Warning Signs Of Venous Insufficiency
Venous insufficiency is a condition that affects the circulation of the blood. Here, the normal function of the walls and valves of the veins is impaired, and blood pools instead of circulating back to the heart. This condition primarily impacts the legs. Risk factors for venous insufficiency include the presence of varicose veins and a personal history of blood clots. Obesity, pregnancy, cancer, and smoking can all elevate an individual's risk of this condition too. Women are more likely to have venous insufficiency than men, and it typically occurs in patients over fifty years old.
To diagnose venous insufficiency, doctors usually perform a duplex ultrasound or a venogram, and a physical examination. Treatment options for venous insufficiency include compression socks and medications such as diuretics, anticoagulants, and pentoxifylline. Surgical repair or removal of damaged veins might be recommended in severe cases.
Leg And Ankle Swelling

Patients with venous insufficiency frequently notice leg and ankle swelling. Also known as edema, this swelling occurs due to the pooling of blood in the veins, and it is normally painless. Occasionally, patients could notice the swelling extends up to their thighs. Individuals who take calcium channel blockers, MAO inhibitors, tricyclic antidepressants, or estrogen could notice increased swelling. The use of compression socks can help reduce swelling, and patients can get a prescription for these from their doctor.
Regular exercise such as walking can help improve blood circulation, and reducing salt intake is generally recommended. While lying down, patients may wish to place their legs and feet on pillows so they are elevated above the heart. Doctors also suggest patients avoid wearing tight clothing around the thighs and lower legs, and individuals who experience ankle swelling might need to make adjustments to their socks and shoes. If chest pain or shortness of breath occurs with leg swelling, patients should seek immediate medical care.
Aching Or Heavy Legs

The reduced blood flow associated with venous insufficiency can cause the patient to have aching or heavy legs. The sensation is often described as a dull ache, and some individuals also notice cramping, tingling, itching, or pain. The aching, heaviness, and pain usually worsen while standing, and patients might feel a tightness in the calves. To reduce aches and pains, doctors recommend lying down with the legs elevated. Some patients may need to take pain relievers to reduce leg aches, and it is important to check with a doctor before using these, especially if the patient has any additional medical conditions.
Applying cold or warm compresses to the legs may reduce pain, and gentle exercises such as walking or tai chi may be beneficial as well. Individuals with venous insufficiency should always let their healthcare team know if they experience sudden increases in leg aches or pains. Since aching in this area can sometimes be a symptom of deep vein thrombosis, patients should seek urgent medical attention if the ache is accompanied by a fever or if the aching leg is noticeably red, warm, or swollen.
Leg Ulcers

