Guide To Pancreatic Cancer Tests
Pancreatic cancer initially develops in the cells that make up the pancreas, or the organ responsible for the production of digestive enzymes and secretion of blood sugar managing hormones. Because of its obscure location in the body, tumors in the pancreas are hard to detect in early stages. Routine screening for pancreatic cancer is only recommended at this time for individuals considered high risk. Numerous diagnostic tests can be performed on a patient who has symptoms indicative of pancreatic cancer to determine if it is the underlying cause. When pancreatic cancer is identified, more advanced tests can be used to determine the exact location, severity, extent, and prognosis of the cancer. Because pancreatic cancer is known to spread easily, many diagnostic tests are not only focused on the abdominal area where an individual's pancreas is located but the rest of the body as well.
Blood Tests
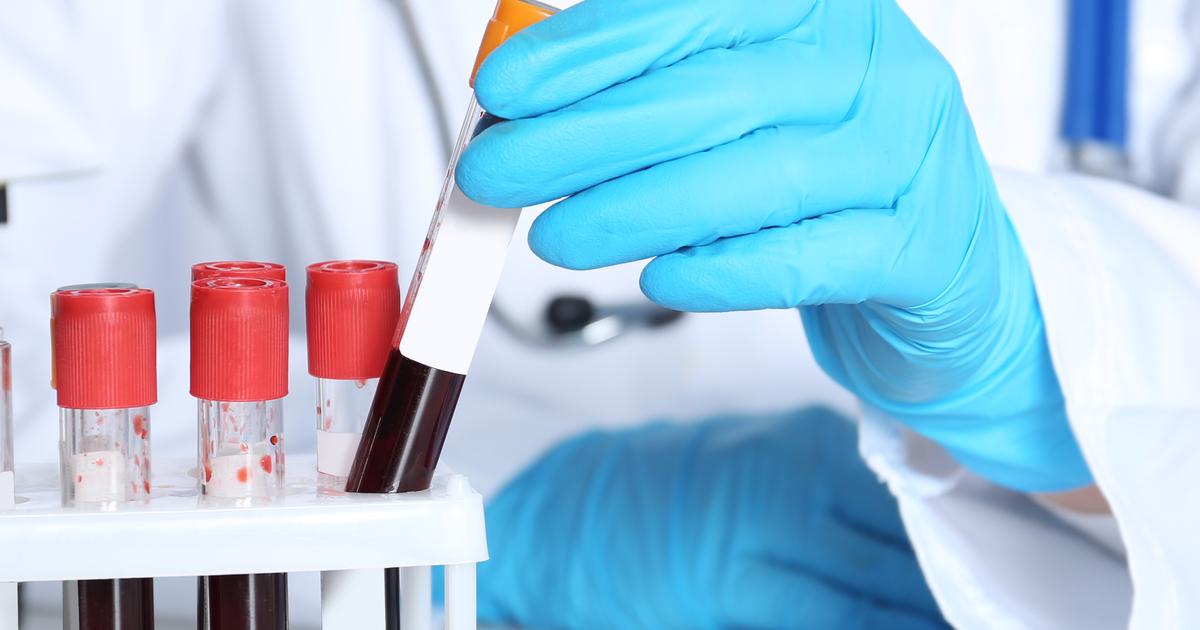
When a patient is suspected to have pancreatic cancer, their physician may be able to use blood tests to aid in making a diagnosis. A metabolic panel that includes bilirubin levels can be run on a patient's blood to check for elevated amounts of bilirubin in circulation. A tumor that begins in the pancreas can wrap around the organ and around the ducts that come from the organ, resulting in a duct obstruction. When these ducts become obstructed, bilirubin and other substances intended to drain into the small intestine begin to build up and enter circulation instead of into the intestine. Other blood tests can check for the presence of certain substances produced at higher levels by malignant tumors referred to as tumor markers. Some individuals with pancreatic cancer will have a high level of a tumor marker called carbohydrate antigen 19-9 or CA-19-9. Imbalances of certain hormones, markers of inflammation, and high blood sugar may also be detected in the blood of some patients as a result of their pancreatic cancer.
Positron Emission Tomography Scan

Positron emission tomography (PET) scans are a type of diagnostic imaging test that can reveal patterns in the way a patient's body is using energy. A PET scan is a unique diagnostic test because it shows cellular changes other tests do not. All cells in the body require glucose to carry out their functions. When cells are growing, they require a larger amount of glucose and use it up faster than healthy cells. Cancerous cells are cells in the body that grow and multiply at an uncontrollable rate, using larger quantities of glucose than healthy cells. During a PET scan, the patient is injected with a radioactive tracer or sugar substance. This substance is taken up by the cells in the body using the most glucose, which would be the pancreatic cancer cells if they are present. The PET machine is then able to form a picture that shows where the cells that have taken up the glucose are. PET scans are often used in combination with other diagnostic imaging tests like CT scans to stage pancreatic cancer and evaluate the efficacy of treatment.
