What Causes Restless Leg Syndrome?
'The most common disorder you've never heard of' is how the Restless Legs Syndrome Foundation describes Willis-Ekbom disease, or restless leg syndrome (RLS) as it is more popularly known. The National Institutes of Health estimates seven to ten percent of citizens in America have restless leg syndrome. Yet, this widespread health problem is still largely unknown and untreated. This can lead to serious issues, such as depression, workplace problems, and anxiety. For this reason, it is vital individuals know the leading causes of restless leg syndrome.
Obesity

The study of restless legs syndrome has not yet identified the main cause of the condition. However, early research has linked restless leg syndrome to problems with the neurotransmitter dopamine, a chemical that helps the body have smooth muscle movements. When dopamine is missing or inhibited from working effectively (as with Parkinson's disease), an individual will experience involuntary body movements.
When researchers discovered obese individuals had reduced dopamine function, they theorized obesity may also be connected to restless leg syndrome. A study published in 2009 reviewed 65,554 women and 23,119 men and did find a link between restless legs syndrome and obesity. They found being overweight increased an individual's risk of restless leg syndrome from forty-two to sixty percent. The researchers concluded 'a greater BMI in early adulthood and weight gain was also associated with a higher prevalence of restless leg syndrome.'
Kidney Failure
Another condition associated with restless leg syndrome is kidney failure. From twenty-five to forty percent of individuals on dialysis suffer from restless leg syndrome. Scientists speculate there may be several factors caused by kidney disease that increases restless leg syndrome. First, National Institutes of Health report patients with end-stage renal disease can have iron-deficiency anemia, a risk factor for restless leg syndrome. This is due to the diseased kidneys' inability to produce adequate amounts of the hormone erythropoietin (EPO), a key component in the production of red blood cells.
With lower levels of EPO in the body, the bone marrow's red blood cell production is decreased, leading to anemia. Second, kidney failure increases uremic toxins in the body, which can cause peripheral neuropathy, another condition associated with restless leg syndrome.
Diabetes

Diabetes patients also have an increased risk of restless leg syndrome. In a 2014 study, researchers compared 140 diabetes patients to a matched control group. They found 28.6 percent of the diabetic patients had restless leg syndrome, while only 7.1 percent of the control group had the condition. "[A] higher percentage of people with diabetes may have RLS, which can be worsened by peripheral neuropathy or nerve damage caused by uncontrolled blood sugars," explained Health and science writer Ilene Rush.
Poor sleep quality is another influence a diabetic condition may have on restless leg syndrome. Experts believe the hindered metabolizing of glucose in the diabetic's body interrupts sleep patterns. Researchers have discovered an association with restless leg syndrome and sleep disorders, such as apnea and periodic limb movement disorder.
Polyneuropathy

This is another condition associated with an increased risk of restless leg syndrome. An individual with this ailment suffers damage to the peripheral nervous system of the body, often caused by a disease like diabetes or Guillain-Barre syndrome. Researchers have found individuals with this condition have from 5.2 to fifty-four percent greater occurrence of restless leg syndrome than the general population.
A study published in 1991 theorized the connection between polyneuropathy and restless leg syndrome is the entrapment of diseased nerves, which may become twice as large as healthy nerve fibers. Researchers in 2015 tested this hypothesis by examining forty-two patients who had surgical decompression of the superficial fibular nerves to treat peripheral neuropathy. All the patients reported a reduction in their restless leg syndrome symptoms.
Anemia And Iron Deficiency
A fifth condition associated with increased risk of rest leg syndrome is anemia and iron deficiency. Several factors have long indicated the link between iron levels and restless leg syndrome. First, researchers have found iron levels in the body naturally decrease during the night, a condition called the circadian variation. This corresponds with the time most restless leg syndrome symptoms occur. Third, pregnant women have an increased risk of restless leg syndrome during the last trimester, when the mother's iron levels are low.
Medical conditions such as these have helped researchers discover the important role of iron in restless leg syndrome. "The brain iron insufficiency in patients with RLS is now well established," concluded Richard Allen, a professor in the Department of Neurology at Johns Hopkins University. Researchers believe low iron levels interfere with the action of dopamine in the brain, which leads directly to restless leg syndrome. Two recent studies found iron supplementation significantly reduces the symptoms of restless leg syndrome.
Allergy Medication

