What Is Autoimmune Hepatitis & Why Is It So Serious?
Many individuals are aware of what hepatitis is, however, very few truly know or have even heard about autoimmune hepatitis. Autoimmune hepatitis is a chronic and long-lasting disease where the immune system attacks the liver and causes severe inflammation and damage to this vital organ. This severe condition can be life-threatening if it is not detected early enough or treated, as it can lead to cirrhosis and even liver failure. Learn more now about this serious and uncommon autoimmune condition, its symptoms, and how it is treated.
What Is Autoimmune Hepatitis?
Autoimmune hepatitis occurs when the liver becomes inflamed due to the body's immune system turning against and attacking liver cells. While the exact cause of this disease remains unclear, it is believed genetic and environmental factors play a significant role as both appear to interact over time and trigger the disease. Fortunately, when autoimmune hepatitis is diagnosed and treated early, it can be safely managed with medications that suppress the immune system and stop it from attacking healthy liver cells. If the patient's body does not respond to medications and treatment or when liver disease has progressed to an advanced stage, a liver transplant is usually a patient's best option for fighting the disease.
Symptoms
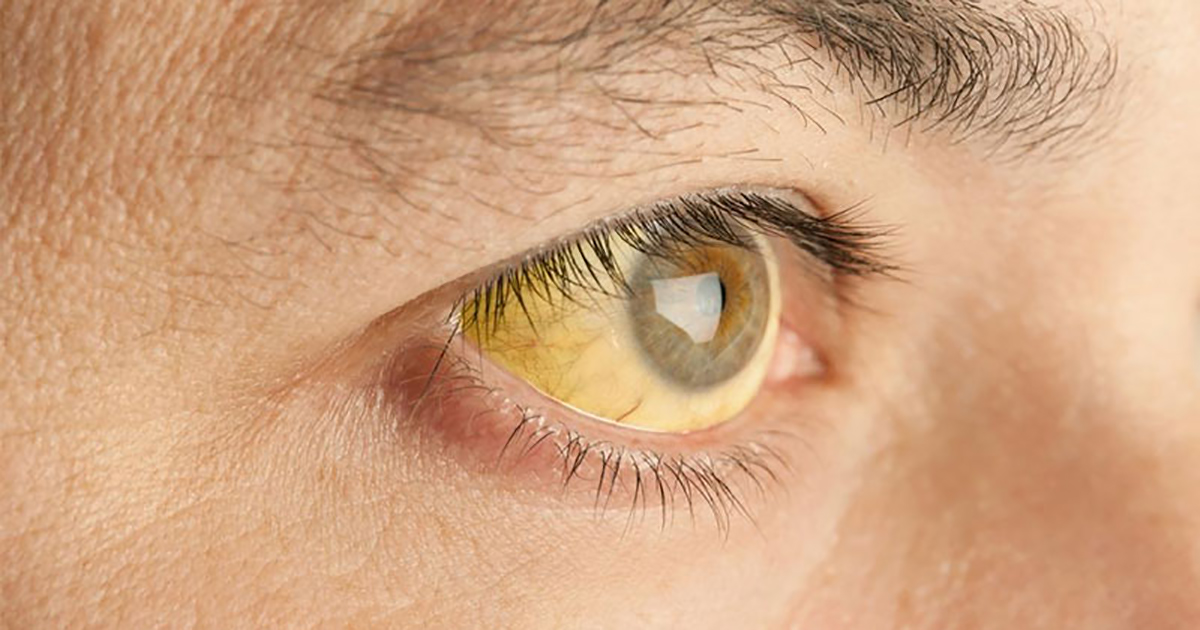
The symptoms associated with autoimmune hepatitis can range from minor discomfort to severe and occur quite suddenly and quickly. Some patients have very few noticeable problems in the early stages of this illness, whereas other patients can experience a variety of symptoms. These common symptoms include fatigue, abdominal discomfort, yellowing of the skin and whites of the eyes known as jaundice, abnormal blood vessels on the skin called spider angiomas, skin rashes, joint pain, and, of course, an enlarged liver. Females who experience autoimmune hepatitis could also lose their menstrual cycle as well.
What Causes It?
As previously mentioned, autoimmune hepatitis occurs when the body's immune system targets the liver and fights healthy cells, rather than viruses, bacteria, or other pathogens like it is supposed to. This attack on the liver can lead to chronic inflammation and incredibly serious damage to the liver cells, which can lead to a whole host of problems for the patient. Unfortunately, why the body's immune system attacks healthy liver cells and ultimately turns against the liver is unclear. However, researchers believe autoimmune hepatitis can be caused by the interaction of genes that control the immune system's function and the body's exposure to specific medications or viruses, therefore resulting in a triggered response of the body attacking the liver.
Risk Factors

