Common Causes And Risk Factors Of A Pneumothorax
Also known as a collapsed lung, a pneumothorax is generally considered a medical emergency. It can include a partial or complete collapse of the lung. As air leaks into the space between the lungs and the chest wall, it places pressure on the lung, leading to collapse. Symptoms of a pneumothorax include sudden onset chest pain and shortness of breath. To diagnose a pneumothorax, doctors will perform a chest x-ray. CT scans and ultrasounds may be helpful in confirming the diagnosis.
A small pneumothorax may be treated with observation. For a larger pneumothorax, medical personnel will perform a needle aspiration. In this procedure, excess air is removed through the insertion of a catheter between the ribs. If necessary, doctors may also need to insert a chest drain. This drain provides continuous removal of air from the chest cavity. Both of these procedures are performed in a hospital setting.
Cystic Fibrosis

Cystic fibrosis is a genetic condition that can increase the risk of a pneumothorax. Patients with cystic fibrosis have chronic lung infections, and as the disease progresses, it gradually limits their ability to breathe. Thick mucus forms in the lungs and patients may have a chronic cough, frequent colds, shortness of breath, and wheezing. They might also have persistent allergies throughout the year. Lung function declines slightly with each passing year, and symptoms increase as the patient ages. Cystic fibrosis can be diagnosed through routine newborn screening tests and genetic testing. Sweat tests and nasal lining measurements may be performed to aid in diagnosis.
To prevent a pneumothorax and other complications from this disease, doctors may recommend airway clearance therapy, mucus-thinning medication, antibiotics, and anti-inflammatory medication. Certain nutritional supplements can be beneficial too. Patients with this condition will be closely monitored by their medical team throughout their lives, and this may enable early detection of a collapsed lung and related conditions.
Chest Injury

A chest injury, both blunt and penetrating ones, is one of the most frequent causes of a pneumothorax. For example, knife or gunshot wounds, fractured ribs from physical assaults, and injuries sustained during automobile accidents may result in a pneumothorax. Patients who seek medical care after an assault or accident will be carefully evaluated to check for the presence of a collapsed lung.
Although less common, a pneumothorax may also develop due to an injury to the chest that occurs during a surgical procedure that involves inserting a needle into the chest. Surgeons are trained to minimize the risk of this complication, and the patient will be carefully monitored so the pneumothorax can be promptly corrected if it does occur. Patients who have experienced a collapsed lung are generally at an increased risk of having another pneumothorax within one to two years.
Mechanical Ventilation
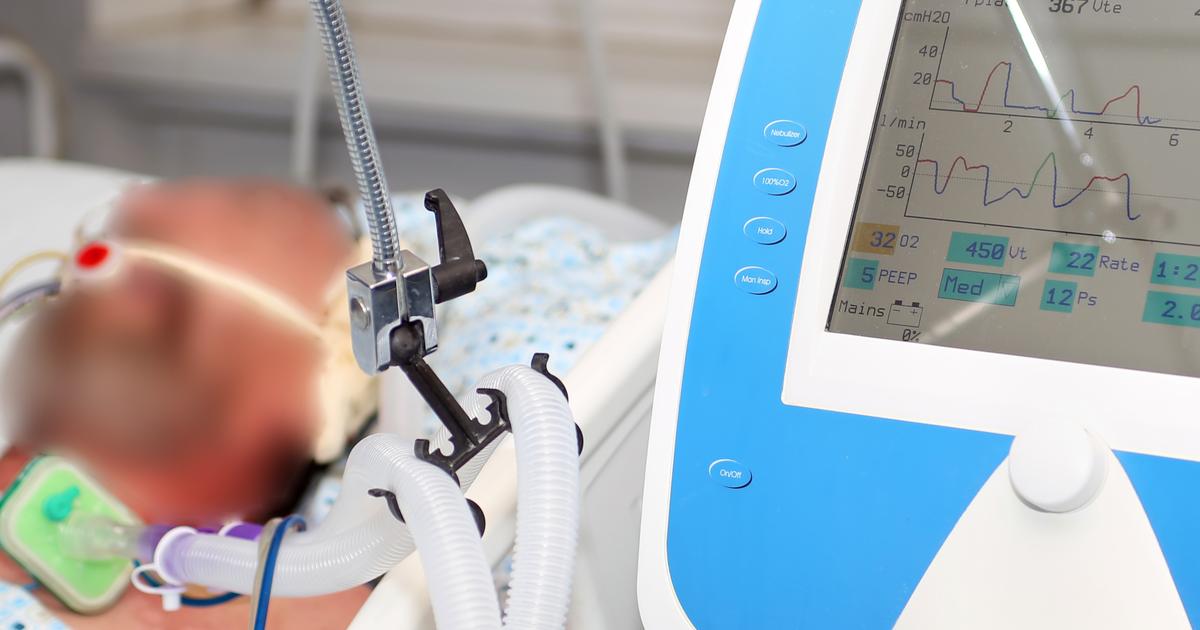
Mechanical ventilation, also known as assisted breathing, is a type of life support treatment. This form of ventilation breathes for the patient when they cannot breathe unaided. Mechanical ventilation is typically provided in intensive care units, and it helps transport oxygen into the lungs and the rest of the body. Before being placed on a ventilator, a doctor must place a tube into the patient's windpipe, a process known as intubation. Ventilation does not cause pain, and patients are carefully monitored while they undergo assisted breathing.
Nurses and other medical staff will frequently check the patient's blood pressure, pulse, and oxygen saturation. Sometimes, however, the use of mechanical ventilation may create an imbalance in the air pressure inside the chest. This could trigger a severe type of pneumothorax that results in the complete collapse of the lung. To reduce the risk of this issue, most patients on ventilators are given periodic chest x-rays, which enable doctors to detect this complication and provide appropriate treatment.
Ruptured Air Blisters
Air blisters, also known as blebs, may sometimes form at the top of the lungs. If these rupture, air could leak into the surrounding space, triggering a pneumothorax. Ruptured air blisters occur most frequently in men between the ages of twenty and forty, particularly in those who are taller than average and underweight. Air blisters are also common in patients who have emphysema. To treat air blisters, doctors may need to perform surgery. Using general anesthesia, surgeons can carry out a bleb resection, which is typically performed with a thoracoscope, a small camera that enables visual inspection of the inside of the chest.
Through a series of small incisions, doctors dissect the blebs and staple them before removing the tissue. With the affected tissue removed, the patient's healthy lung will have more room for expansion. After the procedure, patients will have a chest drain inserted, and this usually remains in place for a couple of days. Once the patient is discharged, they will have physical therapy sessions to encourage healing.
Chronic Obstructive Pulmonary Disease

