What Causes Pituitary Apoplexy?
Pituitary apoplexy is an emergent medical event where a patient experiences infarction or hemorrhage in their pituitary gland. Symptoms of pituitary apoplexy include altered consciousness, vomiting, headache, facial pain, fever, loss of body and facial hair, infertility, appetite loss, weight loss, weight gain, fatigue, dizziness, seizures, visual defect, altered sensorium, neck stiffness, and endocrine dysfunction. Most symptoms are related to hormonal abnormalities caused by hemorrhage or infarction.
Diagnosis of pituitary apoplexy is made with the use of MRI scans, testing of hormone levels, and vision testing. Treatment of an individual affected by pituitary apoplexy includes the high-dose corticosteroid administered at a rapid rate, diligent monitoring of electrolyte and fluid levels, and emergency transsphenoidal surgery.
Pituitary Adenoma
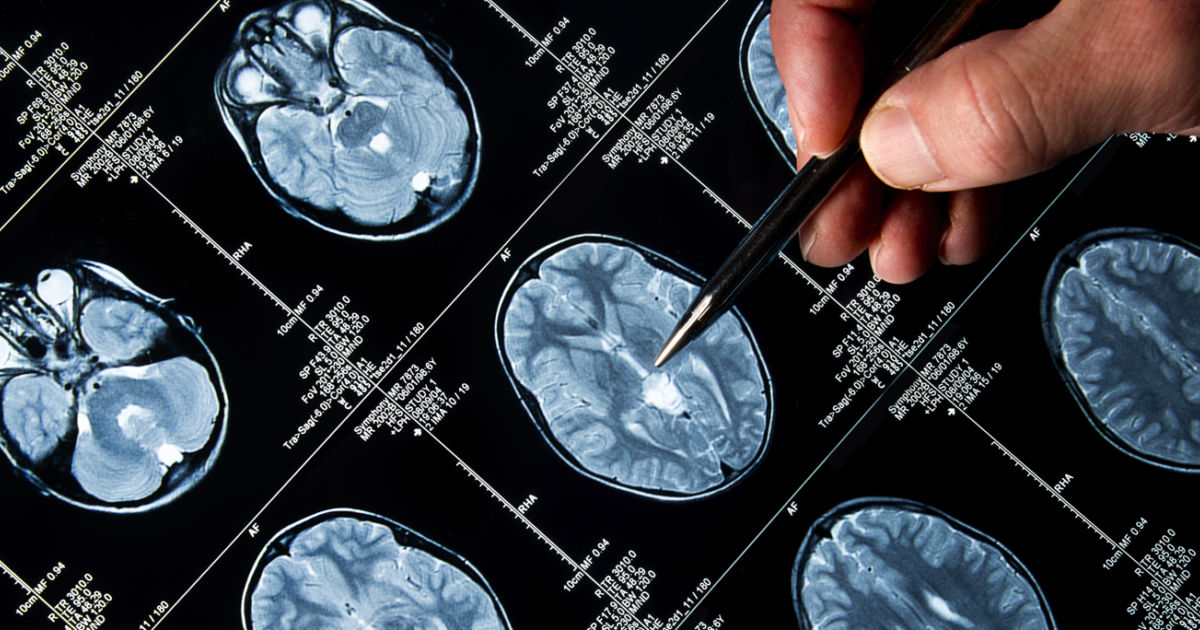
A pituitary adenoma is a noncancerous growth or tumor that develops in the pituitary gland. A pituitary adenoma may or may not produce an excessive amount of certain hormones. Although most pituitary adenomas are slow-growing, they can grow to a large size without causing patients to experience noticeable symptoms. A pituitary adenoma can cause pituitary apoplexy through one of two mechanisms. The first mechanism is associated with the damage and bursting of blood vessels in and around the tumor, producing a significant bleed. The blood from this bleed puts too much pressure on the tissues of the pituitary gland, producing the symptoms of pituitary apoplexy.
Another mechanism where a pituitary adenoma can cause a patient to have pituitary apoplexy involves the pituitary adenoma growing large enough to cause the death of a significant amount of tissue in the pituitary gland. This mechanism also produces a significant amount of pressure on and around the functional tissue of the pituitary gland.
