Guide To The Types of Hemophilia
Hemophilia is an inherited condition caused by deficiencies in clotting factors. Patients with the condition experience difficulties with blood clotting, and they might notice unexplained or excessive bleeding. Bleeding after minor injuries is common, and frequent nosebleeds, bleeding gums, and large bruises may develop as well. Some patients have reported joint pain and blood in the urine or stool, and children with hemophilia may display irritability. To diagnose hemophilia, patients may need to have several blood tests such as a complete blood count, an activated partial thromboplastin time test, a prothrombin time test, and a fibrinogen test. Clotting factor tests, also known as factor assays, will be performed as well. Treatment for hemophilia depends on the specific type the patient has, and it involves the replacement of specific clotting factors. Doctors may prescribe fibrin sealants to encourage blood clotting, and patients might also need to take antifibrinolytics such as tranexamic acid or aminocaproic acid to prevent the breakdown of blood clots.
The types of hemophilia are outlined in detail below.
Hemophilia A

Patients with hemophilia A have a defect in a clotting factor known as factor VIII. In some cases, the clotting factor may be missing. The condition is carried on the X chromosome, and it has three main stages: mild, moderate, and severe. Patients are staged according to the ratio of factor VIII protein in their blood. Individuals with a ratio of six to forty-nine percent are classed as mild, and those with a ratio of one to five percent are classified as moderate. In cases where the ratio is less than one percent, individuals are considered to be in the severe stage. Patients with hemophilia A bleed for a longer amount of time than individuals without the condition, and this bleeding can happen both internally and externally. In mild cases of hemophilia A, patients typically bleed for a prolonged period only after a major surgery or serious injury. Individuals in the moderate or severe stages experience more frequent bleeding episodes, and they might bleed spontaneously. Intravenous infusions of concentrated factor VIII product are the main treatment for this type of hemophilia.
Read more about the different types of hemophilia now.
Hemophilia B
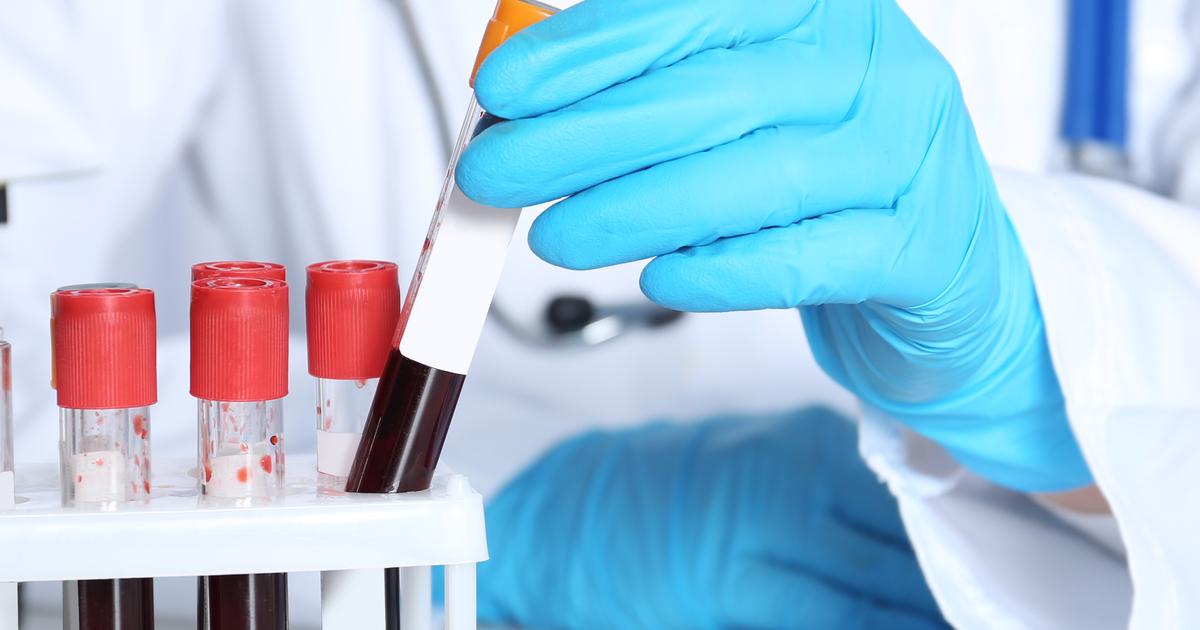
Hemophilia B is carried on the X chromosome, and it involves a defect in (or the absence of) a clotting factor called factor IX. Hemophilia B occurs four times less often than hemophilia A, and the stages and symptoms associated with the condition are the same as those for hemophilia A. Females with hemophilia B could experience very heavy periods, and they may also hemorrhage during childbirth. Treatment for hemophilia B is normally carried out at specialist centers, and patients will need to have clotting time and clotting factor tests to determine the severity of their case. Patients with this condition usually receive concentrated factor IX administered intravenously. Individuals with severe forms of hemophilia B are also placed on prophylaxis treatment so they can maintain enough factor IX to prevent bleeding episodes.
Discover additional types of hemophilia now.
