Diagnosing & Treating Acute Respiratory Distress Syndrome
Acute respiratory distress syndrome (ARDS) is a serious complication due to widespread inflammation of the lungs. The inflammation process causes fluid to leak into the tiny air sacs (alveoli) where oxygen exchange occurs. The fluid decreases the capacity for oxygen and carbon dioxide exchange across the alveolar capillaries. This leads to low oxygen and high carbon dioxide levels in the blood. As a result, tissues throughout the body are starved of oxygen and carbon dioxide levels build up in the blood. ARDS usually occurs in critically ill patients who are already hospitalized. The most common causes are sepsis (infection in the blood), pneumonia, inhalation of chemical agents or smoke, and burns. It has a thirty-five to fifty percent mortality rate.
Imaging
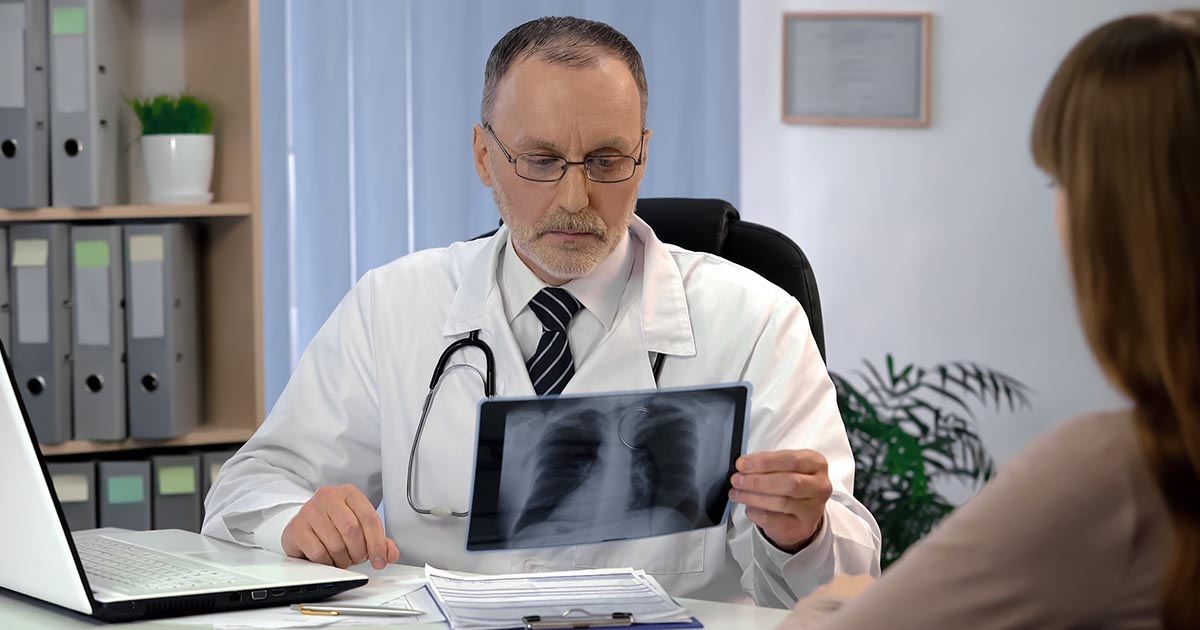
The diagnosis of acute respiratory distress syndrome requires meeting specific criteria. Experts established these criteria during a 2012 meeting in Berlin, Germany. The Berlin diagnostic criteria included rapid onset of breathing difficulties within seven days of the insult to the lungs, bilateral fluid accumulation in the lungs not explained by heart failure, and a PaO2 to FiO2 ratio below three hundred millimeters of mercury (indicating less oxygen in the blood).
Chest X-rays, CT scans, and ultrasound will be used to confirm bilateral pulmonary edema (fluid accumulation in the lungs). In acute respiratory distress syndrome, this fluid is described as a diffuse infiltrate. Fluid leaks from the capillaries that surround individual alveoli, filling the air sacs with liquid and making gas exchange difficult. Imaging studies will rule out other causes and help to determine the extent of disease.
