Ways To Treat Pulmonary Hypertension
Pulmonary hypertension refers to elevated blood pressure in the arteries of the lungs and the right side of the heart. It is a serious disease and is different than systemic hypertension, which affects the whole body and is comparatively minor. Pulmonary hypertension results in both a narrowing and hardening of the blood vessels that transport blood from the heart to the lungs. Early symptoms include chest pain, fatigue, shortness of breath, loss of appetite, pain in the upper right area of the abdomen, and a fast heartbeat. As the disease progresses, symptoms expand to include leg or ankle swelling, fainting or feeling lightheaded, and a bluish tinge to the lips or skin. This form of hypertension can be diagnosed with a series of specialized heart tests, including an electrocardiogram, echocardiogram, cardiac catheterization, and a chest CT or MRI. Blood tests, chest x-rays, sleep studies, and lung perfusion scans may also be useful in obtaining a diagnosis. While pulmonary hypertension cannot be cured, steps can be taken to control and improve symptoms. The following methods provide symptom management and an enhanced quality of life for pulmonary hypertension patients.
Transplant

A transplant may prolong life and extend quality of life for patients who do not respond to conservative treatments. Both lung transplants and heart-lung transplants have been used for pulmonary hypertension patients. The majority of patients receive a double lung transplant. The survival rates following this procedure are seventy-nine percent at one year and fifty-five percent at five years post-surgery. Due to the complexity of the transplant as well as the lengthy recovery time associated with it, many patients will need specialist care at a medical facility for several months after the procedure. Organ recipients need to take daily anti-rejection medication to help their bodies accept the new lungs and reduce the risk of infection for the rest of their life. They also require frequent and careful monitoring for many years following the surgery.
Keep reading to learn about the next method of treating pulmonary hypertension.
Atrial Septostomy

An atrial septostomy is a surgical procedure often recommended to patients with severe pulmonary hypertension. The procedure helps decrease the pressure placed on the right side of the heart. An atrial septostomy can also benefit patients who commonly experience fainting, which occurs due to the sudden increases in lung pressure that can sometimes happen with this condition. During an atrial septostomy, the surgeon makes a small incision in the septum (wall) that lies between the right and left atria of the heart. The hole protects the right side of the heart by allowing it to decompress in the event of a sudden rise in lung pressure. The procedure can be performed using a balloon or a blade. Balloon operations are known as balloon atrial septostomy or Rashkind's procedure, and blade procedures are medically referred to as blade atrial septostomy or static balloon atrial septostomy. Complications from the procedure include tearing of the cardiac muscle and abnormal heart rhythms.
Reveal more ways in which pulmonary hypertension can be treated.
Follow A Healthy Diet