Hypertension
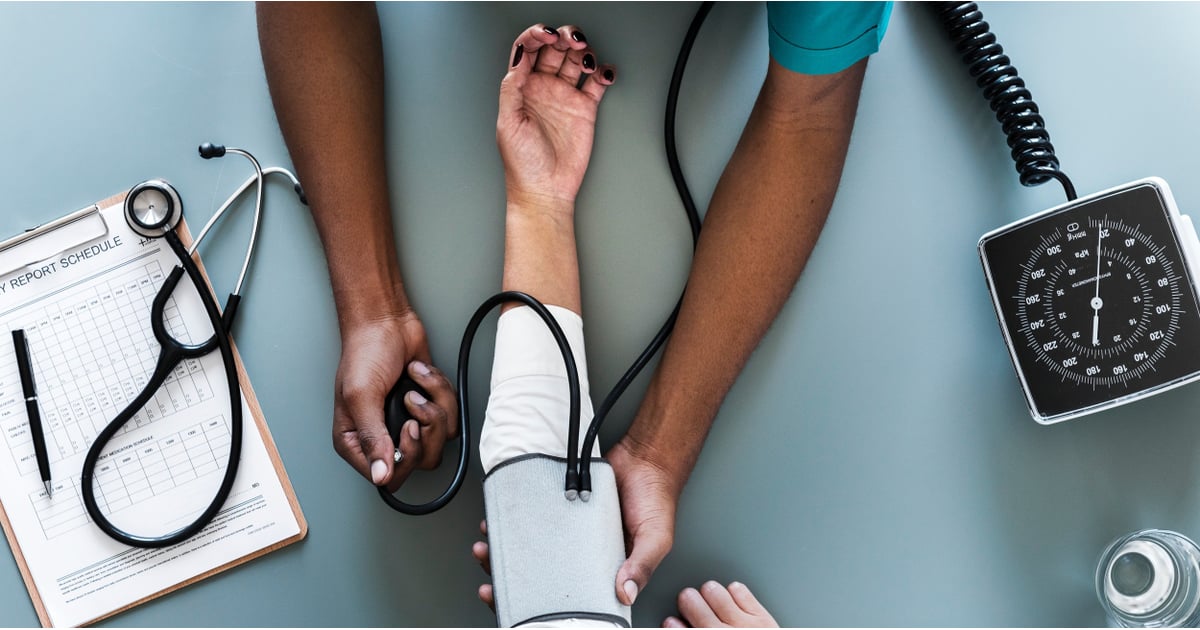
Individuals who have systemic long-term high blood pressure (hypertension) can experience pituitary apoplexy. Hypertension is a condition where the force of the blood against the walls of the blood vessels as it is moving through them becomes too excessive for the blood vessels to handle. Blood vessels are designed to expand with greater blood volume and pressure, but can only do so to a certain degree. Beyond the expansion ability of the blood vessels to cope with increased blood volume and pressure, damage begins to take place in the walls of the blood vessels.
This mechanism can take an immense toll on the smaller blood vessels around the body that weave their way through smaller structures such as the pituitary gland. While the exact mechanism of which high blood pressure causes an individual to experience pituitary apoplexy is not clear, it is thought to involve the damage that occurs in the small blood vessels that provide the pituitary gland with blood. Hypertension causes degenerative alterations in the microvasculature in the pituitary gland tissue, leading to a bleed that causes pituitary apoplexy.