Endoscopic Ultrasound
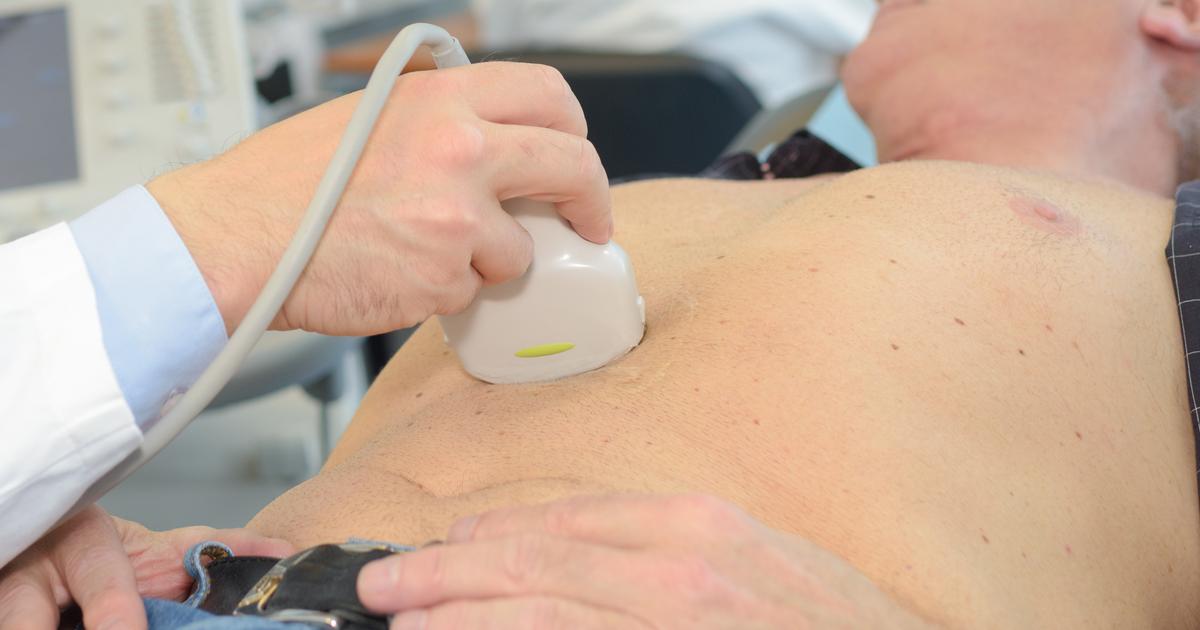
Endoscopic ultrasound is a type of diagnostic imaging test that utilizes a small device that sends sound waves through the body to create an image of the organs by absorbing the deflection of sound waves off internal organs. Transabdominal ultrasound operates with a wand used on the surface of an individual's skin, where an endoscopic ultrasound uses a smaller tube with a light on it and passes it down the individual's esophagus, through their stomach, and into their small intestine. The ultrasound tube is manipulated around in this region to take pictures of the shape and condition of the pancreas. Endoscopic ultrasound is performed by a gastroenterologist while the patient is under sedation. The gastroenterologist may decide to perform a biopsy of pancreatic tissue and other nearby tissue during the endoscopic ultrasound for better diagnostic clarity. Endoscopic ultrasound is helpful in cases where CT scans and other imaging methods are unable to provide a clear visual of the pancreatic cancer.
Pancreatic Protocol CT Scan
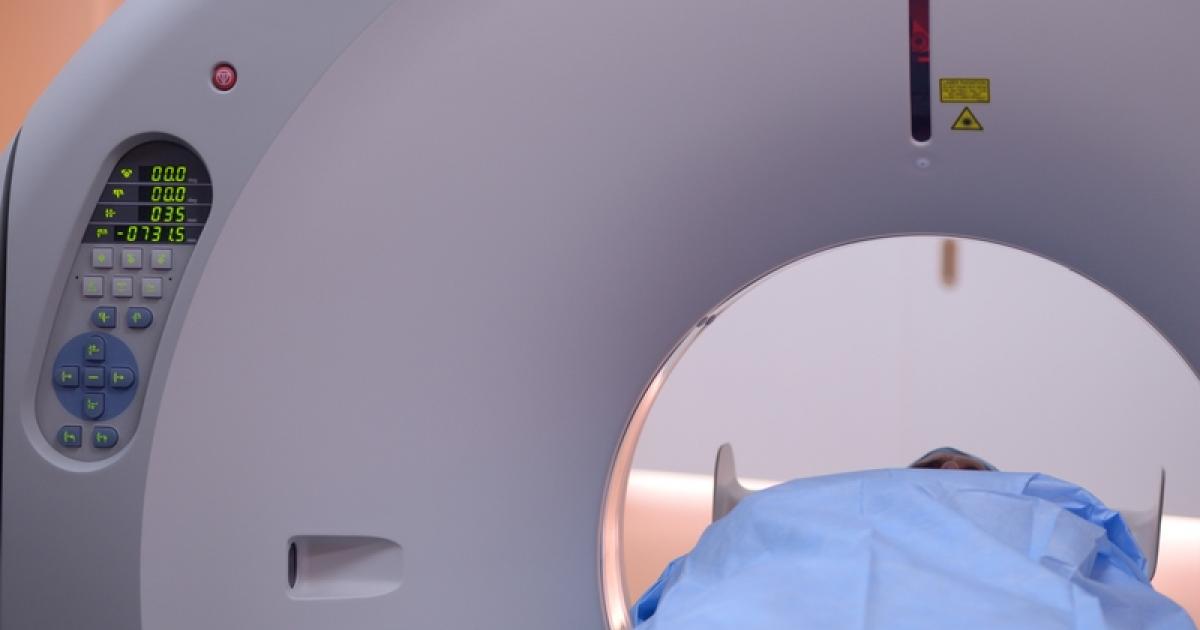
A pancreatic protocol CT scan is a combination of a common diagnostic imaging procedure and a specialized contrast medium administration technique to produce a well-defined representation of a patient's pancreas and surrounding structures. A computed tomography (CT) scan is a machine that takes x-ray images of the interior structures of a patient's body and then utilizes an advanced computer to layer and compound such images into a high-quality