Guide To The Most Common Bacterial Infections
A bacterial infection is a term used to describe when a certain type of foreign microorganism enters an individual's body and causes damage to their tissues. An organism may use the affected individual's body to reproduce, colonize, and sustain itself. Other types of microorganisms that can cause infection in the body include viruses, fungi, protozoa, and parasites. Different pathogens have different shapes, sizes, functions, impacts on the body, and genetic content. Bacteria are organisms considered single-celled and may be referred to as prokaryotes in the medical community. An individual's body naturally contains many types of bacteria that are helpful to the organs and their functions that do not cause any harm. However, an invasion of foreign bacteria or the overgrowth of natural bacteria in the body can produce damage to the tissues or an infection. Different types of bacterial infections affect different parts of an individual's body.
Pneumonia

Pneumonia is an infection that develops in the lungs. Bacterial pneumonia develops when the Streptococcus pneumonia, Hemophilus influenzae, staphylococcus aureus, Streptococcuspyogenes, Klebsiellapneumoniae, Moraxella catarrhalis, or Neisseriameningitidis bacteria invades the tissues of an individual's lungs. Bacterial pneumonia is more likely to develop in individuals who have a compromised immune system whereas viral pneumonia is more likely to develop in a healthy individual. Symptoms of bacterial pneumonia include productive cough with green, bloody, or yellow mucus, sudden chills or shakes, a fever of between 102 and 105 degrees Fahrenheit, chest pain that worsens when breathing or coughing, muscle pains, headache, rapid breathing, breathlessness, pale skin, appetite loss, sweating, confusion, and lethargy. Diagnosis of bacterial pneumonia is made with the use of physical examination, blood testing, sputum culture, and chest x-rays. Bacterial pneumonia is treated with the use of antibiotics to kill the type of bacteria that has produced the infection and supportive measures like intravenous fluids, respiratory therapy, and pain medication.
Otitis Media
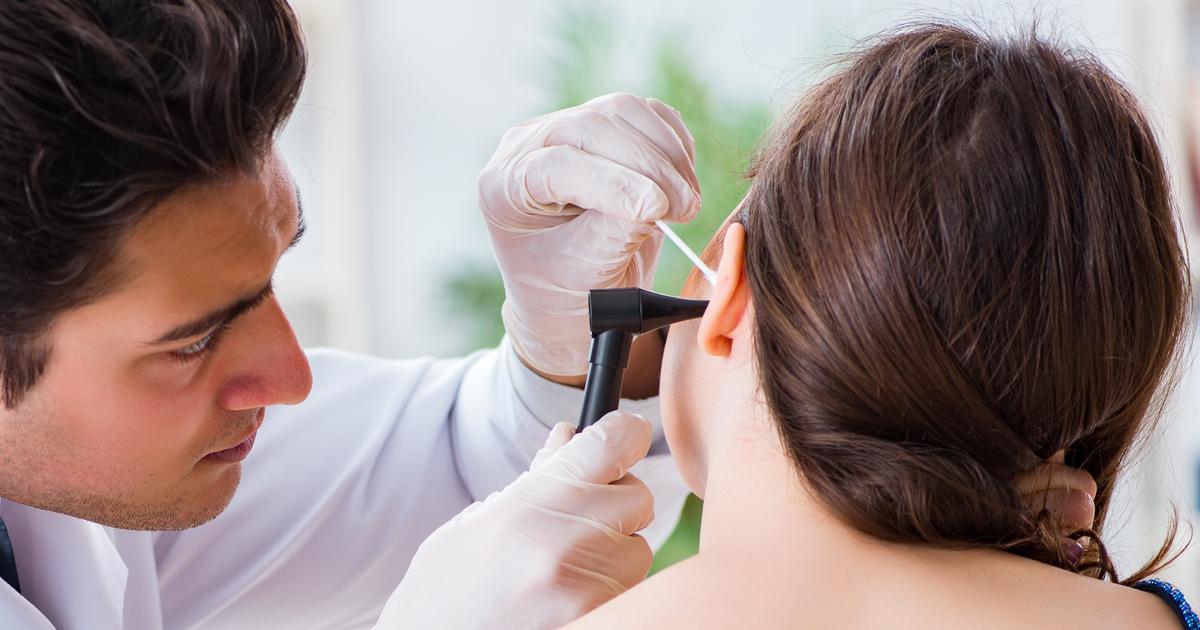
Otitis media develops when an individual's eustachian tubes become inflamed and swollen due to some mechanism that produces an accumulation of fluid in the middle ear. The flu, a cold, allergies, sinus infection, adenoid infection, and cigarette smoke are the most common causes of trapped fluid in the middle ear. This fluid is a hospitable environment that allows pathogens like bacteria to thrive. The most common types of bacteria to cause otitis media include Streptococcus pneumoniae, Moraxella catarrhalis, and Hemophilus influenzae. Symptoms of bacterial otitis media include ear pain, neck pain, fluid drainage from the ear, fever, diarrhea, vomiting, balance problems, hearing loss, feelings of pressure inside of the ear, headache, sleeplessness, and irritability. Diagnosis of otitis media is made with the use of a physical examination and tests with medical devices that include an otoscope, tympanometry, and reflectometry. A hearing test may also be used in otitis media diagnosis. Bacterial otitis media is treated with the use of antibiotics, pain medication, and in some cases, surgery.
Food Poisoning

