Methicillin-resistant Staphylococcus Aureus (MRSA): Prevention and Treatment
Methicillin-resistant Staphylococcus aureus (MRSA) is a type of bacterial infection. These bacteria are resistant to many antibiotics so successful treatment can be tricky, and a proper match has to be made. Individuals affected by this unfortunate condition may not know right away because the infection can start out as something as common as a minor sore, pimple, or boil, and develop from there. This type of superbug can potentially lead to serious conditions or death.
Symptoms Of Infected Blood

Symptoms of methicillin-resistant Staphylococcus aureus can be similar to other conditions when the blood is infected by contaminated bacteria, so proper diagnosis is required. A patient with MRSA may experience chills alternating with a high fever of at least 100.4 degrees Fahrenheit. A general feeling of malaise may be present, as well as dizziness, confusion, muscle aches, swelling, chest pains, coughing, breathlessness, headaches, a rash, or persistent wounds.
Symptoms Of Nasal And Skin Infections
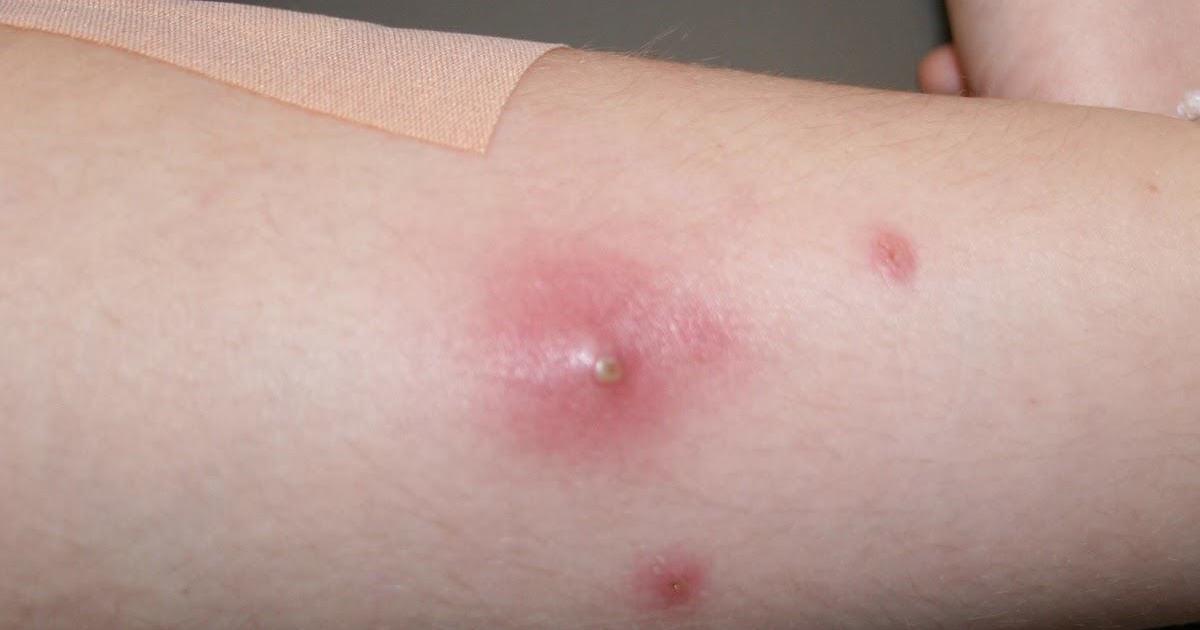
Since the bacteria that causes MRSA can affect various areas of the body, the symptoms will vary. When the nasal mucosa is contaminated, there may be no symptoms. With staph skin infections, it is easy to mistake the resulting bump or irritation for a bug bite. The skin might appear red, inflamed, and sore. It may radiate warmth and be filled with pus. A skin infection could also produce a fever.
Causes
Antibiotic Resistance As A Cause

Some health professionals cite antibiotic resistance as a cause of MRSA. As its name suggests, methicillin is an antibiotic and is a relative of penicillin. Once it could be used successfully against staphylococci bacteria, but a strain of these bacteria became resistant to the antibiotic. Now, the bacteria not only resists methicillin and penicillin but oxacillin and amoxicillin as well. Because these antibiotics are used so often to treat other types of Staph infections, MRSA has become sometimes very difficult to treat. Health professionals believe the Staphylococcus aureus bacteria became resistant because antibiotics have been overused and overprescribed. Though the drugs killed off weaker bacteria, it did not kill stronger bacteria. These stronger bacteria went on to reproduce and are now able to survive the antibiotics in the methicillin family. This is called antibiotic resistance.
Health Care-Associated MRSA

Facilities like hospitals, clinics, and other places delivering health care are often common sources for patients to pick up MRSA if they have weak immune systems. Patients and live-ins are susceptible if they have an open cut or wound or intravenous line under the skin, are older in age, or have multiple ailments or conditions leading to compromised immune systems. Simply being in contact with numerous individuals in the same area can increase the spread among workers and patients.
Community-Associated MRSA

