Guide To Treating Chronic Pancreatitis
Chronic pancreatitis is a progressive disease of the pancreas and causes the pancreas to lose its function and structure permanently. The pancreas is found in the abdomen, below the ribcage, and behind the stomach. It is responsible for the production of various hormones and enzymes required for the proper digestion of foods. The pancreas produces insulin or a hormone that regulates and manages the levels of glucose in an individual's blood. Chronic pancreatitis is most often the result of repeated occurrences of acute pancreatitis, which happens when there is premature activation of trypsin in the pancreas. Trypsin is a digestive enzyme that is meant to stay inactive until it reaches the small intestine. In acute pancreatitis, trypsin activates and begins to digest the pancreas itself. This mechanism results in chronic irritation and inflammation of the pancreas that damages it and causes chronic pancreatitis.
Get the details on treating chronic pancreatitis now.
Pancreas Resection
Severe cases of chronic pancreatitis may require a patient to undergo a pancreas resection to treat severe chronic pain. The head of the pancreas becomes severely inflamed and causes the patient to experience intense pain. In a pancreas resection, the pancreas head is removed to alleviate the inflammatory pain irritating the endings of the nerves. A pancreas resection also decreases any pressure on the ducts.
There are three primary methods used for a pancreas resection. The Beger procedure is a method where the head of the pancreas is removed, and the duodenum is spared. The remaining portion of the pancreas is then attached to the intestine. The Frey procedure is a method intended for patients experiencing pain from blocked ducts and an inflamed pancreatic head. The head of the pancreas is removed, and the ducts are attached directly to the intestines to decompress them. A pylorus-sparing pancreaticoduodenectomy is a type of resection that involves the removal of the ducts, gallbladder, and pancreas. This procedure is reserved for the most severe cases of chronic pancreatitis where the ducts are blocked, and the pancreatic head is very inflamed.
Learn more about how to treat chronic pancreatitis now.
Endoscopic Stent Replacement
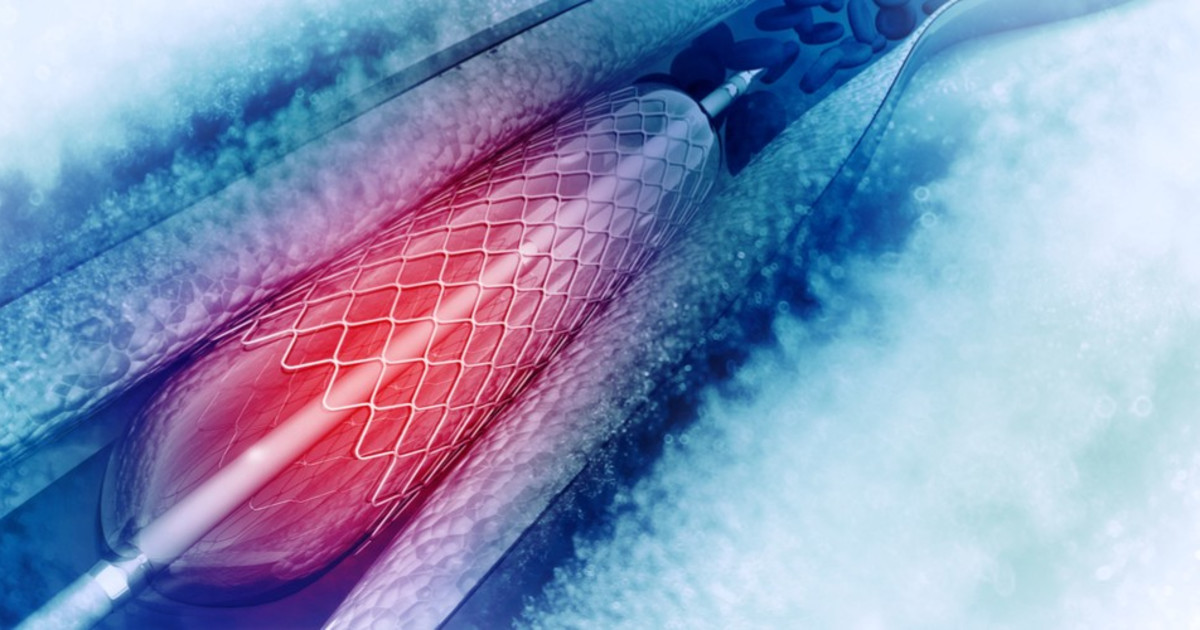
An accumulation of digestive juices in the pancreas may put pressure on ducts that have become blocked, resulting in intense pain. When the pain a patient is experiencing is caused primarily by this mechanism, an endoscopic stent replacement procedure may be needed. This procedure involves the use of ultrasound technology to help guide the surgeon operating the endoscope to the blocked duct. Once the endoscope reaches the blocked duct, a balloon catheter is threaded into the endoscope and to the duct. The surgeon then inflates the balloon on the end of the catheter inside of the duct, effectively widening it. A medical mesh stent is then placed into the duct around the balloon to hold it open. The balloon is deflated, and the stent is left in the duct to prevent it from becoming narrowed again. An endoscopic stent replacement surgery is minimally invasive and carries less risk of complications than traditional open procedures used to widen ducts.
