Guide To Colon Cancer Diagnosis And Treatment Options
Colon cancer is a malignancy that originates in an individual's rectum or colon. An individual's colon and rectum are the last segments food moves through in the digestive tract before it is eliminated from the body. Colon cancer develops as a result of a mutation in cell DNA. Carcinogenesis results from this mutation in the cell, causing it to divide into more cells that grow rapidly, divide constantly, and do not die when they should. An individual affected by colon cancer may experience symptoms such as unexplained weight loss, the sensation of the bowel not emptying completely, blood in the stool, frequent diarrhea, frequent constipation, change in stool shape, weakness, fatigue, and rectal bleeding. Many patients do not have symptoms of colon cancer until it has progressed to an advanced stage. A colon cancer diagnosis is made with the use of a colonoscopy procedure, blood tests, and CT scans.
There are multiple ways in which a patient's colon cancer may be diagnosed and treated. Get familiar with these methods now.
Colonoscopy

A colonoscopy is a procedure used to examine the inside of a patient's large intestine and rectum for abnormalities such as cancerous growths. A colonoscopy is performed with a colonoscope, which is a long, flexible tube equipped with a camera on the end that projects the inside of the rectum and colon onto a screen for the physician to view. When an individual experiences symptoms indicative of colon cancer, like bowel habit changes, rectal bleeding, sensation that the bowel does not empty, unexplained weight loss, weakness, fatigue, and persistent abdominal discomfort, a colonoscopy procedure can be performed to confirm or rule out a colon cancer diagnosis. Individuals over fifty years old are recommended to undergo regular colon cancer screening every decade by having a colonoscopy done if they do not have any other colon cancer risk factors.
Reveal ways to treat colon cancer now.
Polypectomy
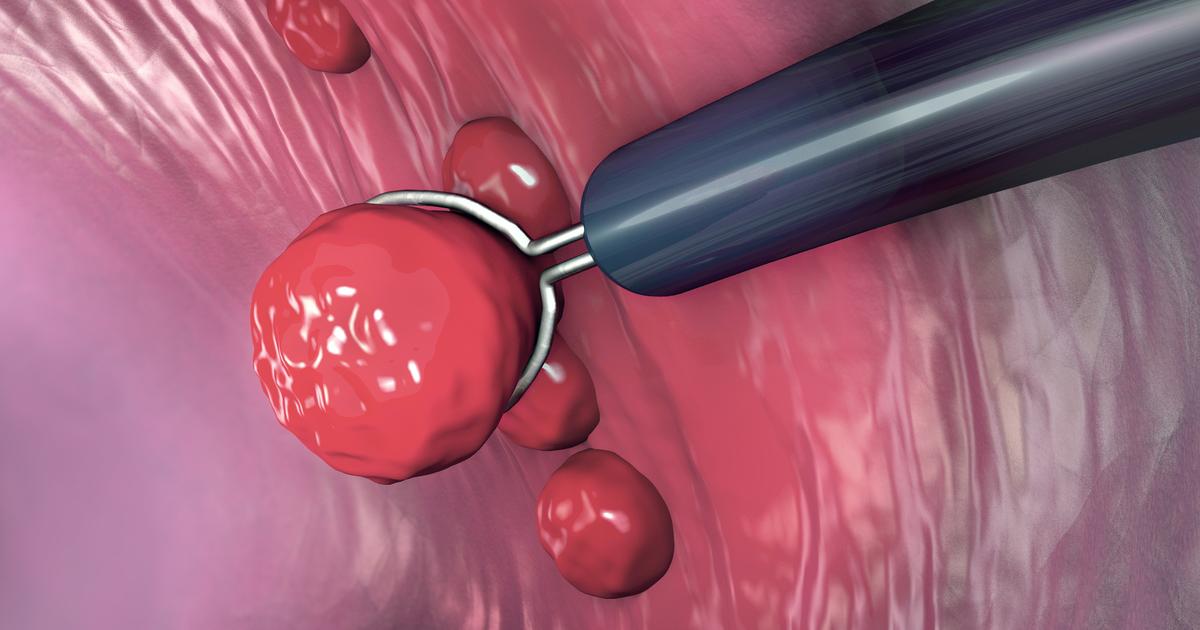
A patient with colon polyps or precancerous growths in their colon may need to undergo a procedure referred to as a polypectomy as part of their treatment plan. This is a procedure involving the excision of a polyp or abnormal tissue growth that contains malignant cells or precancerous cells from an individual's colon. Due to the nature of the procedure, it is often performed at the same time as a colonoscopy, which is a procedure where a surgeon inserts a colonoscope with a light and camera on the end of it into the patient's rectum. The camera transmits real-time video to a monitor the surgeon can use to look for any signs of colon polyps. If concerning polyps are discovered, the surgeon usually chooses to remove them. Depending on the type of polyp found, the surgeon may use a tool with a looped wire to cut the polyp off with heat. The tool can cauterize any leftover tissue or stalk to prevent severe bleeding and expedite the healing process. Most early-stage colon cancers contained within a polyp and have not spread any further are treated using a polypectomy.
