Rare Forms Of Cancer To Be Aware Of
Cancer has directly or indirectly affected us all; whether we are cancer survivors, are undergoing treatment at this moment, know a loved one who has suffered from cancer, or know someone who has lost the battle against it. We all know the major types of cancers and their ribbon colors: pink for breast, white for lung, and blue for colon, as organizations and advocates strive to always make the public aware of these types and many others. But what about rare forms of cancers you may not be aware of or that barely get any attention? Considering our bodies are made up entirely of cells and tissues, an individual can develop cancer anywhere on the body.
The Silent Killer: Mesothelioma
Mesothelioma is a rare, aggressive form of cancer that develops from the thin layer of tissues covering many of the internal organs. The most common area for this cancer to affect is the lining of the lungs, chest wall, and sometimes the abdomen. It rarely affects the sac surrounding the heart known as the pericardium, and the sac surrounding the testis known as the tunica vaginalis. Typical symptoms a patient may experience include shortness of breath due to fluids surrounding the lungs, a swollen abdomen, fatigue, noticeable weight loss, and pain within the chest wall. These symptoms often develop slowly over time.
The main cause of Mesothelioma is exposure to asbestos, with more than eighty percent of known cases being caused by this. It can take an individual who worked with or was exposed to asbestos approximately forty years to develop the disease. Other risk factors for this deadly form of cancer include genetics and infection with the simian virus 40 (a DNA virus). Research indicates by 2015, 60,800 individuals had been diagnosed and 32,000 have died from the condition. Rates vary around the globe, as there are higher rates in Australia and the United Kingdom, with lower rates in Japan. It occurs in approximately 3,000 Americans every year, and it affects more males than females.
Diagnosis And Treatments For Mesothelioma
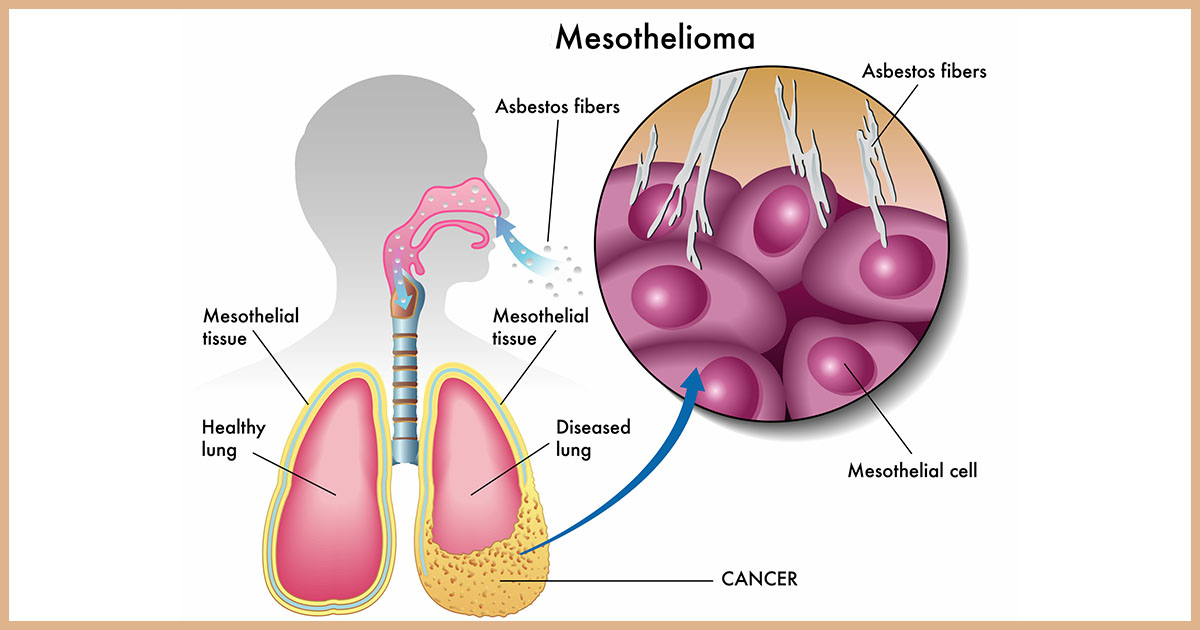
Diagnosis typically occurs for patients after the age of sixty-five, with only a life expectancy of five years or less, as most deaths occur at approximately seventy years of age. On average, only eight percent of Americans will survive past five years following the diagnosis. A diagnosis often occurs with a chest X-ray and CT scan and is either confirmed by examining fluid produced by this cancer or by a tissue biopsy of this cancer.
Prevention of this illness focuses on reducing the exposure to asbestos for those who already have the disease and for those who are prone to developing it. Treatment often includes the traditional methods for treating cancer, such as chemotherapy, radiation therapy, and surgery to remove infected tissue. A procedure known as pleurodesis, which involves using specific substances such as talc to fuse together the pleura (the sac surrounding the lung) to prevent the buildup of fluid around the lungs, can also be used. Chemotherapy can also include cancer destroying medications, such as cisplatin and pemetrexed.
The Skin Condition To Look Out For: Merkel Cell Carcinoma
Merkel cell carcinoma is an incredibly rare form of skin cancer that typically appears as a flesh-colored or bluish-red nodule on the face, head, or neck. The condition is also known as neuroendocrine carcinoma of the skin. This rare skin cancer often develops in older people, especially white males over fifty years old, and is usually caused by long-term sun exposure or weak immune system due to autoimmune diseases and medications. This critical disease tends to grow and spread quite rapidly to other parts of the body, and it is not clear what causes this rare type of cancer.
Researchers do know that cancer begins in the Merkel cells, which are found at the base of the outermost layer of the skin (the epidermis), which are connected to the nerve endings responsible for the sense of touch. Researchers recently discovered a common virus plays a significant role in causing most of the cases of Merkel cell carcinoma, as the virus, Merkel cell polyomavirus lives on the skin and does not show any visible signs or symptoms. How the virus that causes cancer is still unknown, and since the virus is quite common but the development of this form of cancer is rare, it is likely other risk factors play an important role in the development of this particular skin cancer.
Prevention And Treatment For Merkel Cell Carcinoma

