Ankylosing Spondylitis; Symptoms, Treatments, Causes And More
Ankylosing Spondylitis (AS), sometimes called Marie-Strumpell disease is an inflammatory rheumatic disease. The condition mainly hits the lower spine but can also affect the hips, shoulders, knees, chest and other areas of the body as well. AS affects up to 0.1 percent of the world's population, and men develop the condition three times more often than women. While individuals all over the globe are diagnosed with AS, the disease is more prevalent in Caucasian males. There is no specific cure for the disease, but treatment may prevent the progression of AS.
Symptoms Associated With Ankylosing Spondylitis
Typically, the spine is the central area affected by AS. Researchers at Brigham and Women's Hospital report up to twenty-five percent of cases involve peripheral joints including the shoulders, knees, and the hips. Severe symptoms may cause debilitating pain and bone fusion. Kyphosis, a rigid and curved spine may also develop without proper treatment. Uveitis, or inflammation of the eye, has also been reported in twenty-five percent of the population diagnosed with AS and is often seen as a precursor several years before the onset of the disease. Patients with uveitis report pain, light sensitivity, and excessive tears. Up to ten percent of those coping with AS will develop spondylitic heart disease, which includes aortic insufficiency.
What Are The Causes Of Ankylosing Spondylitis?

The cause of ankylosing spondylitis is still unclear, but researchers have determined a link between the genetic marker HLA-B27 and AS. Although there is direct evidence of a correlation between HLA-B27, most people with the gene, including the majority of the Caucasian population, do not develop AS. At least sixty other genes have been identified as markers for the disease, including ERAP 1, IL-12 and IL-23. Some environmental factors may also play a role in the development of the disorder. One hypothesis proposes a link between bacterial infections that may trigger an immune response. Researchers are even trying to understand why AS affects various racial and ethnics groups differently.
Risk Factors Associated With AS

According to the Centers for Disease Control(CDC), it is estimated that 2.7 million people over the age of eighteen suffer from ankylosing spondylitis in the United States alone. Risk factors include having the HLA-B27 genetic marker, although only some people with the gene develop the condition. Researchers have found a strong correlation between a family history of AS and development of the disease. Individuals have a fifteen percent greater chance of developing AS when one parent also has the HLA-B27 marker. Studies conducted at the National Institute of Health also report frequent bacterial gastrointestinal infections as an influential precursor in disease development.
Diagnosis And Assessment Of Pain

Diagnostics include the evaluation of clinical criteria and radiological criterion. Clinical measures include assessment of pain, stiffness, and range of motion evaluations. Additionally, lab tests will be conducted, which include blood work that will search for genetic markers such as HLA-B27. X-rays are used to determine the stage of the disease. In earlier cases, when AS is suspected, computed tomography (CT) and magnetic resonance imaging (MRI) can be used to detect inflammation of the sacroiliac joints. Doctors will also rule out other diseases that sometimes present with similar symptoms. Whipple disease and Paget's disease cause sacroiliac erosions as seen in AS. Tuberculosis and Brucellosis may also affect the SI joints. Rheumatoid arthritis, gout, and degenerative joint disease must also be ruled out.
Primary Goals Of Treating AS

According to the American College of Rheumatology (ACR), the primary goals of treatment are to "reduce symptoms, maintain spinal flexibility and normal posture, reduce functional limitations, maintain workability, and decrease disease complications." Doctors recommend non-steroidal anti-inflammatory drugs (NSAIDs) as the first line of defense. Analgesics like opioids and acetaminophen are prescribed when NSAIDs do not circumvent tolerable pain. Anti-rheumatic drugs may also be included in the treatment protocol. Anti-TNF medications may be used in patients whose disease is resistant to other treatment with NSAIDs and physical therapy. Physiotherapy involves practicing stretching techniques, learning how to protect the affected joints and deep tissue massage as well as the use of alternating hot and cold compresses. Muscle performance with an increase in strength and mobility is emphasized.
Nutrition And Things To Avoid