Read more about the options used to treat colon cancer now.
Endoscopic Mucosal Resection
If an individual is suspected of having cancerous cells that penetrate the tissues lining their colon, they may need to have a procedure called an endoscopic mucosal resection as part of their treatment plan. Endoscopic mucosal resection is a procedure involving the removal of a larger sized abnormal growth in the colon or large intestine along with a small portion of the inner lining of the colon. During a colonoscopy, the surgeon may discover polyps that are suspected of having cancerous or precancerous cells that are too technically challenging to be removed with a polypectomy. The configuration, large size, and location of a suspicious polyp all can cause the need for endoscopic mucosal resection. During this procedure, the surgeon injects saline fluid into the tissue underlying the polyp to help lift it from the origination point. Piece by piece, the polyp is then manually removed. When the origination point of the polyp is reached in the colon lining, a healthy part of the lining is removed as well to ensure all cancerous or precancerous cells are eliminated with the challenging polyp.
Keep reading to reveal more colon cancer treatments now.
Partial Colectomy
A partial colectomy may be necessary to treat a case of colon cancer that has spread into or through the colon. This is a surgical procedure involving the complete excision of part of the colon or large intestine. During a partial colectomy, the surgeon cuts out the region of the colon affected by cancer. Most cases of colon cancer in patients who undergo a partial colectomy do not require additional procedures to make a route for wastes to exit the body. The surgeon is typically able to reattach both ends of the healthy colon or rectum. However, this cannot be done for all individuals who need a partial colectomy to treat their colon malignancy. In such cases, a stoma or an opening in the patient's abdominal wall must be made for waste to be able to exit their body. A special bag is placed over the stoma to collect the waste for disposal. Some patients will have to use a stoma and stoma bag permanently, while others may only need it temporarily during the healing process. If the stoma is temporary, the patient will need to undergo a second procedure to reconnect their rectum to their large intestine.
Discover additional ways to treat colon cancer now.