If venous insufficiency is left untreated, patients could develop leg ulcers, sometimes known as stasis ulcers or venous stasis ulcers. Leg ulcers are open wounds on the skin that take more than two weeks to heal. In patients with venous insufficiency, these ulcers are often found on the just above the ankle, usually on the inside of the leg. The skin around an ulcer may be discolored or hard, and a discharge of pus could develop if the ulcer becomes infected.
To promote healing of leg ulcers, doctors clean and dress the ulcers, and compression bandages or socks are placed over the site to improve circulation to the area. Patients will also be asked to elevate their legs three or four times each day for up to thirty minutes at a time. If infection is present, antibiotics will be prescribed, and some ulcers may need to be treated with debridement, a process that removes damaged tissue from the affected area. Skin grafting and other surgical procedures might be appropriate for certain cases.
Varicose Veins
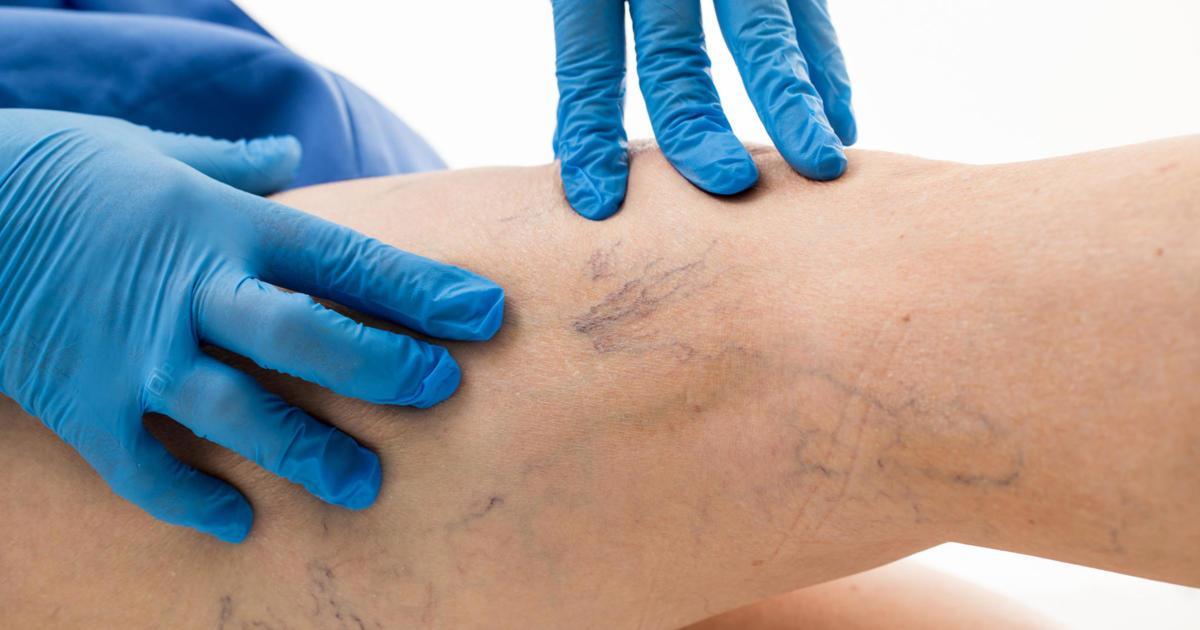
Varicose veins may develop on the surface of the legs in patients with venous insufficiency. These veins are twisted and enlarged, and they sometimes itch. Varicose veins can cause aching and pain in the legs. To diagnose this condition, specialists will examine the patient's legs for swelling, sores, and discoloration. Next, they may perform an ultrasound exam to check the blood circulation in the veins and rule out other issues such as blood clots. Patients with a small number of varicose veins may be treated with sclerotherapy.
In this procedure, saltwater is injected into the affected veins, causing them to harden and disappear. Surgeons may recommend phlebectomy for small varicose veins as well. This treatment involves removing the damaged vein through an incision. For patients who have larger or more widespread varicose veins, surgeons might perform varicose vein stripping. In-office treatments using lasers or radiofrequency waves may be effective for certain patients.
Leg Cramps

Venous insufficiency often produces leg cramps, and patients may notice a throbbing or burning sensation with this symptom. Cramps occur when muscles involuntarily contract, and the affected muscles are immobilized for a few seconds. Leg cramps generally occur in the calf muscle, and they may also develop in the feet or thighs. Patients with leg cramps often report they are more frequent at night. Although the causes of leg cramps are not yet fully understood, experts currently believe they may be related to dehydration or muscle fatigue.
Leg cramps are recognized side effects of medications such as diuretics, birth control pills, naproxen, statins, and albuterol. Individuals who use these medicines and experience frequent or intolerable leg cramping may want to ask about the possibility of switching to another medication. To relieve a cramp, it may help to massage the leg and flex the foot, and gentle walking might provide relief as well.
Worsening Pain Upon Standing

Venous insufficiency typically causes an aching, throbbing, or heavy sensation in the legs, and patients often find they experience worsening pain upon standing. For example, the pain may be worse while walking or standing in line than it is when the patient is sitting down or lying down in bed. Patients might find the pain worsens when they get out of bed in the morning as well.
To reduce the pain, it can be beneficial to take frequent rest breaks to sit down while performing an activity that requires standing. Wearing comfortable footwear could ease pain as well, and patients may want to schedule a rest period in which they sit with their legs raised; this posture has been shown to ease the pain associated with venous insufficiency. Patients should always check in with their specialist if there is any change in the location or intensity of their leg pain.
Thickened Skin On Legs Or Ankles

