Treatment Options For Subungual Melanoma
Subungual melanoma describes a form of malignancy that develops in the cells under the fingernail or toenail. When carcinogenesis takes place in cells that contain skin pigments or melanocytes, it is called melanoma. Subungual melanoma is not usually related to excessive sun exposure, unlike other types of melanoma. Subungual melanoma is not diagnosed in its early stages in most cases because the population is not very aware of this form of cancer.
Subungual melanoma appears similar to a blood blister or a bruise that forms under the nail following an injury. However, subungual melanoma spots do not grow out with the nail the same way bruising and blood blisters would. Other indications of subungual melanoma that help distinguish it from bruising are cracking, thinning, splitting, and distortion of the nail plate. Diagnosis of subungual melanoma is made with a tissue biopsy, and there are several treatments to consider.
Local Removal Of Affected Area
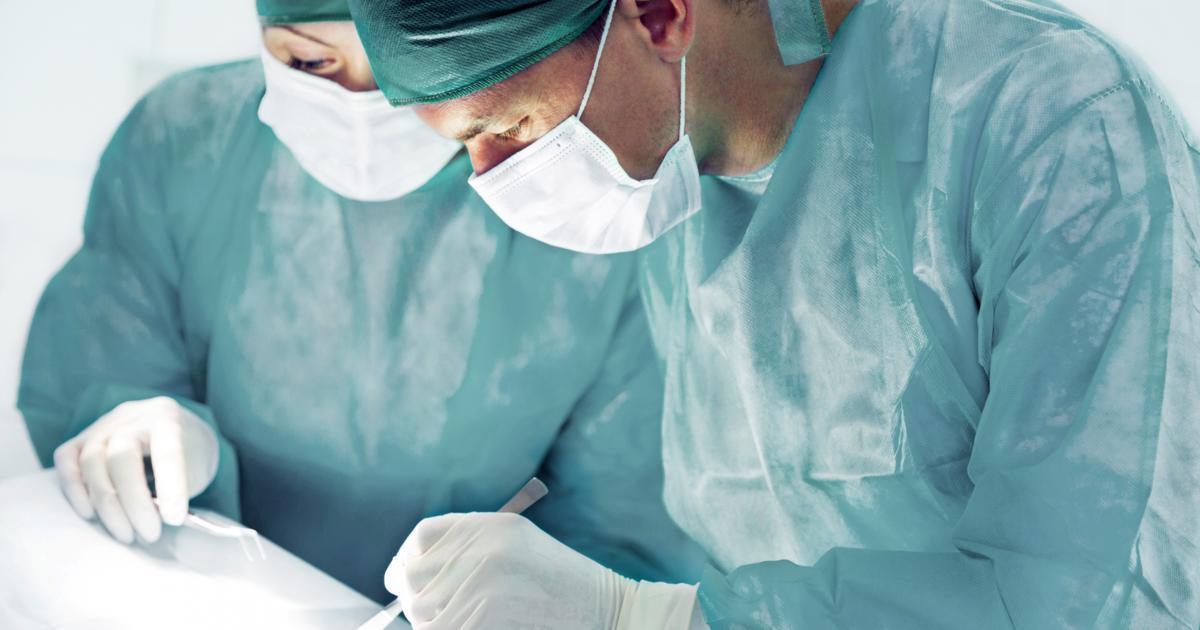
An individual may need local removal of the affected area if they are diagnosed with subungual melanoma. When subungual melanoma is in its early stages, it may be able to be excised without the need to have a full amputation of the fingertip or finger. This type of surgical procedure is referred to as a wide local excision. To even take a sample of tissue from a suspected subungual melanoma lesion, the entire nail plate must be removed.
The amount of tissue that would need to be removed beneath that point would be determined by how deep the melanoma lesion or tumor penetrates the tissues. The margins of the tumor are determined by taking scrapings of the tissue and examining them under a microscope in real-time until the surgeon reaches the layer where no cancerous or abnormal cells are seen. Once the endpoint of the subungual melanoma is determined, the surgeon removes a nominal margin of tissue surrounding the area to ensure no cancerous cells are left behind.