Radiation Therapy
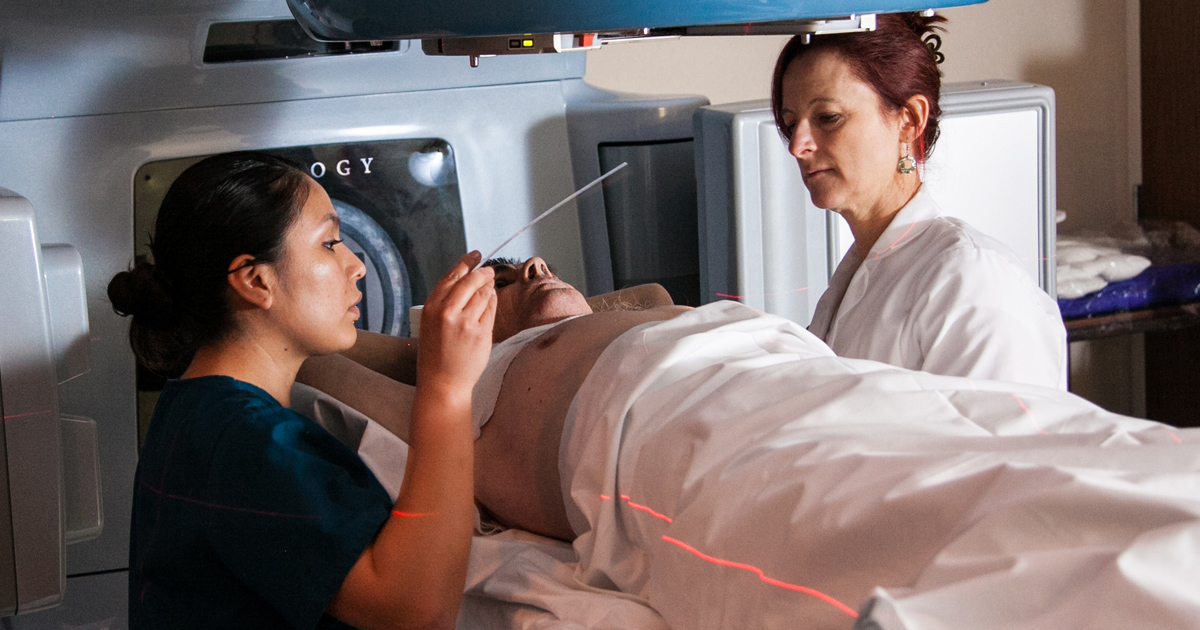
Radiation therapy with or without a surgical procedure may be needed as part of treatment to eliminate all cancerous cells in a colon cancer patient. Radiation therapy is used more often in patients who have cancer that affects their rectum before or following the surgical removal of the tumor. This type of treatment is also used in cases where a patient's colon or rectum malignancy is inoperable, and may or may not be used in combination with chemotherapy. Radiation therapy is a noninvasive procedure where cancer cells are eliminated through the use of high energy x-ray beams. Radiation therapy works by aiming these energy beams at the cancerous cells so the beams cause mutations, partial destruction, or complete destruction of the DNA within the cancerous cells. This process can cause the cells to die immediately, die at a later time, be unable to grow, and or be unable to divide. Radiation for colorectal cancer is typically given five days a week on an outpatient basis for between five and six weeks. For palliative purposes or where symptoms are only being treated, the frequency and duration of radiation therapy sessions may vary.
Keep reading to uncover more options for effectively treating colon cancer now.
Chemotherapy
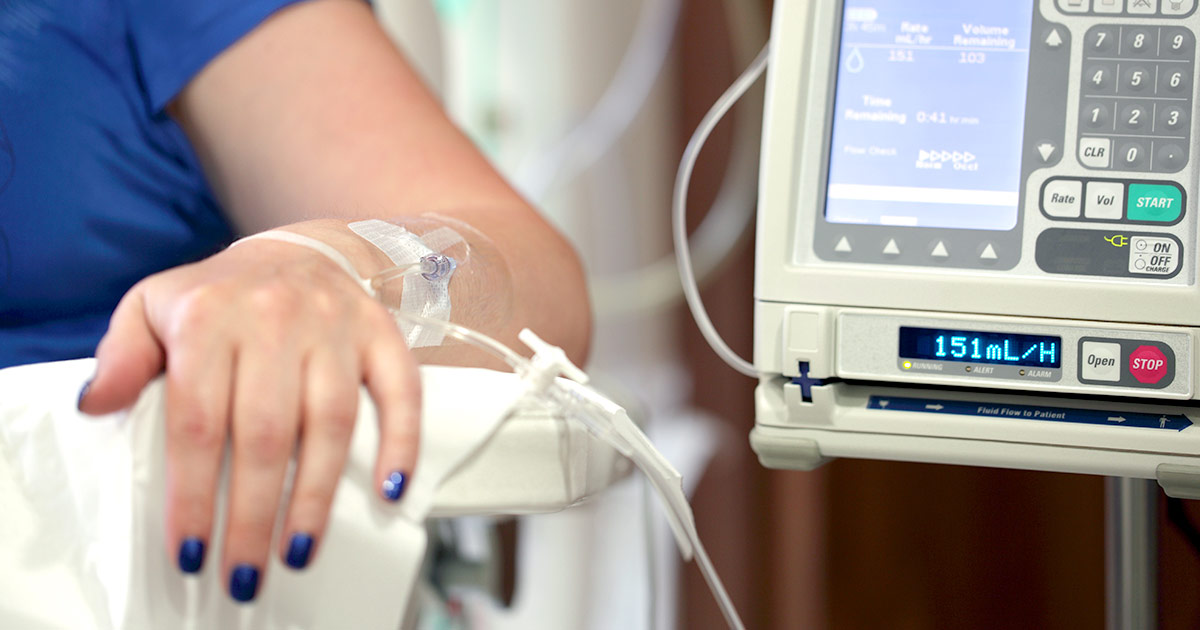
A colon cancer patient may need to undergo chemotherapy independently or in addition to a surgical procedure to ensure all cancerous cells are eliminated from the body. Chemotherapy can be given as a systemic treatment or a regional treatment in individuals affected by colon cancer. Systemic chemotherapy describes a process where chemotherapy drugs are intravenously delivered into a vein so they reach all parts of the patient's body. Regional chemotherapy describes a process where chemotherapy drugs are injected directly into a specific artery that only carries blood to the part of the body where the cancer is located.
