Everything You Should Know About Pulmonary Embolism
Although not many people are familiar with the term 'pulmonary embolism,' it occurs in more than two hundred thousand Americans each year. Prompt treatment is crucial for preventing the condition from becoming deadly. The condition tends to occur in people over the age of seventy years old. Taking precautions early in life by exercising and eating healthy is the best way to prevent a pulmonary embolism from occurring. Here is a short guide with all the necessary information about a pulmonary embolism.
Definition

A pulmonary embolism is one of the most common cardiovascular problems. It affects approximately one in every one thousand people in the United States alone. Derived from the Greek word émbolos, the term 'embolism' means 'plug' or 'stopper.' A pulmonary embolism occurs when a major blood vessel or artery in the lung suddenly becomes blocked by a blot clot. These blood clots may develop in other areas of the body and travel to the lung. In most cases, the blood clots are small and not life threatening, but they may cause severe damage to the lung. Larger blood clots can be deadly and require immediate treatment before the clot prevents blood flow to lung tissues. An embolus is not the same as a thrombus, which stays in one place after it is formed.
Causes
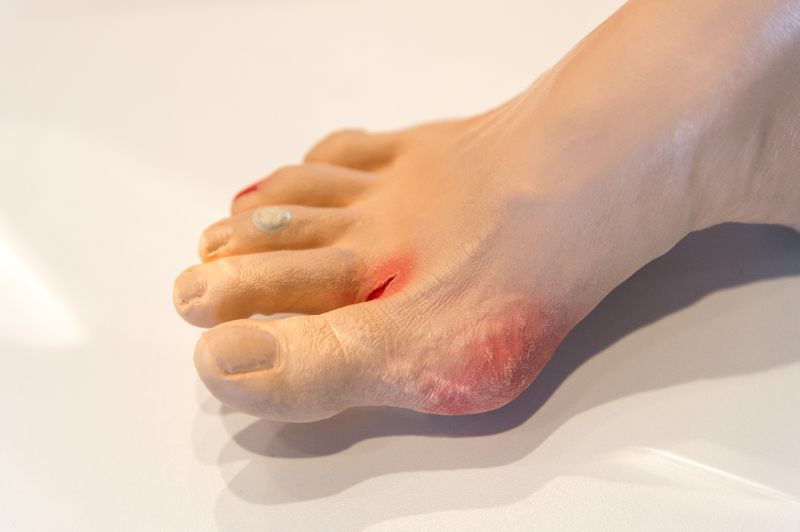
A pulmonary embolism is caused when a blood clot that begins in the legs or another part of the body breaks loose and travels to the lung where it causes a blockage of blood flow and oxygen to the lung tissue. Blood clots that occur in a vein that is located near the surface of the skin are not usually problematic. But when a blood clot occurs deep in veins, it may lead to a pulmonary embolism. People who have had a blood clot in their arm or leg are at an increased risk of developing a pulmonary embolism. Other rare factors that may cause an artery blockage include air bubbles, a tumor, amniotic fluid, and fat that is released into the bloodstream when there is a broken bone.
Symptoms
The most common symptoms of a pulmonary embolism include a sudden or sharp chest pain, especially when a person coughs or inhales. Chest pain can be confused with a heart attack; however, each condition requires immediate attention. Symptoms that may occur over time include rapid breathing or difficulty catchingthebreath; a dry cough; dizziness; and an increased, irregular, or rapid heartbeat. Other symptoms include shortness of breath even without physical exertion, such as during exercise or when climbing stairs, and a cough that results in a pink, foamy mucus. It is important to seek treatment at the first signs of breathing trouble or chest pain to determine whether the condition is life-threatening. Very severe cases may result in loss of consciousness, shock, cardiac arrest, and death.
Risk Factors