Discover more treatment methods for chronic pancreatitis now.
Autologous Pancreatic Islet Cell Transplant
An autologous pancreatic islet cell transplant is a procedure that involves the infusion of the patient's own islet cells into the liver's portal vein. This procedure is only necessary for patients who have pancreatitis that has destroyed most of their pancreatic tissues and deemed the organ non-functional. A pancreatectomy procedure is performed to extract the damaged and diseased pancreas. The removal of the entire pancreas can provide considerable relief to individuals with severe chronic pancreatitis, but it results in an unavoidable complication of type 1 diabetes. The autologous pancreatic cell transplant was designed to mediate this complication by providing a way for the patient's body to make insulin in the absence of the pancreas. This procedure works to accomplish this by infusing the islet cells from the removed pancreas so they become lodged in the liver blood vessels. Once in the blood vessels, the islet cells are activated and produce insulin. Because this is an autologous transplant, there are zero risks of tissue rejection involved. This procedure does not always prevent diabetes after a pancreatectomy, but it does increase the chances of having a milder form of diabetes.
Read more about treating chronic pancreatitis now.
Consume Smaller Meals

Individuals affected by chronic pancreatitis are often advised to consume smaller meals. The pancreas is responsible for the production of certain enzymes necessary for the proper digestion of food. Chymotrypsin and trypsin are produced by the pancreas to break down proteins. Lipase is produced to break down fats, and amylase is produced to break down carbohydrates. All of these enzymes are combined and sent down the common bile duct, where bile joins them. The combination of bile and enzymes then moves into the small intestine where they are all utilized to break down the different components of food. Chronic pancreatitis patients have a reduced function of their pancreas, which means it cannot produce these enzymes very well. The digestive system may have trouble digesting a larger meal due to the fact the pancreas is not providing enough of these enzymes collectively at one time. It is easier on the patient's inflamed pancreas to eat six smaller meals a day, instead of three larger meals.
Learn more about the best options for treating chronic pancreatitis now.
Shift To A Low Fat Diet

Chronic pancreatitis patients may be advised to shift to a low-fat diet as part of their treatment regimen. This diet restriction is to reduce general pancreatic and digestive inflammation and to prevent an acute flare-up. Any food cooked in oil or grease, such as fast food and fried food, should be avoided entirely. Full fat meat, dairy, and creamy sauces are also common suspects of pancreatic inflammation. Foods such as white bread, anything with a significant amount of high fructose corn syrup, and high in sugar should be avoided. Processed meats and canned foods have ingredients that are unhealthy for the pancreas. The reason for these restrictions in the diet for chronic pancreatitis patients is due to their increased sensitivity to foods that are already difficult for even a healthy individual to digest, like fatty foods. Fatty foods can push the pancreas to overwork itself and produce more enzymes than it is able to in order to digest the food. This mechanism may even result in an overproduction of enzymes that do not leave the pancreas before they become activated. When enzymes are activated before they make it to the small intestine, they begin to digest whichever structure is nearest to them.
