How To Manage Von Willebrand Disease
Von Willebrand disease is a type of chronic bleeding disorder that reduces the blood's ability to clot normally. Except for cases of acquired von Willebrand disease that occur later in life, the other forms of this condition are all inherited (genetic). Patients with von Willebrand disease may experience heavy menstrual periods, nosebleeds that last longer than ten minutes, blood in the urine or stool, and easy bruising. Patients with this disorder may notice that their bruises feel or look lumpy, and female patients can have excessively long periods. In addition, patients with von Willebrand disease might bleed more heavily than usual after having dental work or surgery, and they could also bleed more than normal after a minor cut or other injuries.
To diagnose von Willebrand disease, patients will usually have several blood tests, including tests to check the levels of von Willebrand factor and factor VIII. A ristocetin cofactor activity blood test and a von Willebrand factor multimers test will also be performed. Treatment for this condition varies depending on the severity of a patient's symptoms.
The following lifestyle modifications and medical treatments are often beneficial for patients with von Willebrand disease.
Wearing A Medical ID Bracelet

Wearing a medical ID bracelet can be particularly useful for patients with von Willebrand disease. Since this disorder is lifelong and often causes excessive bleeding, it is important for school staff, healthcare professionals, and emergency medical technicians to be aware of the fact a patient has this disorder in the event of an unexpected injury or emergency situation. The medical ID bracelet can provide this crucial information to appropriate personnel if the patient is incapacitated or unconscious, and this knowledge might enable them to provide the appropriate additional medicines to reduce bleeding. Some medical bracelets have enough space to include the patient's emergency contact information as well, and this could assist hospital staff or others trying to treat the patient.
Keep reading to reveal more options for treating von Willebrand disease now.
Avoid Blood-Thinning Pain Medication

Patients who have von Willebrand disease need to avoid blood-thinning pain medication as this could trigger excessive bleeding. In particular, acetylsalicylic acid should not be used, and doctors may recommend that patients also avoid ibuprofen and naproxen as well. Patients should consult their hematologist before taking any over-the-counter pain relievers or natural remedies for pain relief. Most hematologists suggest patients with this condition take acetaminophen to treat pain. If acetaminophen is not sufficient to relieve a patient's pain, the doctor may be able to prescribe a stronger pain reliever that is still safe for patients with von Willebrand disease and will not thin the blood. In addition to medication, patients may also wish to try drug-free remedies for pain, including heating pads, ice packs, and TENS machines.
Uncover more von Willebrand disease treatments now.
Clot-Stabilizing Medication

Clot-stabilizing medication is one of the standard treatments doctors provide for most patients with von Willebrand disease. Known as anti-fibrinolytic medicines, these drugs reduce bleeding by slowing the rate at which blood clots break down. Doctors typically prescribe these to patients with von Willebrand disease before they undergo a tooth extraction or operation, and some patients will need to take these medicines after the procedures too. Some of the most commonly prescribed clot-stabilizing drugs are aminocaproic acid and tranexamic acid. Patients taking aminocaproic acid should be aware of potential side effects such as headaches, itching, ringing in the ears, skin rashes, vomiting, and nausea. Patients who have been prescribed tranexamic acid must remain vigilant for the development of muscle cramps, stomach pain, diarrhea, back pain, and fatigue. If any new symptoms or unpleasant side effects develop, patients should inform their hematologist. It may be possible to switch to another, more tolerable type of clot-stabilizing medication/
Get familiar with more ways to treat von Willebrand disease now.
Replacement Therapies
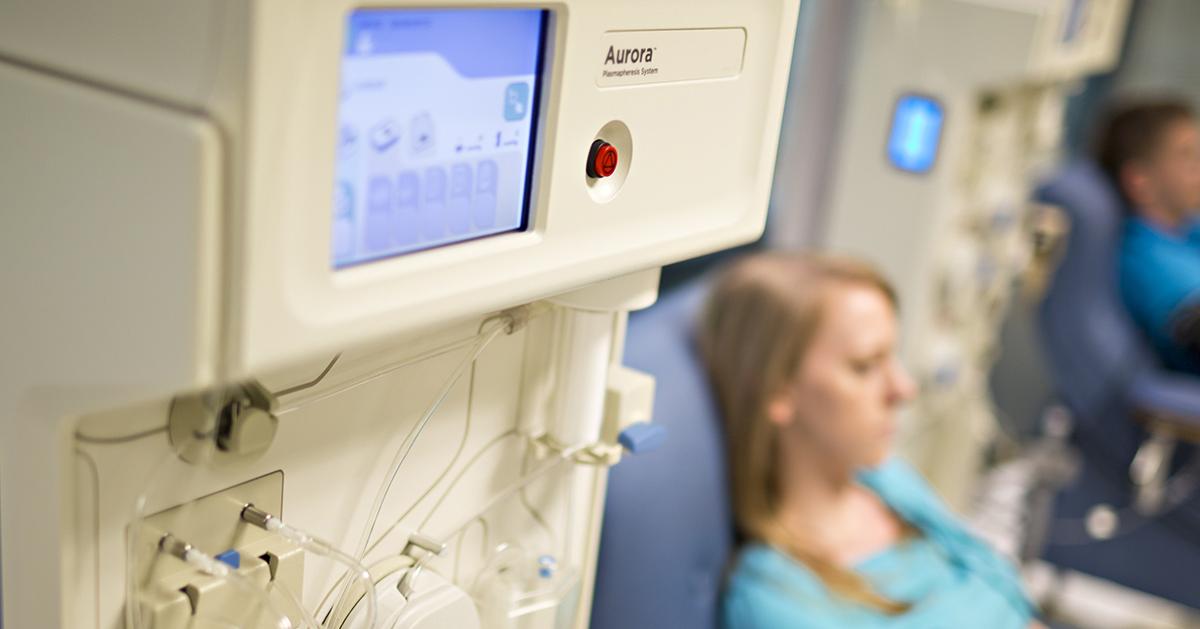
Many patients with von Willebrand disease benefit from the use of replacement therapies. These treatments are given through an intravenous infusion, and they typically consist of specific doses of concentrated blood-clotting factors that contain both von Willebrand factor and factor VIII. Replacement therapies are useful for patients with all types of von Willebrand disease, and hematologists often recommend these treatments both for patients who cannot take desmopressin and for those in whom it has been ineffective. In 2016, a new type of replacement therapy was approved for patients eighteen years old and older. The new therapy is a recombinant form of von Willebrand factor made through genetic engineering. The recombinant production process enables the medication to be produced without the use of plasma, and this can reduce the risk of allergic reactions and viral infections that sometimes occur with older replacement therapies. While receiving an infusion of this new recombinant von Willebrand factor, patients will have their vital signs closely monitored. They should report any side effects, including a fast heart rate, hot flushes, itching, chest pain, muscle twitching, and nausea, to their healthcare team immediately.
Discover additional treatments for von Willebrand disease now.
Pick Exercises Carefully

Doctors encourage patients with von Willebrand disease to pick exercises carefully to reduce the risk of injuries that could lead to excessive bleeding. For example, patients are frequently advised to avoid participation in contact sports such as football, hockey, and wrestling. Similarly, heavy weight lifting is also not advised for von Willebrand disease patients. Safe exercise options include walking, swimming, cycling, and some types of yoga. Individuals who have von Willebrand disease should check with their specialist prior to beginning a new exercise routine. The specialist can advise the patient about the safest types of exercise for their particular needs, and the doctor will also be able to provide advice on safe exercise amounts. Patients may wish to use a personal trainer to help them plan and complete safe, effective workouts. The use of exercise videos can be beneficial as well.
