Guide To The Causes Of Pancreatitis
Pancreatitis is an illness where severe inflammation develops in the pancreas. The pancreas is a large gland located behind the stomach that produces hormones responsible for regulating how the body metabolizes glucose and enzymes that assist with digestion. Acute pancreatitis is a sudden and severe inflammation of the pancreas that lingers for days, and chronic pancreatitis lasts for years. Symptoms of acute pancreatitis include upper abdominal pain, abdominal pain that worsens after eating, rapid pulse, vomiting, back pain, fever, nausea, and tenderness when the abdomen is touched. Symptoms indicative of chronic pancreatitis include upper abdominal pain, unintentional weight loss, and steatorrhea. Pancreatitis diagnosis is made with the use of blood tests, stool tests, CT scans, abdominal ultrasound, endoscopic ultrasound, and MRIs. Treatment of pancreatitis may consist of fasting, pain medication, intravenous fluids, bile duct surgery, gallbladder surgery, pancreas surgery, diet changes, enzyme supplements, and alcohol dependence treatment.
Activated Digestive Enzymes

The pancreas is responsible for producing certain digestive enzymes that move through ducts into the small intestine when food is leaving the stomach. There is a carefully coordinated process that signals the pancreas to produce these enzymes at the perfect time. This process ensures they activate upon moving into the small intestine to assist with digestion. The secreted pancreatic enzymes are chymotrypsin, trypsin, pancreatic lipase, amylase, ribonuclease, deoxyribonuclease, elastase, and gelatinase. A blockage or kink in the pancreatic or bile ducts can cause these enzymes to be unable to reach the small intestine before the activation process begins. This group of digestive enzymes is responsible for breaking down starches, fats, and proteins. To be able to break down these components of the food, these enzymes have to be potent and concentrated. The underlying tissues of the small intestine are protected from the corrosiveness of these enzymes by the mucosal layer in the organ. However, pancreatic tissues do not have this protection when these enzymes become activated. The activation of the enzymes in the pancreatic tissues causes the gland to become severely inflamed and possibly infected.
Abdominal Surgery
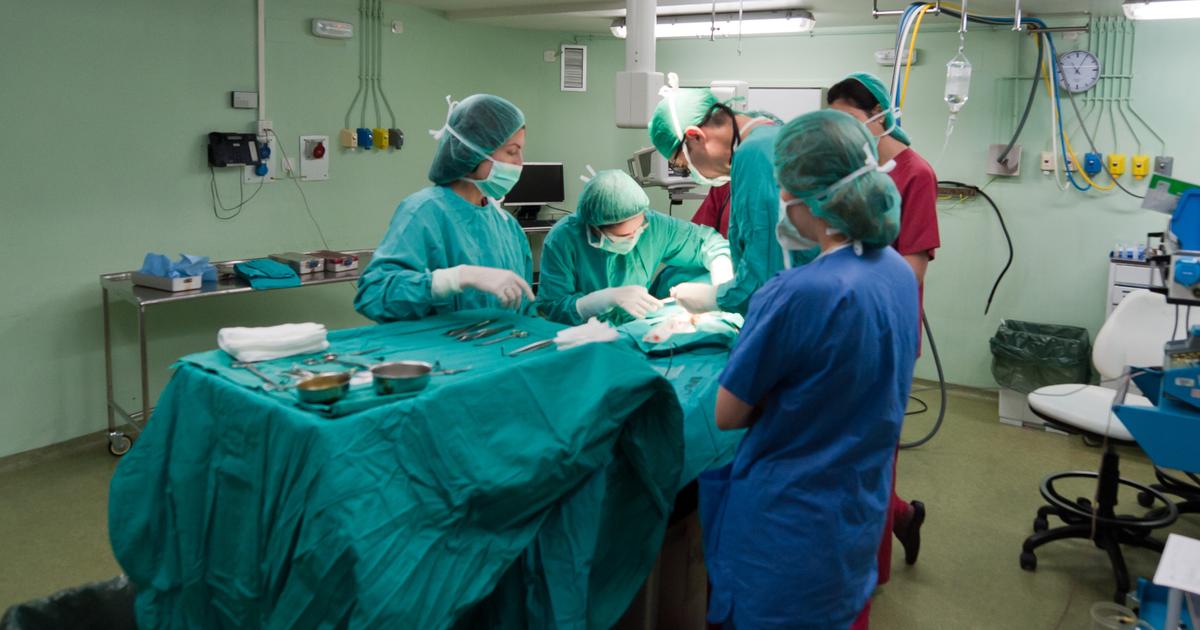
An individual who undergoes abdominal surgery may develop pancreatitis as a complication. The most prevalent procedure known to cause pancreatitis is referred to as endoscopic retrograde cholangiopancreatography. While this is not a major or invasive form of abdominal surgery, it does require the patient to be anesthetized and involves the use of an endoscope. The prevalence of pancreatitis development following an endoscopic retrograde cholangiopancreatography is four percent of all diagnosed cases of pancreatitis. Other forms of abdominal surgery that cause trauma to the abdominal region can cause patients to experience an increase in lipase and amylase levels that may cause them to develop pancreatitis. Other surgical procedures known to cause pancreatitis as a post-operative complication include cardiopulmonary bypass surgery and abdominal bypass surgery. This etiology of pancreatitis has a greater rate of death and other life-threatening complications than pancreatitis that has developed from other causes.