Individuals with AS have a higher risk of developing osteoporosis which leads to bone thinning and subsequent risk for bone fractures. Alcohol should be avoided, as it may interfere with calcium and other nutrient absorption. Calcium intake should be adequate to support new bone formation. Calcium needs vary from person to person and can be determined by a medical care provider. Vitamin D is also an essential nutrient for proper absorption of calcium. Consuming a well-balanced diet that includes plenty of fruits, vegetables, and whole-grain products. Since AS is an inflammatory disease, eliminating or minimizing processed food from the diet is essential as well since these foods often contribute to inflammation.
Anti-Inflammatory Diet For Managing Symptoms

Foods that have been shown to reduce inflammation should be considered for individuals managing symptoms ofAS. "Many experimental studies have shown that components of foods or beverages may have anti-inflammatory effects," says Dr. Frank Hu, professor of nutrition and epidemiology in the Department of Nutrition at the Harvard School of Public Health. Foods that are known to have anti-inflammatory effects include tomatoes, green leafy vegetables, olive oil, and fruits with high antioxidant properties like blueberries, cherries, oranges, and strawberries. Walnuts and almonds also show high anti-inflammatory effects. Additionally, fatty fish like tuna, sardines, and salmon work to reduce inflammation. Incorporating spices like curcumin, turmeric, and cayenne into a diet have also shown to relieve inflammation.
Progression Without Treatment Of AS
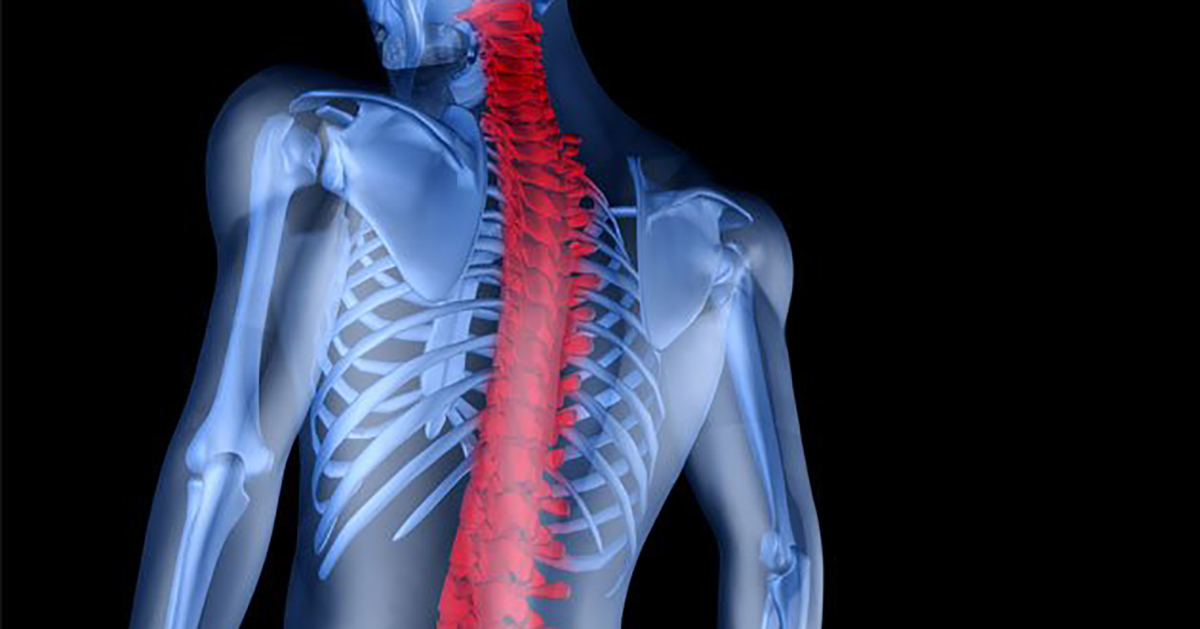
The course of the disease varies widely among each individual. Periods free from symptoms may follow flares or painful episodes. The condition is likely to progress without treatment, so it is crucial to seek a diagnosis and subsequent treatment as soon as possible. Disease onset is usually gradual and the disease may progress over time, moving up from the sacroiliac joints into the spinal column affecting other vertebrates. Progression of the disease may also include, in advanced cases, spinal fusion and complete immobility at the point of fusion. Age is not a factor in the prognosis of AS; however, studies indicate a worse prognosis for individuals who develop the disease during adolescence. An early diagnosis carries the best prognosis for all age groups.
