What Causes Fat Embolism Syndrome?
Fat embolism syndrome is a serious condition that can occur when a segment of intravascular fat becomes stuck inside an individual's blood vessel and obstructs the flow of blood to certain areas of the body. Symptoms of fat embolism syndrome include shortness of breath, lethargy, petechial rash, anemia, rapid breathing, mental confusion, fever, and coma. Severe inflammation, neurological alterations, and multi-organ dysfunction can also occur in fat embolism syndrome patients.
There is no established diagnostic test for this condition, so diagnosis is typically made based on a physical examination, Gurd's criteria, and medical history. Supportive care is the focus of fat embolism syndrome treatment and includes interventions such as supportive oxygen therapy, medication to increase blood volume, steroids, blood thinners, and intravenous fluids. This type of therapy is provided to eliminate free fatty acids from the body that are causing tissue damage and inflammation.
Liposuction
Liposuction procedures can cause an individual to develop fat embolism syndrome as a result of their surgery. Liposuction is an elective cosmetic procedure involving the surgical removal of excess fat. Fat embolism syndrome caused by liposuction typically manifests between twelve and seventy-two hours following the procedure. This type of surgery involves the use of a hollow instrument in a back and forth motion to loosen and dislodge the targeted fat. Mechanically, this process causes widespread rupture and injury to small blood vessels feeding these fat tissues. It also damages cells in the connective tissues designed to store fat.
These two factors explain how micro fragments of fat can enter the affected individual's venous circulation. These micro fragments of fat are propelled in venous circulation to the lungs where blood is reoxygenated, causing damage to the lung tissues. Fat micro fragments can also enter into systemic circulation or circulation of blood from the heart to the rest of the body. Consequently, these fat fragments can cause embolization in the patient's retina, kidney, brain, and skin. The ensuing inflammatory process due to the damage done by fat emboli and the procedure itself contributes to many symptoms seen with fat embolism syndrome.
Bone Marrow Transplant
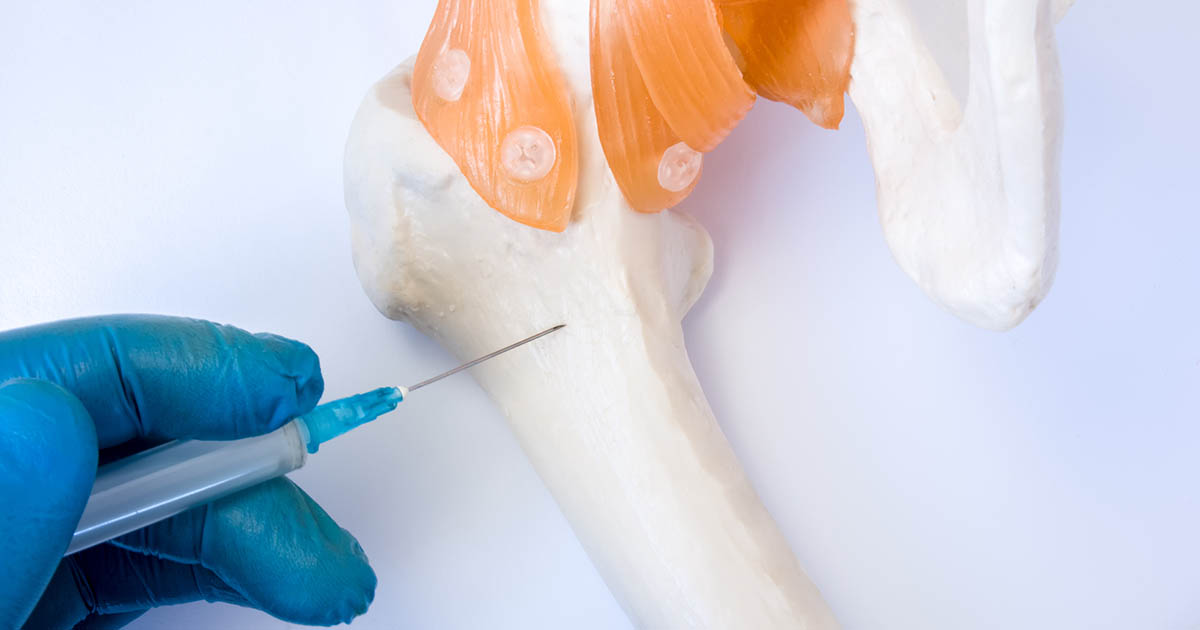
Fat embolism syndrome may develop after an individual undergoes a bone marrow transplant or harvest. An individual who is having bone marrow harvested from their body undergoes a procedure where a large needle is used to puncture through the skin, connective tissues, and into the intramedullary cavity of their pelvic bone to extract large amounts of bone marrow. Fat cells in the bone marrow have a dynamic prothrombotic and proinflammatory aptitude. The trauma that occurs during the harvesting of bone marrow from multiple penetrations of the bone into the intramedullary cavity allow some of these cells to gain access to the sinusoids or veins in bone marrow and other organs that allow easy penetration of small particles.
As these fat cells move through venous circulation, they promote the rapid clumping of platelets and expedited production of fibrin in the blood. From there the fat emboli can enter the patient's lungs and cause symptoms of fat embolism syndrome associated with pulmonary capillary obstruction. Characteristic dermatologic and neurological symptoms of fat embolism syndrome are produced by these fat emboli when they reach arterial circulation through the pulmonary capillary bed or a patent foramen. Macrovascular obstruction by the fat emboli can produce fat embolism syndrome manifestations associated with ischemic shock.