Chemotherapy drugs work by killing or damaging all cells in the process of dividing. However, side effects are more significant with chemotherapy because the chemotherapy drugs cannot distinguish healthy dividing cells from malignant dividing cells. Neoadjuvant chemotherapy is chemotherapy administered before a patient has surgery to help shrink the tumor so it is easier to excise. Adjuvant chemotherapy is given following a patient's tumor removal surgery to kill off any malignant cells left behind from surgery or those that migrated to another part of the body.
Uncover information on more ways to treat colon cancer now.
Immunotherapy

An individual who has been diagnosed with colon cancer may need to undergo immunotherapy, a treatment that uses drugs to manipulate the affected individual's immune system into fighting off the cancerous cells. The cells in the patient's immune system may not be able to recognize colon cancer cells because they make certain proteins that allow them to blend in with other cells in the body. Immunotherapy is a treatment method that causes disruptions in this disguise process, making the colon cancer cells more recognizable to the immune system cells. Some of the most common forms of immunotherapy used to treat colon cancer include immune checkpoint inhibitors, PD-1 inhibitors, and CTLA-4 inhibitors. Immunotherapy is a form of colon cancer treatment that is usually only given to individuals affected by an advanced form of this disease.
Continue reading to learn more about treating colon cancer now.
Targeted Drug Therapy

An individual who has developed colon cancer may need to receive targeted drug therapy to treat their malignancy. Targeted drug therapy is treatment with drugs that target specific abnormal properties of tumor cells to kill them. By disrupting the process that allows these abnormalities to exist in the cancer cells, targeted drug therapy can stop cancer from growing. In most cases, targeted drug therapy is combined with chemotherapy to treat colon cancer. One of the most popular targeted drug therapies used for the treatment of colon cancer are drugs that target the formation of blood vessels or vascular endothelial growth factor, which disable this protein from working. The drugs that use this mechanism are bevacizumab, Ziv-aflibercept, and ramucirumab. Another protein that can be targeted with drugs such as cetuximab and panitumumab to treat colon cancer is the epidermal growth factor receptor.
Get more details on how to treat colon cancer now.
