Guide To The Causes And Risk Factors For Venous Insufficiency
Venous insufficiency is a condition characterized by poor circulation and the pooling of blood in the legs. Healthy veins return blood from the legs and other areas back to the heart. With venous insufficiency, this process is impaired, and the amount of blood that reaches the heart is reduced. Patients with the condition frequently experience leg pain, cramps, swelling in the legs, and leg ulcers. Venous insufficiency is most common in patients over fifty years old, and it occurs more often in females than in males. To diagnose the condition, doctors will perform a physical examination, and patients may also have an ultrasound or a venogram. If venous insufficiency is diagnosed, doctors typically recommend patients wear compression socks to reduce swelling and improve circulation. Elevating the legs several times a day is beneficial, and patients are encouraged to avoid crossing their legs. Some patients may be prescribed diuretics or anticoagulants, and surgical interventions such as laser surgery or a vein bypass may be needed in severe cases.
Some of the major causes and risk factors for venous insufficiency are outlined below.
Varicose Veins
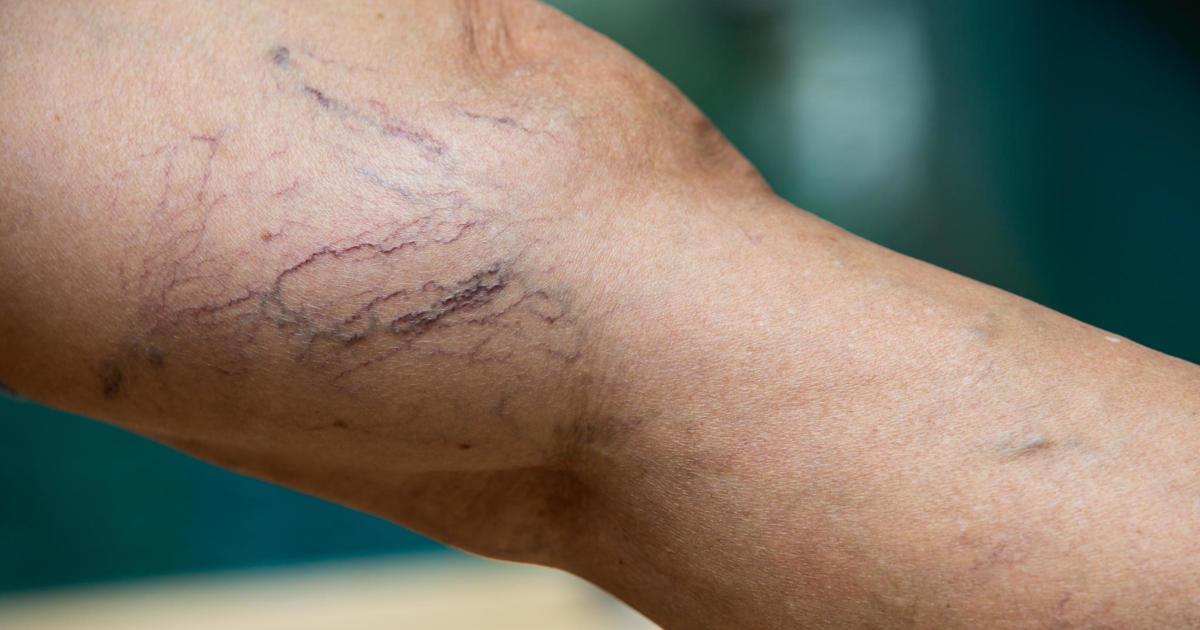
Varicose veins are clusters of swollen, tangled veins, and they often bulge above the surface of the skin. Although these veins can form anywhere in the body, they are most frequently found in the legs. The skin around varicose veins may show signs of discoloration, and itching could develop. Patients typically report burning or throbbing, and the pain may be worse after prolonged periods of sitting or standing. To diagnose this condition, doctors perform ultrasounds to find out more information about a patient's blood flow and the health of their veins. Compression socks can reduce the pain and swelling from mild varicose veins, and doctors also recommend regular exercise. If varicose veins significantly affect a patient's quality of life, surgical interventions might be considered. Many of these operations can be performed on an outpatient basis, and doctors might suggest sclerotherapy, laser treatment, endoscopic vein surgery, or vein stripping.
Get more details on the risk factors and causes linked to venous insufficiency now.
Blood Clots

Blood clots are gel-like, semisolid clumps of blood. If a clot forms in the lower legs, this could lead to venous insufficiency. Small clots may produce no symptoms, and some patients might only notice minor pain and swelling in the calf. Large clots could cause significant pain and increased swelling, and the affected limb might have a reddish discoloration. It could also feel warmer than the unaffected leg. A blood clot in the leg could break off and travel to the lungs or other parts of the body, and this could be potentially life-threatening. If any symptoms suggestive of a blood clot appear, patients should seek emergency medical attention. Doctors will perform blood tests and a specialized ultrasound exam to detect clots, and medication to dissolve the clot can be given at the hospital. Patients who have had previous blood clots may be placed on anticoagulants to reduce the risk of future clots.
Continue reading to reveal more causes and risk factors for venous insufficiency now.
Injury To The Legs

Patients may develop venous insufficiency after an injury to the legs. Broken bones are some of the most common injuries that result in venous insufficiency, and these typically occur as a result of falls, motor vehicle accidents, or blunt force trauma to the leg. Patients who have recently had major surgery on their legs could experience venous insufficiency as a surgical complication. To reduce the risk of injury to the legs, individuals should wear protective gear when participating in contact sports, and patients with limited mobility should use walking aids to reduce their risk of falling. While recovering from leg surgery, patients should let their healthcare team know about any swelling, redness, or pain in their legs. Anyone with leg weakness, walking difficulties, or leg pain should see a doctor for evaluation. Depending on the type of leg injury a patient has, doctors may choose to treat it by placing the leg in a cast. Serious leg injuries could require surgery.
Discover additional causes and risk factors for venous insufficiency now.
Obesity

Obesity is considered a possible risk factor for venous insufficiency. Patients with obesity may have difficulty with physical activity, and they are also more likely to have hypertension. Both physical inactivity and hypertension are recognized as additional risk factors for venous insufficiency. Under current guidelines, doctors define obesity as having a body mass index of 30 or above. Doctors may use waist circumference and measurements of body fat percentage to classify obesity as well. To treat obesity, physicians usually begin by recommending dietary modifications and increased physical activity. Patients will be encouraged to avoid fast food and saturated fat, and eating whole grains, fruits, and vegetables is suggested. Some individuals might want to meet with a nutritionist for help in designing healthy meal plans, and attending an exercise class or working with a personal trainer may help in improving activity levels. Doctors might consider prescribing medications for individuals who need help with weight loss, and surgical interventions could be suggested in certain cases.
Learn more about risk factors and causes linked to venous insufficiency now.
Standing Or Sitting For Long Periods

Standing or sitting for long periods without moving could trigger venous insufficiency. Patients may sit for extended periods while traveling or while working at an office job, and some occupations might require long periods of standing. To reduce the risk of venous insufficiency, doctors recommend that patients try to take a short, gentle walk at least once every thirty minutes. Performing leg stretches could also help encourage blood flow, and some of these can be done in a seated position. Individuals who must stay in bed due to illness will normally have physical therapy to move their legs while they are lying down, and they may also wear compression socks to promote circulation. If a job requires long periods of standing, it may help to change position every few minutes. Alternating between a standing position and a seated one could be beneficial as well. Patients who notice any pain, swelling, or other concerning or persistent changes in their legs after standing or sitting for an extended period should always let a doctor know.