Treatment for Merkel cell carcinoma usually depends on if it has spread beyond the skin to other areas of the body, internally and externally. There are a number of risky behavior that can increase an individual’s chance of developing it. Risk factors include excessive exposure to natural and artificial sunlight, a weakened immune system, a history of other types of skin cancer, older age, and lighter skin color. Despite the risks, there are a few preventative measures individuals can take to minimize their risk. Prevention includes avoiding the sun during peak hours, usually between 11:00 AM until 4:00 PM; shielding eyes and skin from the sun with clothes and sunglasses; and applying sunscreen with a high sun protection factor (SPF) liberally and often. Individuals should also monitor changes in their skin’s appearance and notify a doctor about them.
Treatment for this cancer includes a wide local excision to remove a large area of the affected tissue, a lymph node dissection, as well as radiation therapy after surgery. Even with treatment, Merkel cell carcinoma usually spreads beyond the skin and forms tumors within the body, especially affecting nearby lymph nodes. It can also spread to the brain, bones, liver or lungs. Cancers that spread to other organs, such as this type, are more challenging to treat and can be fatal.
Small Blue Round Cell Tumors

The name might sound non-threatening or even a type to scoff at. However, small-blue-round-cell-tumor, also known as SBRCT, is any one of a group of malignant, and often fatal, neoplasms that appear under a microscope. For instance, this disease consists of small round cells that stain blue on routine Hematoxylin & Eosin stain (H&E) sections, a principle stain in histology. These tumors, unfortunately, develop more often in children than in adults, and they usually represent undifferentiated cells. The significance of the blue staining represents the cells found in the nucleus, where cancer can be detected.
Small blue round cell tumors often lead to Desmoplastic small round cell tumors, which can lead to a multitude of cancers including Neuroblastoma, Mesothelioma, Small cell lung cancer, Wilms’ tumor, Merkel cell carcinoma, and Small-cell lymphoma. Although a majority of these rare types of cancer happen to adults, they can occur in children if small blue round cell tumors occur, due to the primitive cells found in childhood.
The Deadly Desmoplastic Small Round Cell Tumor
This aggressive and rare form of cancer predominantly occurs in the abdomen and can affect other areas of the body including the lining of the abdomen, lymph nodes, diaphragm, spleen, liver, and chest wall. It also affects the skull, spinal cord, brain, large and small intestines, bladder, lungs, testicles, ovaries, and the pelvis. This type of tumor is categorized as a soft tissue sarcoma and is considered a childhood cancer that usually affects boys and young male adults, as the disease rarely occurs in females. There are no known causes of the disease, and it is often misdiagnosed as other forms of tumors within the abdomen due to its rarity. Symptoms include abdominal masses that can grow to enormous sizes and are often hard and round, abdominal distention, abdominal or back pain, gastrointestinal obstruction, lack of appetite, ascites, anemia, cachexia, and masses appearing in other areas of the body.
Similar to small blue round cell tumors, Desmoplastic small round cell tumors can be treated at a sarcoma center due to how rapidly this type of cancer spreads, and there is no standard treatment protocol. Recent research has indicated patients have responded well to chemotherapy, surgery to remove the tumor, and radiation therapy following surgery.
Childhood Kidney Disease: Wilms’ Tumor
Wilms’ Tumor, also formally known as Nephroblastoma, is one of the rarest types of kidney cancer that predominantly affects children. Despite its rarity, it is the most common type of kidney cancer in children. This cancer primarily affects children around the ages of three and four, and it becomes less common after age five.
