What Causes A Hemothorax?
When a hemothorax occurs, blood can be found in the pleural space around the lungs. This blood may be coming from the chest wall, lung, heart, or blood vessels. In many cases, a hemothorax remains a result of an injury. A hemothorax must be treated immediately to avoid serious medical consequences. Blood in the thorax region is usually accompanied by excess air around the lungs. So treatment may involve removing both blood and air from the body using a tube inserted into the chest between the ribs. Get to know the various causes of a hemothorax in great detail with this article.
Blunt Force Trauma To The Chest

In many cases, a hemothorax occurs due to an injury or blunt force trauma to the chest. This trauma causes blood to collect in the pleural cavity, which is in between the chest wall and the lungs. Once the blood enters the pleural cavity, it can only be removed by a medical procedure. Even a tiny injury can cause bleeding to happen in the chest wall and lungs and cause a hemothorax. A hemothorax due to trauma may also cause the pleural space to rupture. If an individual has blunt force trauma due to a car accident, altercation, or sports injury, their lungs need to be inspected for possible damage and bleeding.
Improper Blood Clotting
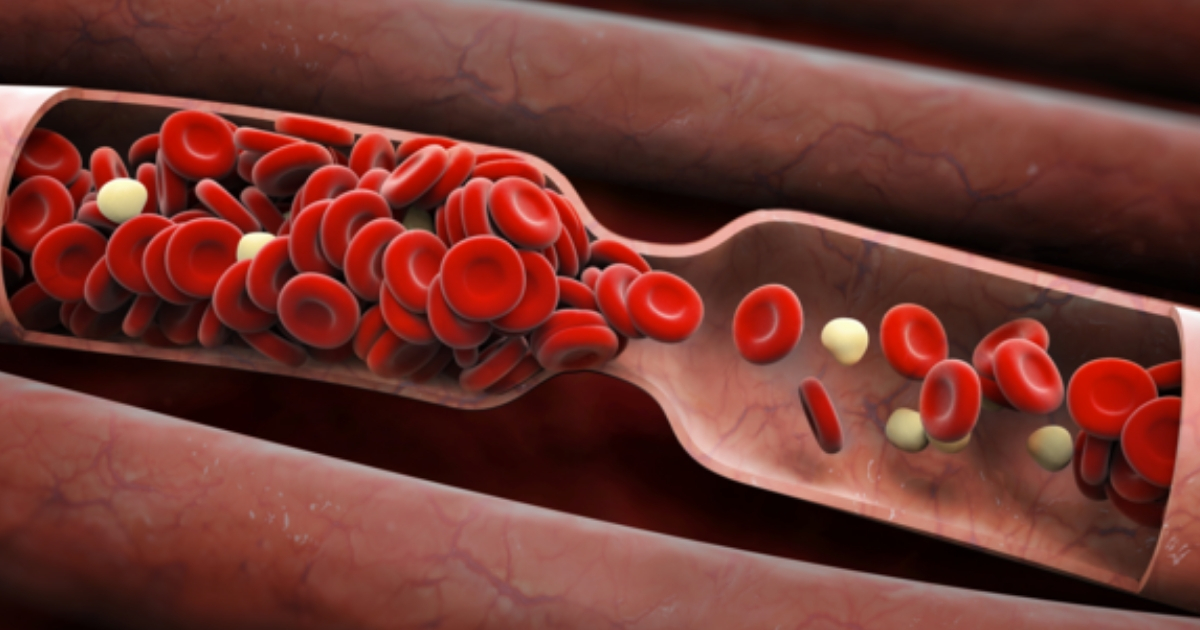
A spontaneous hemothorax can occur in individuals with improper blood clotting issues. Individuals who develop a spontaneous hemothorax may experience symptoms such as chest pain and life-threatening dyspnea. A spontaneous hemothorax may be more likely to happen in patients who take anticoagulant medications or who have hemophilia. A hemothorax may also occur when a plasminogen activator is used for venous thrombosis in pneumonia patients too. Glanzmann thrombasthenia is a genetic disorder that causes clotting abnormalities, which may lead to a hemothorax. Other blood clotting disorders may lead to improper clotting of the blood and hemothorax issues.
Ehlers-Danlos Syndrome

Ehlers-Danlos syndrome is a group of inherited connective tissue disorders. Individuals with Ehlers-Danlos syndrome tend to bleed and bruise easily. The gene COL3A1 is the underlying genetic mutation that effects procollagen production and synthesis. Ehlers-Danlos syndrome can come on quite suddenly and medically catastrophic, so immediate treatment is needed. The condition brings on a hemothorax, arterial dissection, or colon rupture and rapid bleeding. Ehlers-Danlos syndrome should be quickly managed by surgery on the affected area. However, the patient’s health should be stabilized as much as possible before any operation is performed.
Pulmonary Infarction

Pulmonary infarction is tissue death in the lungs because of a lack of oxygen-rich blood. In the case of such an infarction, a portion of lung tissue dies because the blood supply to this area has been blocked. In most cases, a pulmonary embolus causes the blockage of blood to a part of the lungs. Symptoms of pulmonary infarction include chest pain, shortness of breath, back pain, coughing up blood, sweating, and dizziness. If the pulmonary embolus is small, patients may experience few to no symptoms. But if the embolus is massive, more severe symptoms may occur, and these include fever, extreme shortness of breath, chest pain when inhaling, and feeling faint or weak. The leading cause of a pulmonary infarction remains a blood clot in the lungs (pulmonary embolus). Other reasons may be encountered, including infections, inflammatory lung diseases, torsion of the lungs, cancer, and a nonthrombotic embolism. A pulmonary infarction remains a serious condition that needs immediate treatment by a qualified doctor.
Malignant Pleural Effusion
Malignant pleural effusion occurs as a result of the development of cancer. This pleural effusion remains a collection of fluids between the visceral and parietal layers surround the lung. Patients with malignant pleural effusion tend to get the disorder towards the end stages of cancer. The pleural fluid naturally moves through the space of the pleural lining of the lungs. When more fluid is produced than absorbed in this lining pleural effusion occurs. The malignant tumor may be causing blocking the flow of pleural fluid around the lungs, or a tumor may obstruct a thoracic duct. Malignant pleural effusion can come from such cancers as breast cancer, adenocarcinoma of the lung, ovarian cancer, mesothelioma, and advanced lymphoma. Patients with malignant pleural effusion are somewhat hard to diagnose, though chest x-rays, thoracic ultrasounds, and CT scans help determine a diagnosis as well as tests such as protein levels, lactose dehydrogenase levels, and pleural fluid LDH levels.