Another major way of contracting MRSA is outside the hospital environment. This is less prevalent and consists of about fourteen percent of cases reported by the Centers for Disease Control and Prevention. Some of the individuals at risk are players of contact sports, those who live in communal housing, patients with cuts or who inject drugs with needles, or those in contact with facilities or objects contaminated with the bacteria.
Diagnostic Tests
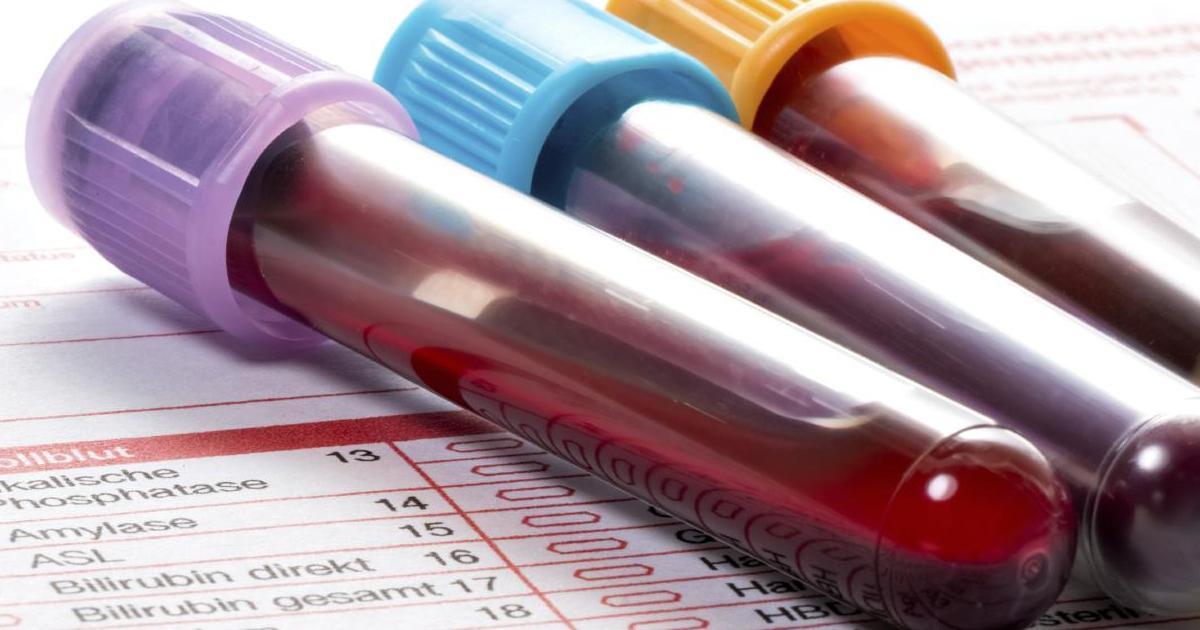
If a doctor suspects a patient has been exposed to the infectious bacteria and symptoms are present, they will conduct a biopsy or tests of all or one of the following: blood, urine, body fluid, or a wound swab. It would then have to be determined which antibiotic would work best to fight the illness. In some cases, antibacterial soaps, nasal ointments, or antibacterial shampoo will do the trick. A reported forty percent of confirmed cases had been reduced using these drug-free methods.
Community-Associated MRSA Prevention Methods

The general public is susceptible to contracting infectious diseases, especially when in the constant presence of others, particularly large groups. Everyone should keep all open wounds covered and only allow them to be drained by professionals. Frequent hand-washing and avoiding shared use of personal items like soap, towels, and toothpaste is also required to prevent the spread of bacteria. Keeping fingernails short will also help prevent potential open skin from occurring on oneself or others.
Health Care-Associated Prevention Methods
Guidelines for health and wellness are implemented in hospitals and care facilities and must be followed to prevent the spread of infectious diseases. Such measures include frequent hand-washing, cleaning of equipment, clothing, and bedding, separation of patients with MRSA from other patients, ensuring visitors are sanitary and are provided with gowns and gloves, and testing other patients for signs of the active bacteria.
Abscess Drainage
One sign indicating MRSA is forming is a boil that appears on the skin. This boil can turn into an abscess, which is often seen on patients with CA-MRSA and affect the trunk, arms, and legs. The patient should not try to drain the abscess or pop the boil themselves. Doctors often use abscess drainage to treat them, which typically involves making a small incision and drawing out the pus, though sometimes this is not enough to make the lesion go away permanently. In that case, the doctor gives the patients a course of antibiotics. Patients who have infections that come and go, a compromised immune system, or systemic disease benefit most from this methodology. It’s also helpful for elderly patients and babies.
Course Of Antibiotics

If an abscess related to MRSA is not resolved with drainage, doctors often resort to a course of antibiotics to treat it. These antibiotics include doxycycline, minocycline, trimethoprim-sulfamethoxazole, and clindamycin. The drugs and how they are taken depend on the needs of the patient. Sometimes they can be taken by the patient at home. The course usually lasts between seven and ten days, and it is important for the patient to finish the course their doctor set for them even if they feel better before the finish. If the patient has had to be hospitalized, they’ll receive the antibiotics intravenously then continue to take them after they’re discharged. They’ll either take them by mouth or continue to receive them intravenously with the help of a visiting nurse. The patient might need to take these antibiotics for as long as two months.
Complications Linked To MRSA
The consequences of methicillin-resistant Staphylococcus aureus range from inconsequential to life-threatening. Complications linked to MRSA include abscesses in the central nervous system, which includes the brain and the spinal cord. The patient can develop a connective tissue disorder called cellulitis; inflammation of the membrane that encloses the heart, called endocarditis; and infection of their bone marrow, known as osteomyelitis. MRSA can set up infections in the patient’s throat, joints and sinuses and can lead to pneumonia. Other patients have inflammation of their veins that lead to blood clots. Complications linked to methicillin-resistant Staphylococcus aureus also include urinary tract infections and toxic shock syndrome. Other patients may develop septicemia, otherwise known as blood poisoning, or ultimately suffer organ failure.
