Guide To The Symptoms Of Cowden Syndrome
Cowden syndrome is a genetic condition where an individual develops numerous hamartomas or noncancerous growths on multiple parts of their body and are at an increased risk for certain types of cancer. Cowden syndrome is the result of one or more PTEN tumor suppressor gene mutations in most cases. Mutations in genes that supply the code for producing certain proteins result in the formation of the hamartomas and higher vulnerability to certain cancers in Cowden syndrome.
One or more mutations in the KLLN, SDHC, PIK3CA, SDHB, SDHD, and AKT1 genes can also cause Cowden syndrome. Cowden syndrome is diagnosed with clinical criterion or genetic testing that reveals a positive result for any of the gene mutations known to cause Cowden syndrome. Treatment for Cowden syndrome focuses on diligent, thorough cancer screening and management of any symptoms benign tumors may cause.
Skin Lesions And Spots
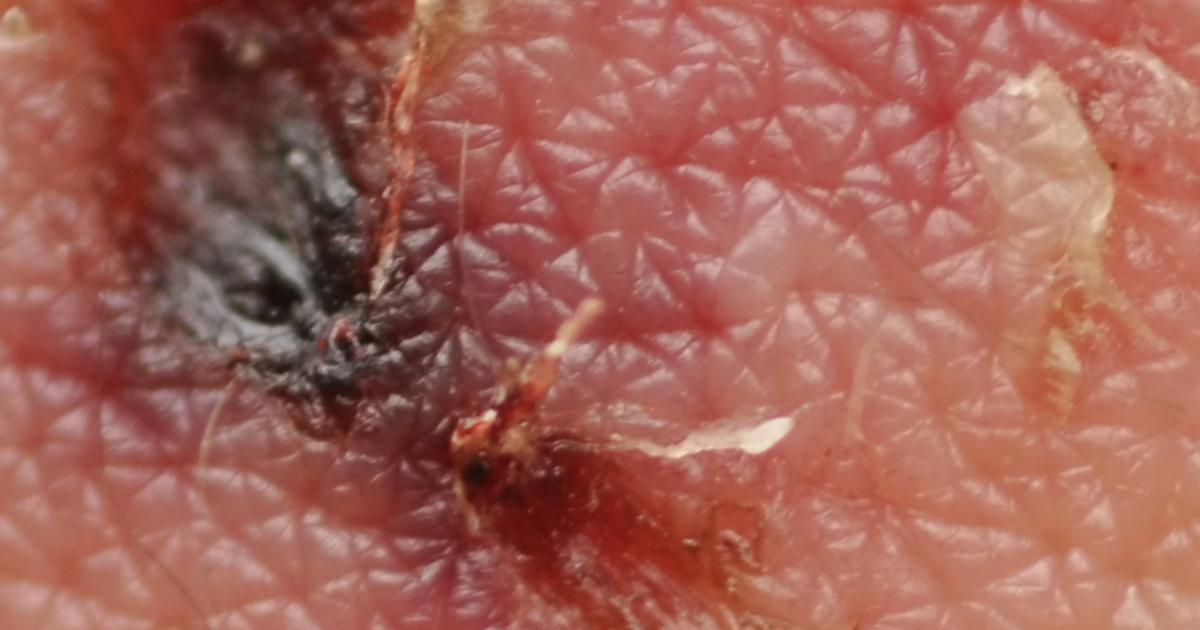
An individual affected by Cowden Syndrome may develop skin lesions and spots. Between ninety and one hundred percent of all Cowden syndrome cases have involvement in the individual's skin. The most common forms of skin spots and lesions in Cowden syndrome patients are acral keratoses, cutaneous facial papules, palmoplantar keratoses, and oral mucosal papillomatosis. Acral keratosis is a term used to describe papules that appear on the upper surfaces of the feet and hands that exhibit a smooth or warty texture and a slightly pigmented color.
Cutaneous facial papules are fibrous papules that are flat-topped, dry, warty, flesh-colored, and between one and five millimeters in size. They are located around the patient's mouth, eyes, and nostrils. Palmoplantar keratosis is a term used to describe spots that appear on the soles and palms where the skin has become abnormally thickened. Oral mucosal papillomatosis is a mass that covers the tongue and appears similar to a cauliflower shape with a white color that may or may not be cancerous. It is rare for a Cowden syndrome patient to not exhibit at least one of these four skin lesions or spots.
Multiple Noncancerous Growths On The Body
Individuals affected by Cowden syndrome tend to develop multiple noncancerous growths on their bodies, including trichilemmomas, lipomas, neuromas, and sclerotic fibromas. Noncancerous bone cysts and benign adenomas in many parts of the body have also been found in patients with Cowden syndrome. Trichilemmoma is a noncancerous tumor in the hair follicle that differentiates in the direction of the root sheath.
A lipoma is a noncancerous growth that occurs underneath the skin as a result of fat cell overgrowth. A neuroma is a noncancerous growth of nervous tissues on an individual's foot between the ball of the foot and the toes. A sclerotic fibroma is a flesh-colored noncancerous growth under the skin made of hypocellular collagen bundles. Every Cowden syndrome patient develops some form of noncancerous or cancerous tumors on their body.