Food poisoning and foodborne illness are terms used to describe when microorganisms from contaminated food or drink are introduced to an individual's stomach and cause tissue damage. This introduction of pathogens to the stomach is most commonly caused by incorrect food handling or contamination during production and or processing of food. The most common types of bacteria implicated in food poisoning are salmonella, shigella, Clostridium difficile, Campylobacter, and Escherichia Coli. Symptoms of food poisoning include nausea, vomiting, abdominal pain, abdominal cramping, fever, bloody or watery diarrhea, appetite loss, and chills. Some individuals who have food poisoning progress to the point of being dehydrated as a complication of their infection. The onset of symptoms depends on the specific type of bacteria that is causing food poisoning. Diagnosis of food poisoning is made with the use of a physical examination, blood tests, and a stool culture. Treatment for bacterial food poisoning includes the use of antibiotics, intravenous electrolytes, and intravenous fluids.
Sinusitis

Sinusitis is a condition where the paranasal sinus cavities in an individual's skull are invaded by a pathogen that causes damage to the lining of the sinuses. Sinusitis develops when some mechanism causes the linings of the sinus channels to become swollen and inflamed, leading to the accumulation of fluid in the sinus cavities. Swelling of the sinus channels is most commonly caused by a virus, allergies, swimming, or a tooth infection. The blocked sinus cavities are a stable environment for bacteria to thrive and reproduce, causing the development of sinusitis. Individuals affected by bacterial sinusitis experience symptoms such as pain in the face, nasal congestion, post-nasal drip, upper jaw pain, yellow or green nasal discharge, fever, cough, feelings of pressure or fullness in the ear, headache, and a decreased ability to smell. Diagnosis of sinusitis is made with the use of physical examination, nasal cavity endoscopy with or without culture, sinus endoscopy with or without culture, and CT scan. Sinusitis is treated with the use of antibiotics to kill the causative bacteria, nasal saline rinses, and pain medication.
Urinary Tract Infections

A urinary tract infection is a condition involving the pathogenic invasion of an individual's urinary tract or urethra, bladder, ureters, or kidneys. The most common causes of bacterial introduction to the lower urinary tract include the prolonged use of urinary catheters, abnormal urinary structure, weakened immune system, kidney stones, incomplete emptying of the bladder, enlarged prostate, spermicide use, sexual intercourse, and diaphragm use. The most prevalent types of bacteria to cause urinary tract infections are Escherichia coli, Klebsiella species, Pseudomonas aeruginosa, Proteus species, and Enterococcus species. Symptoms of a urinary tract infection include cloudy urine, bloody urine, strong-smelling urine, pain during urination, burning during urination, frequent urge to urinate, nausea, vomiting, abdominal pain, and muscle aches. Urinary tract infections are diagnosed with the use of urine tests, urine culture, and in some recurrent cases, ultrasound, CT scan, X-rays, MRI scans, radiation tracking, urodynamics, and cystoscopy. Urinary tract infections are treated with antibiotics to eliminate the causative bacteria, the consumption of extra fluids, and pain medication.