Some people are born with blood that clots too quickly, which increases the risk of developing a pulmonary embolism. Other risk factors include being inactive for extended periods of time, such as during a long car ride, or being bedridden after surgery or during pregnancy; recent surgery of the brain, hips, stomach or legs; certain diseases, such as heart failure, stroke, a severe infection, or cancer; or taking birth control or hormone therapy pills. Smoking and pregnancy may also increase the risk, especially if a woman has had a cesarean section. Being obese or over the age of seventy significantly increases the risk. Other risk factors include having a family history of blood clots, supplements that enhance estrogen, catheters in the veins, certain cancers, and receiving a diagnosis of inflammatory bowel disease.
Diagnosis

A pulmonary embolism is difficult to diagnose because many of the symptoms are similar to those of other conditions, such as a heart attack, pneumonia, or a panic attack. In most cases, a physician will begin by performing a physical examination and asking a patient a series of questions about his or her health and symptoms. The following tests are available to check for a pulmonary embolism: an electrocardiogram (EKG) to test the heart’s electrical activity, an arterial blood gas study to measure gasses in the blood, an X-ray of the internal organs, a pulmonary scan to analyze the ventilation and architectural structure of the lungs, an ultrasound, or a magnetic resonance imaging (MRI) scan. Other tests include a D-Dimer test, which is a blood test that can detect thrombosis, and a pulmonary angiogram to detect blood clots in the lungs.
Treatment

Most cases of a pulmonary embolism are treated by an anticoagulant medication or a blood thinner to prevent or reduce the blood clot. Blood thinners do not cause the blood to become thinner, but they may help to prevent new clots from forming and stop existing clots from getting bigger. People who are at a high risk of developing a pulmonary embolism may have to take blood thinners for the rest of their life whereas individuals with a lower risk may need to take them for only a few months. Some people are not able to take blood thinners and may need a vena cava filter to prevent a clot from reaching the lungs. Individuals who are exempt from taking a blood thinner include those who bleed easily or have atrial fibrillation.
Other Treatments
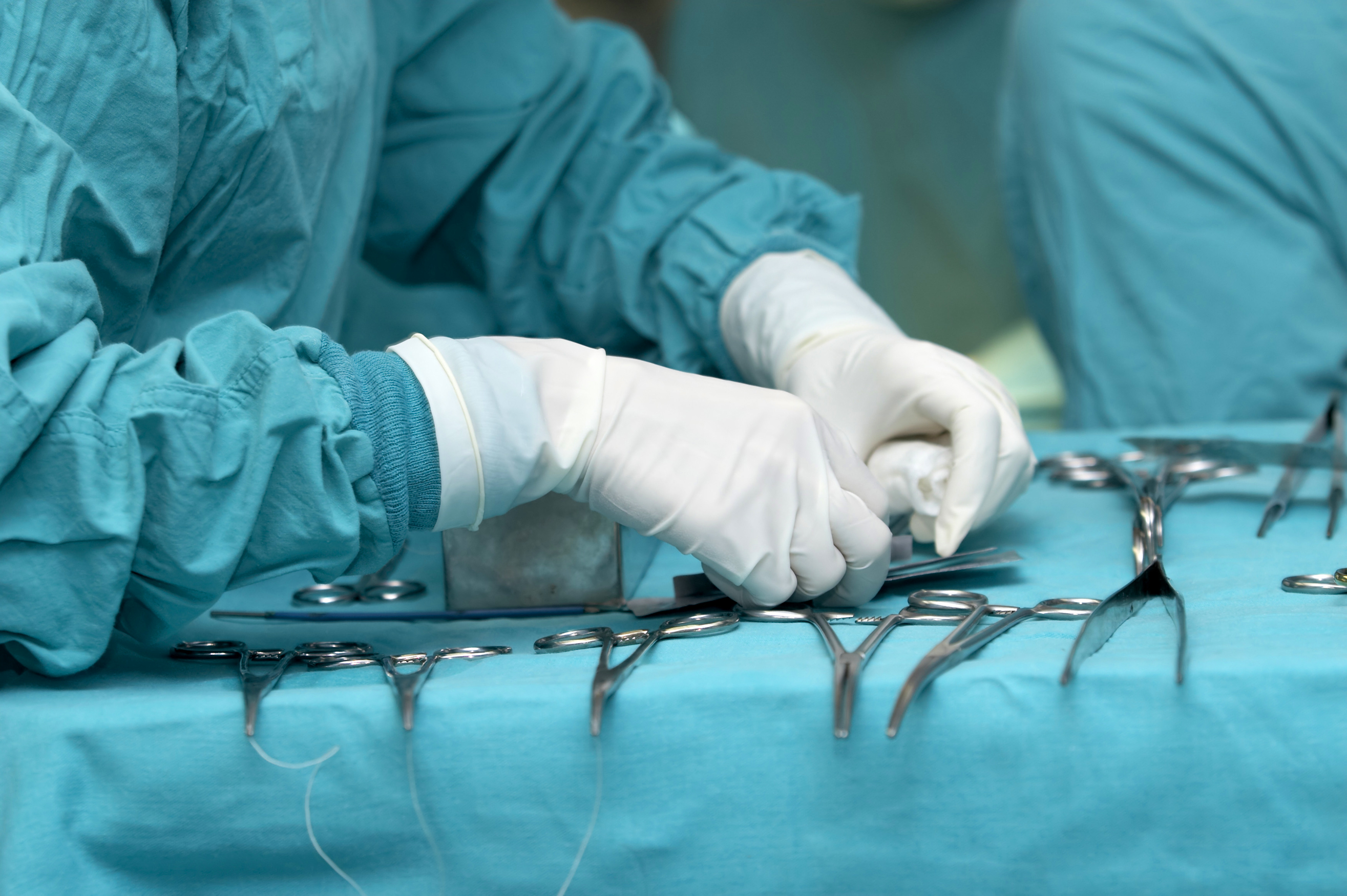
Treatment for an embolism aims to destroy or remove an existing blood clot, prevent new clots from forming, and keep the clot from growing. If a pulmonary embolism becomes severe or life threatening, a clot-busting drug known as a thrombolytic may be used to dissolve the clot quickly and restore oxygen and blood flow to the lung. Thrombolytic medications are highly effective, but they may also increase the risk of bleeding; therefore, they should not be taken by anyone who bleeds easily or has atrial fibrillation. Surgery is an option if a blood clot becomes dangerous. A minimally invasive procedure to remove the clot called an embolectomy is also available. If the patient has low blood pressure, dopamine may be administered to increase blood pressure. Patients usually need to take medications for at least three months to remove a clot.
Prevention Techniques