The illness affects approximately one person for every ten thousand individuals worldwide before the age of fifteen, and patients of African descent have slightly higher rates for developing the disease. Wilms’ tumor usually occurs in one kidney but can occur in both as well. There are approximately five-hundred diagnosed cases in the United States every year, but thankfully, the disease is highly responsive to treatment, with ninety percent of patients surviving at least five years. Common symptoms of Wilms’ tumor include abdominal pain, loss of appetite, fever, nausea, and vomiting, possible blood in the urine, high blood pressure, and a painless, palpable abdominal mass.
Diagnosing, Staging, And Treating Wilms’ Tumor

The first stage in diagnosing Wilms’ tumor is the patient will have a painless abdominal tumor that can be felt by a doctor, which can be confirmed with an ultrasound scan, computed tomography scan, or MRI scan. A tumor biopsy is typically not done as it poses a risk of creating fragments of cancer tissue and planting malignant cells within the abdomen. Next is staging, which is the standard way to describe the extent of the spread of the tumor, and to determine prognosis and treatments. Stage One is the most common form, as it affects forty-three percent of all cases, and is the easiest stage to treat. Stage Two affects twenty-three percent, Stage Three affects twenty percent, Stage Four affects ten percent, and Stage Five affects five percent of all known cases.
Treatment options for children suffering from Wilms’ tumor include surgery to remove the infected kidney, as early removal tends to promote positive outcomes. Chemotherapy and radiation therapy are usually only used if the tumor is deemed a Stage Five tumor, as early stages only require surgery, as well as lymph node sampling to ensure cancer has not spread and has been effectively removed.
The Frightening Truth About Chordoma

Chordoma is a form of bone cancer found in the skull and spine and is only diagnosed in one in a million individuals per year. Chordoma tumors affect approximately three-hundred Americans, and seven-hundred Europeans per year, with the average age being those in their fifties and sixties, however, it can affect anyone at any age. This extraordinarily rare cancer grows from minuscule remnants of cartilage left behind from when the patient was in utero, and experts have indicated it is not caused by genetics. Chordoma is part of a group of malignant bone and soft tissue tumors known as sarcomas. Chordoma grows quite slowly but aggressively, which often leads to headaches, neck pain, double vision, loss of bowel and bladder function, and a tingling sensation in the arms and legs.
This condition accounts for approximately three percent of all bone tumors and twenty percent of primary spinal tumors. Despite its rarity, Chordoma is the most common type of tumor that affects the sacrum and cervical spine.
How To Treat Chordoma Tumors

Chordomas are a unique and complex tumor, making treating them difficult due to the involvement of critical structures within the body, including the brainstem, spinal cord, and important nerves and arteries. Chordoma tumors often reoccur after treatment, usually in the same location, which is called local recurrence. In about thirty to forty percent of patients, the tumor will eventually spread or metastasize, to other parts of the body, making this form of cancer incredibly dangerous to develop.
These specific forms of tumors do not respond well to chemotherapy, radiation, or medications in general and the best option for patients is surgery. Surgery is the primary way to remove the tumor. However, it is a difficult procedure due to the tumor growing on the spine and around vital nerves, meaning surgeons can often only remove parts of the chordoma tumor, but not all of it, hence why there is a chance of recurrence.