Gallstones
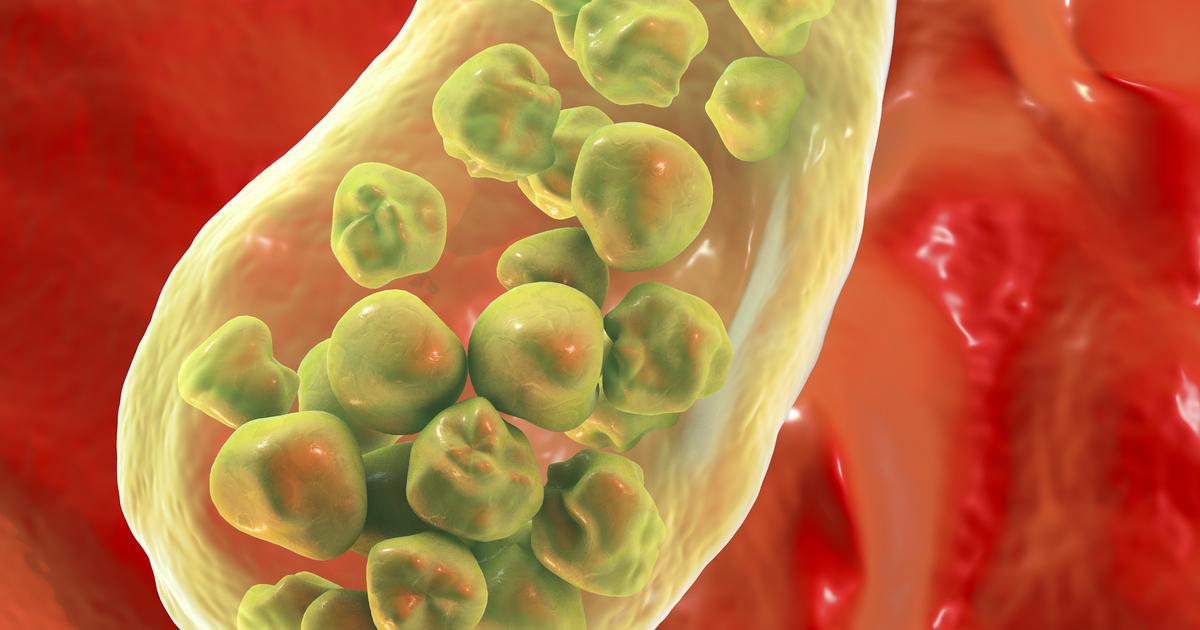
An individual who has developed gallstones may become affected by pancreatitis. The gallbladder is a small sack-like organ that sits just underneath the liver, and it is responsible for the concentration and storage of bile. Bile then drains from the gallbladder to the small intestine when food exits the stomach to help with the digestion of fatty substances. In some individuals, the balance of the components in the bile stored in the gallbladder can become imbalanced or too concentrated. These malfunctions cause the components to pass their solubility threshold and form solid stones in the gallbladder. Stones in the gallbladder can move into the common bile duct, which is responsible for draining digestive enzymes from the pancreas and bile from the gallbladder into the small intestine. When the common bile duct becomes obstructed by gallstones, the pancreatic enzymes are allowed to activate while they are still in the pancreatic tissues. Activation of enzymes in the pancreatic tissue causes pancreatitis or irritation, inflammation, and infection of the gland in some cases.
Certain Medications
An individual may develop pancreatitis as a result of taking certain types of medications. However, this is rare. Between one and six percent of individuals who use medications called 6-mercaptopurine and azathioprine are affected by drug-induced pancreatitis. Azathioprine and 6-mercaptopurine are drugs used to treat patients affected by certain autoimmune disorders, as are immunosuppressants. The exact mechanism of how these drugs cause pancreatitis is not known, but it is thought to be related to an increased predisposition to adverse reactions and infection caused by the mechanism of the drug. A class of medications referred to as ACE inhibitors is also known to trigger pancreatitis in some individuals who take them to treat heart failure, hypertension, and proteinuria. The most common ACE inhibitors known to cause pancreatitis are enalapril, captopril, perindopril, lisinopril, and ramipril. The exact mechanism behind how these medications cause pancreatitis is not known, but it is thought to be related to angioedema around the gland. Other drugs that can cause pancreatitis include 5-ASA, some antibiotics, statins, and some antidiabetic drugs.
Pancreatic Cancer

An individual affected by pancreatic cancer may be affected by pancreatitis as a complication of their malignancy. Pancreatic cancer is commonly seen as a complication that occurs in patients affected by pancreatitis at some point in their life. However, pancreatic cancer can also cause an individual to develop pancreatitis through certain mechanisms. A malignant tumor in the pancreas can grow around the duct responsible for draining pancreatic fluid into the small intestine. The pancreas produces digestive enzymes that help with the digestion and breakdown of protein in food. To protect the pancreatic tissues and ducts, the digestive enzymes do not activate until a certain point in time after they have been produced. By the time the digestive enzymes activate, they are intended to be in the small intestine protected by a layer of mucus. However, a cancerous tumor can cause the pancreatic duct to become crimped or fully obstructed, which stops the digestive enzymes from reaching the small intestine before they become activated. These enzymes damage the tissues of the pancreas and cause inflammation or pancreatitis.