Enlarged Head
An individual with macrocephaly (an enlarged head) may be affected by Cowden syndrome. Someone's head is considered enlarged when the circumference is larger than the ninety eighth percentile for their respective age. An enlarged head is a symptom that occurs in 84 percent of all individuals who are affected by Cowden syndrome. The enlarged head may be caused by a number of hamartomatous growths that develop in the cerebellum or other parts of the head.
Macrocephaly that occurs as a result of Cowden syndrome can produce complications such as increased intracranial pressure, slowed growth of the rest of the body, a higher risk of developing epilepsy and autism, mental disabilities, and mental delays. An enlarged head can be investigated further through the use of an MRI scan and a CT scan. Macrocephaly in some Cowden syndrome patients can be accompanied by dolichocephaly or a head that is longer than average, or too long to be proportionate to the width of the head.
Vascular Abnormalities
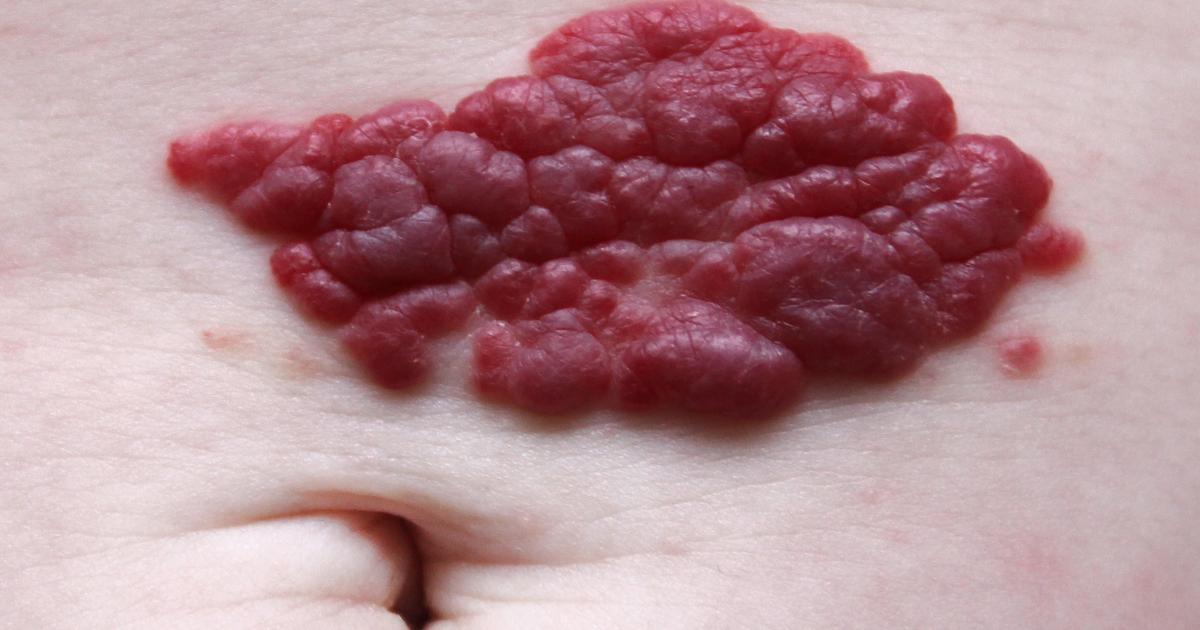
Vascular abnormalities are a common presentation in Cowden syndrome. The most prevalent types of vascular abnormalities are arteriovenous malformations, hemangiomas, and developmental venous anomalies. A hemangioma is a noncancerous growth or tumor on the body comprised primarily of tangles of blood vessels. An arteriovenous malformation is an abnormal clump of tangled blood vessels with arteries that connect to veins, which is an anatomical anomaly that causes a disruption in normal blood flow.
A developmental venous anomaly is an abnormal and noncancerous growth containing small veins that centralize in an abnormal arrangement that appears similar to the spokes found on a wheel and drains into one bigger central vein. These venous malformations are most commonly found in the brain or spinal cord. Most patients who have vascular abnormalities from Cowden syndrome do not experience direct problems from them.
Thyroid Issues
Thyroid issues may present in an individual affected by Cowden syndrome. Approximately two-thirds of all Cowden syndrome patients experience problems with their thyroid gland. Around thirty-five percent of all individuals who have Cowden syndrome will develop malignancy in the tissues of their thyroid gland. Out of this thirty-five percent, most will develop the follicular form of thyroid cancer rather than the less common papillary form of thyroid cancer. Benign adenomas or tumors of epithelial tissue are common symptoms in Cowden syndrome.
Another finding in Cowden syndrome patients is thyroglossal duct cysts or pockets in the front of the neck filled with fluid. These mostly occur in individuals of childhood age. Any benign growths that occur in an individual's thyroid gland need to be closely monitored to ensure early detection if they were to become malignant. In addition, hormones should be monitored, as any growths in or nearby the thyroid gland that precipitate from Cowden syndrome can cause decreased thyroid function.