three-dimensional representation that can better reveal any odd growths or other abnormalities in the organs. A contrast medium or specialized dye is injected into the patient's circulation to provide better clarity of where the tumor is located relative to the neighboring blood vessels and other organs. When using the pancreatic protocol, the CT scans are taken at specific times during and after the intravenous administration of the contrast medium to make it easier to see abnormalities in the structure, function, and blood flow in the pancreatic structures of pancreatic cancer patients.
MR Cholangiopancreatography
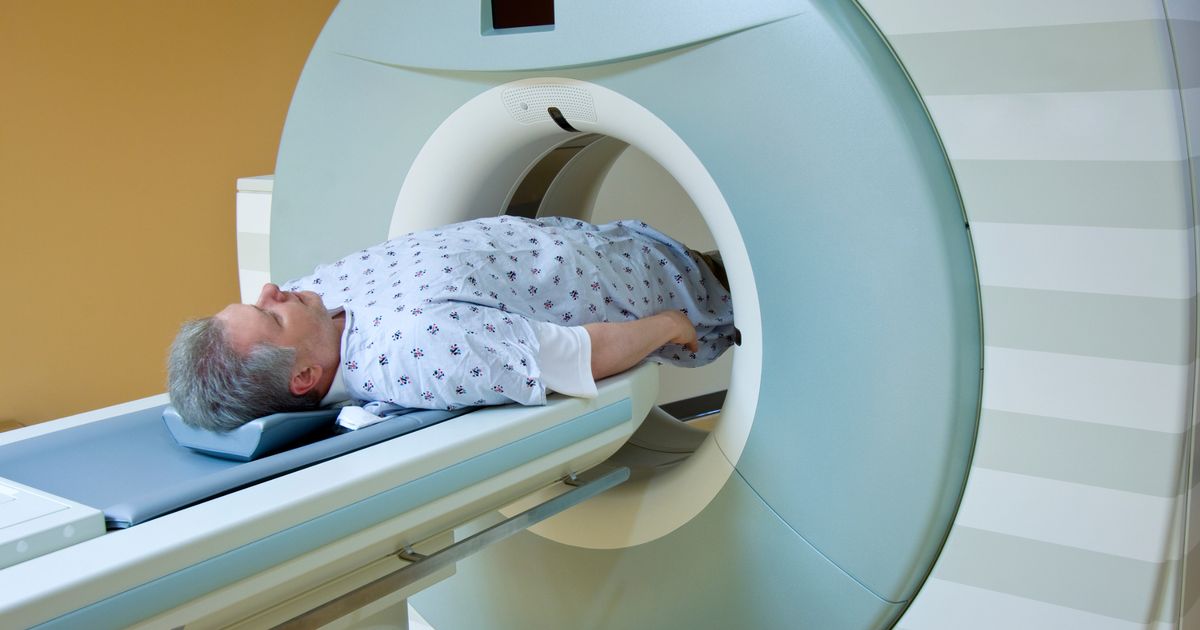
MR Cholangiopancreatography (MRCP) refers to a diagnostic imaging technique to see a patient's pancreatic duct and bile ducts. MRCP is a form of MRI or imaging method where a machine uses a potent magnetic field, a computer, and radio waves in combination to produce detailed images of internal body structures. Unlike other imaging techniques, MRCP does not use x-ray technology and does not produce any harmful changes in an individual's cells. However, because a powerful magnetic field is used, any metal objects on or inside of the body can cause problems with the machinery and may harm the patient by causing burns or becoming projectiles in the MRI room. Intravenous contrast may or may not be used during an MRCP. An MRCP is a better quality imaging test for cancers of the soft tissues in the body because it is a noninvasive way to obtain the same quality and detail as an endoscopic retrograde cholangiopancreatography (ERCP).
