How To Treat And Prevent Femoral Vein Thrombosis
Femoral vein thrombosis is a condition in which blood clots form in the femoral vein. This vein, which stretches from the groin area down the inside of the leg, is situated close to the surface of the skin and can be very prone to the development of blood clots. Prolonged periods of inactivity, such as recovery from surgery, trauma, or bed rest during pregnancy, can put individuals at a higher risk of femoral vein thrombosis.
A history of cancer, blood clotting disorders, and deep vein thrombosis can also place individuals at greater risk. However, even if someone has developed or is at risk of developing femoral vein thrombosis, there are numerous different steps that can be taken to treat or prevent blood from clotting.
Anticoagulation Therapy

Coagulation is the process in which the blood platelets clot. While this is an important process for staunching blood flow when wounded, regular blood clotting can lead to serious health issues, including femoral vein thrombosis. Anticoagulation therapy involves medication taken orally to block the production of vitamin K and other elements in the bloodstream that lead to clotting. This medication is typically prescribed to individuals at risk for developing blood clots, or those who are trying to reduce the size of already formed clots. Anticoagulation therapy is crucial for patients with or at risk of developing femoral vein thrombosis to keep blood thin and prevent blood clots that can lead to a stroke or heart attack.
Injection Of Medication
While many coagulants are administered orally, femoral vein thrombosis can also be prevented and treated through an injection of medication. Typically, injectable medicine is used to initially thin blood, after which oral medications are introduced to keep blood thin and free of clots. Injectable drugs can be administered either intravenously or under the skin, depending on the specific medication. For severe clots, special intravenous medications called thrombolytics can be administered to break up the clot. Thrombolytics can be given either through the IV or injected directly into the clot itself through a catheter.
Elevate The Legs

One of the best ways to prevent the formation of blood clots from femoral vein thrombosis is to elevate the legs. This is an important preventative step when individuals endure prolonged periods of inactivity or spend a lot of time sitting or on their feet during the day. These circumstances can cause leg swelling and blood to pool in the veins. When this happens regularly, and an individual has other risk factors, it is possible to develop femoral vein thrombosis.
It is important to elevate the legs by keeping them supported with pillows or cushions so they remain about six to twelve inches above the heart. This helps keep the blood circulating throughout the body and moving away from the legs to prevent pooling and clot formation.
Compression Socks

Compression socks are also an important precaution for the development of femoral vein thrombosis. Similar in purpose to elevating the legs, these socks keep the blood circulating to prevent pooling and the formation of blood clots. The tight fabric of the compression socks applies pressure to push the blood up and out of the legs. These socks are typically recommended to be worn following surgery or trauma when a patient will be immobile for a long period. Compression garments can also be worn at a doctor's recommendation by anyone who has risk factors for the development of blood clots, including femoral vein thrombosis.
Interior Vena Cava Filter
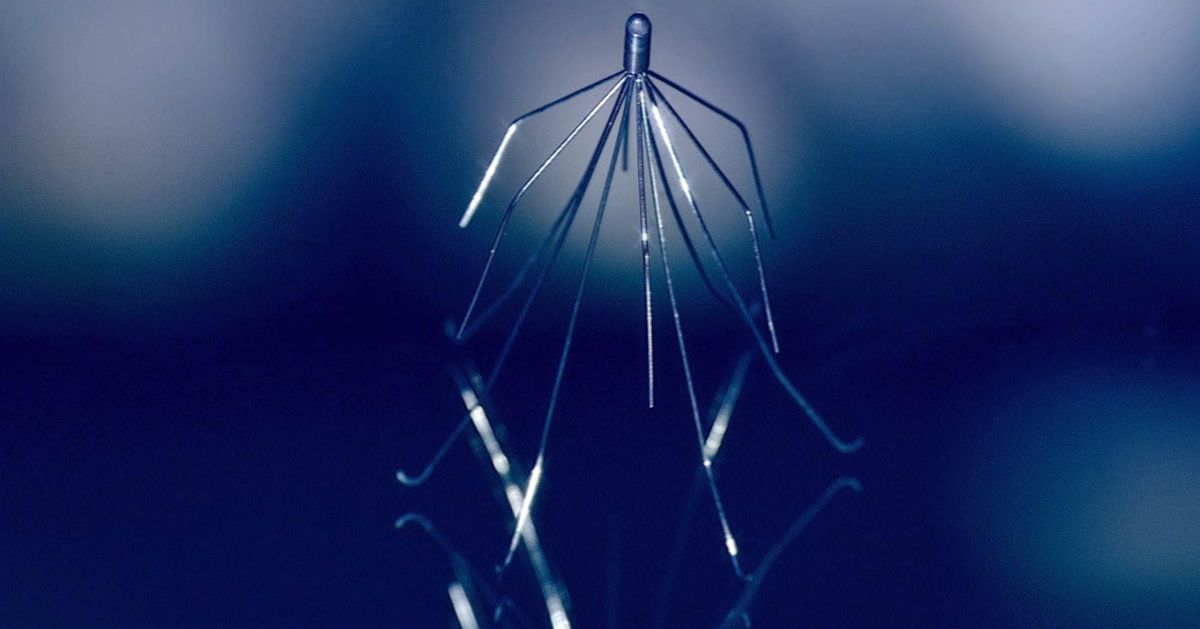
An interior vena cava filter, or IVC filter, is a thin device inserted into the vein. Through a small incision made in either the groin or the neck, a catheter is fed into the vena cava, and the IVC filter is placed. The device then expands and adheres to the walls of the vein, and allows blood to pass through while preventing clots from traveling to the lungs and creating a pulmonary embolism. The IVC filter is typically recommended if an individual has an increased risk of clotting, including those with risk factors for femoral vein thrombosis.
