Serious Symptoms Of Pulmonary Artery Sling
Pulmonary artery sling is an uncommon congenital anomaly of the pulmonary arteries. In a healthy individual, the oxygen-poor blood from the body flows through the superior and inferior vena cava to the heart. This oxygen-poor blood moves through the right atrium to the right ventricle where it is then pumped through a split that ultimately forms the left and right pulmonary arteries. The left and right pulmonary arteries carry the oxygen-poor blood to the lungs to be reoxygenated.
A healthy individual's pulmonary arteries sit in front of their windpipe and esophagus. However, individuals with pulmonary artery sling have a left pulmonary artery that branches from their right one. This abnormal arrangement causes the left pulmonary artery to thread between the windpipe and esophagus to reach the left lung. The symptoms of this anomaly usually manifest shortly after birth, and surgery is the only way to treat it.
Shortness Of Breath

Shortness of breath can be caused by the pressure the right pulmonary artery, left pulmonary artery, and the pulmonary trunk is placing on the affected individual's windpipe. Increased pressure on the windpipe causes it to become compressed, leaving less area for inhaled air to travel through the windpipe and into the lungs. The division of the left pulmonary artery from the right pulmonary artery in a pulmonary artery sling patient sits just on top of their right mainstem bronchus. As these arteries expand to accommodate the volume of blood that flows through them, the right mainstem bronchus can become compressed.
For adequate levels of carbon dioxide oxygen exchange to occur in an affected individual's lungs, a sufficient amount of air must be able to reach the alveoli, which are the small air sacs in the lungs. A compressed trachea or right mainstem bronchus can hinder the ability of air to reach the alveoli, reducing the amount of carbon dioxide oxygen exchange taking place. The brain detects this malfunction and signals the lungs to work harder in an attempt to increase the oxygen in the blood. This mechanism is responsible for an individual's shortness of breath.
Cyanosis
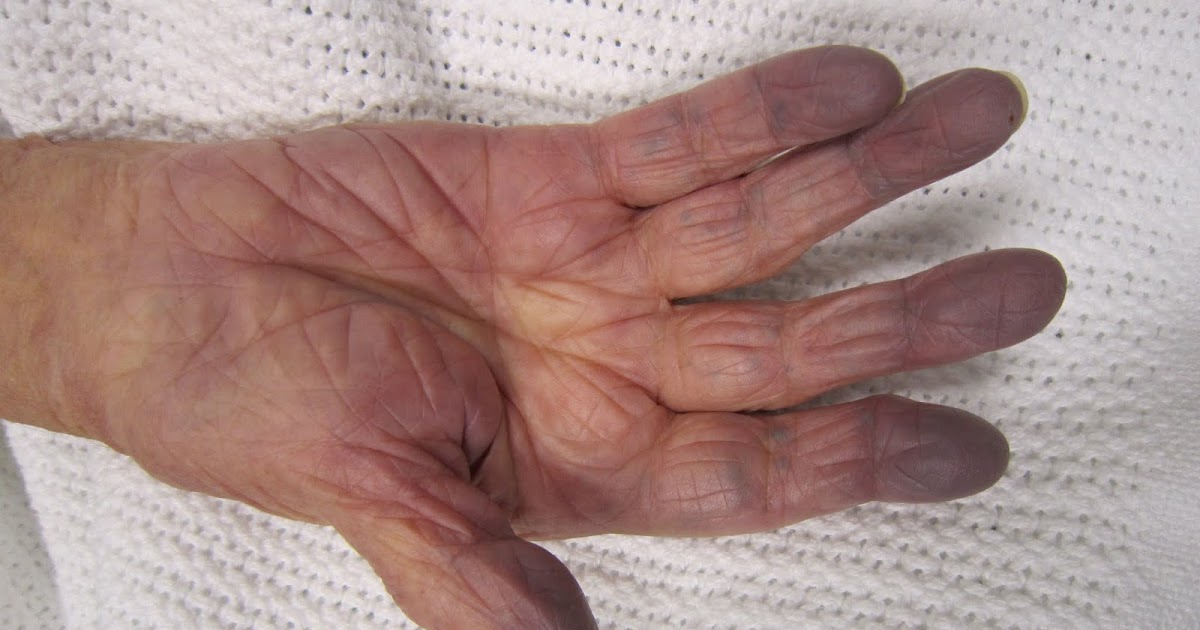
Cyanosis describes someone's fingertips, toes, hands, or feet turn a shade of blue or green due to a lack of oxygenated blood. Oxygen-rich blood is a bright red inside of an individual's body, while oxygen-poor blood is a dark maroon in the body. Light reflects off of these two colors in different ways, which causes oxygen-poor blood to appear blue when looking at it through the skin. Pulmonary artery sling patients may have trouble with inhaling an adequate amount of oxygen due to the effects pulmonary artery sling has on the function of their trachea and right mainstem bronchus.
Not only can both of those main airways become compressed, but an individual affected by pulmonary artery sling may also experience a decrease in the amount of oxygen they can breathe in due to stenosis, the adaptive narrowing of the trachea or windpipe. Not enough oxygen can reach the alveoli, which causes insufficient levels of oxygen in the blood. Low blood oxygen concentration causes the extremities to exhibit cyanosis.
Recurrent Pneumonia

