Guide To The Causes Of Leg Ulcers
A leg ulcer an open wound or sore that develops on an individual's leg. Symptoms include pus at the ulcer site, increasing wound size, enlarged veins, pain at the ulcer site, heaviness in the legs, and swelling in the legs. Medical history, physical examination, CT scan, MRI scan, vascular ultrasound, and x-rays may be used to diagnose leg ulcers. The main concern when it comes to leg ulcers is the risk of developing an infection in the wound that progresses to a life-threatening blood infection.
Thankfully, there are many leg ulcer treatment options out there. Patients may need compression bandages to treat their ulcers. Leg ulcer medication includes antibiotics for infections as well as medication for circulation, topical ointments, and pain medication. Leg ulcer wound care should also include natural treatments and home remedies for leg ulcers, such as diet changes and braces or orthotics. Overall, the best leg ulcer treatment can vary based on the underlying cause. Get to know the common causes now.
Venous Insufficiency
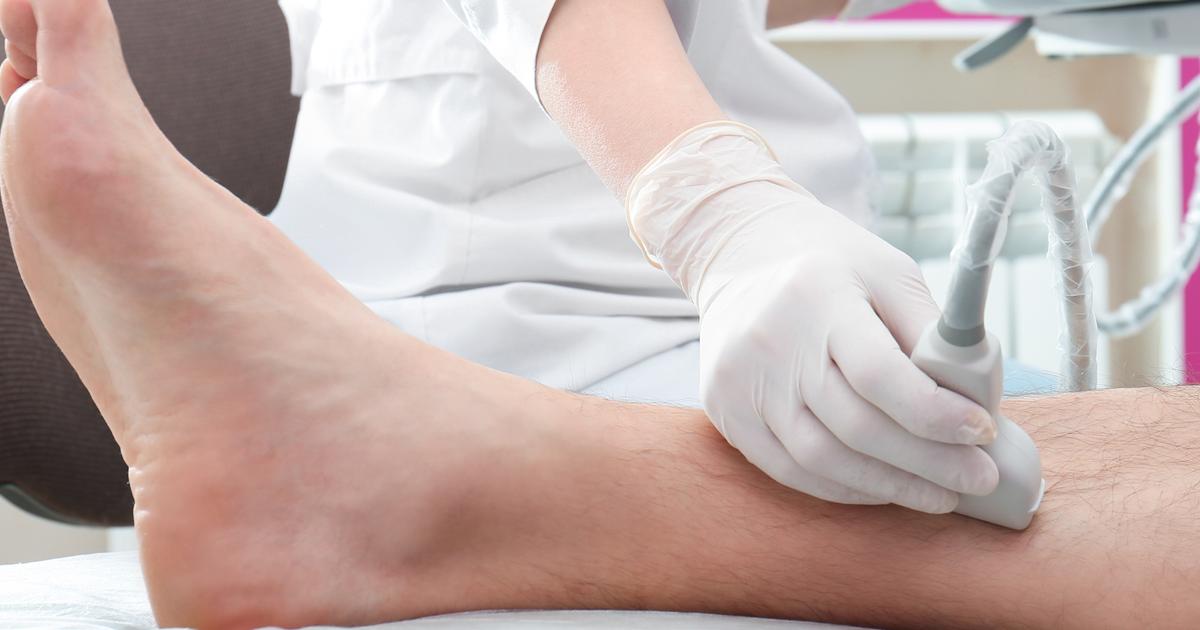
An individual affected by venous insufficiency can develop leg ulcers as a complication. Chronic venous insufficiency is a condition where an individual's venous valves in the legs do not function well enough. The valves in the veins of the legs move blood back to the heart so it can be reoxygenated. However, chronic venous insufficiency patients tend to experience blood pooling in the legs because it gets backed up. When blood pools in an individual's legs, fluid in the blood is forced into the surrounding tissues, causing edema.
Edema left untreated can compress the capillaries responsible for blood delivery to the skin and its underlying fatty tissues. When these tissues become deprived of oxygen, the skin cells begin to die and form a sore or an ulcer. The ulcers can also be relatively painless due to the lack of nerve cell function in the affected area, which results in delayed treatment and infection.