To prevent a pulmonary embolism, avoid sitting for extended periods of time. Stop and take a ten-minute walking break while on long road trips. If that is not possible, try flexing the feet often to get the blood moving. After a major surgery, ask to walk as soon as possible. Drinking lots of water will help circulate the blood. Avoid excessive caffeine or drinks with alcohol. Wearing compression socks may help if a person is at high risk. Be sure to take blood thinners as instructed by a medical professional. Avoiding or quitting smoking is also a good preventative measure to take. In addition, wearing an inflatable glove, sleeve, or boot may be used to hold the affected area and increase pressure where needed.
Diet And Exercise
Maintaining a healthy weight and participating in a healthy exercise program is an excellent way to prevent a pulmonary embolism. Avoid processed sugars and carbohydrates, and eat a diet high in anti-inflammatory foods, such as fruits, vegetables, wild-caught fish, flaxseeds, and nuts. Try cooking at home in place of eating out to gain greater control over the diet. Certain foods and herbs, such as watermelon, cinnamon, turmeric, and ginger, are great for decreasing inflammation and promoting circulation. Check with a doctor before beginning an exercise program. It may help to start slow by walking for thirty minutes three times a week. Gradually incorporate weight resistance training to build lean muscle and increase blood flow. Consult with a trainer for tips on how to properly lift weights.
