Tips For Treating And Preventing Atrial Flutter
Atrial flutter is a type of abnormal heart rhythm similar to atrial fibrillation. In patients who have atrial flutter, the heart beats fast and in a regular rhythm. However, the atria (the heart's upper chamber) beats too rapidly, causing what is heard as a flutter. Often, the heart will beat at 250 to 350 beats per minute during atrial flutter. The condition develops due to problems with the electrical activity of the heart, and it most often occurs in individuals over sixty years old. Sometimes, patients with the disorder may not experience any symptoms. When symptoms are present, they include lightheadedness, fatigue, chest pain, shortness of breath, and fainting.
Patients who deal with diabetes, obesity, and other heart problems are at an increased risk of the condition. If left untreated, atrial flutter can lead to potential strokes and heart failure. To diagnose atrial flutter, doctors perform an electrocardiogram (ECG), and patients may also wear a portable ECG monitor at home to record episodes of fluttering.
Blood-Thinning Medications
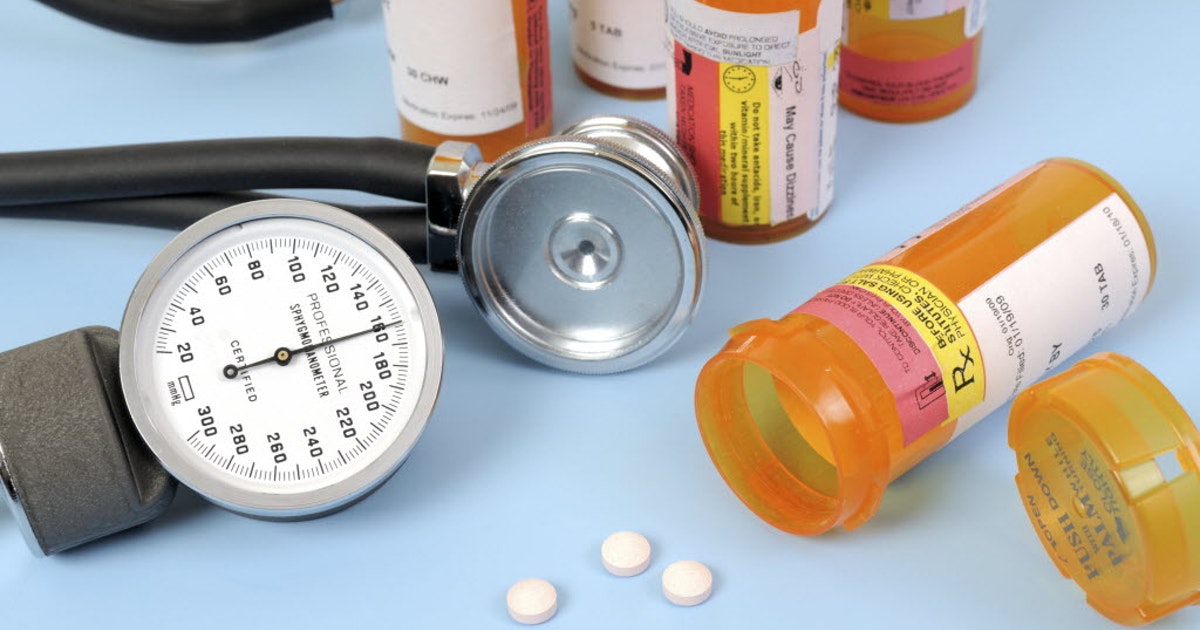
Atrial flutter and other types of abnormal heart rhythms can trigger the formation of life-threatening blood clots. Since atrial flutter does not always produce symptoms and may only occur on an occasional basis, patients may be unaware of when they are experiencing an atrial flutter episode. Doctors prescribe blood-thinning medications, known as anticoagulants, to almost all atrial flutter patients to reduce the risk of blood clots.
Patients often need to continue taking anticoagulants throughout their lives. Some of the most commonly prescribed anticoagulants include warfarin, heparin, dabigatran, and rivaroxaban. These can cause side effects, including easy bruising or bleeding and feeling cold. For patients who cannot take anticoagulants, acetylsalicylic acid is sometimes recommended.
Electrical Cardioversion