If venous insufficiency continues for a long time, thickened skin could form on the legs or ankles. Patients may notice these texture changes on the lower legs, and they could affect one or both legs. The thickening of the skin is often accompanied by inflammation in the affected area, and patients could notice varicose veins and swelling of the legs and ankles as well.
Thickened skin in these areas could make walking, wearing certain footwear and exercising more painful. Since these types of skin changes may indicate a variety of medical conditions, patients who notice them should see their primary doctor for an evaluation. Tests such as a duplex ultrasound may be necessary to evaluate the direction and speed of blood flow, and some patients may need a venogram. Areas of thickened skin should be monitored closely for changes, and these should be promptly evaluated by a physician.
Changes in Skin Color
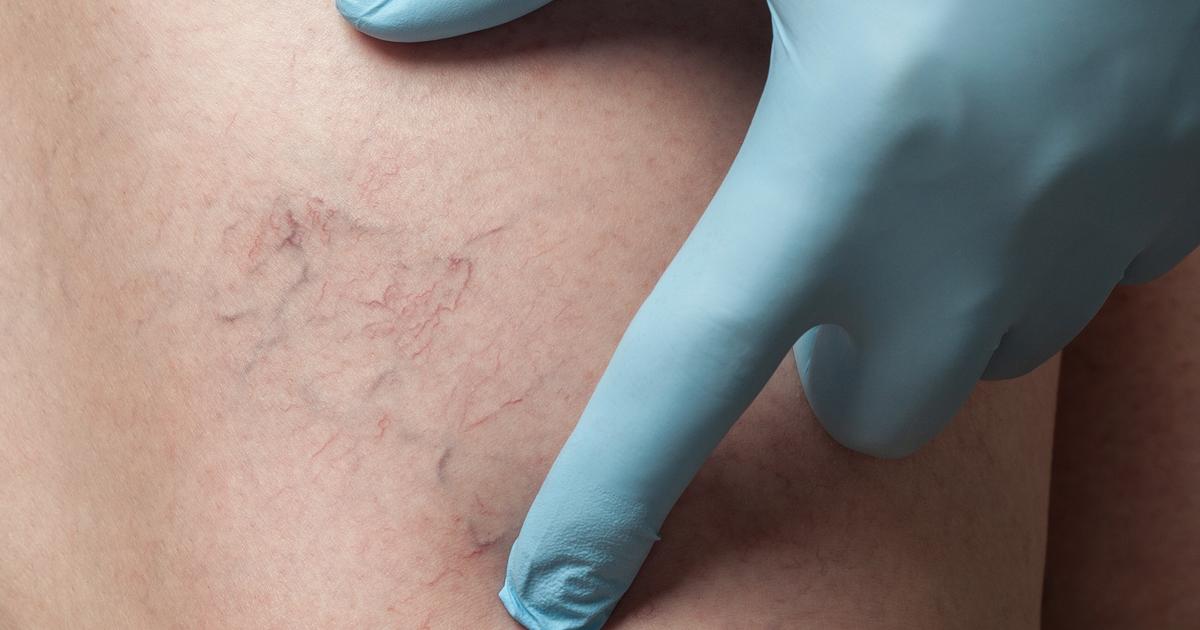
Venous insufficiency causes pressure to buildup inside of the veins in the lower legs, and this triggers changes in skin color. Small capillaries in the legs burst open, and the overlying skin turns a reddish-brown color. Changes in skin color associated with venous insufficiency are typically noticed around the ankles at first, and they can progress to other parts of the legs. Since reddening of the skin in this area could be indicative of a blood clot, patients who notice this symptom should seek urgent medical care.
Doctors may need to perform blood tests and imaging studies to determine the underlying cause of the skin discoloration. Patients who have already been evaluated should continue to monitor their skin for changes in color. They may want to do this by taking periodic photographs of the affected area to look for any increase in the size of the discolored area or any increasing redness. Once skin discoloration occurs, it could lead to the formation of leg ulcers, and patients will need to check their skin regularly for these. In particular, patients with diabetes should ensure they examine their skin thoroughly and report any changes promptly.
Itchy Skin
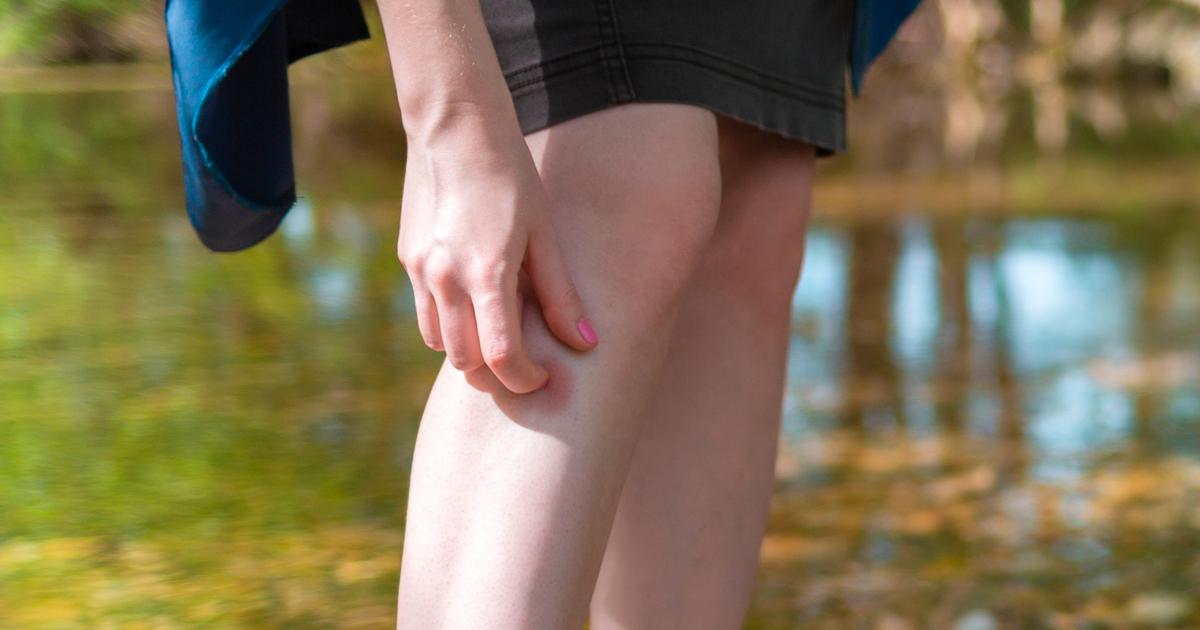
