Treatment Methods For An Iron Deficiency
An iron deficiency refers to an abnormally low level of iron in the blood. Symptoms that can indicate a possible iron deficiency include fatigue, dizziness, fast heartbeat, pale skin, shortness of breath, and brittle nails. Tongue swelling, a tingling sensation in the legs, and unusual cravings for non-food items such as ice or clay may be additional signs of this condition. Iron deficiency affects individuals of every age group, though females who have menstrual periods or are pregnant are at an increased risk. The condition can be caused by several underlying conditions such as anemia, endometriosis, kidney failure, or celiac disease and may also result from internal bleeding or the use of blood thinners. The treatment methods detailed below may help individuals recover from an iron deficiency.
Iron Supplements

Iron supplements are available over the counter, though individuals must speak with a pharmacist for access in most cases, and patients should work with their doctors to set an appropriate dose for their needs. Typically, daily dosages of one to two hundred milligrams are recommended. Doses should be spread throughout the day rather than being taken all at once for maximum absorption. Some extended-release tablets are available, and these can be taken once per day. Iron supplements should not be taken with caffeine, calcium, antacids, or milk and other dairy products, as these can reduce absorption levels. Doctors often encourage patients to take iron with foods or drinks that contain vitamin C, including whole oranges or orange juice, or even vitamin C supplements to increase absorption. Side effects of consuming too many iron tablets include dark stools, heartburn, constipation, and upset stomach. To minimize stomach upset, patients can choose to take their iron pills with a meal. Most patients take these supplements for at least six months after their iron levels are normalized.
Continue reading to reveal the next method of treating an iron deficiency.
Consume Iron-Rich Foods