Numerous factors can increase an individual's risk of developing autoimmune hepatitis, such as being female, as although both genders can develop this condition, it is more common in women, and genetics research has indicated a predisposition for this disease may run in families. If a patient has a history of certain infections, such as the measles, herpes simplex, or Epstein-Barr virus, they may develop autoimmune hepatitis after contracting one of these viruses. Autoimmune hepatitis has also been linked to hepatitis A, B, and C. Finally, if an individual has another autoimmune disease, such as rheumatoid arthritis, celiac disease, Graves' disease, or Hashimoto's thyroiditis, they may be more likely to develop autoimmune hepatitis. To learn more about other autoimmune diseases that could lead to autoimmune hepatitis, check out Uncommon Autoimmune Diseases Everyone Should Be Aware Of.
Types Of Autoimmune Hepatitis
Doctors have identified two types of autoimmune hepatitis, formally known as Type 1 and Type 2. Type 1 autoimmune hepatitis is the most common form and can occur at any age. Approximately half of the patients who have Type 1 also have other autoimmune conditions, such as celiac disease, rheumatoid arthritis, or ulcerative colitis. Type 2 autoimmune hepatitis is most commonly found in children and teenagers, as adults are less likely to develop it. Similar to Type 1, patients with Type 2 tend to also have other autoimmune diseases as well.
How Its Diagnosed
There are two main methods of diagnosing autoimmune hepatitis. The first method is through blood tests. A doctor will take a sample of the patient's blood and test it for antibodies, which are agents created by the immune system to fight pathogens, but in cases of autoimmune hepatitis, these antibodies attack the liver cells instead. Blood tests are important for distinguishing autoimmune hepatitis from conditions with similar symptoms, including viral hepatitis. In addition, an antibody test is useful for pinpointing a patient's exact type of autoimmune hepatitis. The second method is a liver biopsy, in which doctors take a small piece of the liver to confirm their diagnosis and determine the severity of the liver damage. The small portion is extracted through a needle and analyzed at a lab.
How To Treat It
Regardless of the type of autoimmune hepatitis an individual has, the predominant goal of treatment is to slow or completely stop the immune system from attacking the liver. Treatment can help slow the disease's progression through the use of medications that decrease the immune system's activity. Generally, treatment with prednisone is used initially, and doctors can use azathioprine in addition to prednisone. When medications do not work effectively to halt the progress of the disease or the patient develops irreversible scarring of the liver known as cirrhosis, or even liver failure, the only remaining option is a liver transplant.
Liver Transplant Recovery
Patients who do not respond to drugs that may help their autoimmune hepatitis or who have a great deal of scarring in their liver can opt for a liver transplant. A liver transplant is also a solution when the disease starts to cause the liver to fail. The patient's diseased liver is replaced with a healthy one donated from a corpse. They can also have part of a healthy liver from a living person, as the liver is the only organ in the body that can regenerate itself.
Liver transplant recovery begins in the intensive care unit of the hospital, where the patient is kept for about two days. After this, they are kept in the regular hospital unit for about week to ten days before they are discharged. Full recovery takes about three months. Most patients make a good recovery, but it is still possible for the disease to strike the transplanted liver.
Medications Continued

Physicians prescribe prednisone at a high dose for the first month of treatment, and gradually reduce the dose over the next several months until the lowest possible dose can be used to control the condition. This is due to the multitude of side effects prednisone can cause, such as diabetes, osteoporosis, osteonecrosis, high blood pressure, cataracts, glaucoma, and weight gain, especially when taken for an extensive period. Adding azathioprine to the treatment plan could help the patient avoid the deplorable side effects of prednisone. A majority of patients will need to continue to take prednisone for eighteen to twenty-four months and may remain on it for the rest of their lives, as autoimmune hepatitis can return if the drug is not taken regularly.
Cirrhosis
When autoimmune hepatitis is left untreated, it can lead to liver scarring, a condition otherwise known as cirrhosis. In fact, cirrhosis of the liver is often the first complication autoimmune hepatitis patients experience. It is also a common trigger for subsequent complications. The longer it goes untreated, the more damage the liver will incur, until a patient's liver fails entirely. It's important to diagnose and treat autoimmune hepatitis early to avoid liver failure. If the condition leads to advanced liver disease, patients might need to undergo a liver transplant.
Liver Cancer

Liver cancer is one of the complications of autoimmune hepatitis. This is because the disorder causes scarring in the liver, which increases the risk of cancer of the liver. The type of cancer that affects autoimmune hepatitis patients is called hepatocellular carcinoma. This is a primary cancer, which means the malignancy begins in the liver. Sometimes in other cancers, the malignancy will metastasize to the liver and cause a secondary cancer. However, even with autoimmune hepatitis, the incidence of liver cancer is rare.
In some studies of individuals with autoimmune hepatitis, none of the subjects came down with cancer of the liver, even if they had cirrhosis caused by their autoimmune disease. Individuals who were more likely to get hepatocellular carcinoma had hepatitis B or C, liver disease caused by alcoholism, chronic viral hepatitis, or primary biliary cirrhosis. Other patients who developed cancer of the liver had hemochromatosis, a condition where the body stores too much iron.
Fluid In The Abdomen

Fluid in the abdomen is called ascites, and this is common in individuals who have liver disease. It is an abnormal build-up of fluid inside the patient's peritoneal cavity and is a common sign of cirrhosis of the liver. Individuals who have ascites suffer from bloating, pain in the abdomen, and shortness of breath. Ascites gets its name because the fluid in the abdomen is full of protein, or ascetic. It happens because when the liver is cirrhotic, the portal vein that delivers blood to it is under abnormally high pressure, called portal hypertension. Because the blood is brought up from the intestine, one of the complications of ascites due to cirrhosis is a bleed in the intestine. This is considered a medical emergency.
Esophageal Varices
Esophageal varices, swollen veins in the esophagus, are another complication of autoimmune hepatitis. They very much resemble varicose veins. These veins occur in the lining of the esophagus and are a complication of cirrhosis of the liver and high blood pressure in the portal vein. They happen because the pressure in the portal vein forces blood into the blood vessels around it. This includes blood vessels in the esophagus, the tube that links the patient's mouth to their stomach. Varices in the esophagus can also be caused by blood clots in the portal vein. If the pressure in these veins becomes very high, they can rupture and bleed. When that happens, the patient will either vomit blood or swallow the blood, which will then turn their stool tarry and black. As with a bleed in the intestine, rupture of the esophageal varices is a medical emergency.