Amputation

An individual affected by subungual melanoma may need to undergo an amputation of the affected digit to achieve curative treatment. Before the current decade, the only effective treatment for subungual melanoma was determined to be full or partial amputation of the patient's affected digit. It is less common and less effective to amputate at the upper interphalangeal joint of the finger than it is to amputate at the lower interphalangeal joint of a finger to treat subungual melanoma.
New guidelines have been made regarding how much of a digit should be removed in the case of subungual melanoma. A lesion that has become invasive but at a measurement of less than one millimeter, at least one centimeter of the digit should be amputated. Invasive melanoma that has expanded to the size of one to two millimeters should be amputated by two centimeters. Invasive subungual melanoma that has expanded beyond the thickness of two millimeters will need to be amputated by at least two centimeters or greater depending on individual circumstances.
Radiation Therapy

An individual who has a special case of subungual melanoma with specific circumstances may need to undergo radiation therapy to treat their malignancy. Radiation therapy is a type of cancer treatment that utilizes high energy beams of protons, x-rays, or another form of radiation to cause damage to cancerous cells and stop them from growing. Cases requiring radiation therapy are those where the malignancy has metastasized to the lymph nodes or another tissue in the body. Surgery is still used in the treatment of these individuals to amputate the affected finger or toe and to excise all the affected lymph nodes.
Following surgery, radiation therapy is utilized to clear the lymph node basin of any leftover cancerous or precancerous cells. Radiation therapy is not always used in cases where only one or two lymph nodes needed to be dissected, but more for cases where extracapsular disease and or bulky lymphadenopathy were present. When subungual melanoma has metastasized to the point of the disease becoming terminal for the patient, radiation therapy may be used as part of palliative treatment to help reduce pain.
Chemotherapy
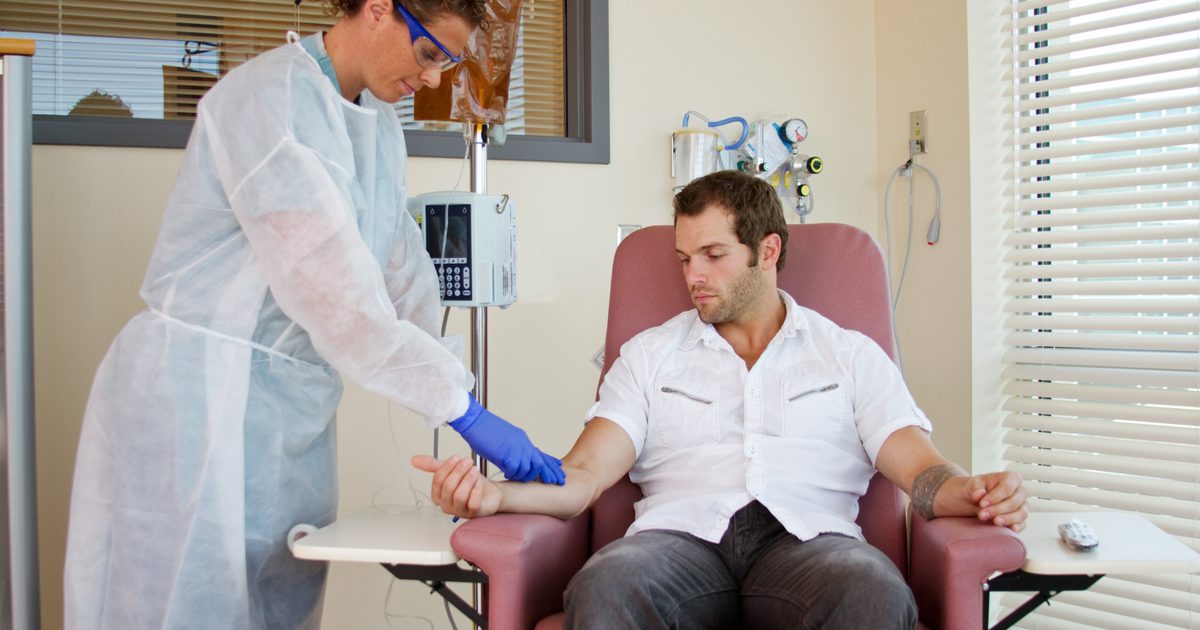
An individual may need to have chemotherapy as part of their treatment for subungual melanoma when other forms of treatment have proven unsuccessful. Since several other methods of treatment offer fewer adverse side effects with the same efficacy, chemotherapy is not used as a first-line option for any melanoma type cancers. Chemotherapy works best for melanoma that has spread into other tissues around the body. Drugs used in chemotherapy for certain forms of melanoma include dacarbazine, nab-paclitaxel, cisplatin, temozolomide, paclitaxel, and carboplatin. These may be administered independently or with one another based on the characteristics of a patient's malignancy.