Electrical cardioversion is one of the most effective ways to restore normal heart rhythm in patients experiencing an active episode of atrial flutter that has not spontaneously resolved. It is a surgical procedure that can be done at an outpatient facility, and it may also be performed in hospitals for emergency cases. Patients receive strong sedatives through an intravenous line during the procedure, and they do not feel any pain.
While patients are sedated, doctors place special pads on the patient's upper chest and back. The pads deliver an electrical shock to the heart, restoring it to a normal rhythm. Following the procedure, patients will often need to start taking special medications to help keep their heart in the normal rhythm. Electrical cardioversion is successful for at least seventy-five percent of patients with atrial flutter.
Catheter Ablation
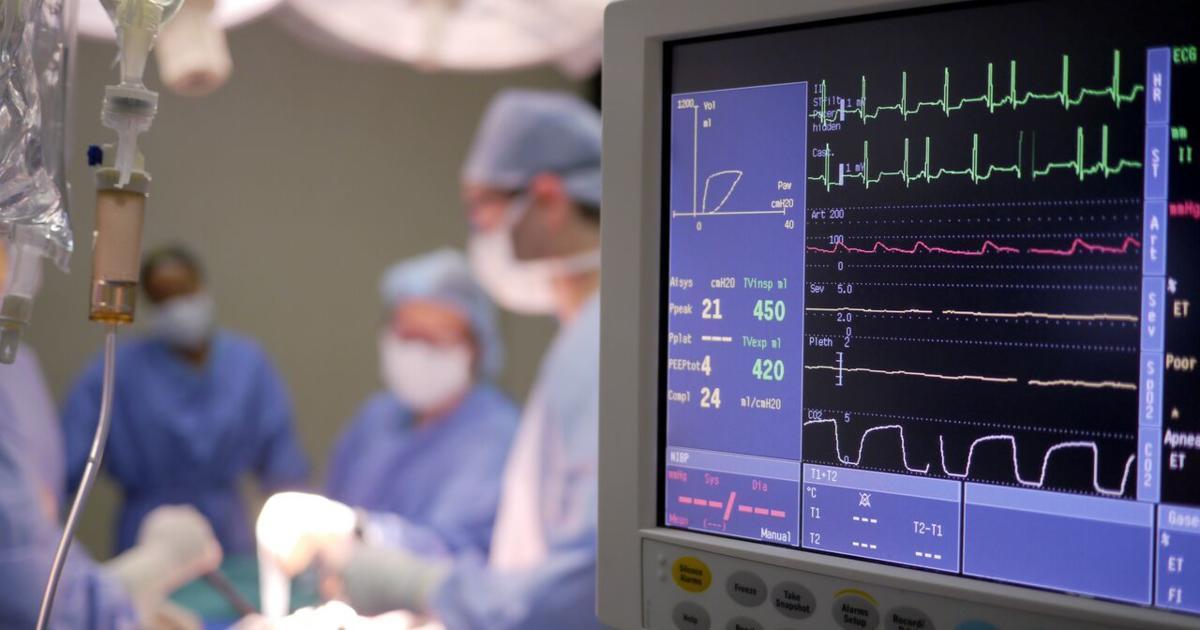
In patients for whom cardioversion and medication are unsuccessful, catheter ablation is often recommended. This procedure is minimally invasive and involves advancing a catheter from a blood vessel in the groin or neck until it reaches the area of the abnormal circuit. The catheters used for the operation have electrodes mounted on them that can monitor the patient's heart rhythm and also send out electrical signals. Doctors first monitor the heart rhythm, and once they locate a particular safe point in the rhythm, they destroy the abnormal heart circuit through either high heat or freezing temperatures.
Ablation usually takes between two to three hours, and patients are transported to a recovery area for monitoring once the ablation has been completed. While many patients can be released to go home the same day, some patients may need to spend a night in the hospital. Doctors monitor the patient's heart rhythms closely at follow-up appointments. If necessary, ablation procedures can be repeated.
Other Medications

In addition to anticoagulants, doctors often prescribe other medications such as beta-blockers, calcium channel blockers, and antiarrhythmics. Both calcium channel blockers and beta-blockers slow the rate at which the heart beats by slowing electrical conduction through the heart's AV node. Additionally, beta-blockers help keep the heart beating in a normal rhythm. Some of the most commonly prescribed beta-blockers include acebutolol, atenolol, bisoprolol metoprolol, nadolol, and nebivolol. In some patients, these medications can lead to side effects such as weight gain, cold hands and feet, fatigue, depression, insomnia, and fatigue.
Examples of popular calcium channel blockers include amlodipine, bepridil, felodipine, and nisoldipine. Patients taking calcium channel blockers may experience low blood pressure and low pulse rate, and doctors usually ask these patients to monitor their blood pressure and pulse at home on a daily basis. In particular, if a patient notices their pulse is too low, they should contact their doctor's office to ask whether to take the calcium channel blocker that day or not. Other potential side effects include increased appetite, constipation, bleeding gums, swollen ankles and feet, and reflux disease. Antiarrhythmic medicines can change atrial flutter back into a normal heart rhythm and prevent future episodes of fluttering. Sotalol, amiodarone, and propafenone are examples of these medications, and doctors typically prescribe them to patients who have recently had cardioversion. Side effects include chest pain, fast or slow heart rate, swollen feet, dizziness, and blurred vision.
Prevention Tips

Patients who have experienced even a single episode of atrial flutter often want to do everything possible to avoid have additional ones. Thus, doctors routinely counsel their patients with several prevention tips. Atrial flutter is often reduced with lifestyle changes, and doctors recommend patients consider trying the DASH or Mediterranean diets to help make their hearts as healthy as possible. Patients who smoke should talk to their doctors about medications and support services that can help in quitting, and patients who are overweight or obese may wish to consider weight loss support groups, online weight loss programs, or nutrition consultations.
When exercising, it is especially important that patients are cautious and do not try to push themselves too hard or too long. They should opt for lighter exercises like slow swimming or light yoga. If patients notice their heart feels out of rhythm during exercise, they should stop immediately and call their healthcare provider for advice. Patients may wish to try meditation, writing in a journal, or reading for stress relief.
