Guide To The Symptoms Of Kearns-Sayre Syndrome
Kearns-Sayre syndrome is a rare genetic disorder caused by problems with the mitochondria, a component found in all the cells of the body. First discovered in 1958, scientists estimate the syndrome occurs at a rate of 1.6 out of every 100,000 individuals. Individuals with this condition normally appear healthy at birth, and symptoms gradually appear during childhood and adolescence, typically beginning before the age of twenty. Kearns-Sayre syndrome patients may have vision difficulties, hearing loss, short stature, heart problems, and diabetes or other endocrine system disorders. Genetic testing can be done to diagnose Kearns-Sayre syndrome, and patients may also need to have an eye exam, blood tests, MRI scans, and specialized heart tests to fully evaluate the severity of their symptoms.
Treatment is tailored to the symptoms an individual is experiencing. For example, patients who have heart problems may need a pacemaker, and individuals with vision difficulties may wish to have surgical intervention. All Kearns-Sayre syndrome patients are closely monitored by specialists, and they typically have regular hearing tests, eye exams, blood tests, and electrocardiograms to check for the development of potential complications. The symptoms produced by Kearns-Sayre syndrome can vary in severity, and they are often different from individual to individual.
Pigmentary Retinopathy
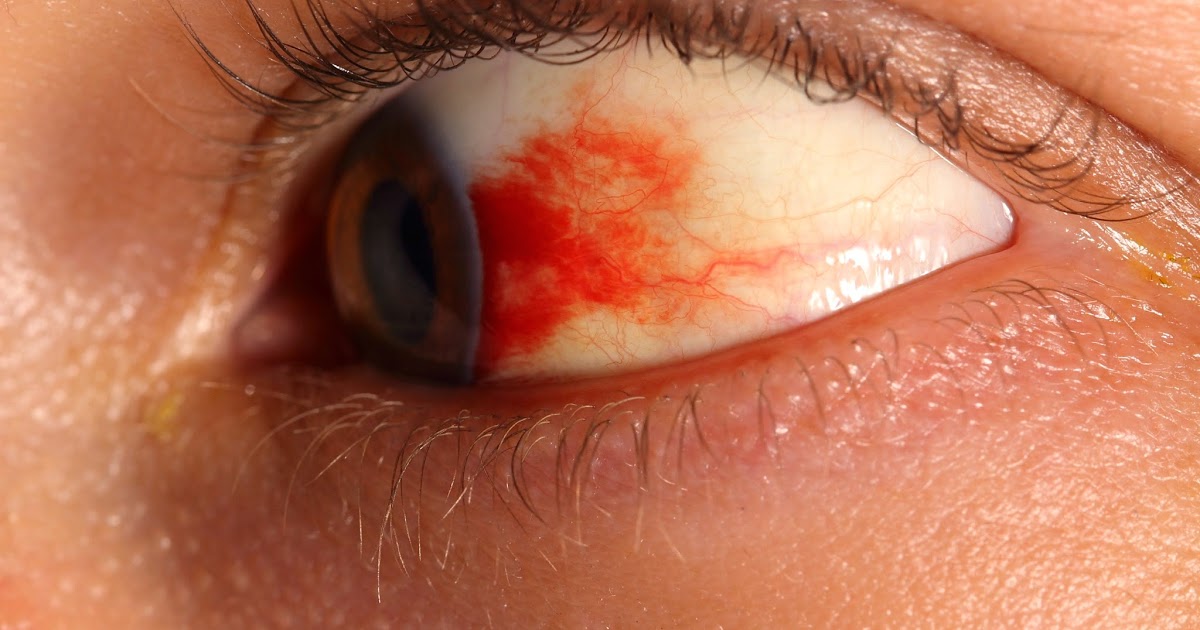
Pigmentary retinopathy is an eye condition that affects between eighty to ninety-nine percent of patients with Kearns-Sayre syndrome, and the presence of pigmentary retinopathy is often used as part of the diagnostic workup. Retinopathy itself refers to damage to the small blood vessels in the retina, the part of the eye that receives images and senses light. In pigmentary retinopathy, the breakdown of the tissues of the retina causes it to become streaked or speckled. While retinopathy can cause vision loss and lead to blindness, the majority of patients with pigmentary retinopathy usually have intact vision, although they may have less than perfect visual acuity. Retinopathy can cause eye pain, decreased peripheral vision, and blurry or double vision.
To diagnose pigmentary retinopathy, an ophthalmologist examines the eye with an ophthalmoscope. Mild retinopathy may not require immediate treatment. In moderate to severe cases, laser treatments and medication injected into the eye may be beneficial. Patients with Kearns-Sayre syndrome should have a yearly eye exam with an ophthalmologist to monitor their retinopathy and any other eye symptoms they may be experiencing.