Lab And Heart Tests

Congestive heart failure can also cause fluid to accumulate in the lungs and will need to be ruled out. In uncomplicated clinical cases, pleural effusions (fluid that accumulates between the pleural membranes), are seen in congestive heart failure but not in patients with adult respiratory distress syndrome. Lab and heart tests including an electrocardiogram can be used to look for cardiomegaly and valve problems. Cardiomegaly often occurs in congestive heart failure. An angiogram can be performed to insert a small pressure probe to test the pulmonary pressure. These tests will determine if the fluid accumulation is a result of heart damage and not ARDS.
Lab tests for acute respiratory distress syndrome include an arterial blood gas, complete blood count, sputum cultures, and blood cultures. Since two of the most common causes of ARDS are pneumonia and sepsis, identifying the pathogen causing the lung damage will be necessary to determine the correct treatment. In addition to these tests, a complete metabolic panel is often needed to look at the electrolytes, acid-base balance, and degree of dysfunction of major organs like the liver and kidneys.
Oxygen
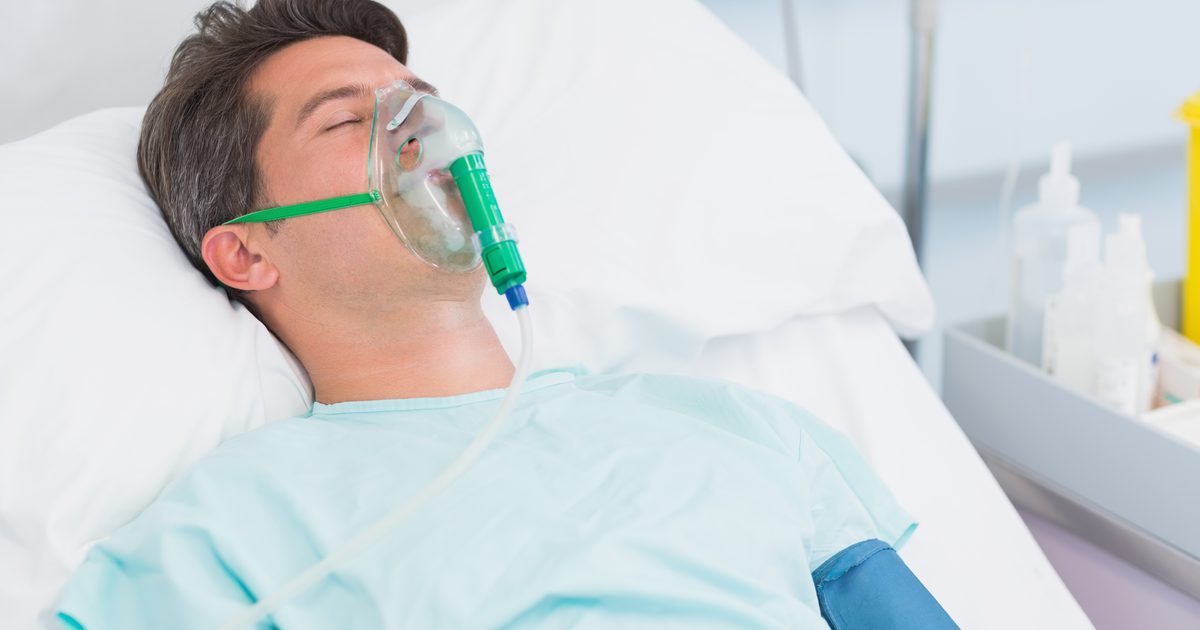
The criteria for an ARDS diagnosis includes three levels of disease depending on the PaO2 to FiO2 ratio. This ratio is the level of oxygen in the arterial blood compared to the fraction of oxygen in the inspired air. In mild acute respiratory distress syndrome, this is between two and three hundred millimeters of mercury. A Pa02/FiO2 of one to two hundred to millimeters of mercury is considered moderate ARDS, while less than one hundred millimeters of mercury is severe. Patients will need oxygen therapy matching the degree of disease.
In very mild cases, one hundred percent oxygen through a mask will be delivered. However, ventilator support is usually needed. In this case, oxygen will be delivered through a tube placed directly into the trachea and the machine will breathe for the patient. There is some evidence that lying face down can increase blood oxygen levels and may help the patient recover. Special beds in the intensive care unit of some hospitals can be used for this treatment. In addition to ventilator-delivered oxygen, there is another complex treatment in which the blood is oxygenated outside of the body. This treatment is referred to as extracorporeal membrane oxygenation (ECMO). Complications are common with this treatment, but it may be an option for some patients.