Hypertension
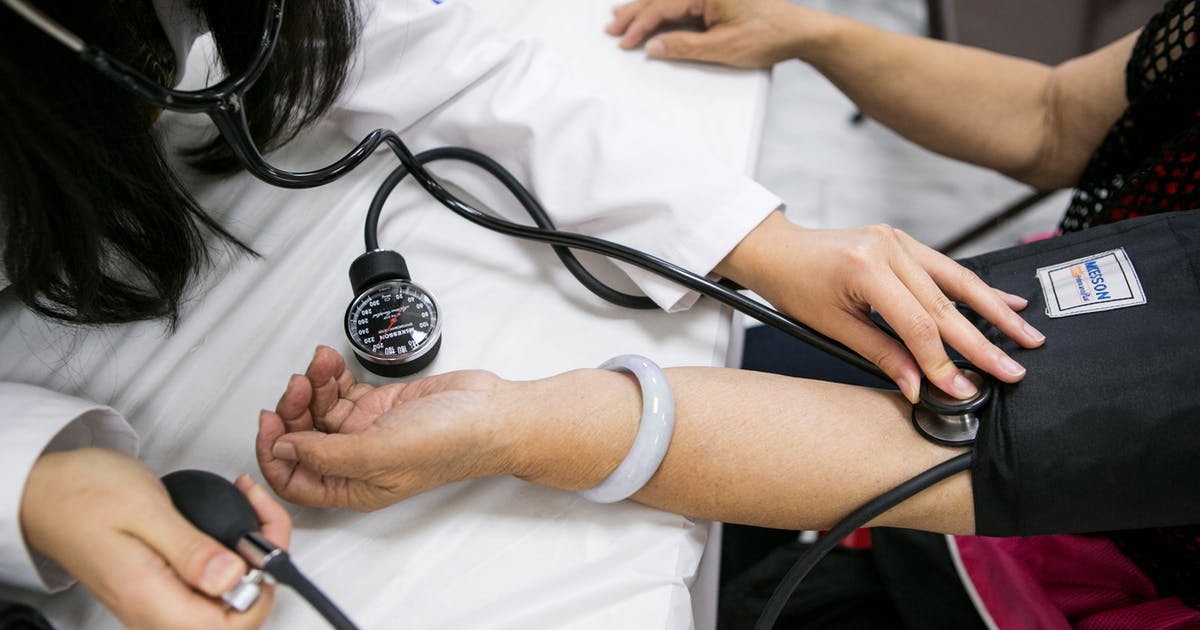
Leg ulcers may be caused by long-term high blood pressure, which is also referred to as hypertension. Blood pressure is the measurement of the amount of force blood is placing on the blood vessels as it is moving through them. Leg ulcers are a complication that can occur in individuals who have poorly controlled hypertension. The exact mechanism of leg ulcer development from hypertension is not well established. However, it is thought to involve the narrowing of the small capillaries responsible for supplying nutrients and oxygen to the skin and underlying fatty tissues.
The narrowed capillaries that feed the skin cause an increased amount of resistance to the blood that needs to flow through them, which causes a reduction in the amount of blood affected tissues receive. Some believe that it is an ischemic process that occurs in hypertension patients that causes the skin cells to die, resulting in the development of sores and ulcers in the legs.
Poor Circulation

An individual who experiences issues with poor circulation in their legs can develop leg ulcers. Someone may experience poor circulation in their legs due to several mechanisms, including the function of their heart, problems with the blood vessels, clotting problems, and blood pressure issues. Poor circulation describes where blood is not moving through the veins back to the heart and through the arteries to be recirculated as fast and efficiently as it should. Leg ulcers are caused by a lack of oxygen and nutrients to the skin cells that causes them to die.
The blood in the body has to move at a sufficient pace and carry an adequate amount of oxygen to the distant tissues in the legs for the skin cells to survive and function. Individuals who have chronic problems with the structure or function of their connective tissues, nerve function, muscle function, and blood vessel function can experience inadequate circulation in their legs. Regardless of the underlying cause, the necrosis of skin tissues due to oxygen starvation is the most common way leg ulcers develop.