Many individuals who suffer from allergies, particularly those of the seasonal variety, tend to take antihistamines, especially drowsy ones, to get rid of symptoms such as a runny nose and sneezing, so they can be more comfortable and get some rest. Unfortunately, however, reports indicate drowsy antihistamines can actually worsen the symptoms of restless leg syndrome and make it even more difficult to fall and stay asleep. While the exact reason for this is unknown, some research indicates antihistamines that do not cause drowsiness don't affect restless leg syndrome as much simply because this medication does not enter the brain as easily. In any case, individuals dealing with allergies as well as restless leg syndrome should turn to other options for allergy relief than antihistamines.
Sleep Deprivation

Sleep deprivation and restless leg syndrome are one of those unfortunate circles of cause and condition. Many individuals know restless leg syndrome can make it quite difficult to fall asleep, and when this effect is prolonged, it can result in sleep deprivation. However, sleep deprivation can also trigger and even worsen symptoms of restless leg syndrome if it happens to occur first, and then disrupts sleep even more. Thus, one significant thing to keep in mind is treating the sleep deprivation that can either cause or accompanies restless leg syndrome to see a reduction in the severity of symptoms.
Parkinson's Disease

Parkinson's disease is a medical condition related to abnormal functioning in the basal ganglia's dopamine pathways. This is important to note as there is a decent amount of evidence suggesting restless leg syndrome is related to a dysfunction of the basal ganglia and its use of dopamine, which is a chemical necessary to have smooth muscle activity. A disruption in the basal ganglia can result in jerky or otherwise involuntary movements. Involuntary movements are hallmark symptoms of both Parkinson's disease as well as restless leg syndrome, which is why Parkinson's disease patients are at an increased risk of developing the latter.
Caffeine Consumption

Consuming caffeine, particularly in large quantities and in the evenings before bedtime, can increase an individual's risk of restless leg syndrome. This is because caffeine is considered a stimulant and can keep individuals awake at night, which as we know can trigger or worsen symptoms of restless leg syndrome. Caffeine can even introduce involuntary muscle twitches when it is consumed in excess, or when individuals dramatically and suddenly cut back on their consumption, causing symptoms of withdrawal. Individuals who drink caffeine and who suffer from restless leg syndrome may wish to try reducing their intake and adjusting when they drink anything with caffeine (such as avoiding caffeine after five o'clock in the evening).
Antidepressants And Antipsychotics

Quite a significant amount of research indicates antipsychotic medication and several types of antidepressants, especially those that increase serotonin, can trigger or worsen cases of restless leg syndrome, though additional research is required to pin down the exact link. These types of antidepressants include selective serotonin or norepinephrine reuptake inhibitors (SSRIs and SNRIs respectively) and tricyclic antidepressants.
Their association with restless leg syndrome is why the condition is listed among the potential side effects of taking the medication. It is also why doctors will only recommend taking these medications when the benefits outweigh the possible risks. Furthermore, if patients do experience restless leg syndrome as a result of taking a certain medication, they may wish to talk to their primary doctor to determine if there is a suitable alternative they can try in an effort to reduce the symptoms of restless leg syndrome.
Fibromyalgia