Fluids
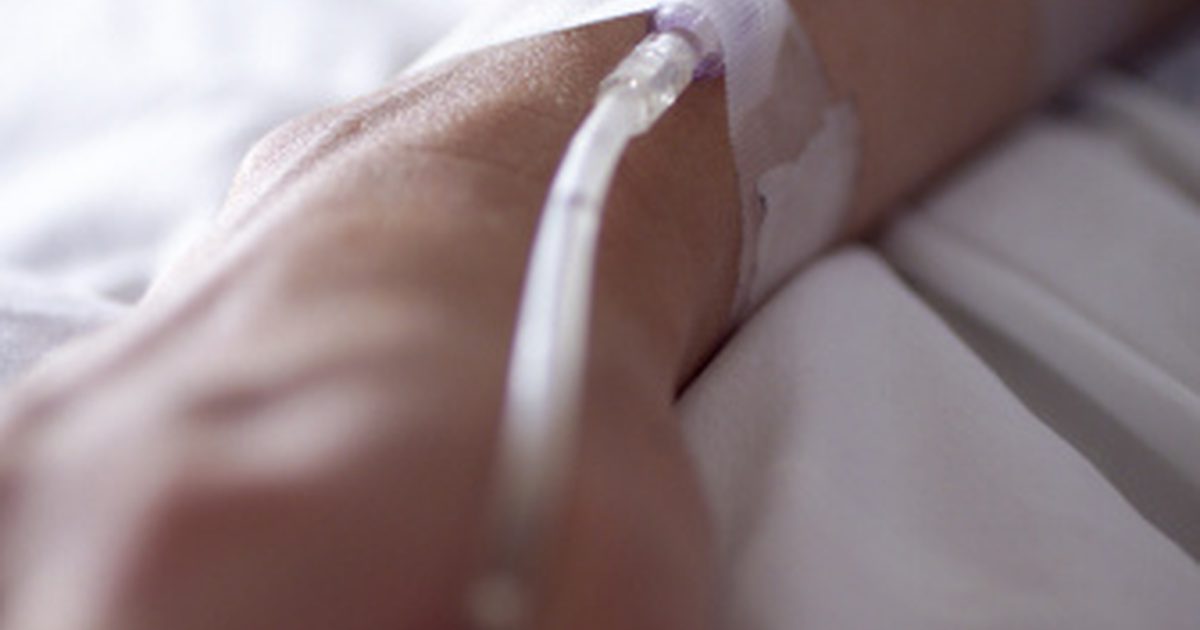
Managing IV fluids for patients with acute respiratory distress syndrome is challenging. The hypoxic patient will need sufficient fluid replacement to increase perfusion of the tissues, without increasing edema in the lungs. Early in the disease, adding fluid to increase tissue perfusion is recommended. If pulmonary edema worsens, fluids should be restricted. The use of diuretics to remove the fluid in the lungs is controversial since the fluid is primarily inflammatory exudates with a high protein content and little water.
Diuretics may also decrease cardiac output and reduce the oxygenation of tissues. Parenteral fluid therapy consists of crystalloids like five percent dextrose, blood products, electrolytes, and nutrient solutions. Hypertonic dextrose can be used to osmotically pull fluid from the lungs to permit better gas exchange. A feeding tube will be inserted for long-term nutrition.
Lifestyle And Home Remedies

Some patients recover completely from ARDS, and others will have lasting damage and health issues. Home remedies can be beneficial for many of these problems. Extreme fatigue and weakness are common after recovery, sometimes lasting months. Physical activity should be restricted during this time. Patients who have been seriously ill often become malnourished as well. A healthy diet during recovery can rectify this. Stopping smoking is one of the most effective lifestyle changes and home remedies for improving breathing ability. In addition to stopping smoking, avoiding second-hand smoke or other toxic fumes is important.
Allergens such as pollen, mold, and cat hair should be avoided or minimized. Alcohol use should be stopped or minimized, as it is associated with worse outcomes. Chronic alcoholism is also a predisposing factor for developing acute respiratory distress syndrome. Depression is common after a serious illness. A customized recovery regimen can reduce anxieties and assist in returning them to normal activities. Exercises to restore lung capacity can improve quality of life and has been shown to help alleviate depression.