Diabetes
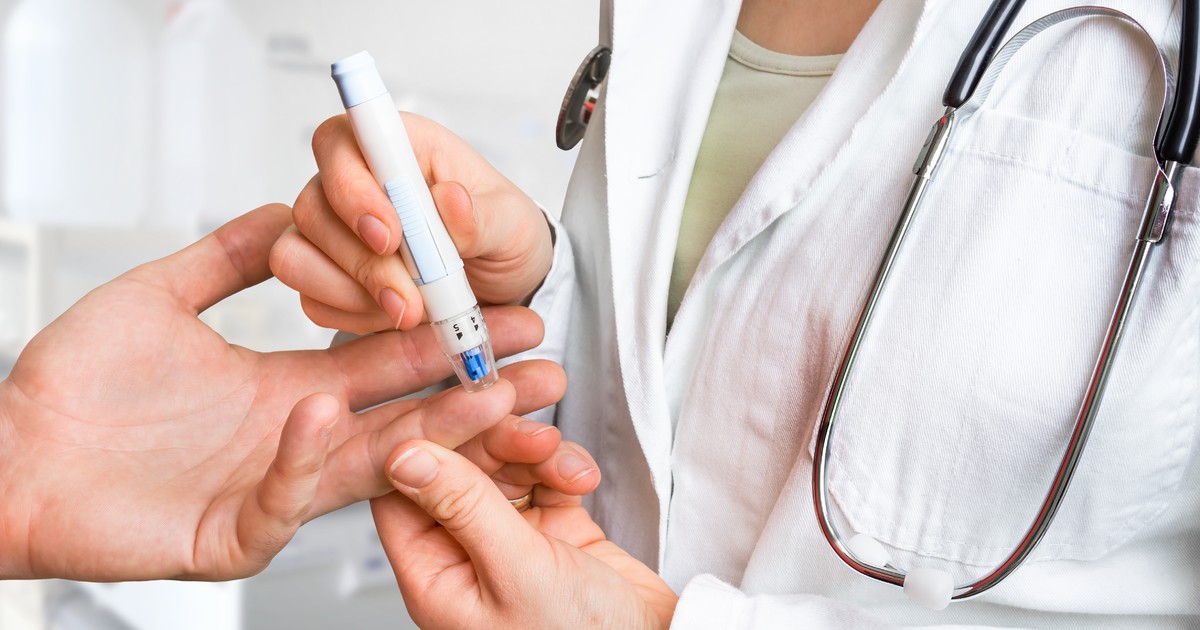
Leg ulcers are commonly found in diabetes patients. Diabetes is a disease where an individual's body does not produce a hormone called insulin or does not respond to the insulin the body does produce. Insulin is a hormone secreted by the pancreas when an individual's blood sugar begins to rise. This mechanism in the body is essential because high blood sugar is known to cause progressive damage to the kidneys, blood vessels, nerves, and other tissues. In diabetes, the body cannot effectively regulate blood sugar due to a malfunction of the natural blood sugar regulation process in healthy individuals.
High blood pressure induced by poorly managed diabetes can cause leg ulcers to develop due to an ischemic process that occurs in the skin tissues. Neurotrophic ulcers are a type of leg and foot ulcer that can develop in a diabetes patient due to diabetes-precipitated neuropathy. The nerves become damaged from unregulated high blood sugar, leading to circulation problems and reduced pain signals. A diabetes patient may develop a small ulcer from secondary causes that can become enlarged and infected due to the unintentional neglect that occurs with an inability to sense pain.
Heart Disease

A heart disease patient may develop leg ulcers as a complication of the disease's effects on their body. Heart disease refers to a condition where the arteries in an individual's body become hard and narrowed due to the buildup of a substance referred to as plaque. The blood vessels in healthy individuals have flexible walls and can accommodate the higher pressure and increased blood volume temporarily. However, patients who have developed heart disease due to the accumulation of plaque in their arteries have blood vessels that cannot compensate under challenging conditions.
Plaque buildup occurs when long-term high blood pressure has damaged the lining of the arteries. This allows cholesterol and other fatty substances to penetrate and calcify in the vessel. As more plaque accumulates, the total amount of space blood can pass through becomes progressively reduced. This mechanism causes a shortage of oxygenated blood in distant tissues of the body, such as the subcutaneous tissues of the legs and feet. Without an adequate blood supply in these tissues, the cells can necrotize and cause open ulcers to develop.