Pulmonary hypertension patients need to be particularly mindful of their nutrition and take steps to follow a healthy diet. To help patients feel better, doctors generally advise them to limit sodium intake and monitor their fluids. A maximum of two thousand milligrams of sodium is advised per day. Fluid intake should be limited to no more than two liters each day, as more than this may cause fluid retention and place added strain on the heart. Some medicines for pulmonary hypertension may cause nausea, which can make it difficult to eat. Unsalted crackers and dry toast can help reduce nauseous feelings.
Patients with this condition will likely be taking blood thinners, and levels of vitamin K, which helps the blood clot, will need to be monitored closely and kept as steady as possible as a result. Low iron levels can exacerbate symptoms of pulmonary hypertension, and patients are advised to eat high-iron foods such as beans, spinach, tofu, lentils, and molasses. All patients should avoid alcohol and caffeine, both of which can stress the heart and increase blood pressure.
Understand more about how pulmonary hypertension can be treated now.
Medications
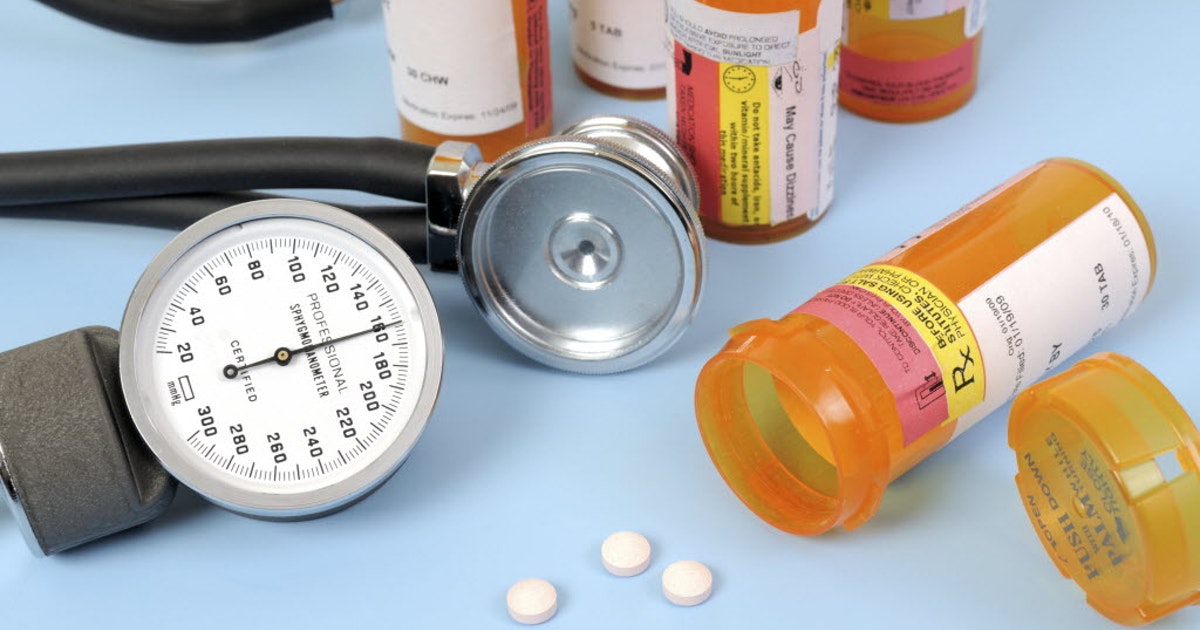
A variety of tablets, sprays, and injections can help in managing pulmonary hypertension. Anticoagulants (blood thinners) such as warfarin prevent blood clots that can worsen the condition, and calcium channel blockers can reduce blood pressure by relaxing certain arteries. To strengthen the heartbeat, doctors may recommend digoxin, a drug particularly useful for patients who also have heart failure or heart rhythm abnormalities. Diuretics can help reduce fluid retention, and these drugs require regular monitoring with blood tests. Medications such as ambrisentan, bosentan, and macitentan can keep blood pressure down by helping blood vessels remain open. Depending on the severity of pulmonary hypertension, some patients may benefit from oxygen therapy. This can be administered at home through a special machine. Patients will likely be on several medicines at once, and because of this, they should be closely monitored by their doctors. Any side effects should be reported to medical staff, and changes in medication may be possible to reduce unwanted impacts.
Unveil the next method of treating pulmonary hypertension now.
Maintain A Healthy Weight

Many patients with pulmonary hypertension are overweight or obese. While obesity alone is not considered to be a risk factor for pulmonary hypertension, individuals who are overweight or obese may have other related chronic health conditions associated with pulmonary hypertension. This includes sleep apnea, in which oxygen levels drop while a patient sleeps. Studies of obese individuals with pulmonary hypertension who have undergone bariatric surgery show marked improvements in their quality of life following weight loss. To maintain a healthy weight or reach a weight loss goal, experts advise limiting red meat, fried foods, processed foods, and fast food. Home-cooked meals that emphasize fruits, vegetables, legumes, and whole grains can help patients feel healthier and may reduce the need for some medications.