Major Surgery
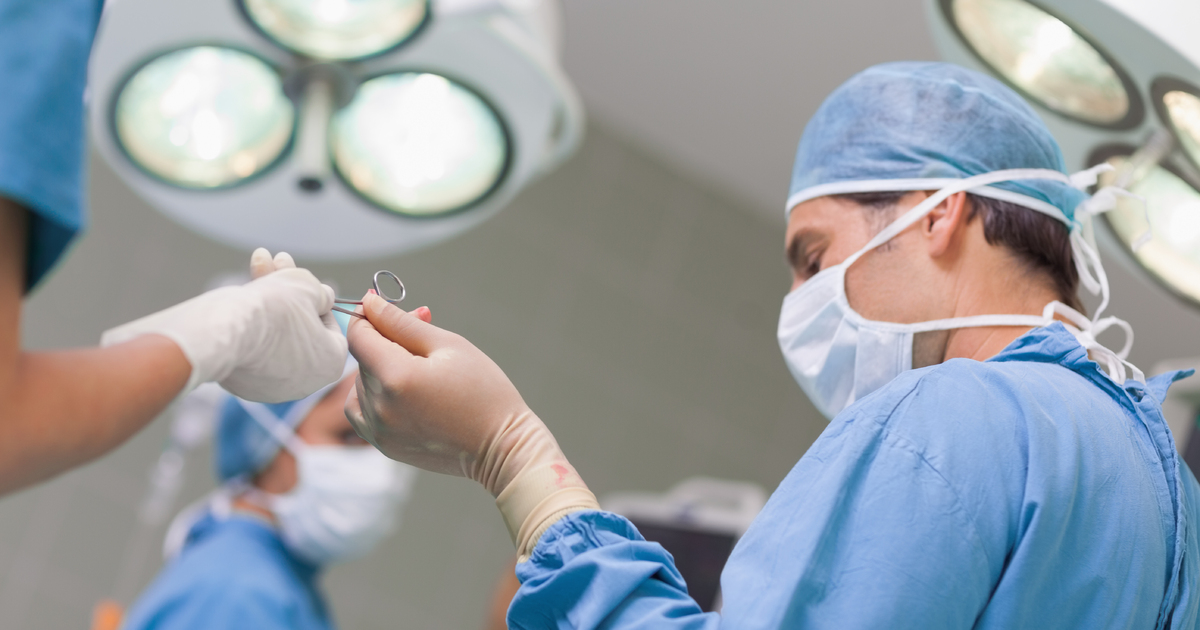
Any major surgical procedure can cause pituitary apoplexy due to surgical stress. Surgical stress describes when the injuries incurred to the patient's tissues during surgery can cause their sympathetic nervous system to become activated. The activation of the sympathetic nervous system produces hematological changes, immunological changes, and endocrine responses. These endocrine responses include an abnormal stimulation of the patient's pituitary gland that puts it under extreme pressure to produce excess amounts of steroids.
In most surgical environments, surgical stress is well managed by the anesthesiologist and surgical team, but this management is not always effective for each patient. Other surgical procedures can also produce pituitary apoplexy through different mechanisms that are the result of changes in the patient's blood pressure and intracranial pressure. These changes can produce a bleed that precipitates pituitary apoplexy. Such procedures include angiography, myelography, spinal anesthesia, pneumoencephalography, and lumbar puncture.
Certain Medications
Pituitary apoplexy can be induced due to certain medications as an adverse but severe side effect. Medications that increase the risk of bleeding excessively that are taken for frequent blood clots, hypercoagulability, heart disease, heart defects, high blood pressure, previous stroke, and high risk of stroke can also cause a bleed in the pituitary gland and neighboring tissues. These medications include anticoagulants, antithrombotic drugs, and thrombolytic agents.
Medications that cause an individual to have elevated estrogen such as birth control and medications for post-menopausal women can cause sudden changes in the pituitary gland tissue that may result in pituitary apoplexy. Certain medications that may be used when a patient undergoes a form of diagnostic testing referred to as dynamic pituitary gland testing can cause an overload of the pituitary gland. The medications known to produce this stressful condition that leads to pituitary apoplexy include thyrotropin-releasing hormone, bromocriptine, and gonadotropin-releasing hormone.
Radiation Therapy To The Pituitary Gland

An individual who experiences pituitary apoplexy may have had recent radiation therapy to the pituitary gland. Radiation therapy is a form of treatment where high energy beams of protons or x-rays are used to damage the DNA inside of cancerous or benign tumor cells to stop the tumor from growing and or reduce its size. During this type of treatment, precautions are taken to ensure the most precise concentration of the potent beams of energy. However, tissues that neighbor the area being treated with radiation therapy still incur damage.
Pituitary apoplexy has been caused by the death of tissues and the bursting of blood vessels that produce a bleed in the pituitary gland that has precipitated from radiation therapy. This particular cause of pituitary apoplexy usually only applies to pituitary adenomas being treated with radiation therapy that exhibit specific characteristics. Tumors with a high density of blood vessels and those considered very cystic are vulnerable to hemorrhagic necrosis-precipitated pituitary apoplexy.