The airways in an individual's respiratory tract have many functions, including the production of secretions in response to certain stimuli. These secretions are meant to engulf the foreign substances and pathogens so the body can eliminate these secretions through the oral and nasal cavities by coughing and other means. However, this secretion elimination process is impaired in many pulmonary artery sling patients. The right pulmonary artery, left pulmonary artery, and the pulmonary trunk sits on top of and compresses the right main bronchus and trachea in an individual with pulmonary artery sling.
This compression leaves less room or volume for the natural elimination of secretions from the airways and lungs. When secretions are not properly eliminated from the lungs and contain a foreign infection-causing pathogen, the pathogen is given the opportunity to colonize in an individual's lung tissues. Once the immune system becomes aware of the pathogen, the inflammatory cascade begins in the lung. The alveoli then fill with purulent material or pus, and pneumonia is the result.
Wheezing

Wheezing is a high-pitched noise produced when an individual exhales and inhales. Some individuals have described the sound of wheezing as a whistling or purring noise. Wheezing is best heard by others when the affected individual is exhaling air from their lungs. This sound is produced when air is irregularly moving through the airways due to structural alterations in one or both of the larger airways that feed the lungs. The types of alterations known to produce wheezing sounds are a partial airway obstruction or narrowing of multiple larger airways in the lungs.
Pulmonary artery sling patients may experience compressed airways due to the awkward and abnormal position of their pulmonary arteries. Wheezing may be an intermittent occurrence because the airway narrowing is caused by the pressure blood vessels place on the airways. The intermittent nature of wheezing can be attributed to the pressure fluctuations on the airways that occur when the offending blood vessels expand and contract to maintain blood pressure.
Obstructive Sleep Apnea

Obstructive sleep apnea is a sleep disorder that causes an individual to stop and start breathing multiple times during their sleep. Obstructive sleep apnea is the most common type of sleep apnea among the population and typically happens when the muscles in an individual's throat allow it to close and block the airway. Pulmonary artery sling patients may have obstructive sleep apnea because the irregularly positioned pulmonary arteries can cause the muscles to become overly relaxed in the windpipe.
The airway becomes temporarily blocked during the affected individual's sleep. This malfunction may occur more often with changes in position. Essentially, this type of sleep apnea can occur when any mechanism involving the pressure from the pulmonary arteries causes the airway to become obstructed. Once the brain detects an abnormal rise in carbon dioxide levels due to the impaired breathing, it wakes the affected individual from their sleep to re-open the airway.