Patients are often advised to consume iron-rich foods to return iron levels to normal as quickly as possible. Doctors recommend women between nineteen and fifty years old consume eighteen milligrams of iron daily. Women over fifty and men nineteen and older should aim for eight milligrams of daily iron consumption. Kidney beans, pumpkin seeds, spirulina seaweed, tofu, oysters, brown rice, lentils, molasses, whole wheat bread, spinach, peanut butter, fortified cereals, and turkey are all high in iron. Patients who struggle with an iron deficiency, particularly if it is long-lasting, may wish to consult a nutritionist for specialized advice about ways to incorporate more foods with high iron into their diet. Iron consumption can be tracked using many online applications, and patients can also do this using a food diary if they do not have regular computer access.
Get to know the next option for treating an iron deficiency now.
Treatment For An Underlying Condition
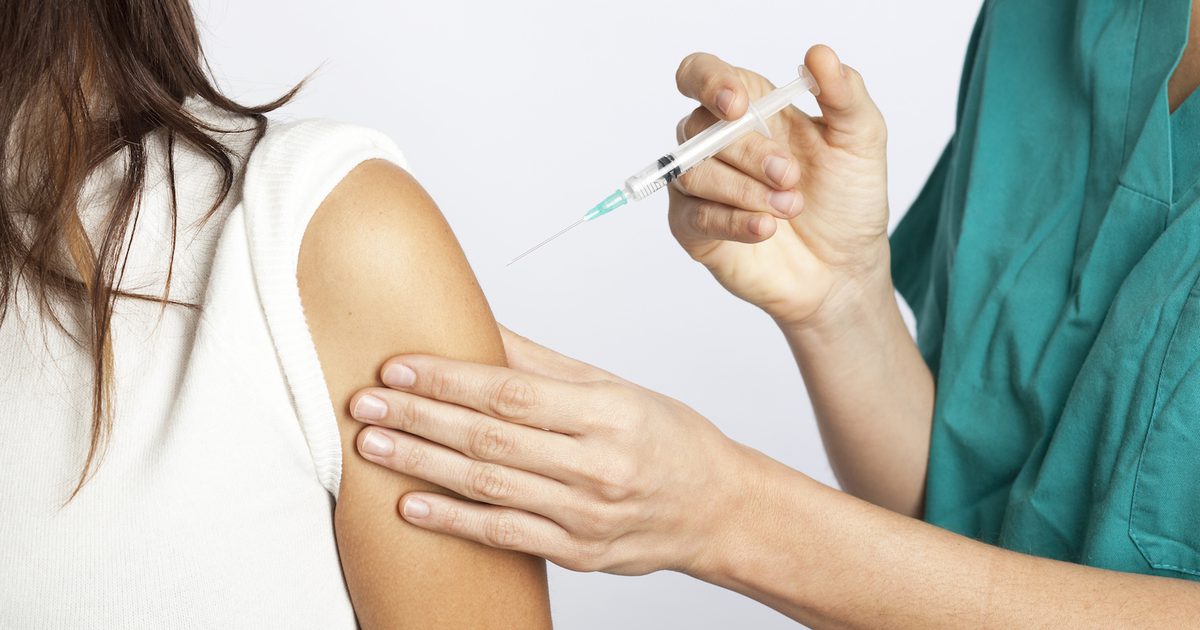
While some cases of iron deficiency may result from poor diet alone, the majority of cases occur due to an underlying condition. Treatment for an underlying condition can help restore normal iron levels and improve the patient's quality of life. Anemia, which results is the most common condition that causes low iron levels. It results from low red blood cells. In addition to iron supplements, patients with anemia may need vitamin B12 injections or blood transfusions to correct the issue.
Women are especially likely to have an underlying condition that causes low iron. Worldwide, twenty-nine percent of non-pregnant females and thirty-eight percent of pregnant women have low iron counts. While women with normal to light periods are generally able to maintain healthy iron levels, those with regular heavy bleeding often have insufficient levels. Women may wish to consider taking birth control or using other methods their primary doctor recommends to light their periods. Endometriosis patients can also have low iron as the condition causes heavy bleeding. Treatment for endometriosis may involve surgery.
Unearth the next option available for treating an iron deficiency now.
Intravenous Iron Infusion
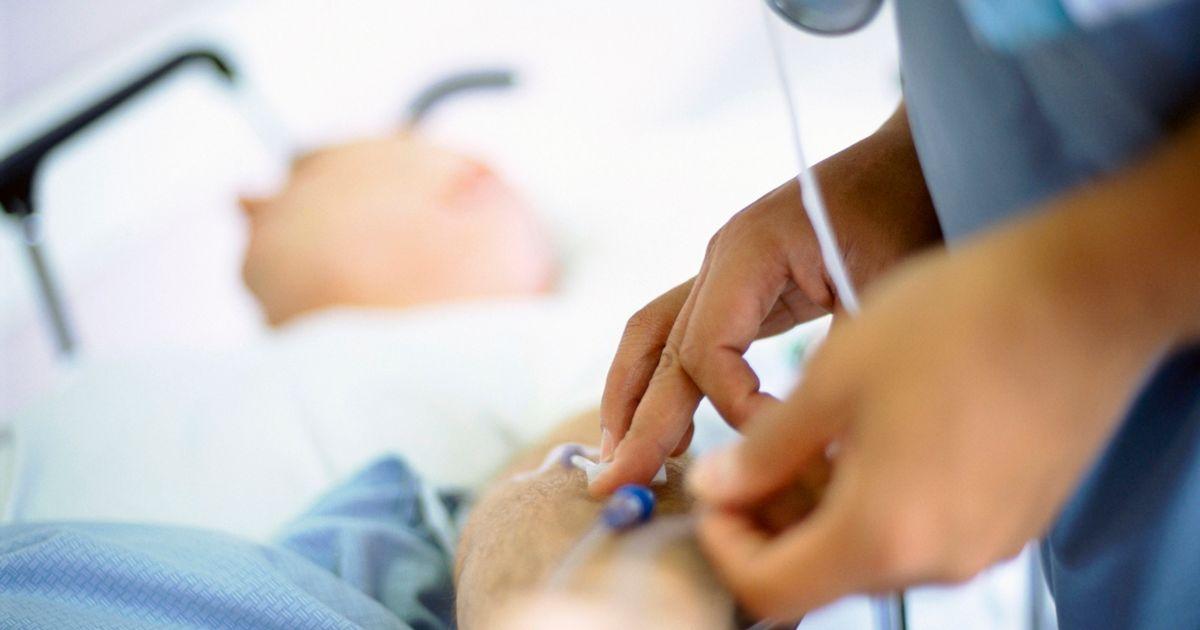
Intravenous iron infusions can help patients who cannot restore normal iron levels with oral supplements and iron-rich diets increase their levels quickly and avoid further complications or the need for blood products. Intravenous iron is typically recommended for patients experiencing low iron due to blood loss. It is also appropriate for individuals who cannot take oral iron and those who cannot absorb sufficient iron through their gut. Iron infusions are often given in a hospital or at a dialysis center, usually take three to four hours, and the mineral is infused slowly to prevent side effects and adverse reactions. Patients remain seated throughout the infusion. Several infusions may be needed to restore normal iron levels.
Side effects of the infusions include rash, temporary changes in the way food tastes, nausea, muscle pain, and changes to heart rate and blood pressure. Most patients find they have increased energy after receiving an infusion and that it is easier to breathe. For some patients, iron infusions can maintain normal iron levels for several years. Iron injections are sometimes used for patients who cannot take infusions.
Learn more about the treatments for an iron deficiency now.
Blood Transfusion

Blood transfusions are a last resort and are generally only offered if other more conservative treatments have failed. They are often essential for patients with chest pain and other severe complications from low iron levels. Several different blood products are available for transfusion. Iron-deficient patients receive transfusions of red blood cells. Before their transfusion, patients have a blood test to determine their blood type so a compatible transfusion can be obtained. Transfusions are given with an IV placed in the arm and can take between one to four hours to complete.
Throughout the transfusion, nurses will periodically check the patient's heart rate, blood pressure, and temperature. Although rare, potential side effects that may occur during a transfusion include fever, chills, a sense of uneasiness, shortness of breath, pain in the back or chest, and itching, all of which should be reported to medical staff immediately. Following the transfusion, a bruise may form at the IV site and remain for a few days. Patients should watch for any shortness of breath or chest and back pain in the week after the transfusion and report these to their doctor.