Many fibromyalgia patients also experience sleep disorders, with one of the most common being restless leg syndrome. In fact, one study showed sixty-four percent of fibromyalgia patients also struggle with RLS. Restless leg syndrome and fibromyalgia are both neurological conditions, but researchers don't yet understand the underlying mechanisms that cause them. They are not sure why so many individuals with fibromyalgia also develop RLS.
One theory is both of the conditions are central sensitivity syndromes. These syndromes involve nervous systems developing sensitivities to certain environments or sensory input. With central sensitivity syndromes, patients are sensitive to strong smells, loud noises, bright lights, pressure against the body, rough textures, and any other stimuli the central nervous system processes.
Venous Insufficiency
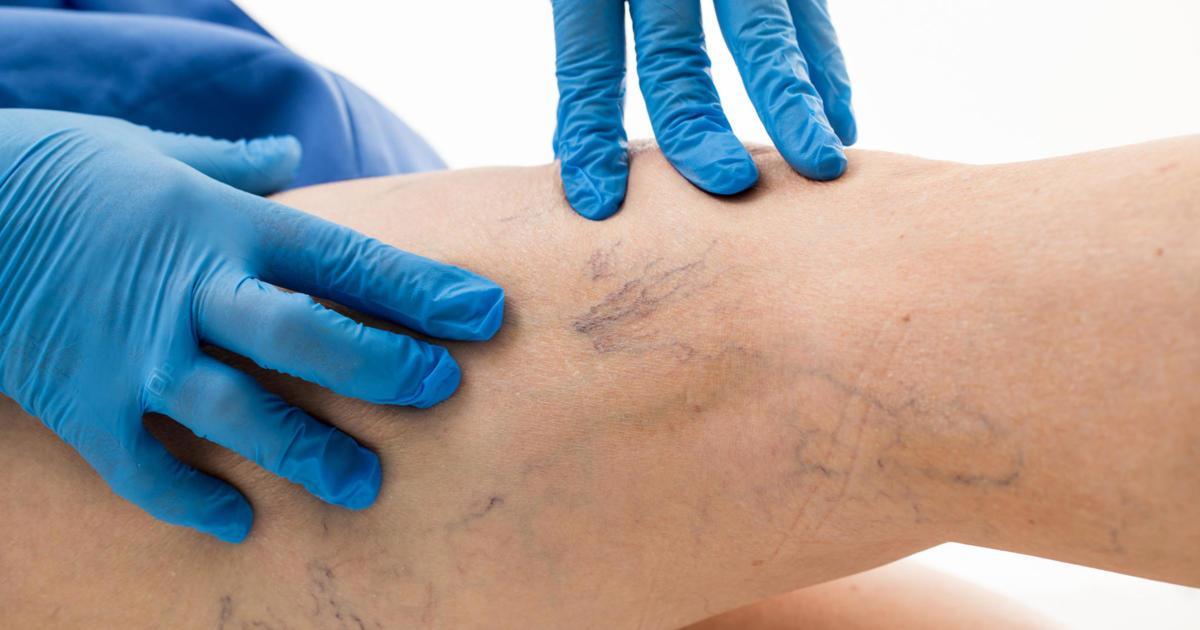
Venous insufficiency can cause restless leg syndrome. In fact, studies show up to twenty-two percent of RLS patients have some form of venous insufficiency. When restless leg syndrome occurs alongside venous insufficiency, one of the best ways to treat it is by also treating the varicose veins. The Journal of Phlebology published a study indicating when patients had both venous disease and restless leg syndrome, ninety-eight percent saw a reduction in RLS symptoms when they had their varicose veins treated. In addition, eighty percent of patients experienced symptom relief on a long-term basis. The first step to diagnosing and treating varicose veins is for individuals to have a doctor evaluate their legs in an office visit. They may also use noninvasive ultrasound technology to get a more definitive sense of the condition.
Hypothyroidism Or Hyperthyroidism
Hypothyroidism or hyperthyroidism and restless leg syndrome often occur together because both conditions are associated with dopaminergic dysfunction. In a study of patients with thyroid conditions, 8.2 percent reported having symptoms similar to those described in RLS. By comparison, the control group without thyroid conditions only have a 0.9 percent prevalence of restless leg symptoms. One-third of the thyroid patients reported their RLS symptoms became completely resolved after their thyroid condition was treated.
Hypothyroidism is caused by the thyroid failing to make enough hormones. The condition can also cause depression and slow metabolism. On the other hand, hyperthyroidism occurs when the thyroid is overactive and creates too many hormones. This can lead to an overactive metabolism and potentially serious symptoms.
Rheumatoid Arthritis

Rheumatoid arthritis has been associated with restless legs syndrome. Studies indicate RLS might occur in around ten to fifteen percent of the population in the United States. Almost one-third of restless leg syndrome patients also have rheumatoid arthritis. One theory for why these conditions occur alongside each other so often is because of iron deficiency. The brain produces a chemical called dopamine, which is essential to the health of an individual's immune system and central nervous system. Dopamine needs iron to function properly. Many of those with RLS symptoms also have low iron levels, which means dopamine isn't functioning as effectively in the brain. Rheumatoid arthritis can affect the amount of iron in the brain or the ability to use iron in the brain.
Spinal Nerve Damage
Spinal nerve damage may sometimes increase an individual's risk of developing restless legs syndrome. The way the condition affects someone depends largely on what kind of damage was done to the nerves, how extensive it is, and how it affects their body. Patients who have lesions on their spinal cord have a higher likelihood of developing RLS. Similarly, if individuals have anesthesia administered to their spinal cord, that can increase their risk of developing restless legs syndrome. It is not commonly understood why RLS is related to spinal nerve damage, but one theory is that nerve damage interrupts the signals between the brain and legs, which can lead to symptoms.