Chemotherapy can be administered in creative ways in individuals who have cancer isolated to a limb. The procedure for this type of chemotherapy involves separation of the limb's blood flow from the rest of the body and isolating the circulation of chemotherapy drugs to the affected limb. The goal of chemotherapy administered in this way is to reduce chemotherapy side effects by keeping treatment isolated to the affected limb.
Immunotherapy
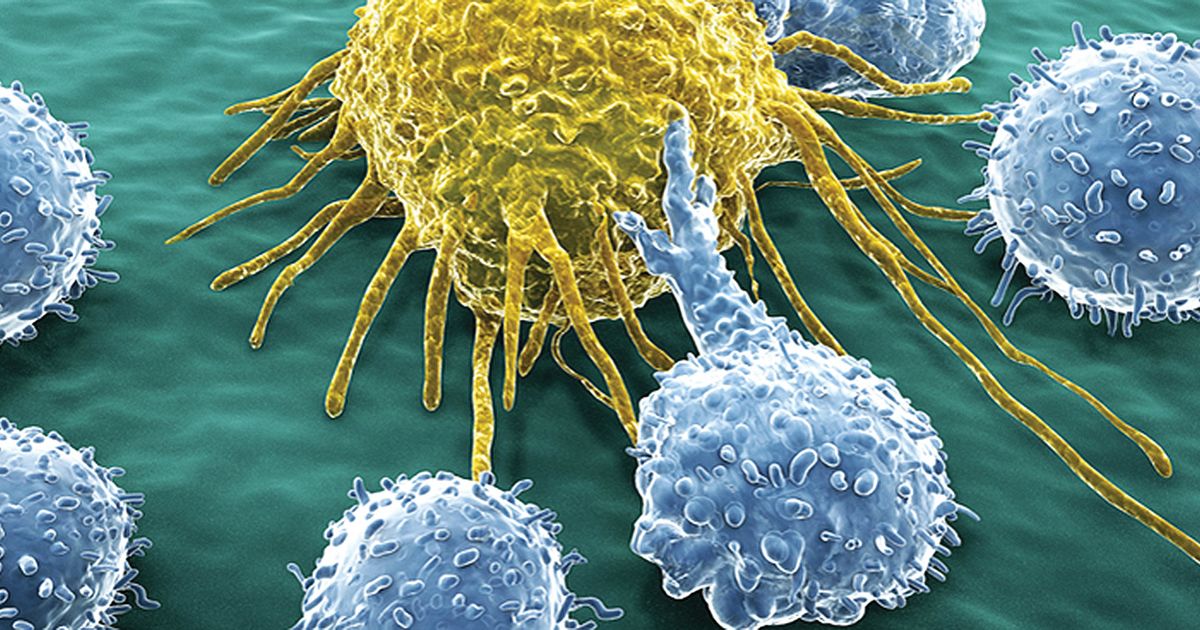
Immunotherapy is treatment involving certain drugs or drug combinations that utilize special characteristics of an individual's immune system to help target and eliminate cancer cells. Immunotherapy is often used in combination with surgery for subungual melanoma. One type of immunotherapy drug is called checkpoint inhibitors, which work by targeting certain proteins that allow cancerous cells to hide from the patient's immune system.
Another form of immunotherapy is referred to as cytokines, which increase the production and activity of the cancer hunting cells within the individual's immune system. Furthermore, oncolytic virus therapy is a form of immunotherapy that works by using harmful viruses that have been modified in a laboratory to fool the patient's immune system into initiating an attack on the melanoma cancer cells. This form of immunotherapy is not taken systemically but is injected directly into the melanoma-infiltrated tissues.