Hemophilia C
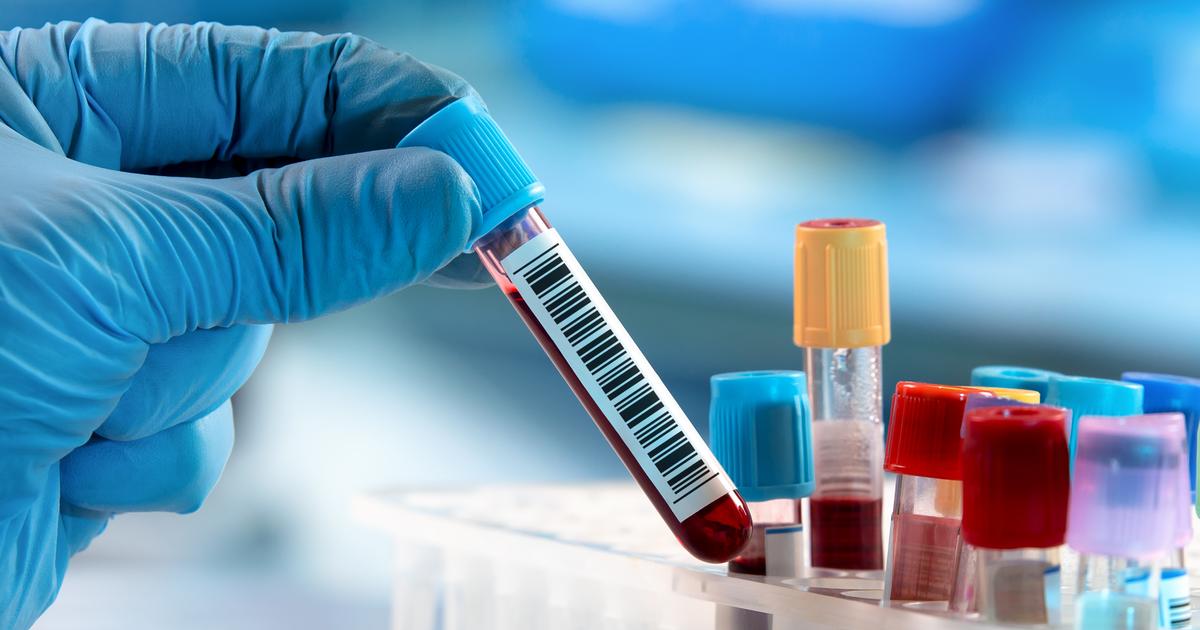
First identified in 1953, hemophilia C is caused by a defective or missing factor XI protein. This type of hemophilia is estimated to occur in one out of every 100,000 individuals in the general population. In Israel, hemophilia C develops in an estimated eight percent of the Ashkenazi population. Both sexes are equally affected by this type of hemophilia. Patients with hemophilia C may experience severe bleeding after oral surgery or tooth extractions, and nosebleeds and soft tissue bleeds are common, too. Unlike other types of hemophilia, the symptoms associated with hemophilia C are not correlated with levels of factor XI. For instance, individuals with lower levels of factor XI might experience less bleeding than those with higher levels. To diagnose hemophilia C, doctors will perform platelet function tests, activated partial thromboplastin time tests, and prothrombin time tests. In the United States, factor XI concentrates are not yet available, so doctors rely on large amounts of fresh frozen plasma as the primary treatment method. This treatment is often combined with fibrin glue, a substance that helps maintain clots after mouth bleeding.
Learn about more types of hemophilia now.
Parahemophilia
Also known as Owren's disease, parahemophilia was first identified in the 1940s. It is characterized by a deficiency in clotting factor V, a protein that speeds up the initial stage of clot formation. Parahemophilia affects both sexes equally, and the prevalence of the condition is approximately one in one million. So far, fewer than two hundred cases of parahemophilia have been reported around the world. Patients with factor V deficiencies typically experience easy bruising and frequent bleeding from the nose, mouth, and gums. In adults with severe parahemophilia, internal bleeding might develop in the lungs and the gastrointestinal tract, and this may become potentially life-threatening. Infants with parahemophilia have an elevated risk of intracranial hemorrhage (bleeding within the brain). To diagnose parahemophilia, doctors carry out a factor V assay test, and tests to measure thrombin clotting time, prothrombin time, and activated partial thromboplastin time may also be performed. Currently, fresh frozen plasma is the only available treatment for parahemophilia, and doctors typically prefer to use solvent-detergent fresh frozen plasma since it contains the most reliable level of factor V. In severe cases that involve acute bleeding, patients might receive platelet concentrates as well.
Get more details about the different types of hemophilia now.
Connection To Other Bleeding Disorders

As a clotting factor deficiency, hemophilia shares a connection to other bleeding disorders. Scientists have currently identified additional bleeding disorders involving deficiencies in clotting factors I, II, VII, X, XII, and XIII. Like hemophilia, all of these conditions are very rare. For example, factor I deficiency is a collective term for three inherited conditions that involve fibrinogen deficiencies. Factor II deficiency is also known as prothrombin deficiency. Patients with factor I deficiency experience prolonged wound healing, and they are at an increased risk of venous blood clots. Individuals with a factor II deficiency often experience severe bleeding after surgery. Both factor I and factor II deficiencies can be treated with fresh frozen plasma, and prothrombin complex concentrates are used to treat factor II deficiencies, too. Tests for most bleeding disorders are the same as those used for hemophilia, and the conditions are all characterized by abnormal or prolonged bleeding. Patients with any kind of bleeding disorder will need regular follow-up appointments with specialists, and they might need to take certain precautions before surgery or dental procedures.
