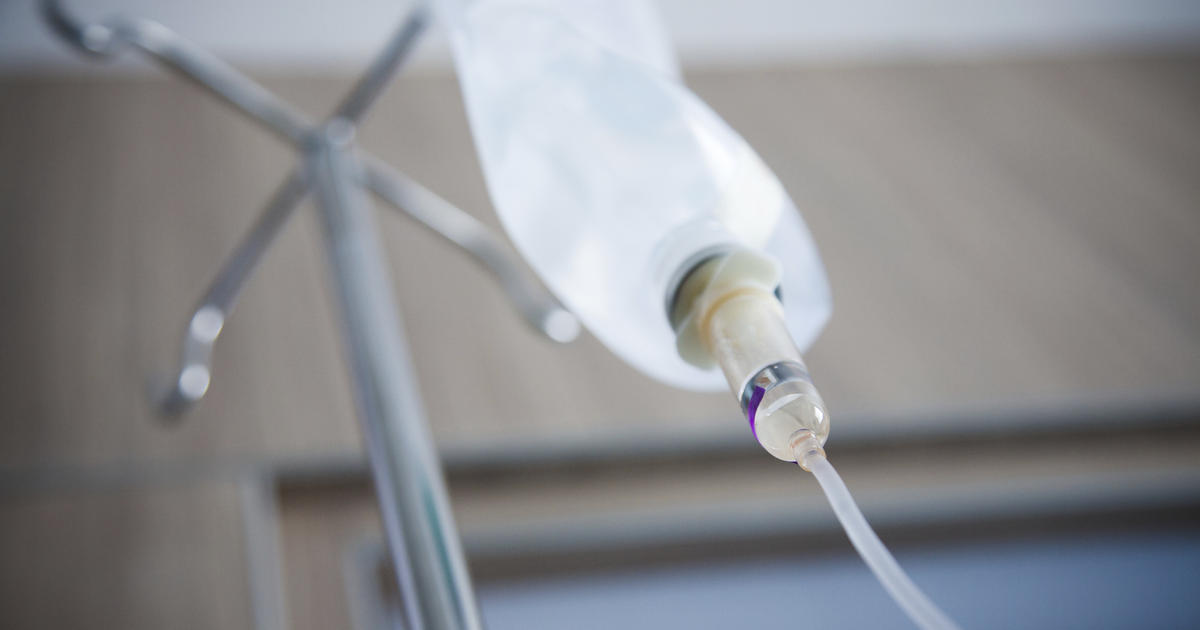
Patients with hemolytic uremic syndrome may sometimes lose fluids and electrolytes. This syndrome compromises kidney function and slows down the normal removal of fluids and waste products, so fluid replacement must be done very carefully. To replace lost fluids, patients will normally receive intravenous treatment, which is the most rapid method of fluid replacement, and it enables patients to feel better in the shortest possible amount of time. Normal saline solution and Ringer's lactate solution are both routinely used for fluid replacement. The dosage is based on weight, so patients will have their weight measured prior to receiving fluids. During fluid replacement, the patient's urine output will be monitored, and the doctor or nurse will determine when an adequate level of fluid replacement has been obtained. In some cases, oral methods may be used to replace lost fluids.
Get more details on options for the treatment and prevention of hemolytic uremic syndrome now.
Plasma Exchange
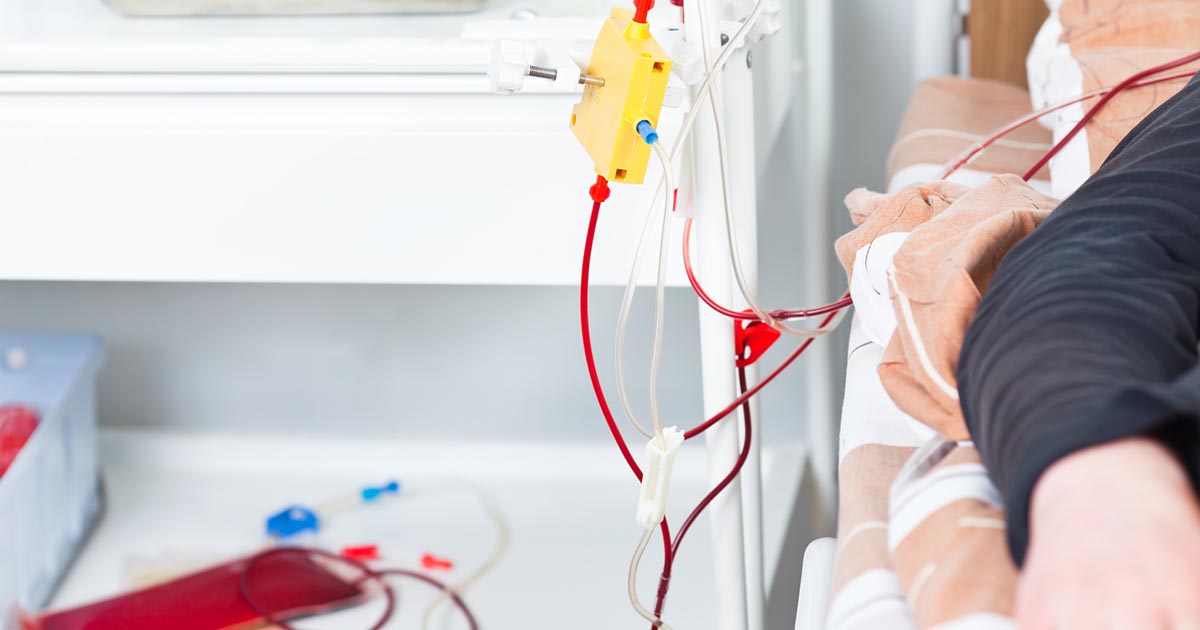
Plasma exchange is a method of cleaning the blood similar to dialysis. Also called plasmapheresis, this procedure involves replacing the patient's plasma with plasma from a donor. Plasma is the liquid part of the blood, and it contains proteins and nutrients that are crucial for overall health. To perform a plasma exchange, a nurse will insert two intravenous lines, one in each arm. The patient's blood will flow out of one of the lines and into a machine. The machine separates the patient's plasma from the rest of the blood cells, and the separated plasma is mixed with donor plasma. This mixture is then sent back into the patient's body through the second intravenous line. The treatment can take between two to four hours, and patients may need treatment two or three times each week for several weeks. While receiving treatment, the patient may have a lower than normal blood pressure, and nurses will carefully monitor this.