Individuals with venous insufficiency might report having intensely itchy skin. This symptom is caused by the pooling of blood associated with this condition and skin inflammation. The itching sensation normally affects the lower legs. If redness and swelling are also present, doctors may identify this symptom cluster as a separate condition called venous stasis dermatitis.
Lifestyle modifications such as the use of compression stockings and elevating the legs above the level of the heart while resting could help ease the symptoms of this condition. Patients are also advised to avoid standing still for prolonged periods and take breaks for walking as often as possible. Antihistamines and corticosteroid creams may be prescribed to reduce skin itching. In severe cases, doctors could consider surgical procedures to repair the veins. Many of these can be performed on an outpatient basis.
Blood Clots

Blood clots are a potentially serious symptom of venous insufficiency. If left untreated, blood clots could dislodge and travel to the lungs, where they could become life-threatening. Patients with blood clots could notice pain, swelling, redness, and warmth in the leg. Blood clots usually occur in only one leg at a time, and patients might notice the leg with the clot is larger than the unaffected leg. In the late stages, the pain of a blood clot in the leg could become so severe that the patient experiences pain from the slightest touch to the area. For example, placing a sheet over the affected leg could cause excruciating pain.
Emergency medical care should be obtained for any of these symptoms. Once patients are at the hospital, doctors will perform imaging studies and blood tests to determine the size and location of the clot. Intravenous medications may be administered to dissolve the clot, and some patients may require surgery or treatment in intensive care. Patients recovering from blood clots will be placed on anticoagulants to prevent future blood clots, and they will be encouraged to make appropriate lifestyle modifications such as smoking cessation and regular exercise. Patients will be monitored closely by their physicians at frequent follow-up appointments.