Chronic obstructive pulmonary disease (COPD) is a lung disease that damages and weakens the lungs. This condition is considered one of the major causes of pneumothoraxes. Patients with COPD may experience wheezing, chest pressure, coughing, shortness of breath, and fatigue. They may be unable to exercise due to their symptoms. Some patients could also develop swelling in the ankles and feet, and unintended weight loss may occur in the later stages of this illness.
To treat this condition and reduce the risk of complications, doctors may prescribe bronchodilators to relax the muscles near the airways. Inhaled steroids and combination inhalers can help to reduce the inflammation associated with COPD. Some patients may need to take antibiotics, and oxygen therapy and pulmonary rehabilitation are typically recommended for patients with moderate to severe forms of this condition.
Pneumonia

An individual affected by pneumonia may develop secondary spontaneous pneumothorax as a complication. More cases of secondary spontaneous pneumothorax precipitated by pneumonia have been reported in children than in adults. The form of pneumonia known to cause pneumothorax is bacterial pneumonia. Pneumothorax can occur due to pneumonia that developed when the streptococcus bacteria, staphylococcus bacteria, and other types of bacteria colonize in the patient's lung tissues.
A pneumothorax can develop when fluid begins to build up between the pleura and chest wall as a result of the quantity of fluid present inside of the lung tissues. When the pressure in the pleural space around the patient's lung becomes more than that of the air entering the air sacs in the lungs, the organ can collapse in on itself.
Smoking

A regular smoker of tobacco products is at a greater risk of experiencing pneumothorax than an individual who does not smoke. Males are around twenty-two times more likely to experience a pneumothorax than individuals who do not smoke, and females are around nine times more likely to experience a pneumothorax than those who do not smoke. Smoking regularly can cause forms of pneumothorax referred to as primary spontaneous pneumothorax and secondary spontaneous pneumothorax.
A regular smoker is more likely to develop lung cancer that can cause pneumothorax by stopping the alveoli from filling with air properly. Long term exposure to irritants can cause damage in the lung tissues that are repaired with fibrous or scar tissue. An individual who smokes tobacco regularly is also at an increased risk of developing this type of fibrosis or scarring in their lungs because of the exposure to harsh chemicals. All of these factors associated with regularly smoking tobacco products can cause a pneumothorax to develop.
Previous Pneumothorax

An individual who has been affected by a previous pneumothorax is at a higher risk of experiencing another pneumothorax than an individual who has never had one. The reoccurrence rate of pneumothorax is reported to be between fifteen and forty percent of individuals who have been previously diagnosed. An individual who previously had a secondary spontaneous pneumothorax is more likely to develop another occurrence than someone who was previously affected by a primary spontaneous pneumothorax.
The highest rate of pneumothorax recurrence is in cystic fibrosis patients. Some researchers have established an association between the presence of air blebs that have been precipitated by inflammation and the development of a pneumothorax recurrence in most patients who have previously had one. An individual who has had a previous pneumothorax and is a female between thirty and forty years old is at a greater risk of developing a severe type of pneumothorax referred to as catamenial pneumothorax.
Genetics

An individual who has certain genetic features or abnormalities may be at an increased risk of developing a pneumothorax. The gene associated with genetic pneumothorax is referred to as the FLCN gene. Currently, eight different mutations in the FLCN gene are known to increase an individual's chances of a primary spontaneous pneumothorax. The FLCN gene is responsible for providing an individual's body with the encoded instructions for how to make a protein referred to as folliculin.
Folliculin is a known tumor suppressor and also plays a significant role in rebuilding, reforming, and repairing tissues in the lungs that have become damaged. A shortage of this protein in states of inflammation can cause the development of air pockets in an affected individual's lungs that eventually rupture and leak air into the pleural space. Approximately forty percent of individuals affected by one of these eight FLCN gene mutations will go on to experience pneumothorax.
Age And Gender

An individual's age group and gender can put them at a higher risk of a pneumothorax than those in other age groups and of another gender. A primary spontaneous pneumothorax is most prevalent among individuals between fifteen and thirty-four years old. Children under ten years old can be at a greater risk of developing a pneumothorax if they are affected by certain conditions that include echinococcosis, foreign object inhalation, measles, and certain congenital malformations. A child may also be at an increased risk of developing a pneumothorax if they have a family member who has had a pneumothorax previously.
Men are more likely than women to experience a pneumothorax overall. Women who do develop a pneumothorax tend to be at least thirty years old, whereas men who develop a pneumothorax tend to be between twenty and twenty-five years old. An explanation for this discrepancy between genders and age groups may be associated with endometriosis-related pneumothorax that tends to occur later in the childbearing years.
