Treatment Options For Polycythemia Vera
Polycythemia vera is a type of blood cancer in which the patient’s bone marrow makes too many red blood cells. The patient’s blood thus becomes abnormally thick, and circulation slows. This, in turn, can cause complications like blood clots that can lead to a stroke or heart attack. Polycythemia vera is uncommon. It also develops slowly, so a patient can have it for years without knowing it. In many cases, the doctor will diagnose the condition while performing a blood test for some other reason.
While many patients do not show any symptoms, others may develop symptoms such as weight loss, fever, minor bruising or bleeding, fatigue, and itchiness, especially after a warm shower or bath. Polycythemia vera is most common in adults over sixty years old and can be life-threatening if it is left untreated.
Phlebotomy
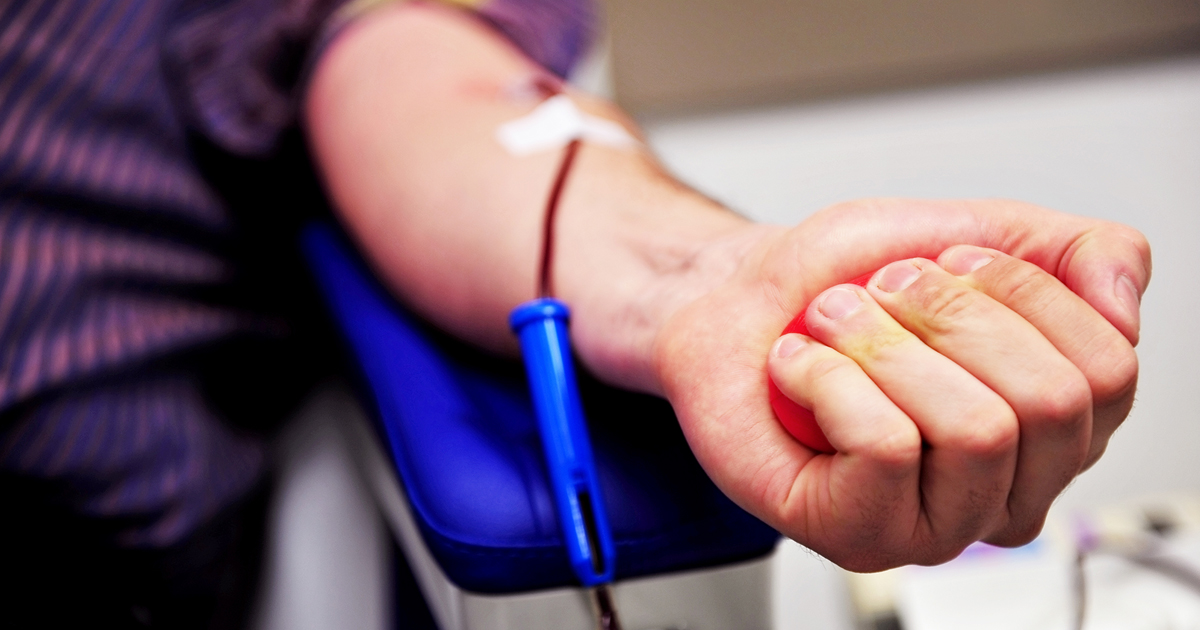
Phlebotomy is usually the first treatment a doctor will try on a patient with polycythemia vera. Also known as 'bloodletting,' it is an ancient practice that dates back centuries. A specialist called a phlebotomist will insert a needle into a vein and draw out the patient’s blood. The process is similar to giving blood, and it can be performed in any clinical setting like a hospital, doctor’s office, or nursing home.
The goal of a phlebotomy is to reduce the number of blood cells and help the blood flow more easily. It can also ease symptoms like dizziness or headaches. The doctor may also draw blood to perform a red blood cell count or another diagnostic test.
Low-Dose Acetylsalicylic Acid
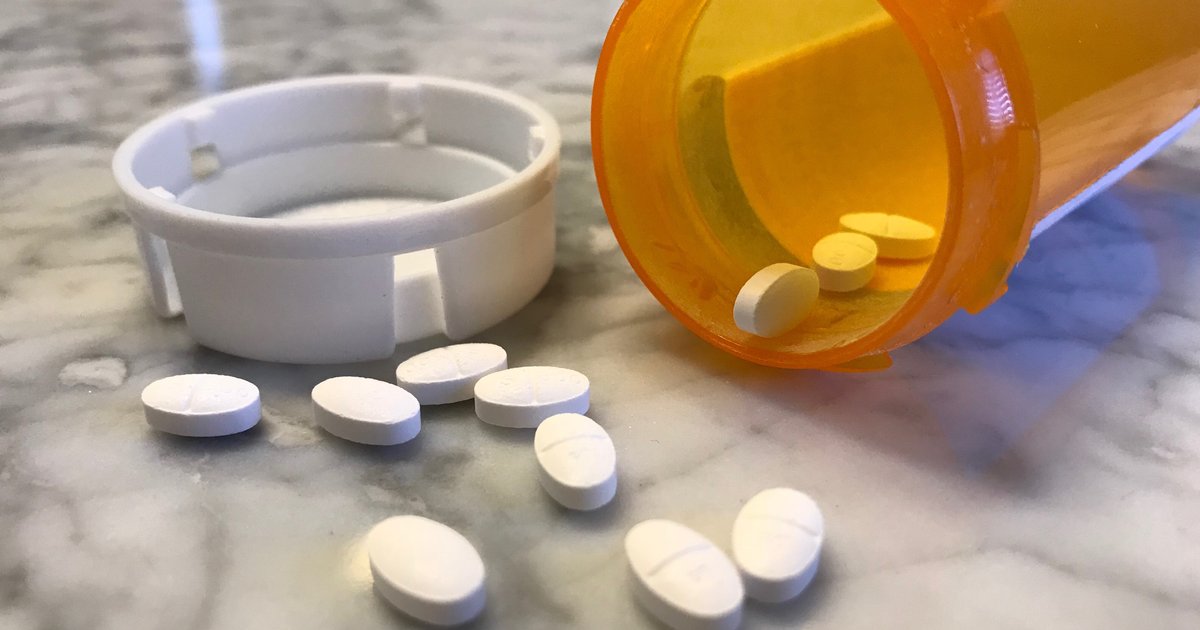
Acetylsalicylic acid (ASA) has long been used to treat fever, inflammation, and pain. It can reduce the risk of blood clots by preventing platelets from sticking together, which is why acetylsalicylic acid is often recommended to individuals who have a high risk of experiencing a stroke or heart attack. Pharmacists make acetylsalicylic acid tablets in standardized sizes. A typical tablet for an adult will be three hundred milligrams, and low-dose acetylsalicylic acid tablets can be seventy-five or eighty-one milligrams. The dosage required will depend on the patient's weight; the heavier a patient is, the higher the dosage they will need.
A doctor treating polycythemia vera will want to regulate the patient’s hematocrit or ratio of red blood cells to total blood cell volume. A woman’s hematocrit should be below .42, and a man’s hematocrit should be under .45. Other medications used to treat polycythemia vera include pegylated interferon, ruxolitinib, and hydroxyurea. The doctor will try acetylsalicylic acid first, however, and then recommend one of the other medications if it doesn’t have the desired results.
Itching Therapy