Sickle Cell Anemia
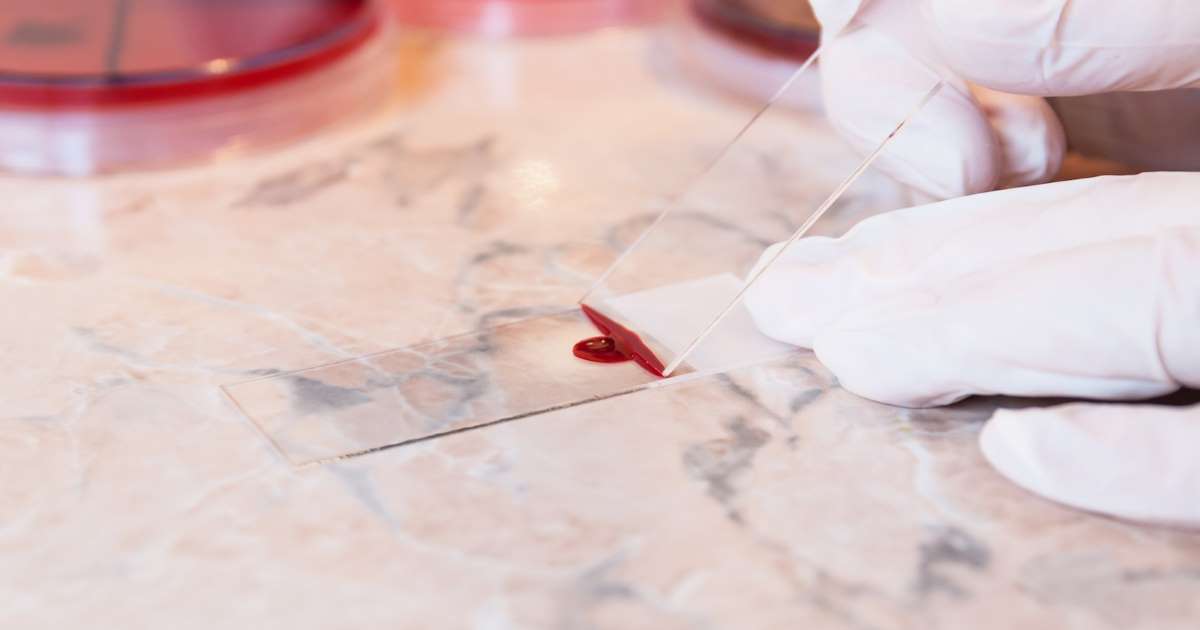
A sickle cell anemia patient may develop fat embolism syndrome as a complication of their disease. Fat embolism syndrome develops after the affected individual has a vaso-occlusive crisis, which occurs when the sticky, malformed sickle cells obstruct small blood vessels, producing cellular injury from oxygen deprivation. Due to a vaso-occlusive crisis, bone infarction can occur or the death of bone marrow cellular elements due to ischemia or lack of blood flow. Inside the bone, the fat globular cellular material leftover from this process can diffuse into the sinusoid veins that run through the bone. Once in the venous circulation, these fat globules trigger an inflammatory response involving the accumulation of chylomicrons, fibrin, low-density lipoproteins, platelets, and other blood elements.
It is thought this congregation of materials triggered by bone marrow fat globules forms the fat emboli that cause damage to the affected individual's lungs and may enter the systemic circulation. Right to left shunts or a septal defect in the patient's heart can allow the perfusion of the fat emboli into the arterial bloodstream. The fatty emboli have the potential to become lodged in the vessels of critical organs such as the brain, skin, and return to the lungs. Obstruction of blood flow to tissues of these organs by the emboli is what produces the symptoms of fat embolism syndrome.
Osteomyelitis
An individual's osteomyelitis may cause them to develop fat embolism syndrome as a complication of their condition. Osteomyelitis describes the infection or inflammation of bone marrow or bone. This type of inflammation or infection is caused by a pathogenic infection entering the bone from the bloodstream or direct injury. When this process happens, immune components like neutrophils are summoned to the bone to try and eradicate the causative pathogen. If the infection overcomes the neutrophils in the bone, these dead cells begin to build at the infection site. This buildup can obstruct the flow of blood to the tissues and can result in bone death.
While the exact mechanism has not been pinpointed, the development of fat emboli in affected individuals is known to be associated with the effects of elevated c-reactive protein. The liver produces and releases this protein in response to inflammation caused by numerous processes, including osteomyelitis and its associated bone tissue damage. C-reactive protein has a high potential to cause clumping or congregation of low-density lipoproteins, chylomicrons, and liposomes of nutritional fat compounds. It is an excessive provocation of this inflammatory process that causes the formation of fat emboli in the venous capillaries traveling to the lungs, producing symptoms of fat embolism syndrome.
Severe Burns
Individuals who experience severe burns on a large portion of their skin area can develop fat embolism syndrome. This pathophysiology is the result of both mechanical factors and biochemical processes. The skin is made up of several layers. The outermost layer is called the epidermis and provides a waterproof barrier between underlying tissues and external elements. The next layer, called the dermis, is packed full of nerves and blood vessels that supply sensation and blood to the skin. The layer below the dermis is called the fat layer or subcutaneous tissue, which stores fat, protects underlying tissues from exaggerated temperature changes, and produces certain hormones. The subcutaneous layer has blood vessels within it that are slightly larger than those found in the dermis.
Extreme heat can scald away the epidermis, all or part of the dermis, and penetrate the subcutaneous layer. This type of injury causes blood vessels in the affected regions of the skin to be vaporized, severed, and or severely damaged. When the burn has penetrated the subcutaneous layer and damages lipid storing cells, micro fragments of fat are allowed to mobilize into the venous bloodstream. Inflammatory processes cause the fragments to materialize further and become lodged in the lungs, producing symptoms of fat embolism syndrome.