Ptosis
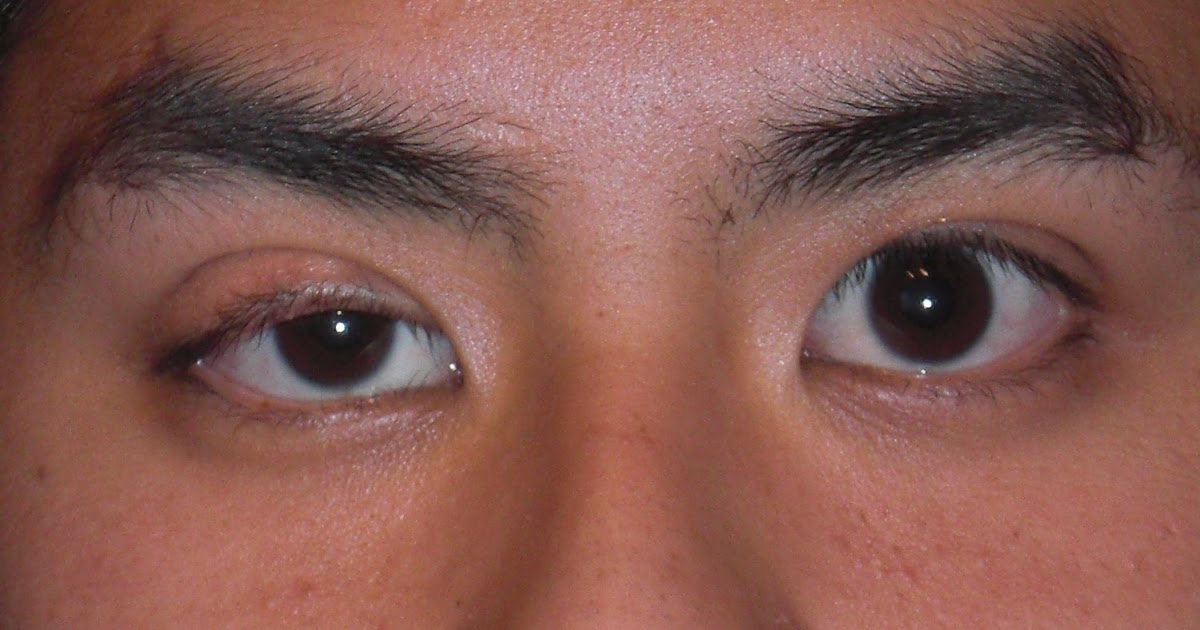
Ptosis refers to the drooping of the upper eyelid, and it can affect either one or both eyelids. For patients with Kearns-Sayre syndrome, ptosis is normally caused by progressive external ophthalmoplegia, a condition that impairs eye movement and weakens eye muscles. As a progressive condition, this type of ophthalmoplegia worsens over time, eventually resulting in complete paralysis of the eye muscles and an inability to move the eyes.
The ptosis associated with Kearns-Sayre syndrome may begin as a slight droop, and it can progress until the upper eyelid almost completely covers the eye. Surgical intervention to tighten the muscles that lift the eyelids may be helpful for some cases of ptosis, and patients with Kearns-Sayre syndrome may wish to ask their eye doctor about additional treatment options for their particular situation.
Cerebral Folate Deficiency

Cerebral folate deficiency is a symptom in which there is a lower than normal level of 5-methyltetrahydrofolate in a patient's cerebrospinal fluid. Patients with Kearns-Sayre syndrome who have a cerebral folate deficiency may struggle with coordination, and they may have developmental delays, speech difficulties, and cognitive impairments that appear similar to autism. This deficiency could also cause seizures and low muscle tone for some patients. Symptoms associated with a cerebral folate deficiency typically begin within the first year of a patient's life.
To detect this type of deficiency, patients will have a lumbar puncture (spinal tap) performed to obtain a sample of cerebrospinal fluid for testing. If a cerebral folate deficiency is confirmed, supplementation with high doses of folinic acid for a prolonged period has been shown to be effective as a treatment option. Patients with this deficiency are normally assessed and treated by a neurologist.
Cardiac Conduction Deficits
Cardiac conduction deficits are especially common in patients with Kearns-Sayre syndrome, and the severity of the deficits often varies for each patient. Also called a heart block, a mild form of cardiac conduction deficit occurs when the two uppermost chambers of the heart beat normally, but the two lower chambers beat slightly later than they should. For patients with more severe heart blocks, only twenty-five to fifty percent of the heartbeats from the upper chambers are transmitted to the lower chambers of the heart. In the most severe form of heart block, also known as complete heart block, the upper and lower chambers of the heart beat separately from each other.
These types of cardiac conduction deficits can cause syncope, shortness of breath, and arrhythmia, and they also increase a patient's risk of sudden cardiac death. To evaluate these deficits, cardiologists generally perform electrocardiograms, echocardiograms, and other specialized heart tests. Patients will need to have these tests repeated at regular intervals to check for potential complications, and some patients may need medication or surgery to treat arrhythmias.
Cerebellar Ataxia
Cerebellar ataxia refers to coordination difficulties that originate in a part of the brain known as the cerebellum. In patients with Kearns-Sayre syndrome, this type of ataxia often results in poor balance, walking difficulties, and problems with the coordination of other voluntary movements such as crawling, writing, and eating. Some patients also have swallowing and speech difficulties, and certain reflexes might be absent.
To assess the extent of cerebellar ataxia, clinicians will perform a neurological exam to check reflexes, gait, balance, sensation, and coordination, and MRI scans or other imaging studies may also be performed. Patients who have cerebellar ataxia may benefit from physical therapy, occupational therapy, and the use of adaptive devices to make walking and other tasks easier.