Polycythemia vera can sometimes cause itching, in which case doctors will recommend itching therapy treatments like ultraviolet light therapy, or they may recommend antihistamines, typically starting with over-the-counter options. Selective serotonin reuptake inhibitors (SSRIs), medications that have often been used to treat depression, can also help relieve itching. Fluoxetine and paroxetine are examples of SSRIs.
Dry skin is particularly susceptible to itching. The patient should, therefore, take steps to keep their skin hydrated. For example, they should not use hot water when bathing or showering, as it will dry out their skin. After bathing, they should pat themselves dry and then apply a moisturizing lotion.
Avoid Extreme Temperatures

The reduced circulation that accompanies polycythemia vera can increase the patient’s vulnerability to injuries caused by temperature extremes. The patient should, therefore, avoid extreme temperatures by always dressing warmly during cold weather, and they should take particular care to protect their hands and feet. In hot weather, the patient should avoid the sun and drink a lot of fluids. The patient should also avoid heated whirlpools and hot tubs.
Patients with polycythemia vera are also quite susceptible to the skin damage caused by ultraviolet rays. They should thus avoid sunlamps and tanning booths, and they should stay out of the sun from 10 a.m. to 4 p.m., which is when the sun’s rays are at their strongest. They should wear long sleeves, a broad-brimmed hat, and protective sunglasses when they are outside. Similarly, they should use a sunscreen of at least a sun protection factor (SPF) of thirty.
Get More Exercise

Exercise like walking can stimulate blood flow and thus decrease the risk of blood clots. It can also help increase the patient’s energy. The patient can also get more exercise by performing exercises while sitting or even lying down. Most of these involve the legs, ankles, and feet, as blood clots are most likely to develop in the lower part of the body. Patients sitting for long periods should generally do five repetitions of each exercise every half an hour, but individuals in high-risk groups should work towards doing ten repetitions of a given exercise.
The leg raise is an example of an exercise that can be done while seated. The patient raises one leg and slowly straightens it. They then slowly return their foot to the floor and repeat the exercise with the other leg. In a variation, they can bring their knee up to their chest, hold it there, and then return their foot to the floor. The thigh stretch is similar to the leg raise, but the patient does it while lying down. In this exercise, the patient lies with their legs straight out. They raise one leg so it is at a right angle to their body. They then gently pull the leg towards their body and hold it for thirty seconds. As with the leg raise, the patient may perform a variation in which they bring their knee to their chest.