Bowel Resection
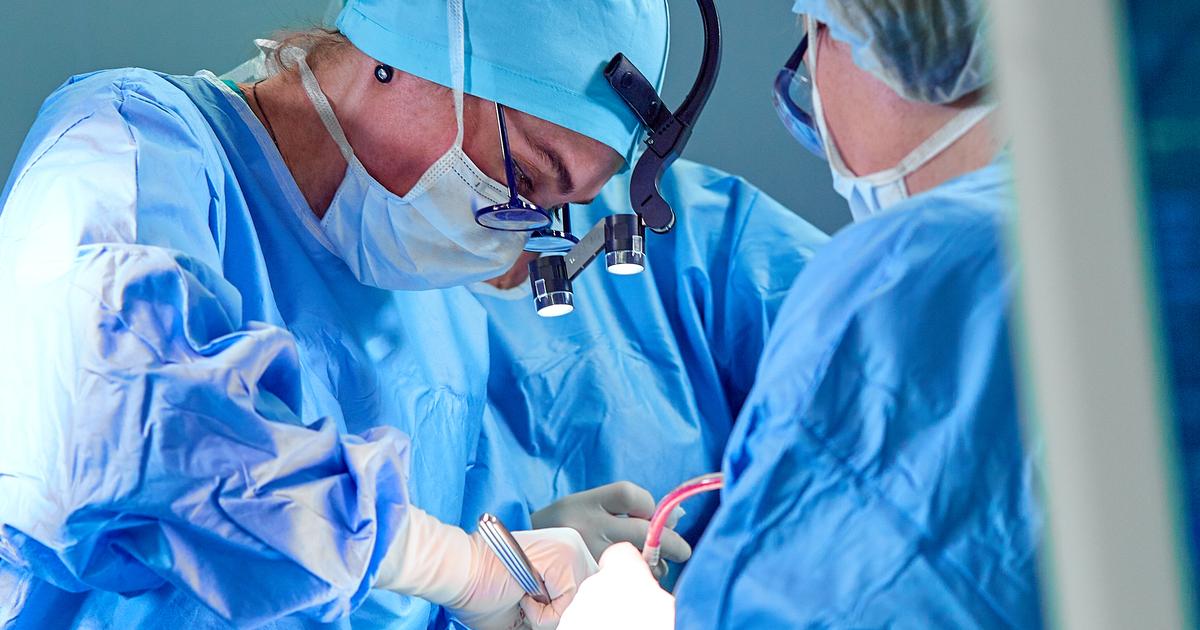
Colon cancer patients may need to undergo a surgical operation referred to as bowel resection. The term resection is used to describe any procedure involving the removal of tissues or parts of an organ. This procedure focuses on the removal of the cancerous tumor from the large intestine. The part of the large intestine that contains the cancerous growth is removed as well as any surrounding lymph nodes that have been affected by cancer. Once the diseased section of the large intestine has been removed, the healthy portions of the large intestine are sewn together. A bowel resection to treat colon cancer can be performed as an open resection where a large incision is made in the patient's abdomen, or it can be done by laparoscopy or through a small incision using specialized scope and instruments.
Read more about treating colon cancer effectively now.
Radiofrequency Ablation

Colon cancer patients often need radiofrequency ablation to treat their cancerous tumor. Radiofrequency ablation is a method where high-energy radio waves are used to destroy tumor cells. Radiofrequency ablation is performed by using an ultrasound or CT scan on a patient to help the surgeon guide a thin probe through the skin and to the malignant tumor. Once the probe is in place, high-frequency radio waves are carried by an electric current to the tip of the probe in the patient's tumor. When the radio waves reach the tumor tissues, it causes damage to the small blood vessels that feed the growing tumor cells. Without blood flow, the tumor tissues experience what is known as coagulative necrosis, or cellular death from lack of blood supply. Radiofrequency ablation is commonly used in conjunction with surgery to treat colon cancer to destroy areas of the tumor that may have spread to other organs and tissues not removed during surgery.