High Cholesterol
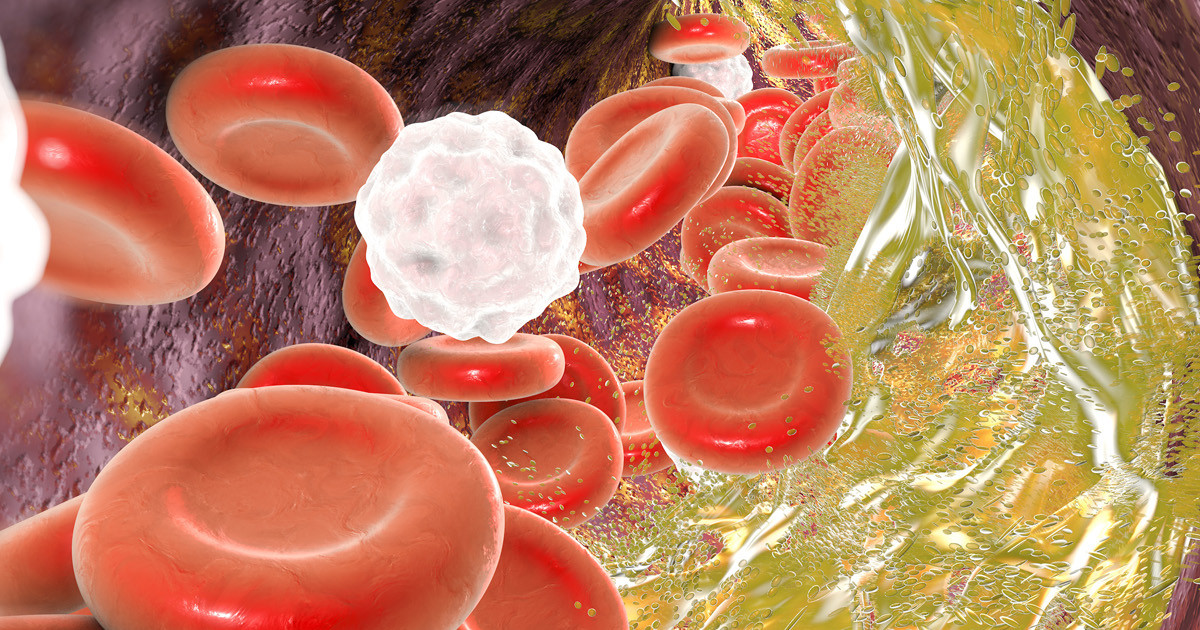
Cholesterol, a lipid, is a waxy substance the liver produces. Everyone needs it, since cholesterol helps form cell membranes, vitamin D, and some hormones. It travels on its own through blood. There are two main types of cholesterol: low-density lipoprotein and high-density lipoprotein cholesterol. Although both forms of cholesterol are found in the body, if low-density lipoprotein cholesterol, the unhealthy kind, is too high, patients are considered to have high cholesterol.
As many individuals know, high cholesterol is a major risk factor for many health conditions. One of these is the development of leg ulcers. Specifically, high cholesterol increases the risk of arterial ulcers. It does this because as the cholesterol builds in their arteries, they will often narrow and become blocked. Thus, other tissues will not receive enough nutrient-rich blood, causing the wound or ulcer to form.
Kidney Failure

Kidney failure is a serious condition in which an individual's kidneys can no longer filter waste from their blood efficiently. Toxins build in the individual's body if their kidneys are not functioning properly, which is what triggers kidney failure. Symptoms include reduced urine output, unexplained shortness of breath, persistent nausea, excessive fatigue, and leg swelling.
Kidney failure increases the risk of leg ulcers for several reasons. One, of course, is that the increased swelling in the patient's legs makes it easier for ulcers to form because they can deprive some areas of the leg of oxygen. A lack of oxygen can make ulcers form. In addition, diabetes is the most common risk factor for the development of kidney failure. This condition is also a major cause of leg ulcers.
Lymphedema

Lymphedema is a serious chronic condition. It refers to swelling due to excess lymphatic fluid building in the soft tissues of the body. Swelling can compromise the healing in the body and prevent enough oxygen and nutrient-rich blood from reaching all of the tissues. This condition can occur in many areas of the body, though the most common is in the arms or legs. It is when lymphedema occurs in the legs that dramatically increases the patient's risk of developing leg ulcers.
Lymphedema is most often seen in patients who have undergone various cancer treatments, including chemotherapy, radiation therapy, and surgery. This is because cancer treatment can include the removal of lymph nodes or damage to them, which results in disrupted lymphatic drainage and, thus, swelling. Extensive swelling in lymphedema often triggers skin changes, including open wounds and leg ulcers.
Genetics

In some instances, leg ulcers can be hereditary, which means that an individual's genetics is what increases their risk of developing them. In other words, if an individual has an immediate family member who has had leg ulcers, they themselves are more likely to develop them. The influence of genetics on the development of leg ulcers is, in some cases, unclear. However, it is also worth noting that some of the previously mentioned risk factors and causes also have a genetic component to them. This means that they also increase the chances of an individual developing leg ulcers. Two examples of this are diabetes and heart disease. Some kidney diseases are genetic and can lead to kidney failure, another risk factor for leg ulcer development.
Scleroderma

Scleroderma is a rare, chronic autoimmune condition. It affects the skin and other organs, resulting in inflammation and other issues, such as tight and thickened skin. Scleroderma causes many problems in the body because of these effects. In many cases, patients can deal with problems in their kidneys, heart, lungs, and other areas.
Examples of these problems include rapid kidney failure, heart disease, and heart failure. In all of these examples, patients are at a much higher risk for the development of leg ulcers. In addition, the chronic inflammation linked to scleroderma is another significant trigger for the formation of leg ulcers. Unfroatunely, there is no cure for scleroderma, though patients can manage their condition with treatments such as laser therapy, exercise, occupational therapy, and a healthy diet.
