What Causes Biliary Atresia?
Biliary atresia, which only affects newborns, is a condition in which the bile ducts are absent or blocked. Babies with biliary atresia typically appear healthy at birth, and symptoms begin to appear around two to eight weeks later. Patients present with jaundice (yellow discoloration of the skin or whites of the eyes), and they pass white or pale stools. A swollen abdomen, enlarged liver, and enlarged spleen might be observed, and patients often have dark-colored urine. Since biliary atresia affects fat absorption and increases metabolism, patients may struggle to gain an appropriate amount of weight, and they might even experience weight loss. Protein deficiencies and vitamin deficiencies are common as well.
To diagnose biliary atresia, doctors perform a physical examination to check for signs of jaundice. They will gently feel the liver and spleen to check for enlargement and if these organs feel harder than normal. Patients will have blood tests, and an abdominal ultrasound, HIDA scan, and liver biopsy may be recommended. A surgical intervention known as the Kasai procedure is the preferred treatment method for biliary atresia. If successful, the operation could restore normal or near-normal bile flow. However, some patients might still need to have a liver transplant to completely cure the condition.
Improper Development
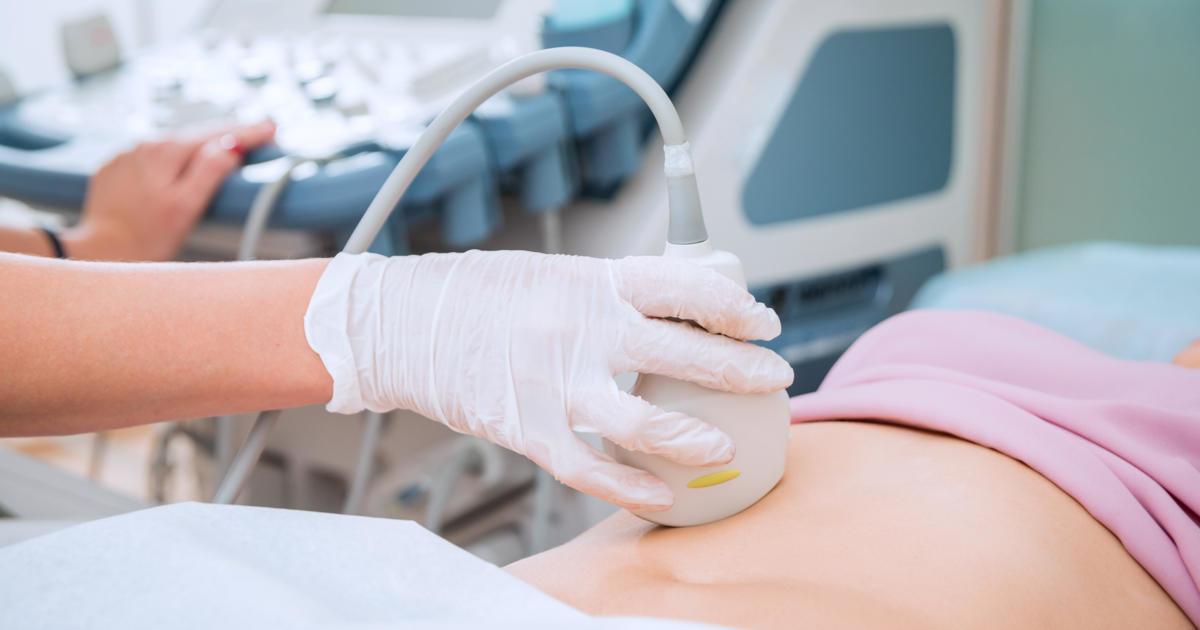
Fetal (embryonic) biliary atresia is the less common form of the condition, and it accounts for between ten to thirty-five percent of all diagnosed cases of biliary atresia. Unlike other forms of the condition, patients with fetal biliary atresia frequently present with jaundice at birth and display improper development of organs such as the heart, spleen, and intestines.
The development of major blood vessels might also be abnormal. While the baby is still in the womb, doctors might notice the improper development of the baby's heart and other organs during routine prenatal ultrasound scans. The organ development will be monitored at regular visits, and the mother may be referred to specialists for further advice and testing. If fetal biliary atresia is confirmed, surgery will likely be recommended shortly after birth.
Damage Due To Viral Infection
Some researchers believe biliary atresia may be caused by damage due to viral infection. As part of the diagnostic tests for this condition, physicians will carry out blood tests to check for viruses such as HIV and hepatitis. Recent studies have shown a possible link between biliary atresia and infection with the Epstein-Barr virus, rotavirus, and reovirus. Human cytomegalovirus (CMV) and human herpes virus-5 are also believed to play a role in the development of biliary atresia. In fact, a landmark study conducted in the 1970s found injecting guinea pigs with CMV led to changes in the bile ducts that were similar to those seen in humans with biliary atresia.
A study from the same period conducted on murine models produced similar results. Currently, the evidence supporting a viral cause for biliary atresia is weak, and further research is needed to establish how viral infections may impact the development of the condition. Parents who believe their child may have been exposed to a virus in the womb or shortly after birth should inform their healthcare team so the appropriate tests can be performed.
Bile Duct Inflammation And Blockage

Bile duct inflammation and blockage is the primary cause of biliary atresia. In patients with both forms of biliary atresia, the bile duct becomes narrowed and blocked, and bile cannot flow properly from the liver to the intestine. When this happens, the bile accumulates in the liver instead, and this causes scarring and other damage. Eventually, the bile duct blockage can cause cirrhosis of the liver. Patients with a bile duct blockage often have trouble getting adequate nutrition, and they may need to be fed through a nasogastric tube. Doctors can detect a bile duct blockage through imaging studies such as HIDA and DISIDA scans.
Using an injection of radioactive dye, these tests produce images that show if bile can flow from the liver into the gallbladder and intestines. A cholangiogram can also be used for this purpose. Cholangiograms are x-rays carried out by surgeons in the operating room. These studies help show if the bile ducts that carry bile away from the liver are blocked. If surgeons determine a blockage is present, they will proceed with exploratory surgery to confirm biliary atresia. The Kasai procedure can be used to restore bile flow to blocked ducts, and a liver transplant may be necessary if this is unsuccessful.
Gender And Ethnicity

Currently, researchers believe gender and ethnicity could be risk factors for biliary atresia. The condition is more common in female infants than in males, and African-American and East Asian communities have higher rates of biliary atresia than other communities. In East Asia, the condition occurs in approximately one out of every five thousand births, and it is diagnosed in an estimated one out of every 16,700 births in Great Britain and one out of every ten to fifteen thousand births in the United States.
In twins, usually only one twin will have biliary atresia, and the other will not have the condition. All parents should be familiar with the potential symptoms of biliary atresia, including jaundice, pale stools, dark urine, and a swollen abdomen, and they should seek help for these symptoms immediately.
Genetics
Research has shown possible connections between genetics and biliary atresia. In a population-wide genome study conducted in China, an association was found between the development of the condition and a gene known as ADD3. This association was also discovered among individuals in Thailand and Caucasians. Other studies have shown biliary atresia could be connected to the deletion of the GPC1 gene. Located on the second chromosome, this gene regulates inflammation and also serves as a regulator for the Hedgehog gene.
An additional study of Egyptian infants with this condition found they had a null GSTM1 genotype. The infant's mothers were all heterozygous for GSTM1. Thus, researchers believe the infants were protected in utero, but they could not cope with the detoxification of aflatoxin load that occurred after birth. More research is being done to better understand how genetics may be involved in biliary atresia.
